Can a Pacemaker Implant Damage the Vagal Nerve?

If a person has recently had a pacemaker implant, but is also suffering from blackouts or fainting spells, one may wonder if the vagal nerve is somehow getting adversely affected by the pacemaker.
Pacemakers Are Close to the Vagal Nerve
“Pacemakers do not damage vagal nerves,” says David N. Smith, MD, a board certified cardiologist with Premier Cardiovascular Care and Wellness in SC.
He continues: “The question may refer to a phenomenon where the pacemaker implantation process stimulates the vagal nerve to cause hiccups.
“There still would be no damage to the nerve itself. If the pacemaker insertion does stimulate the vagal nerve during implantation, this is more of a reflection of the pacemaker lead being close to the vagal nerve.
“There is no damage to the vagal nerve. The pacemaker lead can be repositioned to correct this.”
What Is a Pacemaker?
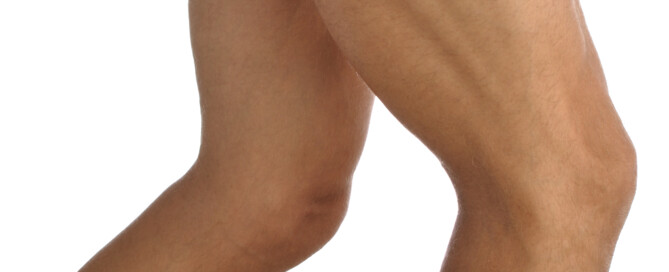
This little device has two parts: a generator and electrodes (leads).
It’s placed under the skin (a minor procedure) in the person’s chest where it will then help control, or pace, the heartbeat.
Usually a person needs a pacemaker due to an arrhythmia or abnormal heart rhythm.
If the heart beats too slowly, a pacemaker can set the programmed pace, such as 70 beats per minute.
A pacemaker may be implanted after a person has a heart attack or undergoes coronary bypass surgery.
The pacemaker can detect if the patient’s heartbeat is too slow.
It then sends an electrical signal to the heart to speed up the pulse.
Some people may fear the idea of something being put just under their skin that sends electrical signals to their heart.
But complications from the procedure are uncommon. They include the following:
• Infection at the site of implantation
• Allergic response to the anesthesia or dye that’s used during the implantation
• Bleeding or bruising at the generator site. This is more likely if the patient is on a blood thinner.
• Collapsed lung
• Damage to the blood vessels or nerves (which would include the vagal) near the pacemaker. This is very uncommon.

Dr. Smith is a published author, national lecturer and Yale-trained physician-scientist certified by the American Board of Internal Medicine in Cardiovascular Disease. From his basic science background combined with advanced clinical research training at the Columbia Mailman School of Public Health, he brings an integrated holistic approach to cardiovascular medicine.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: J. Heuser/CreativeCommons
Why Isn’t the Corus CAD Test Part of Routine Physical?
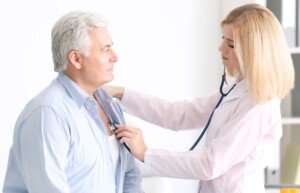
Have you been wondering why a routine physical or even routine cardiologist exam doesn’t include the Corus CAD test?
This blood test uses “gene expression” to quickly and safely determine when chest pain is due to obstructive coronary artery disease (clogged arteries).
Some patients are suitable candidates for this test, called the Corus CAD (coronary artery disease).
They have not been diagnosed with a previous heart attack; are not diabetic; have not had a CABG; are not currently on chemotherapeutic drugs, immune-suppressing or steroid prescription drugs.
Chest pain is quite a common symptom of “clogged arteries” (obstructive heart disease).
Another common symptom is undue fatigue or shortness of breath.
The Corus CAD blood test results are ready in 72 hours, and the test can be done in a doctor’s office.
So why isn’t this simple test part of either the routine physical or a heart patient’s routine visit to the cardiologist?
I asked this to cardiologist David N. Smith, MD, a board certified cardiologist with Premier Cardiovascular Care and Wellness in SC.
Dr. Smith explains, “I believe at this point the test is relatively new and most have not heard of its benefits yet.
“Moreover, the diagnostic accuracy and clinical utility of the test fits best when the patient has non-acute signs and symptoms suggestive of obstructive coronary artery disease.
“Therefore, the test should not be used to screen every patient for obstructive CAD.
“Although the test has proven to be reliable in ruling out obstructive in stable symptomatic patients, the truth is it takes many years before new technology will be adapted into the guidelines by the American College of Cardiology or the American Heart Association.
“While numerous Corus CAD studies have been published in highly ranked peer-reviewed journals, it takes time, experience, and more randomized, controlled evidence-based trials before being completely accepted into standard of care.”

