Long Femur and Short Shins in the Leg Press: Disadvantage?
Can people whose femurs are shorter than their shins, regardless of torso length, have a mechanical advantage with the leg press?
Nearly all the attention regarding the long femur problem is directed at the back squat. (more…)
HOW Can a Knee Replacement Lead to a Heart Attack? Mechanisms

A person can suffer a heart attack only three days after a knee replacement (or other joint replacement) surgery.
Just HOW does this happen? (more…)
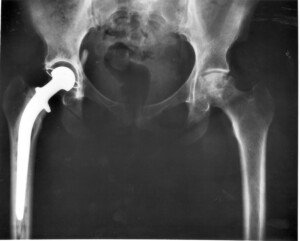
Hip Pain Three Months after Hip Replacement: Causes, Solutions

It’s not always normal to still have hip pain three months after a hip replacement. There are loads of possible causes for this pain.
The first possibility: Total hip replacement patients who fail to adhere to their rehab exercises.
If you’re too sedentary in the weeks following hip replacement surgery, there may be pain located about the hip simply due to stiff structures.
Postsurgical depression can sink in and result in being very inactive and spending a lot of time in bed — leading to a stiffened joint and underused soft tissue.
Patients also must ask themselves if the pain they’re feeling is actually coming from the hip or some other nearby area such as the thigh.
Thigh pain may radiate up towards the hip, creating the illusion that the pain is originating from the hip.
“First let me say that there is NEVER a 100% guarantee of 100% pain relief after a hip replacement,” begins Barbara Bergin, MD, board certified orthopedic surgeon at and co-founder of Texas Orthopedics, Sports & Rehabilitation Associates.
“This is a manmade operation, meant to relieve the pain of hip arthritis. Period.
“It is not meant to allow a person to return to sports or some level of activity they had when they were younger.
“Basing everything else I say on that premise, hip pain at three months might be completely normal.
“With a few exceptions, it takes the body about 6-9 months to completely recover from most injuries and surgery.
“So, pain at three months is kind of expected, and when patients tell me they have NO PAIN three months after a big operation, I thank the cosmos for sending me a happy, tolerant patient with a high threshold for pain, and reasonable expectations.
“Okay, so now that we have both extremes covered, let me think of what dangerous things might be causing pain at three months.
“Let’s start with bad things, which are not the most common things. Complications from total hip replacements are rare.
Blood Clot
“A blood clot (deep venous thrombophlebitis) could cause pain in the thigh or leg three months after a hip replacement.

Blood clot
“It’s unlikely but not unheard of, and in fact, we often keep patients on baby aspirin for three months after surgery on the lower extremity.
“But by then, patients are usually getting around, which means they’re pumping that venous blood out of their legs, so it’s not sitting around forming clots.”
Infection
“Infection can occur at any time following a joint replacement, from the day after, to years later.
“Patients and doctors are always on the prowl when it comes to sudden changes in pain, especially if accompanied by fever, redness or swelling.
“The surgeon takes extreme precautions and steps to prevent this disastrous outcome, and fortunately…it is rare.”
Dislocation
“Dislocations can also occur at almost any time following a hip replacement, but are less likely to occur as time goes by.
“There will be no question in the patient’s mind that something very bad has occurred, when the hip dislocates.
“Not only is it painful, but they will not be able to move. It can occur as the result of a fall, but it can also occur with some very common movements.
“This will require a visit to the emergency room because of the pain.
“The hip will be put back in place. Surgeons also take many steps to prevent this kind of problem, and it too is rare.
“Now to the less dangerous, although always concerning causes of pain.”
Activity
“Soreness from increased activities occurs as patients get more active, once the surgical pain has died down.
“They’ve returned to the gym, started walking more or might have increasing demands placed on them in physical therapy.”
Seroma
“Minor surgical setbacks can occur in this period of time, like the development of seromas (fluid leaking out of the depths of the wound, and causing swelling and pain).”
Small Fracture
“Occasionally a small fracture could result from the surgery. The surgeon usually knows when this occurs and depending on what type of fracture, they might fix it at the time of the surgery.
“There might be some remote possibility that a tiny fracture could be missed, and this could result in pain later on if it doesn’t heal. Again…rare.”
Loosened Hardware
“There is an unlikely chance that something could come loose after the surgery. Again, very rare, but there would be some pain associated with it.”
