Is Burping a Symptom of IBS?
A GI physician addresses the question of burping being caused by irritable bowel syndrome.
- Have you been diagnosed with IBS?
- Do you find that you’ve been burping a lot more lately and it seems to be related to your IBS?
It probably is.
“Burping is a not-uncommon symptom in patients with functional gastrointestinal disorders,” says Michael Blume, MD, a gastroenterologist at MedStar Good Samaritan Hospital, Baltimore.
“It is usually related to problems with the way your stomach empties. We all swallow air, and usually passes through the GI tract and comes out the way air normally comes out.
“In situations where your stomach does not empty normally, air does not travel the way it normally does; your stomach may get distended, and since it cannot travel and be expelled from below, it comes out from above.”
And hence, you burp.
IBS is a functional disorder of the gastrointestinal tract, and to date, no cause has been defined.
This disorder involves symptoms without detectable structural abnormalities or chemical deviations.
This is why it’s a diagnosis of exclusion, which means the patient must undergo a colonoscopy, among many other tests, before getting a truly valid diagnosis of IBS.
Despite extensive research, no single definitive cause has been identified.
Instead, IBS is believed to result from a combination of factors, such as gut-brain communication issues, changes in gut motility, sensitivity, microbiome imbalances and even mental stress.
 In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Vladimir Gjorgiev
Can IBS Cause Joint Pain? Are There Solutions?

Find out what may actually be going on if you’re having joint pains and have been diagnosed with IBS.
“IBS as a rule does not directly cause joint pains, such as with Crohn’s disease or ulcerative colitis,” says Michael Blume, MD, a gastroenterologist at MedStar Good Samaritan Hospital, Baltimore.
“If they do occur they may be from an unrelated issue or may indicate that there may be some other issue going on.”
First off, IBS is not an inflammatory bowel disease. It’s not an autoimmune disease, either.
In fact, irritable bowel syndrome is actually a collection of symptoms.
If you’re having joint aches or “pain” that seem to correlate with your IBS attacks or episodes … it’s possible that these joint aches are connected to your gastrointestinal problem — but this would have to mean that you’ve been misdiagnosed as having IBS!
As mentioned, Crohn’s and ulcerative colitis can cause joint aches or pain. Both these conditions are inflammatory bowel diseases.
However…it’s not likely that Crohn’s or ulcerative colitis will be misdiagnosed as IBS.
There’s another inflammatory bowel disease, that can cause joint aches, that is often misdiagnosed as IBS: microscopic colitis.
There’s symptom overlap. However, the diagnosis for microscopic colitis can be made with 100 percent conclusion: a biopsy of a tissue sample taken from the colon during a colonoscopy.
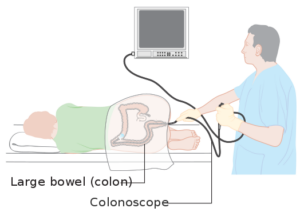
Colonoscopy. Cancer Research UK
The problem is that sometimes, the diagnosis of irritable bowel syndrome is made when there’s been no colonoscopy.
This misdiagnosis is far more likely to occur in a younger person, since GI symptoms in young people aren’t as alarming as they are in those over 40 and especially 50.
When I had my first flare-up of microscopic colitis…as I was being prepped for my colonoscopy…the nurse wasted no time telling me that the diarrhea could be from IBS.
- People with non-retractable IBS may actually have microscopic colitis.
- The treatment for IBS will not work on microscopic colitis.
Microscopic colitis causes joint aches in a small percentage of those diagnosed. I’m one of them.
The joint aches are identical to those that women get with PMS. (Search this site for more information on the joint aches of microscopic colitis, also referred to as enteropathic arthropathy).
If you’ve been diagnosed with IBS, have not had a colonoscopy, and have joint aches that your doctor has said are not rheumatic, you should have a colonoscopy to see if you have microscopic colitis.
And by the way, the joint aches or enteropathic arthropathy from microscopic colitis are benign and transient.
Let them run their annoying course and you’ll soon be back at rock climbing, CrossFit, trail running, power lifting, or whatever your physical passion is.
The joint aches are caused by hormones called prostaglandins, not any degeneration in the joint itself.
 In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/fizkes
Can IBS Cause Hot Flashes?

