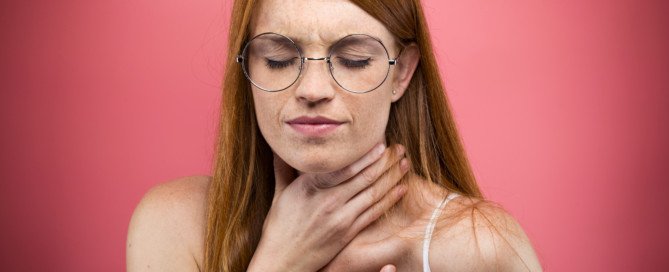
Always Feeling Heartbeat in Chest: Benign or Serious?

A cardiologist explains what it means to often feel your heartbeat in your chest.
This doesn’t refer to feeling your heart beating in your chest after you just did 20 squat jumps or ran hard on a treadmill.
This is about when this occurs in the absence of physical exertion — and anxiety, of course, which could really get the heart thumping good.
“Patients will commonly describe an abnormal sensation of feeling their heartbeat in the chest or an unpleasant awareness of your own heartbeat,” says Chester M. Hedgepeth, III, MD, PhD, Executive Chief of Cardiology at Care New England.
“This can be quite distracting. Fortunately, this is usually a benign finding.
“This sensation can be due to either forceful beating of the heart or due to increase in the heart rate (greater than 100 bpm while sitting still).”
Causes of Feeling Your Heart in Your Chest
Remember, that’s where this organ is located. Dr. Hedgepeth explains, “Forceful beating of the heart and/or increased heart rates leading to palpitations may be caused by anxiety, stress, panic attack or fear.
“Increased caffeine, nicotine levels or other stimulant use (e.g., diet pills, amphetamines, cocaine) are also associated with these types of palpitations.”
The so-called energy drinks can also produce this effect.
These drinks often contain high levels of caffeine, which can stimulate the heart and increase its rate.
Additionally, many energy drinks have other stimulants like taurine and ginseng that can also affect heart function.
For some people, these ingredients can cause the heart to beat harder or faster than usual, leading to a sensation of palpitations or a racing heart.
Dr. Hedgepeth continues, “Recent exercise and fever are common causes. Patients who might be dehydrated for any reason will often describe these types of symptoms.”
- Fill up on more water and less of the energy drinks.
- Cut back on caffeine; replace the diet pills with portion control and more exercise. Then see what happens.
Something of note: If you feel your heart beating in your chest, this doesn’t necessarily mean you’re feeling palpitations or PVCs, which are an irregular heart rhythm.
In fact, the beating may be quite steady and even-paced while you feel it in your chest.
In other words, you have no fluttering, but instead, just that strong awareness or sensation of a beating heart. The resting rate may even be normal during these experiences, too.
The more anxious you get over feeling your heartbeat in your chest — remember, the more this will make you “feel” it.
If your cardiac awareness, though, comes with other features such as lightheadedness, dizziness or chest pain, you should see a cardiologist.
 Dr. Hedgepeth also serves as a physician in the cardiovascular division and arrhythmia service at Brigham and Women’s Hospital, plus is an instructor of medicine at Harvard Medical School.
Dr. Hedgepeth also serves as a physician in the cardiovascular division and arrhythmia service at Brigham and Women’s Hospital, plus is an instructor of medicine at Harvard Medical School.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Theerapol Pongkangsananan
Pain in Chest when Leaning Forward & Backward

