Cause of Muscle Twitching in Arms: Biceps & Triceps

A neurologist answers what could make the arms twitch and whether or not the twitching is a worrisome symptom.
Do your arms (namely biceps and triceps muscles) twitch?
“Many people experience annoying twitching of the arms that can be anxiety provoking if you don’t know why it is happening,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
I myself have had, more than once, a twitching episode in my triceps, and it was prominent.
The muscle twitching followed a training session involving triceps routines.

Freepik.com/jcomp
“Though it is true that muscle twitches can occur in anyone, those who work out at the gym and exercise their upper bodies with weight training are more prone to get them.
“Why? Because the biceps and triceps muscles do MOST of the work.”
Many routines consist of a lot of arm work.
Though I don’t endorse isolation exercises as the foundation for building strength and muscle, I have to say it’s a reality that many people at the gym focus on exercises that involve the arms only.
However, chest routines work the triceps, and back routines work the biceps.
Dr. Geraci continues, “As the muscle exercises, some muscle fibers become ‘injured’ and must repair themselves – hence the twitch.
“Remember, your body is a fantastic organism that will take care of itself, given the proper nutrition and rest.
“So, your body is on its own clock, and muscle twitches will occur randomly and intermittently. Nothing to worry about and totally normal.”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com/halayalex
Normal EMG Means NO ALS even with Neuro Symptoms
Finally, here’s the article that answers the question, “Can a person with ALS have a normal EMG?”
Does a normal EMG always mean no ALS?
Can a person have ALS and have a normal EMG?
What if the EMG is normal but you have symptoms like muscle twitching?
“There are three essential components for diagnosing ALS,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“First, one must have both subjective and objective weakness in muscles both below and above the waist.”
In other words, the neurologist must show, from HIS end, that your perceived weakness is actually clinical weakness.
No, he won’t have you try to lift a 45 pound water cooler bottle over your head. Instead he’ll have you, for instance, press your foot against his opposing hand.
“Second, a neurologist must observe certain findings on examination,” continues Dr. Geraci.
“Third, one must meet certain criteria on a test commonly referred to as an EMG.
“The full name of the test is EMG/NCV which stands for electromyography and nerve conduction velocity.
“EMG is the gold standard for diagnosing ALS, and results from this test can make the diagnosis very early in its course.”
Does a normal EMG mean you can’t have ALS?
Dr. Geraci says, “I use EMG in my office at least 15 times weekly, and about two to three times a month I see a patient who is concerned they may have ALS.
“After I examine them and do the EMG I can almost always give them the answer, and it is usually, ‘You can relax, you don’t have ALS!’”
Why do you say “almost always” and “usually”?
“I used the terms almost and usually because the reality is that rarely I do diagnose someone with ALS who comes in with fascics, but they usually have weakness and neurological findings.
Shutterstock/joshya
“Dozens, perhaps hundreds, of studies have documented the utility of EMG in diagnosing ALS.
“If a person has a normal EMG it is essentially impossible that they have ALS, but, the caveat would be that the person also would have a normal neuro exam (which is not just strength testing but also reflexes, and the discussion gets complicated so suffice it to say abnormal exam).
“It is an absolute that if a person has a normal EMG and normal neuro exam, they DON’T have ALS, period.
“If the EMG is completely normal in a patient with symptoms, ALS is effectively excluded and one would look for other diagnoses.”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Okrasyuk
Twitching Above Ears: Causes & Solutions by a Neurologist
Find out from a neurologist what causes twitching above the ears and what to do about this.
Are you experiencing twitching above your ears?
It may feel like a very tiny muscle moving involuntarily. Or, it may feel like a tiny blood vessel throbbing.
Either way, the sensation is not easy to ignore. So what’s going on?
“Some of the most annoying twitching can be those coming from the face and head,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“Yes, we have muscles on our heads! Most commonly, one may experience twitching of the muscles of the eyelids or even above the ears – the temporalis muscles.”
What causes this twitching (fasciculation) above the ears?