If IBS causes hot flashes, how on earth does this occur?
IBS stands for irritable bowel syndrome. It is common. So are hot flashes.
Can hot flashes be caused by irritable bowel syndrome?
Yes, says Michael Blume, MD, a gastroenterologist at MedStar Good Samaritan Hospital, Baltimore.
“This is not uncommon at all. Many people with IBS attacks feel flushed, warm, clammy and can feel as if they have to pass out.
“This has to do with the nervous system supply to your gastrointestinal tract.
“Part of what governs the function of your GI tract is related to your autonomic nervous system, that part of your nervous system that works without your thinking about it.
“One part of this system is called your parasympathetic nervous system, most notably your vagus nerve, and in many patients with IBS, this often becomes very active.
“When it does, it may give the sensation of hot flashes, as well as the other symptoms mentioned above.
“Many patients with IBS feel that they may be running a fever when it often just is related to a feeling of warmth and clamminess one sees with this phenomenon.
“Most people actually running a fever usually feel cold, and may have chills, rather than feeling warm.”
This sensation of cold is largely due to how your body’s thermostat, the hypothalamus, responds to illness or infection.
Also during a fever your body may reduce blood flow to the skin and extremities to keep heat concentrated in the core of your body.
This narrowing of blood vessels near the skin’s surface helps increase your internal temperature, but can leave your extremities feeling cold.
If you can’t tell if you’re having a hot flash or if you might have a fever, you can take your temperature with an instrument — that you can get at a drugstore or online — that very quickly yields your temperature.
It’s also possible that you can be having a hot flash and a fever at the same time, with each situation having different and unrelated causes.
Unlike a fever, though, a menopausal or postmenopausal hot flash may be preceded by a brief migraine or a strange feeling of offness, anxiety or depression that subsides as the body begins feeling hot.
At any rate, IBS can definitely generate a hot flash.
But if you’re going through menopause or have been having true postmenopausal hot flashes, irritable bowel syndrome is likely not the cause of any of these episodes.
 In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/YAKOBCHUK VIACHESLAV
Can Chest Pain Be Caused by IBS?

Is it possible to tell the difference between IBS chest pain and that caused by a heart problem?
Having chest pain, especially in the middle of the night, is scary as heck. It makes a lot of people wonder if they’re having a heart attack.
“IBS is a disorder that can affect the entire gastrointestinal tract, including the esophagus,” says Michael Blume, MD, a gastroenterologist at MedStar Good Samaritan Hospital, Baltimore.
“If there is spasm or abnormal function in the esophagus, one can complain of chest pain, trouble swallowing, belching or other symptoms.”
The esophagus is behind the sternum (breastbone), so if your IBS involves esophageal spasms…you will feel discomfort or pain sub-sternally.
However, this is the same location that cardiac-related pain can manifest.
An esophageal spasm can be painful and sudden.
The chest pain from this can mimic the sensation of a heart attack.
These spasms occur when the muscles in the esophagus contract abnormally or irregularly, disrupting the normal movement of food toward the stomach.
The pain may even radiate to the back or arms.
You can’t assume that your chest pain is from IBS or not, or a cardiac problem or not, until you undergo thorough medical testing.
“Keep in mind that it is very important to exclude other causes of chest pain, including most notably, cardiac causes, prior to attributing a symptom to IBS,” says Dr. Blume.
“Sometime one can make that determination clinically, but often it may require diagnostic testing to make sure that there is nothing more serious causing this symptom.”
IBS Chest Pain vs. Cardiac Chest Pain
Is it possible for a person to experience episodes of chest pain that are sometimes from IBS and…sometimes from a cardiac problem like angina? Yes! Why not?
There’s no reason why someone can’t just by chance happen to suffer from both a gastroenterological condition and a cardiac condition.
So even if your troubling chest pain has been determined to be IBS, it would be a very smart move to undergo a thorough exam by a cardiologist — just to be as sure as possible.
 In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Monster e
Amitriptyline for IBS: Pros & Cons