A cardiologist explains the possible causes of chest pain when you lean forward and backward.
“Pain in the chest with leaning forward or backward is a symptom commonly associated with pericarditis,” says Chester M. Hedgepeth, III, MD, PhD, Executive Chief of Cardiology at Care New England.
“Pericarditis is an inflammation of the thin, protective membrane that surrounds the heart, and keeps it in its proper anatomic location. Inflammation of this membrane may cause chest pain.”
Dr. Hedgepeth says that “the inflammation in the lining around the heart could be related to a recent heart attack.
“Heart attacks can lead to an immune response that causes inflammation in the pericardial sac.
“You may hear your doctor refer to this type of post-heart attack pericarditis as Dressler’s syndrome.”
What if you haven’t had a heart attack yet are experiencing chest pain or discomfort (or a dull ache) when you lean forward and backward?
There are many possible non-cardiac causes.
“More commonly, this inflammation [periocarditis] is related to infection (virus, rheumatic fever or tuberculosis), cancers (lung, breast, renal cell cancer, Hodgkin’s disease and lymphoma), immune diseases such as lupus, recent radiation therapy to the chest area, or certain drugs,” explains Dr. Hedgepeth.
“Recent chest wall trauma, musculoskeletal injury and herpes zoster should all be ruled out.”
How is periocarditis diagnosed?
If you have pain in your chest when you lean forward and back, there can be many possible causes — linked to pericarditis.
The workup for a correct diagnosis is as follows.
1 Medical History and Symptoms Review: The diagnostic process begins with a detailed discussion of your medical history and symptoms.
The physician will ask about recent illnesses, autoimmune disorders or trauma.
2 Physical Examination: During the physical exam, the doctor will listen to your heart with a stethoscope.
A key finding in pericarditis is the pericardial friction rub — a distinctive, scratchy sound produced by the rubbing of the inflamed pericardial layers.
3 Electrocardiogram (ECG): An ECG records the heart’s electrical activity and may show changes typical of pericarditis.
4 Chest X-ray: A chest X-ray helps visualize the heart’s size and shape and can show the fluid accumulation around the heart.
5 Echocardiogram (Echo): This ultrasound test provides images of the heart and can detect the fluid and assess the thickness of the pericardium.
6 Blood Tests: These tests check for markers of inflammation and identify potential underlying causes, such as infection or autoimmune diseases.
7 Pericardiocentesis: If there is significant fluid accumulation, this procedure may be performed to remove and analyze the fluid, helping to diagnose the cause of the inflammation.
In some cases, CT scans or MRIs may be used for further evaluation.
Bottom line: Chest pain that comes when you lean forward and/or backward should never be ignored. Make an appointment with your doctor.
 Dr. Hedgepeth also serves as a physician in the cardiovascular division and arrhythmia service at Brigham and Women’s Hospital, plus is an instructor of medicine at Harvard Medical School.
Dr. Hedgepeth also serves as a physician in the cardiovascular division and arrhythmia service at Brigham and Women’s Hospital, plus is an instructor of medicine at Harvard Medical School.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Chayatorn Laorattanavech
When Bed Elevation Won’t Prevent Acid Reflux
“My bed is elevated and I STILL get acid reflux overnight! Help!”
Does that describe you?
Overnight acid reflux can cause upper abdominal and/or chest discomfort, a bad taste in the mouth and coughing.
A person may even cough in their sleep — keeping their partner from a good night’s sleep.
“Acid reflux is when the normal stomach acid regurgitates up into the esophagus,” notes Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with of New York Gastroenterology Associates.
“The muscles at the bottom of the esophagus are meant to act as a valve to hold down acid, but in many people,” continues Dr. Desai, “this valve does not function properly.
“When people lie down at night, gravity is no longer helping keep the acid down in the stomach, so there is often worsening symptoms in this position.
“Frequently patients have just eaten dinner, and the food creates pressure which forces acid into the esophagus.
“Raising your head in bed is a good way to help gravity minimize this process.”
When Raising the “Bed” Won’t Help Acid Reflux
“One reason this doesn’t work in some patients is because they just elevate their neck and head (with pillows),” says Dr. Desai.
“For this technique to work, the whole chest needs to be elevated, usually with the help of a bed wedge device.”
So forget the pillows. The esophageal sphincter is in your stomach, not your neck.
The bed wedge devices create an elevation of six to eight inches, and unlike regular pillows or cushions, will not lose their shape or form over time.
Below is a common type of wedge pillow which elevates the torso and will help keep the acid contents in the stomach from refluxing. And below that is a type that’s designed for side sleepers.



Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Photographee.eu
My 600 Pound Life: Pauline Is Another Penny