Dr. Smith is a published author, national lecturer and Yale-trained physician-scientist certified by the American Board of Internal Medicine in Cardiovascular Disease. From his basic science background combined with advanced clinical research training at the Columbia Mailman School of Public Health, he brings an integrated holistic approach to cardiovascular medicine.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Africa Studio
Why Don’t CABG Patients Get the Corus CAD Test?

Why isn’t the Corus CAD test given to people who’ve had coronary bypass surgery?
This test uses “gene expression” to safely and quickly determine whose chest pain or shortness of breath is the result of obstructive coronary artery disease (clogged arteries).
Certain patients are candidates for this blood test, called the Corus CAD (coronary artery disease).
They are as follows:
- not diabetic
- have not been diagnosed with a previous heart attack
- have not had coronary artery bypass surgery (CABG)
- are not currently taking chemotherapeutic drugs, immune-suppressing drugs or steroid prescription drugs.
The Corus CAD test can help identify people who are unlikely to have obstructive heart artery disease as the cause of their symptoms.
Chest pain is a very common symptom of obstructive coronary artery disease, the so-called clogged arteries.
Other symptoms are typically that of shortness of breath upon exertion, and increasing fatigue over time.
Less common symptoms include nausea, burning sensation in the upper body, dizziness, lightheaded feeling, and pressure in the throat, jaw, shoulder, abdomen, back or arm.
Often, the only symptom is pain in the chest or what may be described as tightness or pressure.
Corus CAD Blood Test
The Corus CAD blood test results are available in just 72 hours and the test can be done in a doctor’s office.
I wondered why a CABG patient would not be a candidate for this test, since coronary bypass surgery doesn’t actually reduce plaque buildup in arteries,
The heart disease itself continues progressing despite the surgery. What CABG does is re-route the “plumbing” of the heart. This treats the symptom.
“Patients who have CABG have been diagnosed with severe and/or obstructive CAD, and thus were excluded from the clinical trials,” says David N. Smith, MD, a board certified cardiologist with Premier Cardiovascular Care and Wellness in SC.
“Therefore, the test has not been studied with or validated for patients who have had CABG.”

Dr. Smith is a published author, national lecturer and Yale-trained physician-scientist certified by the American Board of Internal Medicine in Cardiovascular Disease. From his basic science background combined with advanced clinical research training at the Columbia Mailman School of Public Health, he brings an integrated holistic approach to cardiovascular medicine.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
,
Top image: Freepik.com, peoplecreations
Is IBS a Real Disease & Diagnosis or just Symptom Collection?