A GI doctor discusses the effectiveness of amitriptyline for IBS, how it works and possible drawbacks.
Amitriptyline and Irritable Bowel Syndrome
“Amitriptyline is a very common drug used to treat IBS, and can be very effective,” says Michael Blume, MD, a gastroenterologist at MedStar Good Samaritan Hospital, Baltimore.
He says that amitriptyline is usually taken at bedtime and in low doses.
“If you do get prescribed this drug, be aware that it has been used as an antidepressant (as well as for other symptoms, such as migraines, etc.), so the package insert may state that it is an antidepressant drug.
“Do not be alarmed; this is a different use of the drug, and in usually in a much lower dosage than what was used for depression.”
For IBS, amitriptyline works in multiple ways, says Dr. Blume.

Amitriptyline
“It is a very good gastrointestinal analgesic, and it also may decrease spasm in your GI tract, which may help your symptoms.
“Like any drug, there is no drug that does not have side effects, so when one makes a decision to take any medication, one needs to weigh benefits and risks, i.e., what the risk is of taking the drug vs. the risks of not taking the drug.”
Side Effects of Amitriptyline
“The more common side effects include drowsiness, as well as possible palpitations,” says Dr. Blume.
“It should be used with caution in older people and should be avoided in patients with cardiac rhythm problems.”
Remember, IBS is a diagnosis of exclusion, meaning, you should have a colonoscopy (among other important tests) before you’re definitively diagnosed with IBS.
If you’ve been diagnosed with IBS, but it has not responded to treatment, and you have not had a colonoscopy, it’s possible that you actually have microscopic colitis.
The treatment for microscopic colitis is very different than it is for IBS, and that means no amitriptyline.
 In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
In practice for 25+ years, Dr. Blume treats over 65 conditions including abdominal pain, appetite loss, blood in stool, celiac disease, colon cancer, esophageal and liver disease, gas and IBS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Dragana Gordic
Do Pacemakers Prevent Atrial Fibrillation?

Do you have a pacemaker and are wondering if it can also prevent atrial fibrillation?
A-fib is a common heart rhythm disorder that puts a person at considerably increased risk of a blood clot — which could lead to a heart attack or a stroke.
“Pacemakers do not prevent atrial fibrillation, or at least that is not an accepted clinical indication for implantation of a pacemaker,” says Lawrence Kanner, MD, Director, Electrophysiology/Arrhythmia Services, South Nassau Communities Hospital.
He further explains, “Pacemakers are devices that prevent slow heart rhythms. They will allow the heart to go as fast as it wants.
“If your heart wants to go 200 beats a minute (either top or bottom chamber — atrium or ventricle), a pacemaker for the most part just watches.
“But a pacemaker will never let the heart go slower than its programmed lower rate.
“However, modern pacemakers will detect episodes of atrial fibrillation, as long as there is a lead (wire) in the atrium.”
Thus, don’t ever assume that somebody can’t possibly experience an episode of atrial fibrillation just because they have a pacemaker.
A doctor who suspects that a patient has an abnormal heart rhythm will want that patient to wear a portable EKG.
With this portable EKG, every time the patient feels a suspicious symptom (such as a sudden pounding in the chest), they press a button and the device will record the electrical activity of their heart at that moment.
This data is then eventually printed out and interpreted by a cardiologist.
More on Atrial Fibrillation
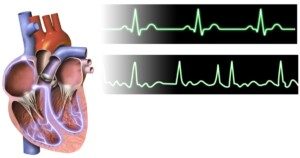
A-fib. BruceBlaus
The patient may feel what they describe as palpitations: an erratic heartbeat, or the sensation of the heart “flip flopping.”
The patient may also report a reduced capacity for exercise, or an unexplained fatigue.
Feeling lightheaded or dizzy are two more symptoms of atrial fibrillation.
This heart rhythm disorder can also cause pain in the chest.
These symptoms have many other possible causes, and not always heart related.
Atrial fibrillation is a risk factor for ischemic stroke, so if you’re having any of these symptoms — see a cardiologist.
Dr. Kanner cares for patients with a variety of cardiac rhythm disorders plus congestive heart failure, with medications, pacemakers, defibrillators and the latest in advanced cardiac ablation techniques.
cares for patients with a variety of cardiac rhythm disorders plus congestive heart failure, with medications, pacemakers, defibrillators and the latest in advanced cardiac ablation techniques.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Steven Fruitsmaak
TIAs: Why Aren’t More Family Doctors Vigilant on Follow-ups?

