Why Some Breast Cancers Stop Responding to Targeted Therapy?

I’t’s very depressing to patients when they are told that their breast cancer has stopped responding to the targeted therapy.
When it comes to breast cancer, “Failure to respond to targeted therapy can be multifactorial,” says Anita Johnson, MD, FACS, a breast surgical oncologist with City of Hope Cancer Center in Atlanta, GA.
What Is Targeted Breast Cancer Therapy?
Cancer cells have specific characteristics. They are not all alike. An example of a characteristic would be the cell growing out of control due to a particular protein.
A targeted therapy for that kind of cancer cell, then, would be to oppose the protein.
Another type of targeted therapy for breast cancer is the use of antibodies that work similarly to the body’s natural antibodies.
Targeted therapy does what the name says: targets these unique characteristics of cancer cells.
This type of treatment is not the same as chemotherapy and, in fact, usually yields less harm to normal tissue.
As hopeful as this sounds, there sometimes comes a point where the targeted therapy ceases to be effective.
Or, to put it another way, the breast cancer cells stop responding to it.
Why Does This Happen?
Dr. Johnson explains, “Tumor types including endocrine positive tumors and HER2 neu positive breast cancers have usually responded well to targeted therapy.
“In certain populations, failure may be due to multiple reasons including stage at presentation, timeliness to treatment as well as, most important, the molecular component of the tumor.”
Early stage disease has a better prognosis than that of later stage.
This is why annual mammograms and monthly self-exams are crucial.
Dr. Johnson also explains, “Several mechanisms have been reported with resistance in HER2 neu therapy and endocrine therapy, including changes in the receptor as well as changes in the micro-environment of the tumor and host-related factors.”
 Dr. Johnson performs lumpectomies, and skin-sparing and nipple-sparing mastectomies, breast ultrasounds, needle core biopsies, infusaport placements, genetic testing and counseling, plus works with radiation oncologists to treat breast cancer using intraoperative radiation therapy.
Dr. Johnson performs lumpectomies, and skin-sparing and nipple-sparing mastectomies, breast ultrasounds, needle core biopsies, infusaport placements, genetic testing and counseling, plus works with radiation oncologists to treat breast cancer using intraoperative radiation therapy.
.
Top image: Shutterstock, otnaydur
Pain & Burning in One Breast for a Month: Cancer or Infection?

If one breast has been painful and burning for the past month, the most likely cause is not as scary as you think, though breast cancer CAN be a cause.
In the U.S., approximately 264,000 women are diagnosed with breast cancer each year.
This estimate is based on data from the American Cancer Society as of 2024.
Breast cancer remains one of the most common cancers among women.
So it’s logical to wonder about all the symptoms that breast cancer might cause.
Could pain and burning be among these symptoms?
“Pain and burning in the breast for one month is usually associated with caffeine and/or nicotine use,” begins Anita Johnson, MD, FACS, a breast surgical oncologist with City of Hope Cancer Center in Atlanta, GA.
“Pain and burning in the breast can also present in women who are either perimenopausal or postmenopausal.
“Infection may be a cause but will usually worsen as time goes by and responds to antibiotics.”
The Worst Possible Cause
“Breast cancer can present as pain and burning, but this is an uncommon presentation,” says Dr. Martin.
“If there is noted swelling of the breast with associated erythema [redness] or dimpling of the skin, this may be a sign of inflammatory breast cancer.” The dimpling resembles that of an orange peel.
“Inflammatory breast cancer does not respond to antibiotics. Inflammatory breast cancer is a very aggressive form of breast cancer and you should contact your provider as soon as possible.”
Most cases of BC do not come with pain, aching or soreness in the breast itself.
When a woman discovers a symptom, it is usually a lump that she finds when performing a self-exam or during an incidental touch such as while dressing or showering.
Sometimes her doctor will discover the lump during a routine clinical exam.
Some Other Symptoms You Should Look Out For
• Inverted nipples, though this doesn’t always mean BC, especially if they’ve been inverting since as long as you can remember.
• Discharge from the nipple other than milk.
• Puckering in the skin.
• A feeling of new-onset hardness or thickening in the skin during a self-exam.
• Sudden but brief shooting, stabbing, piercing or sharp pain in the breast is very unlikely to be caused by a malignant tumor.
The Cancer Treatment Centers of America main site lists additional symptoms to be concerned about, which can suggest inflammatory BC:
• Increasing size or shape of one breast
• Itchiness in a breast
• Warmth in a breast
• A peeling or flaking nipple
 Dr. Johnson performs lumpectomies, and skin-sparing and nipple-sparing mastectomies, breast ultrasounds, needle core biopsies, infusaport placements, genetic testing and counseling, plus works with radiation oncologists to treat breast cancer using intraoperative radiation therapy.
Dr. Johnson performs lumpectomies, and skin-sparing and nipple-sparing mastectomies, breast ultrasounds, needle core biopsies, infusaport placements, genetic testing and counseling, plus works with radiation oncologists to treat breast cancer using intraoperative radiation therapy.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com jcomp
Source: cancercenter.com/breast-cancer/symptoms/
Can a Man’s Deodorant Cause Breast Cancer in a Woman?

