How Much Does an Adult Sunburn Raise Risk of Melanoma?

You’ve heard that severe childhood sunburns raise melanoma risk, but what if you had no childhood sunburns, but got them as an adult?
Don’t think for a moment that the absence of a sunburn during your childhood means you don’t have to worry about melanoma.
Sunburns in Adulthood Count
“It has been commonly taught that 50 percent of sun damage occurs before the age of 18,” says Dr. Joel Schlessinger, MD, a dermatologist with a private practice in Omaha, NE.
“Dermatologists are changing their thought processes on this, however, as the abundance and availability of indoor tanning has increased.”
More and more adults are getting socked with unnatural (tanning booths) doses of ultraviolet radiation.
And let’s not forget the strong doses of sunlight from tropical vacations.
“For this reason, it is likely that sun exposure risks not only continue, but increase, as individuals age,” says Dr. Schlessinger.
“Sunburns are a sign of lack of protection and major damage to the skin. Melanomas are clearly linked to the numbers of sunburns that an individual has over a lifetime.”
The risk of melanoma from sunburns, then, does not stop when one turns 18.

Dr. Schlessinger continues, “Furthermore, sun adds up over the years and magnifies damage as well. With thinning skin as we age, individuals have less protection for their skin as they grow older.
“Many people are able to spend more money on tanning sessions as they age, which further damages their skin.
“Also, sun damage mounts over time, eventually reaching a crescendo where even small amounts of sun exposure or tanning bed exposure can cause significant and irreparable harm.”
The thing with sun exposure is that the damage isn’t instant, like the damage from a car accident.
This suppresses an adult’s awareness and insight into just how damaging cumulative sun exposure and sunburns are.
“Sun exposure doesn’t cause skin cancer right away, which unfortunately leads to people going back to the sun or tanning beds and thinking they ‘got away’ with the sessions/exposures before,” explains Dr. Schlessinger.
“This couldn’t be further from the truth. What actually happens is that they end up waiting about 20 years before the damage is evident.
“Twenty years is a long time, and during the years leading up to finding out what the initial sun exposure damage will cause, they are usually causing further damage!”
This is scary news, because for many adults, what ultimately happens is that they start developing a slew of precancerous lesions and even cancerous lesions (not necessarily melanoma). By then it’s too late to stop this cascade of recurring lesions.
“Additionally, any interventions to stop exposure will result in minimal benefits until another 20 years has passed,” says Dr. Schlessinger.
The solution is to just avoid tanning booths and unprotected sun exposure. Always wear sunblock.
Try to avoid being in the sun between 10 a.m. and 4 p.m.
Otherwise, use that sunblock and reapply every 2-3 hours, and more frequently if you’re swimming, says Dr. Schlessinger.
There are clothing lines with built-in sunscreen.
Sunburns in adulthood contribute to melanoma risk, and there is no way around this fact.
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Chondroitin and Glucosamine Be Taken with Antidepressants?

Is it safe to take glucosamine and chondroitin with antidepressants?
Are you taking an antidepressant and would like to also take chondroitin or glucosamine?
There are certain compounds that should not be taken with antidepressants — for instance, narcotic painkillers, which can suppress the therapeutic effects of an antidepressant.
But what about chondroitin and glucosamine with antidepressants? Can taking chondroitin or glucosamine with an antidepressant create problems?
I wondered about this, and asked Joe Wegmann, psychopharmacologist and licensed clinical social worker, author of Psychopharmacology: Straight Talk on Mental Health Medications.
Wegmann explains: “Chondroitin occurs naturally in the body and is a major component of cartilage — connective tissue that cushions the joints.
“Some scientific studies suggest chondroitin may be effective for osteoarthritis, but others have not shown any positive effects associated with its use.
“I cannot find any contraindications associated with taking chondroitin in conjunction with antidepressants, so I would say the combination is fine.”
What about glucosamine with antidepressants? Wegmann says: “Same as for chondroitin; taking antidepressants in combination with glucosamine is fine, no reported contraindications.”