Penny from “My 600 Pound Life” now has a twin sister, Pauline, who’s in denial and refuses to take responsibility.
An episode of “My 600 Pound Life” in 2015 was viewers’ first exposure to Pauline, a 51-year-old who weighed about 670 when she first saw Dr. Nowzaradan. She has a 21-year-old son, Dillon, who enables her.
Dillon’s pilot light, if he ever had one, is out. He’s obese, apparently has no goals and takes care of his mother full-time.
In Dr. Now’s office, it appeared that Dr. Now was about to point out that Dillon was an enabler after he asked Pauline, “Who gets you your food?” when Pauline interjected and said that her son is not to blame because he listens to the authority of his mother.
At that point, I thought, “What’s Dillon afraid of if he refuses to get her all the food—that she’ll leap out of bed and chase after him?”
Pauline is able to walk but for only a few steps. She and Dillon moved to Houston for the surgery, and she tried to lose 30 pounds prior to surgery at Dr. Now’s instruction.
She kept saying how difficult everything was because she and her son were out of their element.
I think I’m madder at Dillon than at Pauline because he provided absolutely no motivation or inspiration.
This lost young man could have purchased a pair of light dumbbells for Pauline to do upper body exercise throughout the day.
He could have purchased some books and magazines, a crossword puzzle book, anything. Instead they were shown zoning out in front of the TV.
Doesn’t Pauline know how to use a computer?
Why didn’t Dillon have her spend some time on his?
All of these activities would have made it easier for her to stay on a diet.
Pauline gained weight, so Dr. Now admitted her to the hospital where she lost 44 pounds in two weeks.
Pauline Is Another Penny
By the time she was discharged from a lengthy hospital stay following surgery, she had lost about 135 pounds.
In the ensuing months, Pauline continued to lose weight, but only a few pounds per month. Unlike Penny, she was losing, BUT…her attitude was very similar to Penny’s.
Pauline refused the physical therapy, though she was shown wading in a pool on her own.
It never occurred to her pathetic son to get her signed up with a gym to do some upper body workouts.
Dillon continued to bring his mother enough food to prevent her from losing more than a few pounds per month: That’s obviously a ton of food to near-maintain 530 pounds.
Like Penny, Pauline kept making excuses: She gets dizzy when she walks; she’s afraid of falling if she walks for too long.
I wondered why Dr. Now didn’t intercept at that point and say, “Then don’t walk far from your house. Instead walk inside your house back and forth from one end of a room to another.”
I also wondered why Dr. Now didn’t arrange for some mental therapy. I saw nothing in Pauline’s childhood, as it was described, to explain how she got way over 600 pounds.
Pauline really pulled a Penny towards the end when, after leaving the doctor’s office, she said she was offended by the way he kept pushing her too hard, after he had busted her for her lie about the phone calls from physical therapy.
She went as far as proclaiming that she knew her body better than Dr. Now did. And she said more than once that she had to do this at HER pace.
At Pauline’s pace, it will be YEARS before she gets down to a healthy weight, losing only a few pounds a month. She doesn’t have years. At 51, she may have only months to get the whip cracking.
“My 600 Pound Life” – Another Penny
As long as her voiceless son keeps enabling her, Pauline will be another Penny.
The last scene of this original episode showed them at a bingo hall, with Pauline announcing something like, “At least I’m getting out and doing things.”
Yeah, right, playing bingo and feasting on junk food there will help you lose weight.
Final Thoughts on “My 600 Pound Life”: Pauline
She’s in total denial, thinks Dr. Now is too pushy and doesn’t understand her, refuses physical therapy, refuses to work on her walking (Dr. Now kindly admonished her at month 12 for using a motorized wheelchair for her final weigh-in), cries tears but won’t take responsibility, and has a deadbeat, enabling son with no goals.
Update on Pauline
The July 3, 2019 airing of “My 600 Pound Life” reveals that Pauline lost enough weight to get skin removal surgery for her stomach, having gotten down to around 242 pounds at her lowest.
Then she started gaining again, though agreed to home physical therapy to regain the ability to walk.
Often having a good dose of attitude, Pauline ultimately gained back around 60 pounds, disqualifying herself for any additional skin removals for at least six months from that point forward.
Nevertheless, she was able to walk, without any assistance, to what would be her last weigh-in.
Pauline decided to quit the program, announcing that she knew what she had to do and “didn’t need this anymore,” referring to Dr. Now’s program.
However, it’s clear that she’s now headed in the wrong direction: more weight gain to come.
That 60 pounds will very likely soon be 100 pounds and she’ll be back in a wheelchair.
Second Update

As of the April 29, 2020 airing of “Where are they now?” on “My 600 Pound Life,” Pauline’s massive legs got the best of her and she decided to get back on Dr. Now’s program.
She lost enough weight to qualify for skin/lymphedema removal surgery on her left leg.
Several weeks later she qualified for a second surgery on her right leg, bringing her postop weight down to 208, with a total weight loss of around 500 pounds.
Pauline reported that her son Dillon no longer needed to drive her around, and she was last filmed sitting up front in an aircraft (whether she was sightseeing or taking flight instruction was not clear).
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
How to Elevate Sofa 9 Inches to Prevent Acid Reflux