Why don’t more doctors take seriously a transient ischemic attack (TIA)?
A TIA (transient ischemic attack) is very serious – it’s your body’s way of warning you that a stroke may be imminent.
A suspected TIA should be treated as an emergency — because it’s a harbinger of a stroke in the near future for many TIA patients.
Among other permanent disabilities, a stroke can cause paralysis on one side of the body.
Amazingly, it is not all that uncommon for a person to report to his general doctor recent symptoms that sound very suspiciously like a transient ischemic attack.
The doctor sends the patient home with no treatment plan, and instead, tells the patient that he’ll get back to him after consulting with a neurologist.
So what’s this patient supposed to do in the meantime to minimize another TIA or even stroke? Cross his fingers?
Seems to me that if a patient reports TIA like symptoms to a doctor, and the doctor suspects a transient ischemic attack, this doctor should be hopping on the case, immediately putting in an order for a brain, heart and carotid artery scan to explore confirming evidence and location of the transient ischemic attack.
But some physicians won’t get hopping like this.
Instead, they make the patient wait until the physician has heard back from the neurologist. There is alarming laxity here.
“This speaks to the systemic flaw that pervades all healthcare: more attention to the acute problem rather than addressing or preventing the underlying cause,” explains William R. Davis, MD, cardiologist and author of “Wheat Belly.”
So what’s behind a TIA, then?
“The underlying cause is usually atherosclerosis,” says Dr. Davis.
“The standard response to atherosclerosis of the carotid artery, for instance, is aspirin, other platelet-blocking drugs like Plavix, and cholesterol reducing drugs.
However, there are plenty of other strategies that can be pursued that can substantially reduce or eliminate the risk of future TIAs.”
Symptoms of a transient ischemic attack are pretty much identical to symptoms of a stroke.
In fact, another name for TIA or transient ischemic attack is “mini-stroke.”
A TIA is a temporary obstruction of a blood vessel in the brain, formed by either a clot of blood, or plaque debris originating from the carotid or aortic artery.
TIA symptoms: sudden onset of numbness, weakness, heaviness or paralysis on one side of the body; loss of balance; cognitive change or confusion; double or blurred vision, or the sensation of a curtain coming over the eye or blindness; dizziness; headache; slurred speech or difficulty talking.
If you suspect you just had a transient ischemic attack, head straight to the ER. The risk of stroke following a TIA is greatest within three days of the TIA.