So if you’re on a medication such as Cymbalta, Effexor, Lexapro, Zoloft, Pristiq, Paxil or Prozac, it’s perfectly okay to take chondroitin or glucosamine; neither will suppress the actions of selective serotonin/norepinephrine reuptake inhibitor (SS/NRI) drugs.
In fact, if you’re thinking of taking narcotic painkillers while on an SS/NRI, beware:
Narcotics suppress, or depress, the central nervous system; that’s how they numb pain.
Examples of narcotics are Vicodin, Norco, Darvocet, Percocet and codeine.
Since narcotics depress the central nervous system, they will “fight” against your antidepressant.
It’s quite possible that a narcotic painkiller can pretty much cancel out the effect of an SS/NRI, and/or the SS/NRI can cancel out the pain-numbing effect of a narcotic.
Another point to consider:
A possible side effect to narcotics is depression and anxiety. Of course, read the insert to your SS/NRI medication, because depression and anxiety can also be side effects of antidepressants.
However, it’s very possible to experience no side effects from a drug like Cymbalta, Effexor and Pristiq, and yet suffer miserable side effects from the use of a prescription narcotic, which can include depression and even mental confusion.
If you are having joint pain while being treated for depression, consider first taking chondroitin, glucosamine or aspirin/ibuprofen, since these will not interact with antidepressants.
Sometimes these work for pain, and sometimes they don’t, but there’s only one way to find out. Another effective treatment for joint pain is structured exercise.
 Joseph Wegmann is a licensed clinical pharmacist and clinical social worker with more than 30 years of experience in the field of psychopharmacology.
Joseph Wegmann is a licensed clinical pharmacist and clinical social worker with more than 30 years of experience in the field of psychopharmacology.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Do Sleeping Pills Prevent Awakening from Pain?

So will that sleeping pill keep you from waking up with pain?
If you have pain, be it from a knee injury, back injury, tendonitis in the shoulder, carpal tunnel syndrome or a pinched nerve in the neck, taking a sleeping pill will not prevent the pain from awakening you.
It’s amazing how many people will take sleeping pills, thinking that these drugs will keep pain from waking them up.
This is not what sleeping pills are designed for.
Here is what a doctor says: “Be aware that sleep aids generally do not work for sleep that is disrupted by pain,” says Joseph J. Ruane, DO, a sports medicine specialist with OhioHealth Physician Group.
In order for a sleeping pill to induce a slumber strong enough to be impenetrable from pain, the drug would essentially have to be a powerful painkiller — which it is not.
Ambien and Lunesta are frequently advertised on TV as sleep aids, not painkillers. And over-the-counter sleep drugs will be just as useless as far as enabling a person to sleep through pain.
Dr. Ruane continues: “People think sleep is sleep and a sleeping pill should help you sleep if you’re having any sort of trouble.
“Over-the-counter medicines such as Tylenol PM or even prescription medicine made to help people sleep will generally not help if pain is the problem.
“Most of the time, the body ignores sleep aids and the pain will still wake you, so don’t be disappointed.”
The mechanism by which sleeping pills assist in slumber is not the same mechanism by which, for example, narcotics like Percocet, or anti-inflammatories like ibuprofen, work.
It’s two completely different pathways. Pain will barge right through the sedative properties of a sleeping pill and awaken you.
If you are free of pain and are having trouble falling asleep due to stress, poor eating habits or outdoor noise, then a sleeping pill can aid in making you drowsy enough to eventually fall asleep and stay that way.
But if you have a recurring pain problem in, say, your hands from carpal tunnel syndrome, or migraine headaches, then that pain will override the sleeping pill – easily, and wake you up outright.
 Dr. Ruane’s practice is dedicated to comprehensive, nonsurgical musculoskeletal care. He is active in clinical research and is a nationally recognized speaker and educator.
Dr. Ruane’s practice is dedicated to comprehensive, nonsurgical musculoskeletal care. He is active in clinical research and is a nationally recognized speaker and educator.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/fizkes
Cymbalta Fights Depression Caused by Narcotic Painkillers

Cymbalta is an antidepressant that can be used to treat depression caused by narcotic painkillers such as Norco/Vicodin, Percocet, OxyContin, codeine, etc.