“IBS by definition is not a true disease,” says Dr. Saad Habba, MD, a board certified gastroenterologist at Overlook Medical Center in Summit, NJ.
One of Dr. Habba’s areas of interest is irritable bowel syndrome.
He continues, “The condition is a collection of symptoms that are collectively referred to as IBS.
“In fact, many physicians diagnose IBS after some preliminary workup is negative, and it is frequently used as a wastebasket diagnosis.”
If you are ever diagnosed with irritable bowel syndrome but your workup did not include a colonoscopy, this is a reg flag for a wastebasket diagnosis.
Conditions that only a colonoscopy could reveal can cause symptoms that are very similar to those of IBS, namely, microscopic colitis.
“Before diagnosing IBS, a thorough and detailed workup must be done to rule out other medical conditions.”
Dr. Habba performed a large study that demonstrated this very clearly.
It showed that 98 percent of patients with irritable bowel syndrome were prematurely tagged with this diagnosis.
However, when additional detailed workup was performed, other medical conditions were exposed.
It’s vital to get the right diagnosis, even if the symptoms are identical.
For example, people with microscopic colitis are often misdiagnosed with IBS, especially if they’re young adults, because a doctor is less likely to recommend a colonoscopy for a 25-year-old complaining of diarrhea and abdominal cramps (symptoms of both irritable bowel syndrome and microscopic colitis), vs. a 50-year-old reporting the same symptoms.
However, microscopic colitis can only be diagnosed by viewing tissue samples, taken during a colonoscopy, under a microscope.
Dr. Habba says that IBS should not be used as a “catch-all” term as is frequently done.
The symptoms are real alright (who can fake diarrhea, bloating and constipation?), but technically, it’s not a disease.
 Dr. Habba pioneered the concept of IBS being a wastebasket diagnosis and collection of different entities rather than a true single medical condition. He’s been presented and published in 26 national and international medical journals and symposia.
Dr. Habba pioneered the concept of IBS being a wastebasket diagnosis and collection of different entities rather than a true single medical condition. He’s been presented and published in 26 national and international medical journals and symposia.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Bannasak Krodkeaw
When Your Child’s Hamster Dies: Guide for Parents
If your child’s hamster is very sick or seems to be dying, here are clear instructions on what you, the parent, should do and NOT do.
In your mind, the hamster might be nothing more than a mindless rodent.
In your child’s mind, the hamster was a cute, cuddly, furry little thing with a personality.
If your child’s beloved hamster has recently died, this can be just as tormenting as if you lost some prized, inanimate memento or piece of jewelry with sentimental meaning.
So be careful how you react to your child whose hamster just died.
When I was 11 years old, my hamster, “Fang,” died. My mother didn’t respond the way a parent should when a child’s pet dies.
I loved that hamster, and he died before his time, having caught some kind of viral or bacterial infection after being handled by several neighborhood children.
How a parent should respond when a child’s hamster dies begins with when the hamster is in the process of dying.
My hamster didn’t die just like that without warning. Fang was sick for a few days preceding his death – very sick. My mother knew this, but didn’t call any veterinarians.
Because I was a naïve 11-year-old, I didn’t think to open the phone book and look under the listings for veterinarians and start making phone calls.
At age 11, I wasn’t supposed to do things like that. I’m not even sure the idea had even occurred to me, actually.
To complicate things, my hamster got sick on a Saturday, when vet clinics are closed.
However, on Sunday, my older sister made a call or two; I cannot recall to whom, but she definitely was making a few phone calls.
But nothing came of them. I think they were to some vet clinics and they were closed.
She gave up pretty quickly, and I was still with a hamster that was getting sicker — I mean really sick, like remaining huddled inside his sleeping bottle.
He wouldn’t come out; wouldn’t eat; and when he moved, it looked painful.
My mother may have asked every so often how Fang was doing, but that was it. Nothing more.
There was no, “On Tuesday we’ll take him to the veterinarian.” Monday was Memorial Day.
Because I was only 11, I didn’t think there was anything that could be done about my sick and dying hamster.
I was completely dependent upon my parents. My parents didn’t really regard Fang as a true pet.
Maybe that’s because hamsters’ brains aren’t developed enough to “know” their handler, like a dog’s and cat’s brain is.
Hamsters don’t look you in the eye and communicate with facial expressions, as do dogs and cats.
We had never had any pets in the house, either; my parents weren’t pet people.
The only reason I had Fang was because my oldest brother, who was daring, one day brought home Fang; in college he had a hamster from the same litter that Fang had come from.

On Memorial Day, Fang was dead; stiff, lifeless, inside his bottle. I cannot recall how I alerted my mother to this.
My father was even less involved, because this was (in my mind) one of those mother things.
But I do remember my mother nonchalantly taking the bottle, with the dead stiff hamster inside, and tossing it in the rubbish outside. And that was that.
There was no consolation; it were as though the dead hamster was an old pair of socks.
Maybe my mother thought that if she didn’t console me or offer words of comfort, that I’d bounce back quickly or not feel any sorrow.
Maybe my mother didn’t know I was distraught that my hamster had died.
But I was determined to retrieve the bottle, with Fang inside, from the garbage can outside.
I did this behind my mother’s back, because I knew she’d never permit this.
It was raining and I fetched the hamster from the garbage can, still in the bottle.
I dug a hole at the side of the house and buried the bottle with Fang inside.
I was just mortified that the whole situation had been treated so casually and matter-of-factly.
If your child’s hamster is sick or dying, phone a veterinarian. Don’t even THINK about how much it might cost you.