Dr. Davis is founder of the Track Your Plaque program for heart disease prevention and reversal.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: ©Lorra Garrick
Do Migraine Headaches Increase Alzheimer’s Risk?
Migraine headache sufferers may be fearful that this condition raises Alzheimer’s disease risk, because migraine headaches are associated with a higher incidence of small lesions within the brain that are picked up by MRI.
Interestingly, according to a study involving 780 people over the age of 65, having repetitive and significant headaches, or migraines, does not increase the risk of this disease.
In fact, migraines were shown not even to increase the odds of cognitive decline (cognitive decline doesn’t necessarily mean Alzheimer’s or eventual Alzheimer’s).
This research conclusion comes from Inserm and Université Pierre et Marie Curie, Paris.
It is a fact that in people with a migraine headache history, more of these people, when compared to the general population, have lesions in the microvessels of their brains.
However, such lesions are a universal finding in the elderly population.
The severity, though, varies quite a bit from one person to the next, and they are more severe among people with a history of migraine headaches.
Do you suffer from headaches?
“As an Alzheimer’s specialist, I can say that I have never seen any relationship between headaches or head pain and the development of Alzheimer’s,” says Dr. Robert Williams, MD is a family medicine doctor and geriatrician in Lakewood, Colorado and is a medical advisor for eMediHealth.
Dr. Williams explains, “One should be more concerned about a sedentary lifestyle, smoking, obesity and social seclusion.
“For the most part, activities that increase the risk for heart disease and hypertension also increase the risk for dementia.
“One type of dementia is specifically due to having multiple small strokes over a lifetime which is typically due to poorly controlled cardiovascular disease.”
Lower the Risk of Alzheimer’s
- Stop smoking or don’t start.
- Lose weight if you have excess body fat.
- Limit drinking.
- Maintain a normal blood pressure.
- Avoid excess dietary sodium.
- Work out regularly.
- Limit processed foods.
- Get annual heart checkups after age 50.
- Keep intellectually active.
Based in Lakewood, CO, Dr. Williams has been in practice for over 19 years. In addition to Alzheimer’s disease, Dr. Williams’ areas of expertise include neurology, pulmonology and autoimmune disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Source: sciencedaily.com/releases/2011/01/110119120400.htm
Can Daily Aspirin Cause Chronic Subdural Hematoma in Elderly?

Since aspirin is a blood thinner, how likely could this drug trigger a chronic subdural hematoma in an older person who’se on a daily aspirin regimen?
The issue becomes mighty tricky when an elderly person must take aspirin every day, and at the same time, is at risk for chronic subdural hematoma.
Being elderly, in and of itself, is a risk factor for chronic subdural hematoma.
“As a blood thinner, daily aspirin use can increase the risk for subdural hematoma formation in the elderly,” says Kangmin Daniel Lee, MD, a neurosurgeon with New Jersey Brain and Spine.
“Commonly, chronic subdural hematomas start out as small acute subdural hematomas,” continues Dr. Lee.
“Over time, they become chronic.” They can also slowly bleed over time, versus the kind that a boxer or skier might suffer, in which the bleeding is rapid and deterioration comes quickly.
“As people age, brain atrophy occurs and brain volume decreases. Since the elderly are at increased risk for falls or other minor traumas, there is an increased risk that such traumas could tear a small bridging vein and result in a hemorrhage,” explains Dr. Lee.
Atrophy means shrinkage; the brain has a tendency to shrink as a person gets older.
Dr. Lee continues, “Because aspirin is such a common and often necessary medication for those with a history of stroke or cardiac disease ( i.e., a cardiac stent), the immediate or near immediate risk of a bad event such as a repeat stroke or stent occlusion will often outweigh the remote risk of a subdural hematoma.”
The reason aspirin increases risk of chronic subdural hematoma is because aspirin thins the blood; thin blood is more likely to bleed (less likely to clot).
Blood thinners are a godsend for people at risk for clotting disorders, which can be life-threatening if not treated promptly.
But to prevent clotting (i.e., stroke, heart attack, deep vein thrombosis), the risk then goes up for chronic subdural hematoma, which translates to slow, gradual formation of a mass of blood beneath the dura of the brain.
“I believe that the risk of subdural hematoma is probably under-emphasized with the elderly patient who takes aspirin, and should be more widely discussed.
“Certainly when a neurosurgeon sees an elderly patient who has been on aspirin and has developed a chronic subdural hematoma, there is a thorough discussion of the risk of a repeat hemorrhage.”
How true.
The possibility of chronic subdural hematoma was never mentioned to my elderly mother after it became clear to hospital staff that she was at risk for falling due to orthostatic hypotension; she was recovering from coronary bypass surgery and was on daily aspirin … and also on the king of blood thinners, Coumadin!
Six and a half weeks after surgery, she blacked out while standing in the bathroom, fell dead-weight and hit her head on the bathtub.
No symptoms…until six weeks later when she awakened with the worst headache she’d ever had, and compromised function of her legs.
Diagnosis in the ER later that day: chronic subdural hematoma!
“Also, chronic subdural hematomas can often go unrecognized, as patients can often be minimally symptomatic,” says Dr. Lee (who was not my mother’s neurosurgeon).
“With the general population living longer and getting more medical attention, the reported incidence of chronic subdural hematoma will likely increase, and greater scrutiny will likely be placed on the routine use of antiplatelet agents (like aspirin).”