Yes, narcotic painkillers can cause serious depression as a side effect. This side effect, if disabling enough, can be treated with Cymbalta, an SNRI antidepressant that also has an on-label use as a painkiller; namely for nerve discomfort.
I asked questions about Cymbalta for depression caused by narcotics to Jacob Teitelbaum, MD, medical director of the Fibromyalgia and Fatigue Centers nationally, and author of “From Fatigued to Fantastic!”
Fibromyalgia is a nerve pain disorder that causes pain throughout the entire body, and one of Cymbalta’s on-label uses is for treating the discomfort of fibromyalgia.
Suppose a person has been taking narcotics for pain and develops clinical depression as a side effect.
What do you think of taking Cymbalta (or any SNRI type of drug), to fight this depression?
This is a two-pronged question, because on one hand, the person might continue taking the painkillers, and on the other hand, the person might stop the narcotics but the depression lingers, so in essence, they transition from painkillers to Cymbalta to mop up the depression.
And in that last scenario, at what point might they quit the Cymbalta (via tapering) with the idea that the narcotic depression is long gone from their system?
Dr. Teitelbaum: “Very reasonable to add Cymbalta to the narcotic to help BOTH the pain and depression. I would likely, when both pain and depression are controlled, consider slowly tapering off the narcotic — but would be okay with continuing both as long as needed.
“I would note that I would be treating the underlying causes of the pain using “SHINE” —
Sleep,
Hormonal support,
Infections/Inflammation/Impingement,
Nutritional support, and
Exercise as able.
“Remember, pain is your body’s way of saying that something needs attention, like the oil light on your car’s dashboard. Add oil and the oil light goes out.
“Treat with SHINE, and the pain often goes away. Other treatments can be tailored to the specific type of pain as well (e.g., vitamin B6, thyroid and wrist splints for carpal tunnel syndrome).
“Six months into pain being relieved, it is reasonable to taper down the dose of pain meds if pain relief persists.”
If you’ve been incapacitated by depression that seems to have developed at about the same time you began taking narcotics, there’s a real possibility that this mood dysfunction was caused by the painkiller itself; or, the mood disorder may have been pre-existing in a milder form, and then intensified from narcotics use.
Taking Cymbalta in conjunction with your prescription painkillers to combat this secondary depression is something to strongly consider.
If you decide to ask for a Cymbalta (or other SNRI drug) prescription, your doctor needs to know that you believe your depression is being caused or aggravated by your narcotics use.
The narcotic induced depression may also be caused by B vitamin or testosterone deficiency caused by the narcotics, and these deficiencies can be easily treated.
Dr. Teitelbaum is a board certified internist and nationally known expert in the fields of fibromyalgia, chronic fatigue syndrome, sleep and pain.
is a board certified internist and nationally known expert in the fields of fibromyalgia, chronic fatigue syndrome, sleep and pain.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Can Celiac Gene Raise Cancer Risk if You Don’t Have Celiac Disease?

Celiac disease specialist, Dr. Stefano Guandalini, addresses the cancer issue.
You may know that having celiac disease increases your risk of developing intestinal cancer.
This is because as celiac disease progresses, the damage to the inner lining of the small intestine progresses, making it more vulnerable to cancer.
I wondered, however, if merely having the gene(s) for celiac disease could somehow raise the risk of cancer.
The gene(s) for celiac disease has been identified, and if you do not have the gene, you cannot get CD.
However, having the gene does not guarantee you will develop this illness, either, which is when the body mounts an ongoing immune response to the consumption of gluten-containing foods.
So does having the celiac gene, in and of itself, predispose a person to a higher risk of cancer?
“It does not appear that this is the case; there is in fact no evidence that intestinal malignancies occur more frequently in people with only the gene(s),” says Stefano Guandalini, MD, Founder and Medical Director, The University of Chicago Celiac Disease Center.
Mayoclinic.com states: People with celiac disease who don’t maintain a gluten-free diet also have a greater chance of getting one of several forms of cancer, including intestinal lymphoma and bowel cancer.
Suppose you find out that you have the genetic predisposition to CD, but you are not experiencing symptoms of this disorder, which include digestive disturbances such as diarrhea; joint pain; mouth sores; muscle cramps; tingling in the feet and legs; anemia; unexplained weight loss; nausea/vomiting; constipation; chronic diarrhea; brain fog; fatigue and grayish stools. Should you go gluten-free?