When you have kids, you should realize that raising kids isn’t cheap, and unexpected things come up.
- You can put the vet bill on a credit card.
- You can work overtime if you have an outside job.
- You can borrow money from friends and family.
Just GET the dying hamster to a veterinarian — and your child will look up to you for years.
If the hamster is dying on a weekend, call vet clinics until you get one that’s open.
If one is not open, stand by your child and talk about the dying hamster; maybe the hamster isn’t dying and will recover; maybe the hamster will get better if you do certain things with it.
This is something that you, as a parent, should be prepared for; you can get this information from a veterinarian at the time your child first gets the pet.
Do not assume veterinarians are only for dogs, cats and birds. There’s a such thing as a “small animal clinic.”
This means rodents! Hamsters are extremely common as pets, and parents often get a hamster for a child begging for a pet because hamsters are relatively low maintenance pets.
They don’t bark, don’t need to be housebroken, don’t require a lot of food or space, don’t scratch up furniture, etc.
If your child’s hamster dies, you had better be there as emotional support if you want to win permanent brownie points with your child.
And YES, parents SHOULD care if their child “likes” them!
If your child doesn’t have faith and confidence in you, then don’t expect him or her to come running to you for life advice in the future, and don’t be surprised if your child seeks advice about life from his peers instead of from you.
This is Parenting 101, and the School of Common Sense offers this free class year-round.
A hamster is a real pet to a child, even to adults who have them.
I bet you yourself are attached to some nonliving object that has special meaning to you.

Freepik.diller
What if it were stolen or lost? Think about that before you brush the death of your child’s hamster off as trite and trivial.
If your child’s hamster is dying, you have plenty of time to prepare a memorial.
Encourage your child to be a big part in the planning, and do not dismiss the idea as petty and ridiculous.
Instead, be glad that your child has compassion for a creature as small and as helpless as a hamster.
If your child’s hamster has already died, you can still create a memorial of sorts.
Sit down with your kid and ask him or her for ideas. Allow a mourning period for the dead hamster, and do not make your child think you feel it’s silly or nonsensical.
Take it from me, a former child who had a hamster that died prematurely; this makes me an expert in the area of how a parent should react when a child’s hamster is dying or has died.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can GERD Cause Constant Chest and Back Pain?
Are you wondering (hoping) that your constant chest and back pain is being caused by GERD rather than a heart problem?
GERD stands for gastroesophageal reflux disease and is notorious for causing chest pain.
“Acid reflux is when the normal stomach acid regurgitates up into the esophagus,” explains Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
“The muscles at the bottom of the esophagus are meant to act as a valve to hold down acid, but in many people this valve does not function properly. These symptoms can manifest differently in patients.
“In some patients, especially those with severe reflux, they can have constant chest pain.”
Sometimes, this sensation is more like an ache, including a duller type of ache.
Dr. Desai adds about the constant chest pain, “In general this is due to ulcerations in the esophagus from acid exposure.”
What about back pain?
“Back pain is less commonly associated with reflux. The treatment for this is antacid medication, which helps heal the damage of the esophagus from the acid.”
Keep a record of when your back pain or aching occurs.
-
- Is it only when the chest pain occurs?
- Have you seen a cardiologist to rule out a problem with your heart?
- Have you been diagnosed with GERD?
If you haven’t seen both a gastroenterologist and cardiologist, it’s time to.
Chest plus back pain should never be ignored. One of the conditions that can cause this duo-symptom is a dissecting aortic aneurysm.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Acid Reflux Cause a Heavy Pounding Heart?

Can the acid that’s refluxing up from your stomach and into your esophagus actually trigger a pounding heartbeat?
“Acid reflux is when the normal stomach acid regurgitates up into the esophagus,” says Jay Desai, MD, who specializes in colon cancer screening, upper endoscopy and consultative gastroenterology with New York Gastroenterology Associates.
“This happens to everyone to some degree. However, in some people, the symptoms can be more severe.
“This can be due to the presence of a larger amount of reflux compared to the average individual, or to the esophagus being more sensitive than in others.
“The symptoms of acid reflux can vary between individuals, but most people describe a ‘burning’ sensation in the stomach and chest.
“In some people, these symptoms can feel like a pressure sensation.”
Can acid reflux directly affect the way the heart beats?
Dr. Desai continues, “While a pounding heart is not a typical symptom, sometimes patients with acid reflux can become anxious that another issue, such as a heart attack, is occurring, which can lead to a pounding heart sensation.
“It is important for anyone with these symptoms to discuss them with their doctor to differentiate whether this is reflux related or a primary heart issue.”
Just because GERD or acid reflux doesn’t directly stimulate the heart to beat faster or harder doesn’t mean that a person can’t have both a digestive issue and a cardiac problem.
See a cardiologist for a thorough exam of your heart to rule out any issues such as an arrhythmia.

