Indent in Outer Thigh Muscle Explained
Here is why you should calm down and stop worrying about that indentation in your outer thigh muscle.
I’m going to tell you why seeing an indent in your outer thigh is actually a GOOD sign. I’m a former certified personal trainer and of course, a fitness expert — very knowledgeable of human anatomy and the musculoskeletal system.
By far, and I mean VERY FAR, the most likely explanation for an indent in your outer thigh muscle is NORMAL HUMAN ANATOMY.
We are not perfectly smooth and flat under our skin.
Take a good look at the quad indents in the legs shown at the top of this article. How many do you see? I count four on the leg closest to the viewer.
Look at the outer right thigh in the woman below.

Frankly, I think that the “dent” is attractive. There is a less obvious dent above it, just below her panty line. Both are normal human anatomy.
Do you see YOUR indent in the above photo?
I know the indent you’re speaking of, because it’s usually the first one to show when a person’s bodyfat gets low enough and they already have some tone to the thigh muscles.
Below is an anatomical illustration that clearly shows grooves between major muscles. These grooves are the sources of dents, when bodyfat is low enough.
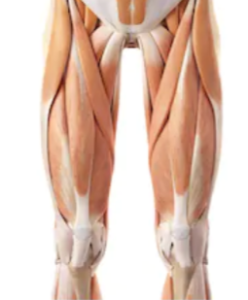
Shutterstock/Sebastian Kaulitzk
Depending on your bodyfat level, you can make the indent in your outer thigh disappear (or rather, get hidden) by gaining fat.
Eat up, gorge and put on fat, and this additional fat will conceal the indent or make it less noticeable. Guaranteed for normal anatomy.
The less bodyfat with toned muscles, the more visible will be the separation between the muscles. Less bodyfat is a desirable feature!
Physique athletes (not just bulky bodybuilders) LOVE to see indentations in their quads.
It’s a sign of reduced bodyfat.
The lingo in the muscle-building community is cut, definition or crack. But you need NOT be a physique enthusiast to “get” an indent in your outer thigh.
People with flabby, mushy muscles but also low bodyfat will probably not see this groove; or, it’ll be hardly noticeable.
The people most likely to notice it, who are not deliberately trying to get it, are those who exercise or play sports (and therefore have toned leg muscles), and have a low bodyfat level in that area.
When I say “low,” I don’t mean as low as a physique athlete posing on stage, but “low” as in: There’s really no excess fat there, no plumpness kind of fat.
If your weight fluctuates or you’re a yo-yo dieter, take notice of what these weight fluctuations do to the indent. The heavier you are (with fat), the less visible the indent.

Shutterstock/Syda Productions
People may panic if they notice that the indent comes and goes, but this coming-and going parallels weight fluctuations.
Other types of athletes also have this indent in their outer thigh, and the fact that athletes have this should reassure you that it’s benign, harmless.
Do some googling of images for soccer players, tennis players, any athlete where there are generous views of their outer thighs, and you’ll see lots of indentations — just like yours!
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Top image: Shutterstock/Weitwinkel
Angina Vomiting vs. from Bad Food or Anxiety