Is there a link between using a man’s deodorant and breast cancer in women?
With all the fear of this and that causing breast cancer, some women are seriously wondering if using a man’s deodorant can lead to cellular mutations that can trigger malignant transformation in breast cells. (more…)
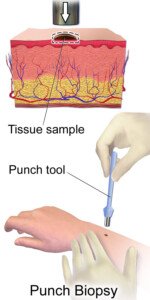
Percentage of Mole Biopsies that Come Back Melanoma?

If you’ve ever had a mole removed for biopsy, have you ever wondered what the mathematical odds were of it coming back as melanoma?
It’s unimaginable how many moles every year in the U.S. or any other given industrialized nation are removed for biopsy on a yearly basis.
The number must be astronomical, but the percentage of these mole biopsies that come back positive for melanoma would be a constant, not a variable, as long as the parameters remained the same (e.g., only those moles that a dermatologists finds suspicious).
For instance, five percent of 100,000 is the same “odds” as five percent of 100 million.
Percentage of Mole Biopsies that Are Positive for Melanoma
“The percentage of mole biopsies that come back as melanoma is dependent on why the mole is biopsied,” begins Jena Martin, MD, a board certified anatomic and dermatopathologist based in the Minneapolis area.
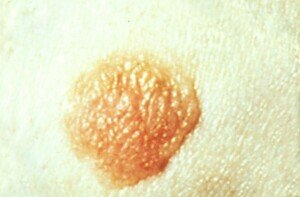
Common mole
“I like to think of this concept (statistically called the positive predictive value) as ‘garbage in, garbage out.’
“So if your doctor biopsies a mole that he or she believes is benign, the odds it will be melanoma is nearly zero.
“When we look at biopsies of moles that dermatologists are worried about (moles that look odd or funny), the typical rate is about 15-20 biopsied needed to diagnose melanoma.
“In the medical literature this is called the number needed to diagnose (NND).
“For every 15-20 worrisome moles that a dermatologist biopsies, they can expect to find one melanoma.”
What does this mean in terms of percentage?
Let’s look at the upper end of this: one in 20. A ratio of one out of every 20 is five percent.
If you recall your grade school math, to figure out a percent, divide the “out of every” number INTO the smaller number.
So one divided by 20 equals 0.05. Move the decimal to the right two places to get 5: five percent.
Using this grade school formula to figure out percentages, you’ll see that one out of 15 means 6.6 percent.
So if a dermatologist wants a suspicious spot removed, the odds that this will come back as the deadliest skin cancer are 5 to 6.6 percent.
But remember, this percentage pertains strictly to moles that a dermatologist is concerned about.
If the doctor says, upon examining your moles, “I’d like to remove this one here because its network gets my attention,” then there is probably a 5 to 6.6 percent chance that you’ll get horrible news.
“Many moles that are benign are also removed for cosmetic reasons, or because a patient is worried and the dermatologist is not; those don’t count in that statistic,” says Dr. Martin.
A study of over 80,000 skin samples which included lesions other than moles, that were sent out for biopsy, turned up a different percentage rate of melanoma diagnoses. Continue reading…
 Dr. Martin trained at Mayo Clinic Pathology and has been practicing for 20+ years.
Dr. Martin trained at Mayo Clinic Pathology and has been practicing for 20+ years.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Andrey_Popov
When a Skin Sample Is Sent for Biopsy: Handling the Anxiety
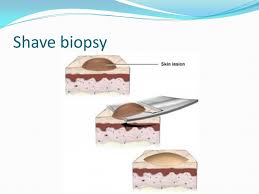
It’s just plain total anxiety when a skin sample is sent off for a biopsy, especially when you did not expect this to happen, and all you can think of is “What if it comes back as melanoma?”
If this occurs on a Friday, your entire weekend will probably be shot down with intense anxiety. (more…)
How Common Are Bloody Stools with Colon Cancer?