Activities that Can Loosen Hip Replacements (especially cement) and Cause Pain
- Impact (jogging, tennis, horseback)
- Heavy weightlifting
- Jumping from heights
- Gaining excess weight
Not following the rules for the first eight weeks following hip replacement surgery could result in pain that lingers.
Don’t bend the operated hip beyond 80 degrees.
Don’t raise your knee higher than hip.
Avoid sitting on low seats.
Avoid leaning forward when sitting.
In rare cases hip pain can result from leg length disparity or nerve damage.
If you’re still having pain three months out, or you have new-onset pain three months or so out from the hip replacement, don’t put off making an appointment with your surgeon.
It’s rare that a pain after surgery would not have an explanation.
Additional Causes of Hip Pain that Can Persist or Develop Three Months After Surgery
(Source: Clinical Cases in Mineral and Bone Metabolism, Ferrata et al, 2011)
• Bone loss
• Abnormal formation of bone
• Bone remodeling in response to physical stress
• Inflammation of synovial fluid
• Allergy to metal wear debris
• Prosthesis impingement
• Iliopsoas tendinitis
• Abductor muscle damage

Dr. Bergin is a general orthopedist, surgically and conservatively treating all manner of bone and joint conditions. She enjoys educating patients so they can emerge stronger than they were before their orthopedic injury or surgery.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Sources
bertjthomasmd.com/after-operation-thomas-orthopedics.html
ncbi.nlm.nih.gov/pmc/articles/PMC3279074/
Best Strength Training Exercise for Anxiety After Menopause

One of the simplest strength training moves is actually the best for fighting off anxiety during postmenopause.
Women of all sizes can do this exercise! (more…)
Barefoot Babies & Toddlers in Public: Safe or Unsanitary?
A baby or toddler barefoot in public can catch a nasty infection.
But sanitation aside, some people think it’s gross. Little dirty feet can stink and appear grubby.
Babies’ and toddlers’ bare feet will get grimy, soiled and filthy after being on a dirty public floor or other surface.
Many babies will play with their toes at some point, once they’re placed back in a stroller in the car.
One day I was standing behind a woman and her toddler barefoot son.
She picked him up and placed him feet first on the checkout conveyer — which was filthy!
She did this so that he could stand and grab an item from the display on the other side of the conveyor.
After she set him back in the shopping cart, lo and behold, he began playing around with his toes, then put his fingers in his mouth.
Fungus Infection, Stomach Flu
“The most common infections contracted from bare skin coming in contact with a contaminated surface are fungal skin infections (e.g., ringworm, aka tinea corporis),” says Irene Tien, MD, a board-certified emergency medicine and pediatric emergency medicine physician in MA.
Dr. Tien continues, “A child whose feet come in contact with any bacteria that can cause food poisoning (e.g., salmonella, E. coli, norovirus, rotavirus) and then are put in his mouth can make the child develop a stomach flu (vomiting, diarrhea).”
Salmonella and E. coli can easily make their way onto a grocery store conveyor belt!
Babies routinely put their toes in their mouths. Is this any more hygienic than if a flexible 12-year-old had his dirty toes in his mouth?
I’m betting most people would deem this very uncouth and unsightly, simply because the boy is 12 years rather than 12 months.
How to Keep Feet Covered
“Baby shoes” are often considered unnatural and uncomfortable, but supportive sneakers for babies have been on the market for many years.
And there are also booties for babies. Plus, toddlers are ready for little sneakers.
Walmart’s Floors and Barefoot Babies
Parents allow their babies and toddlers to scamper about on Walmart’s floors barefoot.
Indoors or out, a toddler’s bare feet can get punctured by particles of glass; bits of sharp food like peanuts, peanut shells and tortilla chip fragments; a thumbtack, rusty nail or other tiny piece of hardware.
And of course, animal feces.
This problem also occurs at airports. Why don’t parents put socks or booties on their babies’ and toddlers’ feet? The floors of airports are filthy.
Toddlers and babies who can walk love this freedom to ambulate.
The irony is that when they’re barefoot, their ability to ambulate is hampered.
They also run the risk of stubbing a toe (not to mention stepping on something sharp).
Barefoot baby proponents may argue that bare feet can “breathe.” They may insist that those hard baby shoes will ruin bones (though certainly, special supportive footwear and booties won’t).
They may also point out that their baby will remove the booties, so what’s the use?
- Find booties that can’t be pulled off.
- Many parents haven’t even tried booties.
It takes only moments to slip on booties or footwear, so it’s doubtful that saving a few seconds is the reason parents don’t cover their babies’ feet in public.