If you sleep on a sofa, here’s a safe, easy way to elevate it 9 inches to help prevent acid reflux overnight.
I sleep on a sofa (not a pull-out sofa, but the actual sofa). This is because my back doesn’t like mattresses.
I’m also not the type of sleeper who thrashes around all night, and thus, the confined space of the sofa poses no problem whatsoever.
One morning, I’d had it with the acid reflux, so I wondered how to elevate the sofa on my head side. I had some large loose bricks outside, so I put one under each “leg” of the sofa, elevating it six inches.
I was leery because I kept thinking that I might turn a little overnight and throw the sofa off balance. It did wobble somewhat when I got into it.
However, I still got the acid reflux, so I decided to elevate the sofa three more inches by placing blocks of wood (purchased at Home Depot) on top of the bricks. This made the sofa even more unstable, in that it shook when I got into it.
I also worried that in the middle of the night, one of the legs would slip off the wood block. So I decided to place my 12-inch exercise stool under the sofa, smack between the elevated legs.
It fit nearly perfectly, with just a little bit of space to spare. I now knew that should the sofa leg ever slip off a block, the sofa wasn’t going anywhere, as the stool would support it.

Though the stool is 12 inches off the ground, the net elevation is nine inches due to the leg nubs being about three inches.
In other words, the bottom of the legs is nine inches from the floor.
The exercise stool is the type commonly seeing at gyms and health clubs, either with a red base or black base, and black surface.
These stools are sold online and are extremely durable, able to support a heavy sofa.
Incidentally, after all this time, the legs have never slipped off the blocks of wood.
I need to say, however, that lifting the sofa up in the first place, to set the bricks in place, requires a degree of strength.
If you don’t have much upper body strength, you’ll need to have someone help you.
Nevertheless, this is an easy way, at least from a logistical sense, to elevate a sofa nine inches to prevent acid reflux.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
.
Top image: Shutterstock/Agenturfotografin
Sensation of Pill Stuck in Throat But No Pills Swallowed
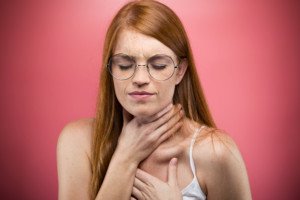
A GI doctor tells why you may feel that pills are stuck in your throat when you didn’t even swallow any.
Ever have that sensation that you can only describe as, “It feels like a few pills are stuck in my throat, but I didn’t even swallow any pills or tablets or anything like that today — not even yesterday!”?
“The sensation of something being stuck in your throat, when nothing is actually there, and you haven’t swallowed something recently is called the globus sensation,” says Jay Desai, MD.
Dr. Desai specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
“The cause of this sensation is poorly understood, but could be the sign of an underlying disease, such as acid reflux disease, a motor disease of the muscles of the esophagus, or a post-nasal drip.”
If you have a motor (motility) disease of the esophageal muscles, you’ll also experience difficulty passing food through the esophagus.
This article strictly relates to the feeling that something like a pill is stuck in your throat — and you do not have any other associated symptoms such as trouble swallowing or difficulty with food going down the esophagus.
Dr. Desai continues, “The typical way of treating this [globus] is first with an antacid medication or antihistamine, and if the symptom doesn’t improve, using a camera to look in the esophagus.”
This “pill stuck” feeling in your throat can also be caused by anxiety.
There was the case of a middle-aged man who had so much health anxiety that one day, upon reading about symptoms of laryngeal cancer, he began feeling a lump in his throat.
There was the case of a middle-aged woman (these fears can also strike younger adults) who thought she tasted blood one morning every time she swallowed.
So she kept swallowing at a more frequent rate to “test” to see if the taste of what she thought was blood was still there.
All day long she was swallowing more often than usual, and because many of the swallowings were deliberate, they were tense rather than relaxed.
As the day wore on she developed globus — a distinct feeling of a little food stuck in the throat.