Dr. Lee focuses on minimally invasive techniques to treat traumatic and degenerative diseases of the spine and brain tumors. He’s been invited to speak at the regional and national levels on his research areas.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Masha Petrakova
Spontaneous Subdural Hematoma in the Elderly: Incidence?

Chronic subdural hematoma can occur spontaneously and being elderly is perhaps the No. 1 risk factor for developing this condition.
It is not to be confused with acute subdural hematoma from a car accident, skiing accident or other significant blunt force trauma to the head.
My mother developed a chronic subdural hematoma as a result of striking her head on the bathtub after passing out while standing at the sink – from a drop in blood pressure.
Her neurosurgeon informed me that chronic subdural hematoma was “not uncommon in the elderly,” and that it can occur “spontaneously” due to weakened bridging veins, and brain atrophy.
If elderly people take daily aspirin or other anticoagulants, this increases risk even more.
So based on my conversation with my mother’s neurosurgeon, spontaneous chronic subdural hematoma in the elderly is far from a rare occurrence, and this made me wonder why there’s no media attention to this.
I never heard of this condition until my mother developed it, and I write medical articles for a living.
I receive Kaiser Permanente’s monthly magazine which highlights common conditions of the elderly (diabetes, heart disease, osteoporosis, osteoarthritis, dementia), but never have I seen anything on spontaneous (or otherwise) chronic subdural hematoma.
Kangmin Lee, MD, says that the occurrence rate of spontaneous subdural hematoma, compared to non-spontaneous causes such as getting hit in the head or heavy drinking, in the elderly is 30 percent.
This sounds like a lot.
“Thirty percent seems like it would be fairly common,” continues Dr. Lee, a neurosurgeon with New Jersey Brain and Spine.
“However, the overall incidence of chronic subdural hematoma in the entire population is approximately one to five per 100,000.
“So it would be 30 percent of that number (the one to five) that would fall into the spontaneous cSDH number.
“With respect to other medical issues such as heart disease and cancer — it is less common. However, as our elderly population continues to grow in number, we will likely see the incidence numbers start to rise.”
The elderly are particularly prone to falling, either due to weakened hip bones, general leg weakness, transient ischemic attacks, and miscellaneous factors such as orthostatic hypotension (plummets in blood pressure after standing from a seated position that can cause a blackout).
The elderly are also more likely to be on anticoagulant therapy, like my mother was (daily aspirin and Coumadin at the time she fell), after undergoing coronary bypass surgery (as did my mother).
And then there’s the age-related brain shrinkage.
Combine these factors, and it would not be accurate to say that chronic subdural hematoma is rare in the elderly population, but more accurate to say that spontaneous chronic subdural hematoma in the elderly (patient has no risk factors other than old age) isn’t particularly prevalent.

Dr. Lee focuses on minimally invasive techniques to treat traumatic and degenerative diseases of the spine and brain tumors. He’s been invited to speak at the regional and national levels on his research areas.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.