Babies’ feet can stink.
I once read about a woman who said her nine-month-old daughter’s feet were really stinky, so she always rubbed cream on them and kept her barefoot in public (as well as at home).
Finally she consulted with a pediatrician and was told to stop applying the cream, wash the feet daily with soap and water, and have the baby wear clean socks; the socks would wick away any perspiration.
I wonder how often a baby’s bare feet are dry and odorless, rather than moist, sticky and stinky. Feet, by nature, stink.
Especially bare feet that have been pitter-pattering around on filthy public floors.
And if socks fall off?
Well, as one anti-barefoot mother said on a posting board, “Just put them back on!”
A baby or toddler will repeatedly drop their “binkie,” but mothers don’t mind repeatedly picking the germy thing up from the floor and placing it back in the child’s mouth.
So why is putting socks or booties back on so daunting?
 In practice for 20+ years, Dr. Tien is a leading medical voice on social media, providing the public with accurate information to empower them to live their healthiest life.
In practice for 20+ years, Dr. Tien is a leading medical voice on social media, providing the public with accurate information to empower them to live their healthiest life.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Sources:
whattoexpect.com/forums/hot-topics-1/topic/barefoot-babies
answers.yahoo.com/question/index?qid=20080603195036AAnhwTT
Two Menstrual Periods Back to Back, Right in a Row

Ever had one menstrual period right after the other—so just as one period ends, the next one begins?
This phenomenon is characterized by about 10 or so consecutive days of bleeding.
The first cycle in this duet is nothing out of the ordinary.
The second period right on top of it is also nothing out of the ordinary.
The only thing really crazy is that these two periods are back to back.
This once happened to me, and I want to assure you that nothing ever came of it. It happened years ago.
I had my typical period, which includes cramping a few days before real flowing. Prior to real flowing was spotting.
Often, I’d feel cramps for at least two days, occasionally on the third day.
So for this first of the two cycles, I had cramps the first three days and the flowing peaked. Then the bleeding began tapering off.
Just when I thought that this period was over, I began feeling cramps.
Cramps at the end of a period had never before occurred, and I thought this was really strange.
Why was I having cramps at the end – like day 6 or 7, which normally just consisted of brownish-red spotting (residual blood)?
The spotting then began morphing into a pinkish tan, resembling the spotting at the front-end of a menstrual cycle.
And each day after the first period apparently ended, I continued to spot…more and more, until it dawned on me: I’m having another period!
The cramping kicked up and so did the bleeding. The flowing was now like a normal period, and I had to replace my panty liners with maxi pads.
A second period…two smack in a row, back to back! How odd was THAT?
This incident of back to back periods happened only once in my entire life. I’m now postmenopausal.
Back to Back Periods vs. Prolonged Menstrual Bleeding
These two issues are not to be confused. Two periods in a row without any “rest” in between is not the same event as is a single period in which the bleeding is prolonged.
In my case, the first period began with the typical spotting and then escalating amount of blood, peaking on the first and second day.
Then the flow began dwindling on day 3, getting less and less by day 5. And of course, the cramping tapered off early on.
But then things started kicking up again, and the backend spotting morphed to the appearance of frontend spotting, which escalated to full-blown bleeding in the same timeline as any of my typical menstrual cycles.
So there were clearly two cycles here.
Causes of Prolonged Bleeding in a Single Menstrual Cycle
Prolonged bleeding of a single period is a different issue.
“There are multiple possible causes for prolonged bleeding with menses,” says Lindsay Appel, MD, an OB-GYN with the Family Childbirth & Children’s Center at Mercy Medical Center in Baltimore.
“Sometimes, hormonal imbalances can cause anovulation which can lead to irregular episodes of bleeding. In addition, thyroid abnormalities can also impact the menstrual cycle.
“Structural abnormalities of the uterus and endometrium (the lining of the uterus) can also contribute to prolonged bleeding.
“These include uterine fibroids, endometrial polyps or endometrial hyperplasia which is an overgrowth of the endometrium and can lead to endometrial cancer.”
If you can’t tell if you’ve had a prolonged cycle vs. two back to back periods, make an appointment with your gynecologist.
 Dr. Appel addresses a full range of obstetric and gynecologic needs for women. She has participated in several OBGYN research presentations at professional conferences.