If you have the feeling of a pill (or food) stuck in your throat, even if it comes only when you swallow, you may also want to re-evaluate your recent anxiety levels.
Anxiety can unconsciously (or consciously, as in the above case) affect how you swallow.
Eagle’s syndrome is another possible cause of this annoying symptom.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Josep Suria
Why Acid Reflux Can Cause Pepper Taste in Mouth

Have you been experiencing a peppery taste in your mouth, particularly upon awakening in the morning or even in the middle of the night?
Where is this coming from if you haven’t been eating peppers or anything with pepper in it?
“Acid reflux is when the normal low pH secretions in the stomach are pushed up into the esophagus,” explains Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
“Sometimes these fluids can regurgitate as high as into the mouth.
“Because of the low pH of these secretions, they have distinct tastes, such as metallic or pepper.”
Ironically, the pepper spice can cause acid reflux in some people.
Pepper, especially the black variety, can actually trigger the production of stomach acid.
Spicy foods such as pepper can also cause the lower esophageal sphincter to relax too much.
This is the valve that separates the esophagus from the stomach. If the LES relaxes or doesn’t close properly, it can allow stomach acid to escape into the esophagus — and still higher into the mouth, causing that metallic or peppery taste.
Sometimes the taste to some individuals is like cardboard or vomitus. It’s always a bad taste, no matter how it’s described.
If you’re finding that this peppery taste in your mouth occurs only when you awaken in the morning (or in the middle of the night), then see if you can elevate the bed so that your torso is elevated.
This non-horizontal position will help keep the stomach’s acid juices from making their way up into your throat and mouth.
Elevating your torso allows gravity to prevent the acid from traveling into your esophagus and higher.
Elevating only your head will not work. The actual bed needs to be elevated.
Another option is a wedge that you can lie your back on.
You’ll need to arrange some pillows so that your head is comfortable unless your head is actually on the wedge. Another option is to place a small pillow on the wedge.

Source: medcline.com
If you sleep on a sofa (not sofa bed, but actual sofa), it should be fairly easy to elevate the end of the sofa where your head lies.
If six inches doesn’t work, try nine or 10. Sometimes you just need a higher elevation to get gravity working.
Elevation is a very effective way to relieve acid reflux that occurs overnight, including that which causes a pepper taste in the mouth.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Exercise-Induced Acid Reflux Cause LPR?

LPR can make it difficult to breathe, but can acid reflux from exercise cause this scary situation?
“Acid reflux is when normal stomach acid regurgitates into the esophagus and causes symptoms,” says Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
“During exercise, this can be exacerbated, especially if you are significantly bearing down on the abdomen (such as in weightlifting, doing crunches, etc.).
“This pressure pushes on the stomach and can cause more acid to be pushed into the esophagus.
“If the acid goes high enough it can irritate the vocal cords. This is called laryngopharyngeal reflux (LPR), and can be diagnosed by an ear, nose, and throat doctor by looking at the vocal cords with a small camera.
“When the vocal cords get irritated by acid, you can develop symptoms of coughing or a hoarse voice.
“Treating the underlying reflux with antacid medication may help these symptoms.”
LPR is often misdiagnosed as exercise-induced asthma when it occurs during or shortly after exercise.
This is especially true if the exercise is of an aerobic nature. The symptoms of laryngopharyngeal reflux disease and asthma are similar enough that this misdiagnosis isn’t all that uncommon.
However, LPR will not respond to the asthma inhaler: “intractable asthma.” If this describes your situation, it’s advisable that you see an ear, nose and throat doctor (otolaryngologist).
LPR involves the vocal cords and can lead to difficulty breathing, whether it’s caused by acid reflux or an extraneous irritant.
Other symptoms of laryngopharyngeal reflux disease include a hoarse voice, persistent cough, bad taste in the mouth/throat and a sensation of a lump in the throat.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/MikeSaran
Acid Reflux Comes and Goes: Causes
What can make acid reflux come and go if the patient avoids food triggers?
“Acid reflux is when the normal stomach acid regurgitates up into the esophagus,” says Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
Dr. Desai continues: “In most people it improves and worsens periodically. For example, in periods of severe stress, symptoms of reflux can worsen substantially.
“Acid reflux can also vary in relation to changes in sleep habits, so it is important to try to identify what exacerbates symptoms in each individual patient, and to try to avoid this.
“In some patients, when this is not possible, treating with medical therapy is required.”
If your acid reflux comes and goes with seemingly no rhyme or reason, then it’s time to keep a documentation of it.
• For example, does it seem to come more often when you’re sleeping over your significant other’s house?
• Does it seem to arise only when your in-laws visit?
• How about on the same days you have business meetings?
• Does the fluctuating nature of your acid reflux occurrence seem correlated to when you eat — either the time itself, or perhaps the amount of food, or even the type of food?
• What about exercie? Does it seem to “come” during or right after exercie, and then go away once you’ve been rested for a while?
• Make sure everything even remotely relevant goes into this documentation; do not skip a day. In fact, make note of the days when you’re free of acid reflux symptoms
• Over time, you may begin to see a pattern develop to your acid reflux.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Where to Get the Instruction Manual for Raising Children