Most people with celiac disease do not have symptoms, so if you have the gene(s) for this condition, yet feel perfectly fine, the illness may still be in full swing. And in that case, you do have a heightened risk for certain cancers.
If you have the gene for celiac disease yet no symptoms, it would not be practical, at that point, to eliminate gluten-containing foods.
After all, only about 5 percent of people with the gene actually develop CD.
“First-degree relatives of those with biopsy-diagnosed celiac disease who have the genetic predisposition are a high-risk group that should be screened every three years or immediately upon symptoms,” says Dr. Guandalini.
An antibody blood test called transglutaminase is used for screening. But in rare cases, this test can be negative in someone who has the illness.
The gold standard for diagnosis is an endoscopic biopsy of the small intestine.
You will need to discuss your options with a gastroenterologist, especially if family members have celiac disease.
 Dr. Guandalini is an internationally recognized expert on celiac disease, Professor Emeritus, University of Chicago, and the founder of the University of Chicago Celiac Disease Center. His clinical and research efforts have greatly influenced how celiac disease is diagnosed and treated today.
Dr. Guandalini is an internationally recognized expert on celiac disease, Professor Emeritus, University of Chicago, and the founder of the University of Chicago Celiac Disease Center. His clinical and research efforts have greatly influenced how celiac disease is diagnosed and treated today.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/KongNoi.
Sources: mayoclinic.com/health/celiac-disease/DS00319/DSECTION=complications; mayoclinic.com/health/celiac-disease/DS00319/DSECTION=symptoms
Sjogren’s Syndrome: How Common Are Memory Problems?

How many people with Sjogren’s syndrome suffer memory problems?
Sjogren’s syndrome indeed can cause memory problems, even though this autoimmune condition is associated with dry mouth and dry eyes.
Because Sjogren’s (pronounced show-grens) syndrome is potentially systemic, the entire body can be affected, including organs, and this can mean the brain.
“Patients with Sjogren’s syndrome may suffer from a number of different neurologic abnormalities,” says Ali D. Askari, MD, Professor of Medicine – Case Western Reserve University; Chief, Division of Rheumatology – University Hospitals Case Medical Center; Director, Rheumatology – University Hospitals Case Medical Center.
Rheumatologists often deal with Sjogren’s syndrome patients, since the disease often initially manifests with joint pain or stiffness.
Dr. Askari continues, “Unlike lupus (another autoimmune disorder which can affect the joints), which has more of central nervous system involvement, Sjogren’s syndrome has peripheral nerve involvement more commonly.”
Neurological problems affect as many as 20 percent of patients. However, Dr. Askari says that dementia is a rare complication of Sjogren’s syndrome.
“In our own study reported to the international SS conference in Japan, we found 14 of 200 patients having neurological abnormality.
“Six had variety of central nervous system involvement; only one had dementia. Dementia therefore is rare and can happen at any time.”
Though Sjogren’s syndrome is most associated with dry eyes and dry mouth, these aren’t necessarily the first presenting symptoms.
The very first symptom may be dementia, though, again, it’s a rare complication.
Dr. Askari continues, “The abnormalities of the central nervous system include abnormal MRI without any abnormal serologic findings, but also brain abnormalities such as shrinking of the brain and dementia.”
It’s possible for a person diagnosed with Alzheimer’s disease, which is terminal, to actually have Sjogren’s syndrome, which is not terminal if treated and managed.
“Although this is difficult to differentiate from Alzheimer’s disease, neurologists believe that the cerebrospinal fluid contains a specific protein found mainly in Alzheimer’s.
“This protein is called Tau which is not found in Sjogren’s syndrome and dementia.
“Fogginess and slight memory loss can happen in both systemic lupus and Sjogren’s syndrome, and may respond to anti-inflammatory medicines; if not it may be associated with permanent brain changes.”
Dr. Askari adds, “The peripheral nerve involvement as mentioned is more commonly associated with Sjogren’s syndrome and that includes peripheral neuropathy or injury to the nerve fibers of the lower or upper extremities.