Is there a way to tell the difference between the vomiting from angina and that from anxiety or bad food?
“Angina vomiting would be similar to any form of angina; that is, it would be brought on by physical activity or severe emotional stress and go away when the stress is removed,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“It would typically be associated with chest pain (but not always), sweating, difficulty breathing or other signs of a heart attack.”
Bad Food
“Vomiting caused by bad food will usually start just after eating the food, be accompanied by abdominal cramping and/or diarrhea.
“True food poisoning may include fever and chills and the vomiting will be very copious until the stomach is emptied.”
One time when I gorged on pizza loaded with ground beef, I upchucked rather copiously.
When my mother vomited two days before a catheter angiogram showed life-threatening blockages in her coronary arteries, it was just a few gobs of goop in the waste can, but nonetheless, it was vomitus. And there’d been no abdominal cramping or diarrhea.
Nevertheless, Dr. Denier says, “These scenarios can be very similar in real life and even a doctor cannot always tell the difference right away.
“A bad gall bladder episode can look just like a heart attack! Any concerning symptoms should always be reported to your doctor.”
Vomiting from anxiety is uncommon. Don’t confuse anxiety with viewing a stomach-turning scene—anxiety is not the same as being “grossed out.”
I’m talking about anxiety from job stress, an unhealthy relationship, worrying about debt—just the classic chronic anxiety.
Vomiting from Unstable Angina
“Vomiting related to unstable angina is caused by stimulation of the autonomic nervous system,” begins Dr. Denier.
“In unstable angina, there is a severe blockage of blood flow to the heart. The heart is starved of oxygen and it is under stress because of that.
“When the body or parts of the body are under stress, the autonomic nervous system is triggered. This can result in vomiting, sweating and clammy skin.”
My mother had quintuple bypass surgery three days after mysteriously upchucking the goop; not the typical volume of vomitus that you’d see from bad food.
It was morning, prior to breakfast, and she hadn’t had that much food the previous day.
Dr. Denier says, “Unstable angina is a sign of an impending heart attack.” Three doctors told me that my mother would likely have a massive heart attack within a week without the bypass.
“In some cases, sweating and vomiting may be more significant symptoms than chest pain,” adds Dr. Denier.
“In fact, some patients have no chest pain at all. That is why unexplained vomiting should be taken seriously.” Even if the person has anxiety.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Left Side Chest Pain When Exhaling: Possible Causes

A cardiologist explains possible causes of left side chest pain when exhaling.
“Left sided chest pain that occurs with exhaling only is very rare,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“Usually pain that is related to inflammation of the lining of the heart or lungs (pericarditis or pleurisy) will occur with inspiration (inhaling), but it can happen with both (inhaling and exhaling) because it is worsened by any movement of the lining.”
Of course, pleurisy, which is inflammation of the lining of the lung, wouldn’t cause left side chest pain only when exhaling — but rather, both exhaling and inhaling.
“Asthma is a condition where exhaling can become difficult and there may be a sensation of pain on exhaling,” says Dr. Denier.
“Other things to consider are pulmonary embolism (blood clot), rib fracture, pneumonia [which can be only on the left side], spontaneous collapse of the lung or shingles (herpes zoster).”
A pulmonary embolism is likely to also present with difficulty breathing.
Risk Factors for a Blood Clot in the Lung (Pulmonary Embolism)
Prolonged Bed Rest
———
Recent Orthopedic or Abdominal Surgery
———
Pregnancy
———
Birth Control Pill Use
———
Obesity
———
Smoking
———
Recent Long Trip in an Airplane
If your rib is fractured, you’ll likely recall getting hit there or taking a hard fall.
If you’re healthy and fit, it’s not likely that your lung has suddenly collapsed, and shingles usually comes with additional symptoms.
Nevertheless, these above conditions can cause left side chest pain with each exhalation.
Can left sided chest pain only upon exhaling be related to heart disease?
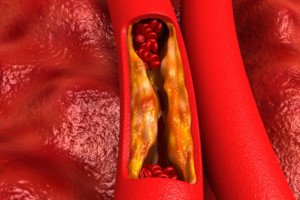
Plaque buildup in artery. Shutterstock/Explode
“This type of pain (only on exhaling) is not likely to be from coronary artery disease because angina is not related to respiration but is more likely to be influenced by exertion,” explains Dr. Denier.
“Even though the heart is located slightly to the left side, pain related to the heart is most often substernal or right under the sternum, the bone in the middle of your chest.
“Heart pain can be on the left however, and heart pain that is associated with breathing is usually inflammatory in nature and called pericarditis.”
I’ve had left side chest “pain” upon only exhalation more than once, and it correlated to my gym workouts (I suspect involvement of the pectoralis fascia).
The “pain” was more like an ache, but was quite noticeable.
The last time this happened, I could make it disappear if I leaned forward in my chair — even a hard exhalation couldn’t bring it out.
But if I sat back in the chair and exhaled, it was there. By late evening, it was completely gone.
Chest pain from coronary heart disease is not influenced by a change of position or, as Dr. Denier says, respiration.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Korawat photo shoot
Can Angina Last for Only Seconds?