But kids DO come with instruction manuals!
Why do we keep hearing “Children don’t come with instruction manuals,” especially in this day and age of online parent communities, tons of websites and blogs about how to raise kids, not to mention all the books published in the past 30 years about childcare?
The irony is that the motto, “Kids don’t come with instructions,” sometimes appears on parenting sites and forums—which give instructions on how to raise kids!
Of all the topics in the world, parenting is probably in the top three when it comes to the availability of instructions, directions, help and advice.
Go to a large newsstand and count how many parenting magazines are on display.
Information on How to Raise Children Is Everywhere

Shutterstock/Just dance
The information will vary from source to source, but the point is that the information is overwhelmingly available.
It’s there at the touch of a mouse, not to mention the following:
- Community in-person support groups
- Free classes at social service agencies, hospitals and recreational centers
Between the Internet, books and magazines, the volume of parenting instructions is simply staggering.
In fact, the wealth of information is so enormous that there are magazines and books on very specific situations, such as publications strictly for newborns, few-months old, under one year, preschooler, gifted, ADHD and many more.
There are parenting magazines that cater to single moms, those who work outside the home, those who have a military spouse, daughters only, party planning, identical twins and much more.
Books on parenting are a sizzling goldmine for “instructions.” There are books on:
- Divorce
- Tough love
- Logical love
- Lenient love
- Bullying
- Raising kids without corporal punishment
- Death/loss
- Only children
- Adopted kids
- Biracial kids
- Life skills
- Sibling relationships
- Talking about sex
- Getting kids to listen
- How to raise “explosive” children
- How to raise boys
- How not to scream at your children
- How to raise caring kids without religion
- How to raise kids with sensory processing disorder
- Autism
There’s even an entire book on how to calm a crying baby (“The Happiest Baby on the Block” by Harvey Karp) and an entire book devoted to how to keep a child occupied while waiting in long lines or during lengthy car rides (“Fun on the run!” by Cynthia L. Copeland).
The only place where there are no instructions on how to raise kids is the moon!
You Need a License to Fish and Cut Hair, but Not Raise Kids
“There is no mandated training to become a parent, no license that you have to obtain,” says Dr. Tia Kern-Butler, a licensed psychologist for over 20 years who treats a broad range of issues including relationship problems and behavioral issues of children and adolescents.
“So I think when this [the instructions mantra] is said, it’s to validate for parents that parenting is the hardest job there is — and one that we are the least prepared to actually take on.
“It’s a phrase that I think was meant to make it safe for parents to admit that it’s okay not to have all the answers.
“While I do agree that there is an abundance of resources for parents to access, the key is for parents to feel comfortable enough to seek these resources without the parent guilt and shame.”
Get the Instructions if You’re a Struggling Parent
What’s really unfortunate is when a flustered parent will state, “Kids don’t come with an instruction manual,” but then refuses to reach out to the massive treasure troves of help, advice and direction – including other parents on the block or at school.
Even a childless person may have some wisdom to share. Sometimes, a solution comes from creative problem solving skills rather than the firsthand experience of raising kids.
Stop kidding yourself that there are no instruction manuals for raising healthy and well-adjusted children. The resources are insanely abundant.
 Currently in private practice Dr. Kern-Butler spent 10 years as the lead child and adolescent psychologist with Winter Haven Hospital and served as the mental health liaison for the Children’s Advocacy Center for 14 years.
Currently in private practice Dr. Kern-Butler spent 10 years as the lead child and adolescent psychologist with Winter Haven Hospital and served as the mental health liaison for the Children’s Advocacy Center for 14 years.
Professionalpsychologyofpinellas.com/about-me
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.