Board certified in internal medicine and gastroenterology, Dr. Desai provides a wide range of GI services including for bacterial overgrowth, constipation, acid reflux and GERD, IBS, incontinence and small bowel disease. Twitter handle: @NYGADocs
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Hriana
Parenting Mistakes that Make Child Bully Younger Sibling

One mistake parents can make is to blow off the bullying as normal sibling rivalry.
Sibling bullying isn’t “normal” or “healthy” just because the parents experienced it with their own siblings or just because it seems to be common.
Rivalry or competition among siblings is common and by definition, is not emotionally destructive or damaging. But bullying among siblings is exactly what it is: b u l l y i n g.
Most halfway decent parents don’t want bullying to occur among their children and will take efforts to stop it.
The problem is that many parents have the wrong approach, including failing to address the root causes—which is the secret to the cure.
What mistakes do parents make that create a fertile environment for sibling bullying?
One of the biggest factors is when the parents themselves bully one of their children.
If there’s a child in the house who’s younger than this target, chances are pretty good that this younger brother or sister is going to be the recipient of cruel treatment by that older targeted child.
Think of this as a pecking order effect. The older sibling doesn’t awaken one day thinking, “Well, Mom is always so hard on me, so that gives me the right to treat little Kassie the same way.”
Instead, the repeated cycle just naturally happens. You can say it’s learned.
But you can also say that the older child has a lot of hurt and pain inside, and needs a non-threatening dumping ground for it: the helpless younger brother or sister.
“Another often overlooked source of the older child’s anger is that when the younger child does inform the parents, they then reprimand or punish the older child, often accompanied by the castigation:
“‘You’re older! You should know better! You should set an example for your younger sibling!’
“So the older child now feels victimized by the younger sibling and their parents, and wants revenge!” says Israel (Izzy) Kalman, MS, nationally certified school psychologist; director of Bullies to Buddies and author of multiple books and publications on bullying and relationship problems.
Kids Do As You Do, Not As You Say
It’s Psychology 101. You’ve probably seen it right under your nose: A parent haranguing their child, and then the child behaving in a similar way to the younger brother or sister.
The bullying will fester if the victim is afraid to report it to the parents, or if the reporting results in the victim getting scolded and criticized.
Jack and his brother Jake get “beaten up” by their older brother Robby whenever Robby babysits them while their parents are away.
Robby threatens his brothers that if they “tell,” he’ll beat them up worse next time. This 11-year-old has more power over his eight- and seven-year-old brothers than their full-grown parents do.
How is this possible? Robby doesn’t feed them. Robby doesn’t provide them shelter or buy them things.
The parents here see parenting as a job, not as a relationship. Though Dad is a good provider materially and Mom keeps the house in excellent condition, they’re intimidating.
Dad is emotionally disconnected from his kids, and Mom is hard on all three, but especially the oldest, approaching her motherhood duties like a drill sergeant. No wonder Jack and Jake are scared to report the bullying.
It’s a “duhhh” situation: It’s only natural that “tough” Robby heap on two younger, smaller, helpless siblings. But he wouldn’t DARE talk back to his mother because he knows she’ll slap him if he does.
Don’t blame TV and video games on sibling bullying.