Seeing blood with your stools is just plain frightening, as this immediately brings to mind colon cancer.
Though hemorrhoids are a common cause of blood mixed with poop, it’s hard to ignore more sinister explanations. (more…)
Can Melanoma Be Mistaken for Normal Cells Under a Microscope?
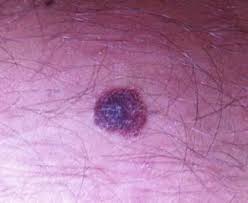
It’s scary but true:
For any number of reasons, a pathologist may mistake melanoma for benign cells under a microscope and incorrectly diagnosed the sample. (more…)
How Long It Takes a Lab to Analyze Mole Biopsy for Melanoma
When a dermapathologist views mole cells under a microscope, how long does it take them to identify if it’s melanoma or benign?
Your doctor will tell you it takes a week to two weeks for “the results to come back.” Sometimes the doctor will say it’ll take “a couple days.” (more…)
Can a Mole Be Too Tiny to Biopsy for Melanoma?
If your dermatologist told you that a mole is too tiny to be biopsied, and to wait a little longer to see if it gets bigger, get a second opinion. (more…)
Is the 16:8 Diet Just Another Passing Fad?
Let’s get the straight & narrow on the 16:8 diet: Is it effective or just another hyped up fad?
In the 16:8 diet, you eat whatever you want for eight hours only during a given day, and then absolutely nothing (other than water and zero-calorie drinks) for the other 16 hours. No exceptions.
The hours of feasting are from 10 am to 6 pm.
The hours of fasting are from 6:01 pm to 5:59 am.
Sounds easy enough, right?
Well, according to a study of 23 obese people (average age 45, average body mass index 35), the 16:8 diet has merit.
The participants followed the 16:8 diet for 12 weeks and lost weight plus improved their blood pressure.
• On average they ate 350 fewer calories/day.
• The average weight loss was three percent of their body weight.
• This is the first study of the 16:8 diet, and the full report is in Nutrition and Healthy Aging (June 2018).
During the eight hours that one can eat, there are no limits on type of food or quantity.

Shutterstock/Hurst Photo
On one hand, it’s easy to see why there was some weight loss. Many overeaters do much of their feasting after they get home from work – the very hours that are off-limits from eating on the 16:8 diet.
But on the other hand, knowing that you can’t eat even a bite between 6 pm and bedtime might encourage more overeating earlier in the day to avoid feeling hungry later in the evening.
Overall, though, for the 23 participants, this did not happen enough to thwart a collective weight loss over 12 weeks.
Another point to consider is that for some individuals, most overeating occurs at home for several reasons, and most people are away from home, at work between 10 am and 6 pm — where binge eating can be impossible with certain jobs.
Being at home, watching evening TV shows, means a strong conditioned stimulus for overeating.
The study authors do not recommend that the 16:8 diet be a permanent solution, as it still encourages overeating, and includes unlimited amounts of junk food.
Sustainability of the 16:8 Diet
“16:8 is one of the many versions of intermittent fasting which is not sustainable in the long run,” says Shana Spence, MS, RDN, CDN, a registered dietitian nutritionist based in New York, and was not involved with the study.
“There are some researched benefits to fasting — weight loss being one. Yes, you’ll definitely lose weight if you’re restricting your intake — but is it sustainable? I don’t think so.
“As for my overall opinion, the idea of limiting yourself to an eight hour window seems like an extreme.”
 Shana Spence of The Nutrition Tea is committed to providing trending information and nutrition facts covering a wide range including nutrition for heart disease and diabetes, pediatric nutrition and healthful lifestyles.
Shana Spence of The Nutrition Tea is committed to providing trending information and nutrition facts covering a wide range including nutrition for heart disease and diabetes, pediatric nutrition and healthful lifestyles.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.