“In particular pure sensory neuropathy, meaning that just lack of sensation found by nerve conduction tests (EMG), is specific for Sjogren’s syndrome.”
High doses of corticosteroids and other immunosuppressant drugs, when administered early in the course of these symptoms, can bring on improvement.
If you’re suffering from what seems to be neurological or memory impairment, request tests for SS.
Dr. Askari explains, “It is prudent to consider Sjogren’s syndrome in the differential diagnosis of neurologic abnormalities and particularly abnormal findings on MRI of the brain or spinal cord, or peripheral neuropathy.”
Update: As of April 2024, Sjogren’s syndrome is now known as Sjogren’s disease.
Dr. Askari’s special interests include diseases of the muscles, fibromyalgia, general rheumatology, lupus and Sjögren’s syndrome.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Shutterstock/Vadim Zakharishchev
Does Sjogren’s Syndrome Shorten Life Span?

How much does Sjogren’s syndrome affect life span?
Sjogren’s syndrome may bring to mind simply that of chronic dry mouth and dry eyes, which don’t sound too serious.
Many people with Sjogren’s syndrome suffer only from dry mouth and dry eyes, and often experience joint pain.
However, some patients with Sjogren’s (pronounced show-grens) suffer more serious complications of this autoimmune disorder, which affects about two to four million Americans, with 90 percent of patients being female (for reasons not known).
Since Sjogren’s syndrome often affects joints, specialists in this disease are usually rheumatologists.
“Rheumatic diseases by in large cause pain and stiffness and don’t impose death threats,” says Ali D. Askari, MD, Professor of Medicine – Case Western Reserve University; Chief, Division of Rheumatology – University Hospitals Case Medical Center; Director, Rheumatology – University Hospitals Case Medical Center.
“In general, inflammatory states such as rheumatoid and lupus lead to more coronary artery disease and short life span.
“In Sjogren’s syndrome this matter is not settled (not well-studied), and the disease in general is benign but annoying, and people have their regular life expectancy. By-and-large patients without complications live a normal life.”
However, living with just dry mouth and dry eyes can be arduous.
The reduced saliva flow predisposes a patient to:
- a high risk of dental decay
- bad breath
- chapped lips
- and a burning sensation in the lips, tongue and throat, not to mention difficulty swallowing food that necessitates sipping water before every mouthful of food.
Dr. Askari continues, “The development of lymphoma (cancer) occurs in less than 5 percent of patients having SS in which the life expectancy shortens.
“The undesired complications with Sjogren’s syndrome include a renal condition referred to as renal tubular acidosis in which more kidney stones are formed.
“Kidney failure, however, is rare and is due to inflammation of the cortex of the kidney, unlike lupus in which this complication is more frequent.”
Lupus is also an autoimmune disease that can affect the entire body.
“Patients with Sjogren’s syndrome could have lung inflammation with cough and shortness of breath which could affect life span expectancy.
“The most important rare complication in Sjogren’s syndrome is the inflammatory changes of the vessel walls, or vasculitis, which leads to the presence of a rash on the skin, and inflammatory changes within the different organ systems such as the kidneys, lungs and brain.
“In each complication mentioned, however, there are sufficient treatments available, which are effective and control the complications.”
Update: As of April 2024, Sjogren’s syndrome is now known as Sjogren’s disease.
Dr. Askari’s special interests include diseases of the muscles, fibromyalgia, general rheumatology, lupus and Sjögren’s syndrome.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: ©Lorra Garrick
The Youngest a Child Can Get Melanoma Skin Cancer?
How young is too young for a child to get melanoma?
Children CAN develop melanoma — the deadliest type of tumor that can arise from a type of skin cell known as the melanocyte: a pigment producing cell.
“There is no age that is too young to develop melanoma as a child,” says Dr. Joel Schlessinger, MD, a dermatologist with a private practice in Omaha, NE.
“In my practice I have seen melanoma in many young patients and have one 17-year-old who nearly needed to have an amputation due to melanoma of the toe.”
What’s with the increase in melanoma cases in younger and younger people, including children?