Freepik.com
Though these forms of entertainment offer violence, a child in a healthy, stable and fair household will be able to see this entertainment for what it is: entertainment only, not something to cruelly use on a younger sister or brother.
Violent video games won’t bring out what’s already NOT placed there by a dysfunctional household. “It is easy to blame entertainment for our children’s behavior and problems,” says Kalman.
Sibling bullying is NOT rivalry or competition. And it’s not necessarily physical.
It could come in the form of relentless belittling. Words are powerful.
Kids are told to shrug it off by adults who’d never tolerate the same kind of behavior from their coworkers in the workplace!
 Dr. Kalman is a psychotherapist in private practice and has treated many victims of bullying for over 20 years. He has published extensively on solutions to bullying.
Dr. Kalman is a psychotherapist in private practice and has treated many victims of bullying for over 20 years. He has published extensively on solutions to bullying.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/igor kisselev
Popular Articles on Diarrhea
One day I began noticing oddly shaped and colored bowel movements that were loose enough to be considered mild diarrhea.
I thought this was related to my period, which was due in several days.
Very soft stools preceding the onset of menstruation had happened to me before, so I really didn’t think a whole lot about this.
However, it was difficult to dismiss the fact that these poops just plain looked weird.
I really began worrying when every day, I kept having this strange looking diarrhea, and my period had already begun.
So I knew this diarrhea wasn’t related to menstruation at that point. Furthermore, I was getting up in the middle of the night to have this diarrhea.
And like clockwork, almost right after getting out of bed in the morning, I had to do another poop. I’d feel this odd unfamiliar churning in my lower stomach. I knew something was wrong.
I was also wondering why the joint aches that began more than a week prior to my period were still with me.
My menstrual related joint aches (PMS) had always disappeared by the time I officially began flowing.
But this time, the joint aches – and the diarrhea – persisted even after my period ended.
At the time, I didn’t connect the joint aches to the diarrhea. Instead I attributed them to some oddball hormonal fluctuation related to my monthly cycle.
I soon had a colonoscopy and some tissue samples from my large colon were extracted and set to a lab for analysis.
A few days later I was told I had microscopic colitis of the lymphocytic type.
This is a benign inflammatory bowel disease.
The cause is not known, but in my case, the onset was preceded by enormous longstanding anxiety over a family situation.
Since being diagnosed with microscopic colitis (which, by the way, is known for causing transient joint aches), I have written quite a few articles about this uncommon condition. Below are links to some of them.
What do microscopic colitis and IBS have in common and their diagnosis
For how long do the joint aches of MC last before the diarrhea finally comes?
Ever wonder if all that diarrhea takes with it all the nutrients you’ve worked so hard to get from eating healthful food?
Can microscopic colitis diarrhea actually strip you of some nutrients?
As for natural approaches to manage the diarrhea, perhaps you’ve been wondering about trying intermittent fasting.
This means confining all food intake, even small snacks, into predetermined segments of time, such as only four, six or eight hours.
Water intake can be at any time, though.
Here’s info on intermittent fasting if you have frequent episodes of diarrhea.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ Pixel-Shot
Dent in Thigh: One of the Most Feared Symptoms
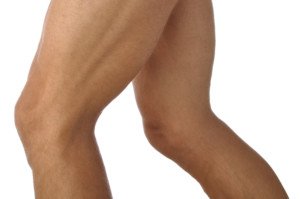
Let’s get to the bottom of whether or not a dent in your quadriceps muscle means you might have ALS.
The “quad dent” evokes fear in tens of thousands of people. Are you one of them?
Because I recognize the prevalence of how frightening this symptom is (it usually makes anxious people believing they might have ALS), I decided to write three articles on this topic.
Read all 3; they are a bit different from each other.
I’ve also included an article on dents in the calf muscle, since this location apparently is the second most cited for these mysterious dents that show up.
Wait till you find out what the most likely explanation is for this scary “symptom.”
Just what is the cause of a dent in your quadriceps muscles: atrophy? MS? ALS? or what?
Are you sick of having to inspect your leg all the time and wish you could cure this affliction and just forget about that dent in your muscle?
Shutterstock/joshya
Dents can appear anywhere where there is muscle — this means almost anywhere on your body.
But the legs may be the most common spot where odd grooves or depressions are noticed.
The outer thigh is one specific area where many people will notice an indent or an area that caves in a little.
But it’s not on the other leg. This can cause a lot of worry. Here is an explanation for what’s likely going on.
What about the middle or center of the front of your thigh? Have you noticed any indentations or grooves there?
If your quadriceps muscle group has a dent, this is very likely benign and harmless.
After all, muscles aren’t as smooth as polished wood. They’re supposed to have typography.
But there’s something else that perhaps you haven’t considered: That dent in your thigh might not even be the muscle.
There’s tissue between what you see as the external surface of the skin and the muscle underneath.
Perhaps that indentation is coming from that tissue, which consists of fat (even if you’re on the thin side), connective tissue, blood vessels and nerves. Beneath all that is fascia, a thin sheet of connective tissue that surrounds muscles.
As for those nerves, they themselves don’t cause dents, but changes in fat, fascia, or muscle tension around them can create dimpling in the thigh.
Now what about the calves?
In addition to being a common area for ongoing twitching, this portion of the body can also have a lot of visible indentations or grooves.
Are you so worried about this that your focus is off throughout the day?
Let’s take a look at what’s happening when calves are twitching and/or have a depressed area.