Here’s what a cardiologist says about that sudden chest pain that lasts only seconds: angina or is this somehow related to your heart?
Any kind of pain or ache in the heart area (“beneath” the breasts or “behind” the breastbone) can be frightening.
Angina is chest pain that results from a shortage of blood flow in the heart, which means an insufficient oxygen supply — and hence, pain.
“A flicker of chest pain, especially if it happens at rest, is not likely to be angina,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“Anginal chest pain is related to a lack of blood flow to the heart muscle.
“It usually occurs when the demand for oxygen-rich blood to the heart is greater than the supply.
“This type of chest pain typically occurs when a person is performing some type of physical activity or is under extreme emotional stress.
“The pain will come on when the demand on the heart is present and will go away when the activity is stopped.”
Dr. Denier points out that if someone who has angina over-exerts themselves, thus evoking the pain in the chest, they may immediately cease the offending activity, causing the pain to promptly go away — so in that case, the angina was brief.
“Most brief chest pains are not angina but other causes such as gastrointestinal or musculoskeletal pains. All chest pains should be reported to your doctor.”
Can angina last for five seconds?
“Five seconds of chest pain, especially if it happens randomly or at rest, is not likely to be angina,” says Dr. Denier. She says the same goes for 10 seconds: not likely to be.
Possible causes of chest pain that comes on suddenly and lasts only seconds:
- Motility of fecal matter through the large colon
- Skeletal muscle spasm
- Nerve pain caused by muscles stressed from a recent weight workout
- Acid reflux
- Esophageal spasm
What about unstable angina? Can that last only seconds?
“No, unstable angina is not likely to last for only seconds. Pain that is very brief like that is not likely to be caused by the heart,” explains Dr. Denier.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/femme
Will an Unstable Angina Attack at Rest Worsen if You Start Moving?

If you have an attack of unstable angina while at rest, will the pain get worse if you begin engaging in physical activity?
Rest may be in the form of watching TV, standing while doing something passive, soaking in a bathtub, etc., and then suddenly, you have an episode of angina: pain in the chest.
What is unstable angina?
The unstable type is that which occurs while the patient is at rest or even asleep; it’s not predictable. When it decides to come, it will come.
It’s interesting to wonder about the following situation: The pain of unstable angina coming on while the patient is relaxing in a recliner watching TV.
The patient then exits the chair, picks up a vacuum cleaner or a 20 pound crate of books and carries it up a full flight of stairs.
Will the chest pain worsen or is the pain “set” once it occurs?
Chest pain from coronary artery disease that occurs at rest is called unstable angina because “it suggests that there is a serious blockage of blood flow to the heart,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“There is not enough blood getting through the blockage even at rest, and this could mean that if anything worsens the situation by increasing demand on the heart or reducing the flow, it could result in a heart attack.
“So, yes, if you are already having chest pain at rest, it will likely get worse with activity and cause the artery to close all the way, causing permanent damage to the heart.”
Persisting with the offending physical exertion will NOT train your heart to be stronger and thus eventually prevent the unstable angina.
Being in denial will not toughen up your coronary arteries.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/fizkes
HOW Sudden Stress Can Cause Fatal Heart Attack or Stroke