Dr. Appel addresses a full range of obstetric and gynecologic needs for women. She has participated in several OBGYN research presentations at professional conferences.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Dense Breasts: What an Automated Breast Ultrasound Feels Like

The automated breast screening ultrasound is the latest technology that women with dense breasts should have.
Perhaps the biggest advantage to this technology is that it pretty much eliminates operator error. (more…)
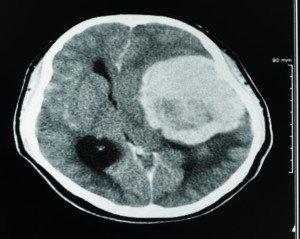
Can a CT Scan Detect a Brain Tumor?
If you had a non-contrast CT scan of your head for whatever reason, such as you fell on your head and feel sick, would it necessarily show a brain tumor if you had one?
“The test of choice to evaluate for brain tumor is the MRI with and without the contrast,” says neurosurgeon Charles Park, MD, Director of The Minimally Invasive Brain and Spine Center at Mercy Medical Center in Baltimore.
“CT’s are usually better to assess the bone related problems and MRI is better for the soft tissue,” says Dr. Park.
However, the CT scan can be used as part of a diagnostic assessment if a brain tumor is suspected.
According to hopkinsmedicine.org, a CT scan “can be helpful in diagnosing some types of brain tumors,” particularly “those near or involving bone.”
The CAT scan can also show bleeding, swelling, bone and tissue calcification that would be caused by a cancer.
If a person has a seizure or exhibits some other alarming sudden symptom such as cognitive impairment, a family member is apt to get that person to the emergency room.
A CT scan will be ordered to find out what’s going on. It will generate an image much faster than will an MRI. Its speed makes it the head scan of choice in emergency situations.
Contrast Dye with the CT Scan?
Dr. Park says, “Using contrast for CT usually is better, since brain tumor will usually enhance or gets brighter on contrast CT.
“Non-contrast may hint at an abnormality but not as conclusive as enhanced CT or MRI.”
The MRI is the gold standard for diagnosing most brain tumors. A contrast dye is used.
The cancerous mass usually “soaks up more dye than normal brain tissue,” says hopkinsmedicine.org.
This will clearly show up on the scan. However, there’s the occasional cancer mass that will not absorb more dye than the surrounding tissue.
CT scans without any contrast are terrific for showing bleeding in the brain from head trauma, but not the mass of a tumor.
Dr. Park specializes in minimally invasive surgical techniques for treatment of conditions affecting the brain and spine. He’s skilled in advanced procedures and techniques that utilize innovative computer technology and image-guided surgery systems.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Richman Photo
Source: hopkinsmedicine.org/neurology_neurosurgery/centers_clinics/brain_tumor/diagnosis/how-to-diagnose-brain-tumors.html
Can a Blood Test Detect a Brain Tumor?
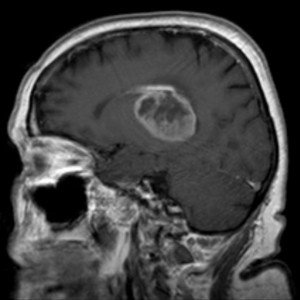
“Depending on the tumors, some blood tests can be used to detect a brain tumor,” says neurosurgeon Charles Park, MD.
“But most of the cases, we find the brain tumor and then do the blood test to see what kind of tumor it is,” says Dr. Park, Director of The Minimally Invasive Brain and Spine Center at Mercy Medical Center in Baltimore.
“For example, if someone has a pituitary tumor, we will do the blood test to see if that tumor is active and producing a certain kind of hormone.
“If it produces prolactin, then we can use medicine to shrink the tumor without surgery.”
How close are researchers to developing a blood test that detects the presence of a brain tumor?
Microvesicles are cell particles that are shed by cancer cells and end up in the bloodstream. They are small enough to cross the blood-brain barrier.
If these can be picked up by a blood test, they potentially can diagnose a brain tumor.
The most common primary brain tumor is a glioblastoma multiforme. By the time this is diagnosed, a patient will usually be dead within 15 months.
The only way currently to diagnose and also monitor a GBM is via imaging tests and biopsies. This is anything but efficacious.
But a simple blood test to do these tasks would change medicine.
Enter Nanotechnology
This groundbreaking technology can be used to magnetically (nuclear magnetic resonance) label the microvesicles.
Researchers are now able to, using a handheld nuclear magnetic resonance instrument, reliably detect microvesicles from tumors in blood samples.
The blood samples with the reliable detection came from both mice and humans with the GMB brain tumor.