Dr. Geraci explains, “Both of these muscles have smaller than normal fibers, and the nerves to these muscles have to traverse ‘wild terrain’ as they course from inside our heads to the muscles on the outer portion of our skulls.
“So, the nerves can get irritated, and then the muscle fiber’s membrane becomes unstable and twitches.”
The situation, then, involves muscle fibers, not blood vessels, even though it may feel that way at times.
What can be done to subdue twitching above the ears?
“Substances such as caffeine can cause twitches also, so if you drink a lot of java, consider cutting back,” says Dr. Geraci.
“Otherwise, don’t let it worry you – I’ve never seen a patient with muscle twitches above the ears who had any medical problem to explain it!”
You may also want to ask yourself if you’ve been extra stressed or anxious lately.
Stress and anxiety may cause twitching of the muscles in the head or around the ears.
The stress/anxiety response can fire up the nervous system, increasing muscle tension and involuntary contractions (the “twitchies”), which may occur around the head or ears.
Heightened stress hormones and overactive nerves can cause these small muscle movements.
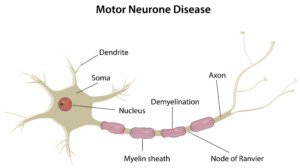
With all that said, you do not have to worry that you might have multiple sclerosis, Parkinson’s disease or any motor neuron affliction.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Muscle Twitches During Sleep that Aren’t Myoclonus Jerks

Find out about regular muscle twitching during sleep or shortly before, not the “jerks” of myoclonus…
This article is about regular muscle twitching as one falls asleep or during sleep, not the jerking movements that are termed myoclonus.
“A different sensation can occur during any sleep stage, but is most pronounced in some people as they first hit the pillow and start to fall asleep,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“I am referring to muscle twitches, or fasciculations. These can occur in any muscle but are most pronounced in the upper arms and calves. Generally they do not occur in the muscles of the back.
“Here’s the rub: We tend to notice twitches as we start to fall asleep because there is nothing in our environment to distract us.
“As we fall asleep, we are essentially going into a deep meditation and our thoughts are turned inward.
“This may cause us to over-interpret normal twitches of the muscles. Remember, our muscles are constantly repairing themselves from being used while awake, and during that process the muscle membrane can become unstable and contract.
“That’s it; ignore the twitching and let yourself slumber. Your muscles will do their thing and prepare for the next day of activity.”
I’ve had fascics upon awakening in the morning. It’s possible that the muscle was twitching while I was asleep.
There is nothing unique about slumber that would make typical twitching any more meaningful than fascics you experience while fully awake.
It’s just that for many people, sleep is mysterious, so any twitching right before or coming out of sleep tends to really grab one’s attention and lead to worrying.
Dr. Geraci adds, “If you think you are getting too many twitches, twitching of the back muscles or jerking movements that wake you from sleep, see your doctor or a neurologist.
“I see young and healthy patients with these symptoms on a weekly basis and invariably everything checks out fine!”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Cause of Twitching Muscles in Your Chest
A neurologist explains what’s going on when your chest muscle (pecs) keeps twitching.
Does your chest muscle keep twitching?
“For those of you who bench press and are bulking up, the major upper chest muscle that provides the strength for pushing up the weights is the pectoralis major,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“It would be very normal to feel a twitch in the chest, and many people feel that the twitch is deep and perhaps even under the pectoralis major,” continues Dr. Geraci.
“Well, there are only two muscles under the pectoralis major: the pectoralis minor and the intercostal muscles, neither of which contribute much to the power needed to bench press.
“The pectoralis minor rotates our upper arm, and the intercostals allow us to expand our chest when we inspire (breathe in).
“If you feel a twitch in your chest but don’t actually see it, that is because muscle twitches can occur anywhere in the muscle, and if they are in the deep part of the pectoralis major you probably won’t see it depending on the bulk of your muscle.
“Not to worry though, it is still just a benign fasciculation (twitch), and you can keep on pushing up that bar!”
What is the biochemical explanation for a twitch in the chest during or following exercise?

When a muscle cell is stimulated by exercise such as a chest press, several key chemical changes occur.
Calcium ions are released from the cell, enabling muscle contraction by facilitating the interaction between protein filaments in the cell.