When someone says, “You stress me out so much you’re going to give me a heart attack,” maybe they’re onto something.
Ever hear someone say, “All this stress is gonna give me a stroke!”?
David Davies did a study based on a theory that heart attack and stroke can be triggered by a type of hormone that’s released when we are under acute stress.
And of course, we all know that a heart attack can be fatal. So can a stroke. Sometimes the death occurs days or weeks after the event, and other times, that very same day.
This “fight or flee” chemical messenger that Davies looked into is called norepinephrine, a type of catecholamine hormone.
Davies, from Binghamton University, says in his report that a stroke or heart attck often happen after an event in which elevated levels of catecholamine hormones get released into the blood and tissues.
The carotid artery supplies blood to the brain. If a clot forms in this artery and travels to the brain, it can lodge in a blood vessel and block off oxygen to the area of the brain that the vessel feeds: a stroke (ischemic).
If a clot forms in the heart and cuts off oxygen, that’s a heart attack (ischemic).
The clot can be made up of soft arterial plaque, and the clot in this case is often referred to as a “fragment.”
Broken Heart Syndrome — Another Avenue to Consider
Though this name implies that a romantic breakup can harm the heart, that’s not what this term refers to.
“Sudden stress can cause a heart attack due to Takotsubo syndrome or broken heart syndrome,” says Nieca Goldberg, MD, medical director of NYU Women’s Heart Program and radio show host of “Beyond the Heart” on Doctor Radio SiriusXM.
Dr. Goldberg explains, “It this form of heart attack the patient has abnormal heart function and normal arteries. Over time the heart function improves.
“Elderly people [who suffer heart attacks soon after a stressful event] may have underlying heart disease, and this may be due to plaque rupture, but another cause may be Takotsubo syndrome.”
Stress-induced cardiomyopathy – another name for broken heart syndrome – is when the left ventricle in the heart weakens.
This has nothing to do with clogged arteries or plaque fragments obstructing blood flow.
That left ventricle is the heart’s main pumping mechanism. Severe emotional stress – such as that would be experienced by a home invasion, home fire, a car accident or learning tragic news – can literally weaken this pumping chamber.
What causes arterial plaque to rupture in the first place?
Soft plaque is unstable; it can rupture, but what Davies has found is that the rupturing can be triggered by sudden stress.
His team removed diseased carotid arteries from patients, and multiple species of bacteria were isolated and cultured from the walls of these arteries.
These bacteria exist in the form of “biofilms” along the inner arterial walls, and these biofilms were present in every diseased carotid artery in this study.
Under normal circumstances, bacterial biofilms are resistant to antibiotics; the films remain intact. The immune system can’t shake these films, either.
However, something else can: norepinephrine. Norepinephrine delivers a message to the biofilms to break up and release enzymes. These enzymes dissolve the biofilms.
But because the biofilm is in such close proximity to the soft plaque—you guessed it—the soft plaque breaks up, too!
We now have fragments of the soft plaque in the bloodstream, poised to create a blockage of oxygen transport to the brain or heart.
Davies tested his theory by adding norepinephrine to biofilms on the interior walls of silicone tubing.
The amount of this hormone that he added was at a level similar to what a person undergoing extreme stress would have.
At least one species of bacteria, that’s commonly associated with the carotid arteries that were studied, underwent a biofilm disperson response when subjected to norepinephrine, says the paper.
This discovery is new to the world of medical research, so you can anticipate that this will set the stage for bacteria being considered as part of the management of cholesterol levels.
This study, however, does NOT rule out broken heart syndrome as a pathway to emotional stressors leading to a heart attack.
But one thing’s for sure: The more physically fit you are and the more natural is your diet, the lower your risk of suffering from a heart attack in the wake of emotional or physical stressors.
 Dr. Goldberg is senior advisor, Women’s Health Strategy, NYU Langone Health; founder and former medical director, Joan H. Tisch Center for Women’s Health; and clinical associate professor, NYU Grossman School of Medicine.
Dr. Goldberg is senior advisor, Women’s Health Strategy, NYU Langone Health; founder and former medical director, Joan H. Tisch Center for Women’s Health; and clinical associate professor, NYU Grossman School of Medicine.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/photofriday
Source sciencedaily.com/releases/2014/06/140610102010.htm
What Is the Shortest Time Angina Pain in the Chest Can Last ?

