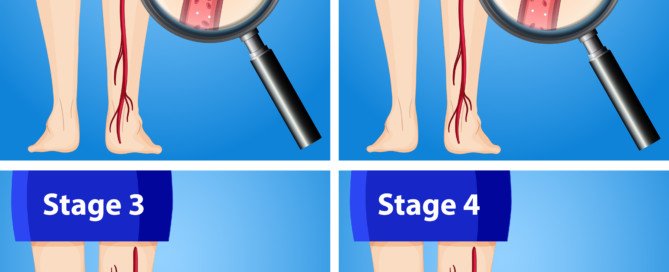
Why Kids Have a Lower DVT Risk than Adults with Air Travel

Children have a lower risk of DVT from long plane rides than do adults. They’re not immune to blood clots, but are much less likely to get them. Why is this?
Herniated Disc Pain Relief: Simple Non-Surgical Treatment
Before hastily deciding to have surgery for your newly diagnosed herniated disc, you should take this non-surgical approach.
Can a Chronic Subdural Hematoma Be Caused by Jumping Exercise?

If you’re over age 65 and do jumping exercises, could you end up with a chronic subdural hematoma?
Can Frequent Staircase Use Cause Knee Arthritis?

Can all that walking up and down a staircase possibly cause your knees to become arthritic?
And what about using a staircase or stepping machine for exercise? (more…)
Can You Get a Stroke if Your Carotid Angiogram Is Normal?
Does a normal carotid angiogram mean you’re safe from getting a blood clot that can cause a stroke or TIA?
Why Is Melanoma Follow-up Screening Only Annually?
After treatment for melanoma, the patient’s follow-up screenings eventually default to yearly, when initially they are every three to six months for up to two years after diagnosis.
Is Chest Pain in Women More Likely a Heart Attack or Benign?
Is there anything unique about heart attack chest pain in a woman that she could tell it’s probably a heart attack rather than something benign?
How Many People Get DVT While Not on Blood Thinners?
Out of 900,000 annual U.S. cases of DVT, how many patients are not on Coumadin, a potent prescription blood thinner?
Are Compression Stockings on Airplanes Needed to Prevent DVTs?
Shouldn’t ALL people on an airplane wear compression stockings to prevent a DVT?
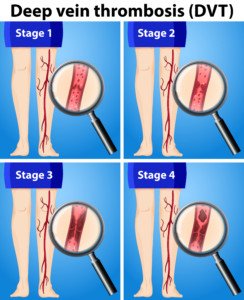
Sitting cramped in an airplane for many hours can cause a blood clot to form in the leg.
If you’re familiar with deep vein thromboses, then you know that a piece of one can spontaneously break off and quickly travel to the lungs, cutting off blood flow. Death can occur rapidly.
“Dehydration, especially during plane trips, can cause the blood to be thicker,” says Steven Elias, MD, a vein specialist with Englewood Health in NJ.
Thick blood is more likely to clot. A DVT most often develops in the lower leg, but they can also develop behind the knee and in the upper leg.
A person can have a deep vein thrombosis without any symptoms.
Young adults on plane trips are not immune to these blood clots.
One way to offset this problem is to keep hydrated while on the airplane: with water or juice, not alcohol or soda!
The latter two types of fluids have a dehydrating effect.
You should hydrate before the long airplane trip, not just during, even if that means having to get up several times to use the airplane’s restroom.
What about compression stockings for even younger, healthy and fit adult flyers?

Shutterstock/Lentpjuve
Dr. Elias explains, “Over the counter or prescribed graduated compression knee-high stockings can also help maintain good blood flow in the veins.
“I feel it is important to wear these on long plane or car trips. The business traveler should be aware of these simple preventative measures.”
In other words, you need NOT have blaring risk factors for DVT to be a candidate for wearing compression stockings while on an airplane. This advice applies to healthy fit people.
DVT Doesn’t Discriminate
Fit and healthy people can develop a DVT during long airplane rides — especially if they drop their guard and end up immobilized in the seat for several hours engrossed in computer work, reading or sleeping.
However, wearing compression stockings while traveling by air does NOT offset the need to keep hydrated and to avoid staying inert for long periods.
Don’t remain seated for longer than an hour, and while seated, move the legs frequently. Do all you can for DVT prevention.
If you have leftover TED hose from a previous surgery, don’t use these on an air flight, says Dr. Elias.
He explains: “TEDs are used for bedridden patients in the hospital/nursing home. To prevent blood clots for air travel/car trips, patients should wear gradient compression stockings (knee high) and not TED stockings.”
Next time you’re on an airplane, check the airline’s magazine that should be tucked in the pocket of the seat in front of you; most airline publications include exercises one can do to help prevent deep vein thrombosis.
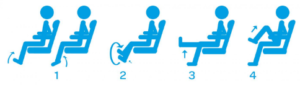
Basic exercises to prevent DVT on a flight.
 Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.