Muscle cells use adenosine triphosphate (ATP) for energy, which is rapidly replenished through a chemical process.
This process produces lactic acid, which can lower the muscle’s pH and cause temporary fatigue or that all-too familiar “burn.”
One of the outcomes of this chain of events is “injury” to the cell membrane. (But it’s a good kind of injury because it trains the muscle to be stronger for the next chest day.)
This alteration in the muscle fiber’s “chemical soup” leads to random firing of nerves that contract the fiber: the twitching.
Think of this as your body’s built-in massager.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Visible Muscle Twitches: Why You Can See Them, What It Means
A neurologist explains why some muscle twitching is visible and if there’s a difference between ones you can see and hidden fasciculations.
Have you been wondering if being able to SEE a muscle twitching has a specific meaning, versus not being able to see the twitching that you can so easily feel?
“A trap you don’t want to fall into is excessive worry simply because you can see a muscle twitch,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“That just means that the twitch is near the surface, and the skin just above the muscle moves when the muscle fiber contracts,” says Dr. Geraci.
Translation: You probably have low body fat! This makes things more visible (e.g., veins in the forearms, “definition”).
Dr. Geraci continues, “These occur throughout the entire muscle in a random fashion and actually, you are having several-fold the number of twitches you actually see – you just aren’t aware of them!
“Seeing a muscle twitch rather than feeling one has no meaning at all and is no cause for concern.”
What about a visible twitch that’s like half a foot long?
I myself once had an elongated visible muscle twitch. After I did a set of pull-ups, a thumping fasciculation developed in my chest.
Though the chest is not a primary mover in a pull-up, it isometrically contracts during the movement.
At the gym, I could easily see the twitching in a mirror. It was a horizontal fascic about five inches long!
It was “flashing” beneath my chest muscle, right under the clavicle bone.
This visible muscle twitching persisted all day long and evening, but was completely gone come next morning.
It really is true: What you can see won’t hurt you.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Cause of Muscle Twitching in Quads from Lifting Weights
A neurologist explains exactly what makes the quad muscles twitch after a workout of squats, deads or whatever leg workouts you do.
You trashed your quads in the gym and now they’re twitching like mad; what’s going on here? Is this normal?
“Many people experience an annoying, random or rhythmic twitching of the large thigh muscles of the leg called the quadriceps,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“These twitches, also named fasciculations, can occur in many muscles throughout the body, and are particularly noticeable in some people after exercise.”
Dr. Geraci says that during exercise, “the muscle uses glucose and oxygen from the blood as its energy source.
“After a certain amount of time, say 20 minutes, the muscle must turn to other sources of energy as its requirements go up, but the fuel of available glucose goes down.
“This is when the muscle metabolizes fats in the body to use as fuel, leading to a buildup in the cell of lactic acid.”
What weightlifting enthusiast hasn’t heard of lactic acid?
Dr. Geraci continues, “As lactic acid builds up in the muscle, a chain of events takes place that temporarily ‘injures’ the muscle cell and destabilizes its cell membrane.
“Normally, the muscle membrane is kept stable by the single nerve fiber attached to it.
“However, if the chemical soup within the muscle is temporarily toxic to the membrane, it will set off an electrical impulse, referred to as depolarization. This is the basic process that leads to muscle fiber contraction.
“During the resting phase after exercise, the muscle cleanses itself of the lactic acid and other free radical metabolites (bad molecules that destabilize the membrane) and within time the twitches subside.”
So there’s your explanation for what causes your quads to twitch after lifting weights.
But what if the twitching persists long after your weightlifting session?
Dr. Geraci says that the twitching is a “manifestation of a destabilized muscle fiber membrane.
Remember, each muscle has tens of thousands of muscle fibers, so if a few have unstable membranes that contract and cause a twitch, there will be no consequence to strength or muscle health.”
So as long as next leg workout, you can get under that heavy barbell and squat as usual, or execute your typical deadlifts, leg presses or single-leg dumbbell step-ups, there is nothing to worry about.