So if chest pain lasts under a certain period of time, like really short, would this mean it CAN’T be from angina and thus nothing to worry about?
Or can angina cause sudden but very brief shots of chest pain?
Here’s the answer from a cardiologist to what the shortest duration of time is for angina pain.
“Anginal pain typically lasts at least a few minutes and sometimes as long as hours,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“It lasts as long as the demand on the heart is greater than the supply. That means that the pain usually lasts as long as the activity or stress that is causing it.
“Once a person knows they have angina, they may stop an activity as soon as they feel the pain come on. In that case, it may last only a very brief time like a minute or so. This is not common, however.
“Most brief episodes of chest pain (seconds) are not angina. All chest pain should be reported to your doctor.”
What about unstable angina?
This is when the pain, from insufficient blood flow in the heart, occurs spontaneously—when the person is at rest, under no stress.
This type may even occur in their sleep and awaken them.
How long can unstable angina last?
“Unstable angina means there has been a change in the pattern of your known angina,” says Dr. Denier. “It may be more frequent, last longer than usual or be brought on more easily, sometimes even at rest,” she explains.
“It suggests that there is a serious blockage of one of the coronary arteries. This type of angina may last for hours.”
It wouldn’t be short-lived, “and it would most often be associated with other signs of coronary artery disease such as sweating or nausea or shortness of breath.”
In particular, this kind of angina will be brought on by physical exertion (as will the stable kind) — even something as seemingly innocuous as going up a flight of stairs or quickly pushing a shopping cart across asphalt will usually bring it on.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Dan Kosmayer
Breast Cancer Thermography: Truth or Hype?
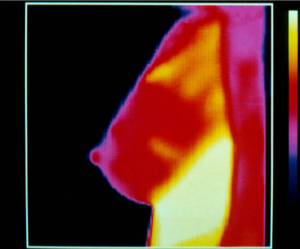
What is REALLY the truth — or hype — about how effective breast thermography is at detecting cancer?
Some claims are that thermography can detect breast cancer years before a mammograph would pick it up.
Is this too good to be true? And if it’s all a lie, how is it that thermography companies are getting away with these claims?
I decided to get a radiologist’s take on this. But to be fair, keep in mind that this article represents the doctor’s perspective.
My job here is to accurately represent Dr. Debora Fineman.
Dr. Fineman is a former diagnostic radiologist with Cancer Treatment Centers of America.
Breast Thermography Claims: Too Good to Be True?
You may have read somewhere that thermography, which does not use radiation, can detect breast cancer years before it actually develops, and that this imaging device does not require the painful compression of the breast, but instead, uses heat.
So it’s fair to wonder just how accurate these reports are and why thermography isn’t a standard screening tool for the detection of breast cancer.
Here is how Dr. Fineman responded to my questions:
I’ll refer you to a position paper from the American College of Radiology, which is the main board determining policies and procedures for radiology including mammography.
The appropriateness criteria from 2012 states, “There is insufficient evidence to support the use of other imaging modalities such as thermography for breast cancer screening.”
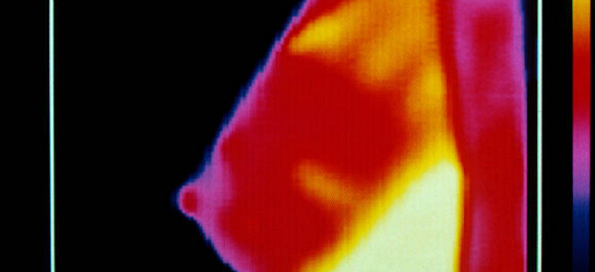
The American Cancer Society position on thermography quotes a 2012 research review that found that “Thermography was able to detect only a quarter of the breast cancers found by mammography.
In other words it failed to detect three out of four cancers that were known to be present in the breast. Digital infrared thermal imaging, which some people believe is a newer and better type of thermography, has the same failure rate. This is why thermography should not be used as a substitute for mammograms.”
When I type into the search engine, “Can thermography detect breast cancer that a mammogram misses?” the results indicate that there has been no research on this; that there’s no data.
 Dr. Fineman has been in practice for 30+ years.
Dr. Fineman has been in practice for 30+ years.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Workplace Bullying Leads to Depression

Workplace bullying is a serious problem that can lead to a depressing low mood and/or insomnia.
The recipient depends on their job for income — which throws a real huge kink in the chain.
A study that appears in the journal BMJ Open says that even just witnessing bullying on the job increases the odds that employees will be on drugs for depression, taking prescribed sleeping pills or tranquilizers.
The study participants were between age 40 and 60 and they were part of the Helsinki Health Study.
The association between workplace bullying and the use of prescription psychoactive drugs (for depression, sleep and anxiety) was present for both genders.
A hostile work environment can be incentive enough for people to feel so crummy and “depressed” — not to mention being riddled with anxiety — that they ask their doctor to “prescribe something to help.”
This association of medication usage remained after variables (that could influence the study results) were adjusted for, such as being bullied in childhood.
Is there bullying at your workplace?
“We must distinguish between low mood and brain depression,” says Rupali Chadha, MD, former chief of medical staff at Metropolitan State Hospital in Norwalk, CA.
“If you have major depressive disorder in yourself or even your family, sure, any stressful situation can cause you to fall into a depression (brain type).
“If not, of course, a stressful situation can demoralize you (just plain low mood, not necessarily needing medicine).
“The best way to tell is to see an MD psychiatrist, not a psychologist, to see if this has blossomed into a brain depression — or is low mood treated better with stress management, therapy, yoga … even maybe a new job (or standing up to the bully with HR).”
 In addition to general psychiatry, Dr. Chadha is also a forensic psychiatrist who treats the brain conditions of the criminally insane and serves as an expert witness in trials. She has a passion for fitness plus how the body, mind and spirit come together to build a healthy individual.
In addition to general psychiatry, Dr. Chadha is also a forensic psychiatrist who treats the brain conditions of the criminally insane and serves as an expert witness in trials. She has a passion for fitness plus how the body, mind and spirit come together to build a healthy individual.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com/katemangostar
Source: sciencedaily.com/releases/2012/12/121212205727.htm
Causes of ADHD: Bad Parenting or Brain Wiring?