The report, published in Nature Medicine (2012), says that this blood test for the brain tumor can be done in a doctor’s office.
So why isn’t this a standard test in doctors’ offices? Well, like any research, this technology must go through a series of phases before it becomes commercialized
Another Possible Blood Test for Detecting a Brain Tumor
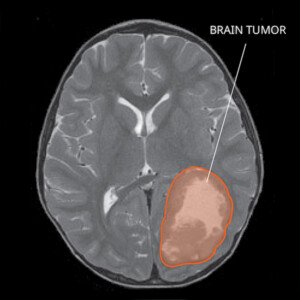
In another study, “nearly all forms of cancer were identified,” says cancer researcher Jonas Nilsson in the report, “which proves that blood-based biopsies have an immense potential to improve early detection.”
The study that he’s referring to, which had a 96% detection accuracy rate, comes from Umeå University in Sweden and was published in Cancer Cell (2015).
The test was done on 228 people with cancer. That was just the detection of a cancer.
As for the origin of the malignancy, there was a 71 percent success, and this origin pertained to the lung, colon, breast, pancreas, liver, rectum, and the brain.
Dr. Park specializes in minimally invasive surgical techniques for treatment of conditions affecting the brain and spine. He’s skilled in advanced procedures and techniques that utilize innovative computer technology and image-guided surgery systems.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Hellerhoff
Source: sciencedaily.com/releases/2015/11/151112123708.htm
Cause of Two Periods 14 Days Apart Happening Only Once

The cause of a period coming exactly two weeks after the one before that, and never happening again, may very well be from desire and will.
A subconscious instruction to start menstruating 14 days after the previous period? Yes, it’s possible.
But it’s also possible for the instruction to be conscious or more deliberate.
“Menstrual bleeding that comes two weeks after the previous period is likely due to anovulation or lack of releasing an egg,” Dr. Kimberly Langdon, MD, medical advisor at Medzino.
“Lack of ovulation may be due to stress, and that certainly can be the case prior to one’s wedding [or vacation],” adds Dr. Langdon.
Vacation to Be Ruined by Period
Some years ago I had planned a trip to Hawaii. The days I’d be there fell smack on the days I was expecting my next period. I was infuriated.
This was a big thorn in my side in the weeks leading up to the vacation.
According to the first day of my previous period, my next cycle would begin a few days after I arrived in Hawaii! I was fuming!
14 Days Between Two Periods
However, two weeks after the preceding menstrual cycle began, I started another period; the interval was only 14 days.
This meant that the last day of this next menstruation was the first day of my 10-day vacation!
I just felt SO elated, sitting on that plane as it flew over the ocean, knowing that THIS day was the LAST day of my cycle!
I just couldn’t believe it worked out this way – a 14 day interval! It was a gift!
Never before had I had a two week interval (my next-shortest interval had been 19 days, and these were only a few or so), and no 14-day interval ever occurred again.
I have to believe there was a psychological component to this. Could my internal griping about the projected date of my next cycle have actually “instructed” my cycle to come much sooner to spare me the inconvenience during my vacation?
There is no way that this was a coincidence.
In all the years that I had been menstruating, what are the odds that the ONLY time I have two periods 14 days apart coincides perfectly with a much-anticipated trip to Hawaii?
Is “willing” menstruation to begin sooner a dependable method?
Dr. Langdon says it is not.
“There are medical ways to cause a period to come early or to delay one for a week or two,” says Dr. Langdon.
“Birth control pills can be used to delay a period by skipping the placebo pills and starting the next pill pack during the week that the period is expected.
“The mind is a powerful tool for change, so it’s not out of the realm of possibility that one could ‘will’ an early period — especially if anxiety is severe enough.
“Anxiety is stressful, and stress affects our menstrual cycles among other bodily processes.”
Because I am now postmenopausal, I can say with 100 percent accuracy that the 14 day interval between two periods was a one-time event.
 Dr. Langdon, who is now retired from clinical practice, has delivered over 2,000 babies. Besides obstetrics, she specialized in gynecologic situations such as menstrual disorders, vaginitis, menopause, contraception, pelvic pain and minimally-invasive surgeries.
Dr. Langdon, who is now retired from clinical practice, has delivered over 2,000 babies. Besides obstetrics, she specialized in gynecologic situations such as menstrual disorders, vaginitis, menopause, contraception, pelvic pain and minimally-invasive surgeries.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.