This seems to contradict our evolutionary biology; after all, ancient man spent hours every day smack in the sun, before umbrellas, tents, wide-brimmed hats and sunglasses were invented.
Researchers point to the intermittency of sun exposure as a risk factor for melanoma.
Intermittent blasts of sun exposure shock the DNA and damage it, causing changes that can, over time, give rise to melanoma.
Dr. Schlessinger continues, “Sadly, we are now seeing a huge spike in melanoma cases due to indoor tanning and the trend of tanning before proms, weddings and all other events.
“Additionally, damage to the skin as well as moles is being done on a daily basis when going to tanning booths.”
Tanning booths are not safer than the sun; in fact, their dose of radiation is much more concentrated, which is why you can get burned in just five minutes.
“Moles often go through a process whereby they change from innocent moles to more concerning moles over time,” says Dr. Schlessinger.
“Eventually, many moles become what is called ‘dysplastic’ or unusual under the microscope and to the eye.
“These moles can ultimately end up turning into melanoma, but they don’t have as great a chance if the skin is protected.”
There is a strong correlation between childhood protection from the sun, and low incidence of melanoma later in adulthood, as well as during childhood.
Next time you’re tempted to encourage your pasty-faced child to “get more sun,” think of “get some color in your skin” as synonymous with “get some melanoma in your skin.”
Moles that are present since birth are more likely to develop melanoma, says Dr. Schlessinger.
If your child has congenital (since birth) moles, this doesn’t mean they all must be removed.
However, the parent should keep a close watch on these moles in their child for any signs of melanoma.
Don’t obsess and live your life in fear, though. Just make sure you know your child’s moles, and have a dermatologist evaluate them once every year or two.
“Dermatologists frequently encounter moles that are ‘on the fence’ and at that time may choose to either carefully observe them or remove them,” continues Dr. Schlessinger.
“There are some moles that are both congenital and quite large that simply can’t be removed.
“These are frequently the ones that are the most concerning of all and need to be evaluated on a yearly basis.
“Dermatologists may look at parts of them by biopsy or perform a small incision to test them.
“Additionally, there are tools to magnify the mole without having to do a biopsy, known as dermoscopy.
“Many dermatologists have these tools and can perform an initial evaluation of the mole using this technology.”
All in all, melanoma is still very rare in children, but this rarity is no consolation to parents who find out that their child has melanoma, especially when the disease was caught later, rather than sooner, when it was much more treatable, even curable.
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Andrey_Popov
Are Teens Really at Risk for Skin Cancer from Tanning Beds?

Teens who use tanning beds increase their risk of deadly melanoma skin cancer risk.
More and more teens are using tanning beds, such as in about a million visits daily in the U.S.
Using a tanning bed before age 35 increases risk of melanoma skin cancer by up to 75 percent, says a study reported in the March 2007 International Journal of Cancer.
Does your teen use a tanning bed?
The most significant known risk factor for this cancer is the unprotected exposure of the skin to ultraviolet light – essentially the modus operandi of a tanning bed,” says George Hollenberg, MD, a dermatopathology specialist in Plainview, NY, and former medical director of Acupath Laboratories.
Melanoma rates in the U.S. continue to rise, relative to the increasing population, and these increased rates have particularly occurred in children and young adults.
Dr. Hollenberg says, “Melanoma diagnoses are increasing at a rate of 3 percent each year for children ages 10-19, and more rapidly for young women in their 20s and 30s.” Melanoma is the leading cause of death for women 25-29.
And here’s more frightening news, from the American Academy of Dermatology: The Academy predicts that by 2025, melanoma may be the # 1 cause of cancer death for Americans. Even naturally dark people can get melanoma.
As a responsible parent, you certainly care about your teen’s teeth; his or her posture; and perhaps you’ve ordered your kids to eat their vegetables. Why not include melanoma awareness in your parenting program?
Over two dozen states actually restrict access by teenagers to tanning salons.
This restriction ranges from the requirement that teens have parental consent to use the tanning bed, to absolute prohibition of teens using tanning facilities.
It’s tough to make a stubborn teen start wearing sunblock for the very first time in his or her life.
But don’t let that stop you from enforcing its use. If your kids are very young, you have a far better chance of ingraining the sunblock habit into them.