What more likely leads to ADHD? Parenting methods or innate brain wiring?
If you’ve ever known someone whose child was diagnosed with ADHD, or, if your own child has received this diagnosis, perhaps you’ve often wondered if errors in parenting were mostly responsible, as opposed to just how the child’s brain is naturally hardwired.
“ADHD is a ‘brain wiring’ issue,” says Dr. Divyansu Patel, MD, a psychiatry specialist for 15+ years.
Dr. Patel explains, “It can be genetically inherited, meaning at least one of the parents has had symptoms.”
What if the child seems to have a behavioral issue, such as acting “bratty” in the presence of his or her parents?
What if one of the parents is very lenient, and the other seems to be indifferent, which then creates the illusion of a parenting issue that promotes the hyperactive, impulsive or “rude” behavior?
Dr. Patel points out that in such a case, though the child may have clinical signs of ADHD, that child may also have what is known as oppositional defiant disorder.
Though some people may be tempted to consider this a more technical term for “disobedient child” or a “child whose parents are not consistent with rules,” Dr. Patel explains the following:
“This is a comorbid disorder with ADHD about 40% of the time.
“ODD is more about behavior issues, as it is managed with therapy and then medication.
“Typically, it can originate or be exacerbated when parents are not on the ‘same page’ about parenting.”
ADHD and the Brain
Neuroscientists are looking more towards the miswiring of the brain’s reward system as a potential cause of ADHD, vs. so-called bad parenting.
For instance, study results appear in the journal Neuron.
The researchers from the Mayo Clinic in Florida and Aarhus University in Denmark investigated a type of neuron that regulates pleasure, reward, motivation and cognition.
These dopaminergic neurons are thought to be connected to the development of attention deficit hyperactivity disorder.
SorCS2 is a receptor system that’s responsible for the correct wiring pertaining to the dopaminergic neurons. This occurs during embryonic development.
However, after the brain matures, if there’s a cut in SorCS2, a two-chain receptor results. This two-chain receptor causes cell death.
SorCS2 acts as a molecular switch, say the scientists, between what seems to be opposing effects in proBDNF, a neuronal growth factor.
This growth factor aids in the selection of cells that can most benefit the nervous system, and it also gets rid of the cells that are less beneficial.
This way, a finely tuned network of neurons is established.
Mice that are deficient in SorCS2 lack a response to proBDNF.
The contacts between dopaminergic neurons are dysfunctional.
The paper also notes that numerous other studies have reported that people with ADHD commonly exhibit miswiring in the said brain region.
Think of a single-chain protein that’s the SorCS2: a long chain composed of amino acids.
Now, imagine it gets snipped in two. It now functions differently, leading to damage in the nerves of the peripheral nervous system.
What is ADHD?
“ADHD” is actually a term that describes a number of symptoms or signs.
So if someone “has ADHD,” they have enough of these features to get the diagnosis.
ADHD is also considered a neurodevelopmental disorder that one never outgrows. A first-time diagnosis may even occur in adulthood.
“Typical symptoms include inattention, poor concentration, poor organization, poor attention to detail, forgetful in daily activities,” says Dr. Patel.
“They can also have hyperactivity which is typical in childhood, which can include fidgeting, squirming when seated, difficultly with remaining seated, hard time playing quietly, talking excessively.
“Impulsivity is also a symptom including impatience, a hard time waiting for a turn and interrupting.”
ADHD in the form of atypical brain wiring also comes with perks such as easily adapting to fluctuating schedules and the ability to hyperfocus on a topic that one is passionate about.











 Dr. Patel
Dr. Patel
