Twitching, even in one specific group such as the quads, during or after lifting weights can also be caused by something you’re drinking before, during or after the workout that contains caffeine.
Dr. Geraci says that caffeine can cause twitching. Other causes are stress and many prescription drugs.
“The bottom line is that twitches, particularly in young persons who are active and exercising, are almost NEVER a sign of a serious neurological condition – just a sign that you are using you muscles the way they were meant to be used!”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Perceived Weakness vs. ALS Weakness: Telling the Difference
A neurologist explains in detail how to tell perceived weakness from ALS weakness.
Is there a way to tell the difference between perceived weakness and weakness from ALS?
“Imagine: You just completed your workout at the gym and you feel that you couldn’t bench press the amount you are accustomed to,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“You wonder about it and if you might be weak on that day; maybe you are just tired. This is perceived weakness, a very subjective measure of strength.
“It is very important to understand that the strength of our muscles varies due to a variety of variables on any particular day or time.”
Perceived weakness also often comes in the form of how a muscle group “feels” at rest.
A person may feel that the muscle group is weak and begin fearing ALS.

But the perception of weakness disappears the minute they must pick up heavy boxes from the garage.
But the perception of weakness disappears the minute they must pick up heavy boxes from the garage.
The minute they sit before the computer, they start perceiving weakness and fearing ALS.
Why the ALS fear? Because this is the channel that their mind gets tuned into.
“Perceived weakness is NOT true weakness,” says Dr. Geraci. A healthy person may feel a weakness in their leg when sitting before the TV.
The perceived weakness disappears when they find themselves dashing down the street after their dog.
Dr. Geraci explains, “True weakness can only be identified by two means: The first is by identifying the weakness in one limb or part of one limb that leads to functional impairment.
“In other words, a weak hand that drops objects and gives you trouble buttoning your shirt.”
In other words, clinical weakness is exhibited by having trouble doing simple things like blow-drying your hair or hanging up clothes, opening a car door or removing a pot roast from the oven, as opposed to bench pressing 195 pounds this week when last week you pressed 205.
“The second is by having a neurologist objectively determine weakness in a group of muscles,” continues Dr. Geraci.
“Weakness from ALS always is accompanied by atrophy of muscles, and objective findings that only a physician can identify.”
When worried people find this out, they become prone to inspecting the body part in question for signs of atrophy.
They decide on what atrophy must look like, that a “dent” in the calve must absolutely mean muscle atrophy.
This is the mind playing tricks!
We’ve all seen true muscle atrophy; anybody who uses a wheelchair exhibits noticeable atrophy in their legs.
Or, the person with one side of their body mobility-impaired (stroke, cerebral palsy) has very visible muscle atrophy on that side.
But back to perceived weakness…
“In the age of the Internet, it is very easy for people to have a twitch here and there, and a couple of days of bad workouts at the gym followed by an Internet search that spits out ALS as the answer to their symptoms,” says Dr. Geraci.
“My advice is this: First, ALS is very rare, and second, try turning the symptoms around and looking at them as a manifestation of the normal state of affairs in the body you are exercising.”
If you haven’t been exercising, apply this advice to household duties such as carrying the vacuum cleaner up the stairs, carrying children or running down the staircase.
“If you are worried about having ALS, consider the above and ask yourself which group you fit into and I’ll be willing to bet you’ll come to the most likely conclusion: You are just fine.”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer. \
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer. \
.
Top image: Shutterstock/Huntstock.com
Why the Room Gets Black & You Feel Dizzy when Standing Up
When you rise after sitting for a while, do you feel faint or like the room is blacking out?
This is called syncope or orthostatic hypotension.
“It is a result of a drop in blood pressure after standing,” says Robert M. Davidson, MD, a cardiologist with SignatureMD.
“It is particularly likely if your blood pressure is usually on the low side,” adds Dr. Davidson. My blood pressure is typically low, sometimes just under 100 over the low 60s or even high 50s.
Usually it comes in at something like 105 over 67. I sometimes experience that blacking out sensation after rising from being seated for a while.
“The easiest way to prevent it is to get up slowly, or to exercise your legs (pushing up on the floor) while sitting before standing,” says Dr. Davidson.