Every so often, I see very young children with sunburns. This is inexcusable.
According to the Centers for Disease Control, only one in seven high school students reported using sunblock rated at least SPF 15.
You make your children brush their teeth every morning and every night before bed. Well, every morning make them put on sunblock, or, put it on them yourself.
If you require your kids to do yard work, send them out before 10 a.m. or after 3 p.m.
Yes, you need to get serious about this, because the National Cancer Institute says that melanoma is one of the fastest-spreading cancers.
How familiar are you with the moles on your kids’ or teens’ skin?
How familiar are THEY with them? I have two young nephews and a niece who are full of moles.
All three are dark from spending huge amounts of time in the sun without sunblock. Having over 100 moles is a significant risk factor for melanoma.
My 14-year-old nephew has a ton of moles on his bronzed back, and he’ll undoubtedly acquire more before age 20.
Your teens should be familiar with their moles, so that if one ever starts changing, they will know it.
Melanoma can also arise from non-mole areas of the skin. If you find a suspicious growth on your child or teen’s skin, don’t wait:
Take him or her to a dermatologist and insist on a biopsy.
Dr. Hollenberg passed away in 2013.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Melanoma Sentinel Lymph Node Biopsy Technique Eliminates Second Surgery
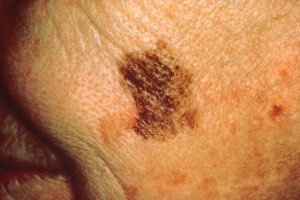
A second surgery for sentinel lymph node removal, if you’ve just been diagnosed with melanoma, may not be necessary, if your doctor knows about the MCW Melanoma Cocktail.
As a new skin cancer patient, you may already know that a sentinel lymph node biopsy might be in order, to see if any melanoma cells are in nearby lymph nodes.
Key to five-year melanoma survival rate is the ability to detect metastasis in a fast, accurate manner.
The quicker that melanoma is “staged,” the sooner doctors know precisely what the treatment protocol is.
Acupath Laboratories has a technology that eliminates the need for a second surgery for newly diagnosed melanoma patients.
Not only is a second surgery eliminated, but the technology eliminates the 1-2 days’ anxiety that the patient must suffer awaiting results of the sentinel lymph node biopsy.
Depending on how “deep” the tumor is in the skin, the biopsy will be required.
The routine protocol for this consists of the initial surgery to remove the melanoma tumor, and then a biopsy of the sentinel lymph nodes is taken.
However, it takes 24-48 hours for the results of the sentinel lymph node biopsy to come back. During that time, the patient must endure anxiety.
Furthermore, if the biopsy of the sentinel lymph nodes comes back positive for melanoma cells, the patient must then return to the doctor for additional surgery, to remove the surrounding nodes.
With Acupath’s MCW Melanoma Cocktail, it can be determined, right then and there during the first surgery, if the sentinel lymph nodes test positive for cancer cells.
The MCW Melanoma Cocktail was developed by researchers at the University of Wisconsin.
- The MCW Melanoma Cocktail mixes together several antibodies that can detect cancerous cells in the sentinel lymph nodes.
- The surgeon takes tissue from the patient’s sentinel lymph nodes, during the first surgery to remove the malignant spot.
- The tissue is placed on slides; and the antibody mixture is applied to this tissue on the slides.
Because the mixture can detect cancer cells within 30 minutes, any need to remove the sentinel lymph nodes for additional study can be done right there, during the very same surgery.
“Surgeons and pathologists can now determine in the operating room during a patient’s first surgery whether the sentinel nodes show sign of metastasis,” says George Hollenberg, MD, a dermatopathology specialist in Plainview, NY, and former medical director of Acupath Laboratories.
“If so, the remaining nodes can be removed during that same surgical procedure, eliminating the second invasive surgery entirely.”
If surgery is planned to remove a spot that you think might be skin cancer, ask your surgeon if he or she knows about the MCW Melanoma Cocktail for on-the-spot sentinel lymph node biopsy results during the first surgery.













