I’ve noticed that when I must quickly and unexpectedly rise from a chair to tend to something, there is no blacking out or faint feeling whatsoever. Getting up in transitory steps will prevent the problem.
Another way to prevent blacking out from standing is to, for 30 seconds: hold tightly clenched fists; or press the palms together tightly; or press the inner thighs together tightly. This will raise blood pressure.
My mother had a unique kind of orthostatic hypotension following a pacemaker implant.
The blacking out did not occur immediately after she rose from a seated position.
The event would start unfolding usually about a minute after she was up and about, sometimes a few minutes.
Not only that, but unlike typical orthostatic hypotension, once it started unfolding, it could not be reversed by simply sticking it out while standing still.
In other words, people who feel faint or like everything is blacking out, after rising, typically stand still and lean on something to let the experience run its course.
After several moments, everything clears up and they resume walking.
In my mother’s case, this didn’t happen. She’d lose consciousness. This was discovered before she had a chance to take a hard fall to the floor. So while she suffered from this problem, I had to shadow her to prevent the fall.
Since the orthostatic hypotension would not resolve while simply holding my mother up (she’d instead lose consciousness), I had to “sink” her (from behind) to the floor on her fanny.
A chair was not a viable option because her altered mentation (from the blood pressure drop’s diminished oxygen to her brain) rendered her incapable of “aiming” her butt into the chair, and her legs were usually stiffened up, which made it very cumbersome for me to steer her butt into the nearest chair.
So, wherever we were when the passing out began to take grip, I sunk her to the floor or ground (e.g., inside Walmart, outside on sidewalk).
Only when my mother was on the floor and I leaned her back against my arms and legs, would the orthostatic hypertension begin reversing.
As mentioned, the blood pressure drop impaired her reasoning, rendering her incapable of having the mental faculties to realize that she had to sit down as quickly as possible.
So she’d continue walking about, not realizing that as seconds passed, she was becoming increasingly clumsy, bumping into things, off-balance and losing her wits.
The doctors involved in her cardiac care had no solution to this and no explanations. Amazingly, the problem eventually cleared up spontaneously.
That all aside, if you experience blacking out or faintness soon after rising from a seated position, and it clears up while you wait it out, you have nothing to worry about.

Dr. Davidson is with the Division of Cardiology at Cedars-Sinai Medical Center, Los Angeles, and has been practicing for 35+ years. Areas of specialty include coronary artery disease, heart attack and palpitations.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can ALS Be Diagnosed with an EMG Test Alone?
Are you suffering from the agony of thinking you might have ALS, but have not had an EMG test?
When a doctor suspects that a patient might have ALS, the patient is told they should have an EMG done.
Many people who experience symptoms that make them think of amyotrophic lateral sclerosis wonder just how soon an EMG can detect this ruthless disease.
Another name for this test is the electromyograph.
So how soon can an EMG detect ALS?
“If a patient has symptoms from ALS, then a proper EMG will be able to detect abnormalities,” says Michael Cartwright, MD, a board certified neurologist at Wake Forest Baptist Medical Center in Winston Salem, NC.
“However, this requires that the correct muscles be tested and the EMG be performed by a physician with experience assessing for ALS.”
Some neurologists specialize in EMG testing.
What many people do not know is that this fatal neurological disorder is a clinical diagnosis.
This means that the physician makes the diagnosis based on what he or she observes in the clinical setting with the patient.
Dr. Cartwright explains, “An EMG is used to exclude other diseases, and there are certain patterns of EMG change seen with ALS. But EMG alone does not make the diagnosis of ALS.”
Wow, this could explain why so many patients fear that they were misdiagnosed with BFS (benign fasciculation syndrome) — believing they actually have amyotrophic lateral sclerosis.
So though the EMG is an important tool…it unfortunately isn’t definitive enough to reveal that a patient definitely has ALS.
As a matter of fact, the site for Massachusetts General Hospital Neurology states:
“The EMG may not clearly identify a problem early on in the disease. Sometimes, it must be repeated at a later time.”