How Long Can Chest Pain from a Heart Problem Last?
Heart problems, namely severely clogged arteries, cause chest pain — even at rest if the disease is severe enough.
But how short is too short for chest pain to be heart related?
“Anginal chest pain is by definition, chest pain that is located in the substernal region, brought on by exertion and relieved by rest,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
But how long, or how short, can angina chest pain actually last?
Dr. Denier says, “There is no specific limit to the time that it may last. It may last only a few minutes or persist for a more extended period, but is most often from one to 15 minutes.
“Typically, it would be expected that the pain would subside shortly after stopping the activity that brought it on.
“Chest pain of cardiac etiology does not always follow an anginal pattern, particularly in women. There are many atypical presentations which also need to be carefully evaluated.”
When angina chest pain is brought on by physical activity (or high-charged emotions), and dissipates with cessation of the activity, this is called stable angina.
However, this symptom may also occur without any precipitating event. In this case, the condition is known as unstable angina, and it’s far more serious than the stable type.
My mother awoke one morning at 5 a.m. with chest pain that was extremely localized, about the size of a quarter or smaller—she could point to the specific area of her chest where this tiny area of pain was occurring. That morning it persisted till 7 a.m.
I took her to the ER anyways. She was admitted to the cardiac unit and next day, a catheter angiogram revealed “significant disease” in five main arteries.
She was immediately prepped for quintuple bypass surgery and mitral valve replacement.
I would later learn that for a few months preceding the surgery, she had been having the chest pain on and off, sometimes brought on by housework and sometimes for no apparent reason.
Regardless of how long you have chest pain for, get it checked out by a cardiologist rather than assume that it’s a digestive problem.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock, SewCream
Low Ejection Fraction without Congestive Heart Failure?
Can a person have a low ejection fraction, even like 35 percent, yet not have congestive heart failure?
Ejection fraction means how much blood the heart pumps out with each beat.
For this article I consulted with Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
My mother’s ejection fraction is low, coming in at 35 percent, yet she has not been diagnosed with congestive heart failure even though she’s had EKGs and echocardiograms, part of ongoing follow-up care since her quintuple bypass surgery more than two years ago.
So this got me thinking, because her doctor wanted to put her on a drug to raise the ejection fraction, even though he did not actually tell her, “You have congestive heart failure.”
His nurse called her a few weeks later after a blood test came back deeming her suitable to take the drug, and the nurse asked if my mother was experiencing shortness of breath (one symptom of congestive heart failure) or swollen ankles/lower legs (another symptom of congestive heart failure).
Congestive heart failure is when the heart does not pump out an adequate supply of blood with each beat.
Ejection fraction measures how much blood is pumped with each beat.
Dr. Denier explains, “It is possible to have an ejection fraction of 35 percent or less without clinical signs of heart failure.
“With good medical management, some of these patients will never suffer an episode of overt heart failure.
“On the contrary, patients can have clinical heart failure even with a normal ejection fraction.
“For patients with low ejection fractions, development of symptoms is influenced in part by other co-morbid conditions such as coronary artery disease, hypertension, diabetes and kidney disease.
“Other significant factors are age, diet, presence of arrhythmias and structural abnormalities of the heart.
“Heart rate, blood pressure and the amount of demand placed on the heart are also influential.
“Although elderly patients are more likely to have more contributing factors to develop heart failure, they may actually tolerate symptoms better.
“A typical 40-year-old may put more demand on the heart with strenuous activities, where an 80-year-old may be more sedentary.
“This of course is very individual and not always predictive of who will develop clinical signs of heart failure.”

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Africa Studio
Costochondritis vs. Heart Attack, Angina: Symptom Comparison
People with costochondritis may say it “feels like a heart attack,” that the pain can be severe, but is there a way to tell the difference?
Is there a way for a layperson to tell the difference between costochondritis chest pain and that of angina or a heart attack?
“Chest pain caused by costochondritis is a common mimic of cardiac chest pain,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“It comes from the chest wall and usually involves the joints between the ribs and the sternum in the anterior chest.” Anterior means front.
“In contrast to cardiac chest pain, this pain is more likely to be sharp in quality and worsened by movement, respiration or coughing,” says Dr. Denier.
“This pain is musculoskeletal in etiology and is similar to other types of arthritis pain.”
The medical prefix of “chond” refers to cartilage, and the suffix of “itis” means inflammation. “Costo” refers to location in this case.
Dr. Denier continues, “It is aggravated by use of the pectoral muscles of the chest, may flare up after strenuous upper body exercise or with changes in weather.”
Weightlifters with costochondritis have reported that pectoral exercises can bring on a lot of discomfort.
“On physical exam, there is often reproducible soreness to palpation directly over the joints in this area,” says Dr. Denier about costochondritis.
“This finding is helpful in establishing the diagnosis, but it is important to remember that its presence does not rule out chest pain of cardiac origin.”
In other words, if your chest area is sore to the touch, this doesn’t mean it’s costochondritis and not a cardiac problem.
In fact, by coincidence, you can have both costochondritis and a heart problem, but remember, though the symptoms can be very similar, these two conditions are unrelated.
“Relief of costochondritis pain is best achieved with anti-inflammatory drugs,” says Dr. Denier.
“In contrast to cardiac chest pain, costochondritis does not usually worsen with generalized exertion such as walking uphill.
“Costochondritis will persist throughout the day, where cardiac chest pain tends to come and go in limited episodes.
“Cardiac chest pain can radiate to the arms, jaw, neck or upper back and is often associated with other symptoms such as shortness of breath, diaphoresis and nausea.”

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/OBprod
Pain After Total Knee Replacement: Your Course of Action
Learn exactly what you should do, tests to have, etc., if you have knee pain and swelling long after TKR.
If you have knee pain despite having “recovered” from total knee replacement surgery, and especially if there’s swelling and warmth about the joint, then you should immediately suspect loosened implants so you don’t waste time on a wild goose chase.
My father was led astray by a litany of doctors, when all along, a simple test could have nailed why he was having pain in both knees after having TKR in both.
Knee pain right after, and for a few weeks following, the surgery is normal.
After a few months you should be feeling great, and my father was, but then he began noticing pain in the surgical knee.
He also had a TKR on the other knee, and that joint never felt good at any point afterwards, and ultimately, that joint developed the most pain.
He didn’t receive follow-up treatment with his original orthopedic surgeon about this, because by the time he realized there was a knee problem, he had switched medical plans.
Following is a faulty time line that YOU should not have to endure.
January 2010: Knee pain begins, despite having TKR.
June 2010. Sees Dr. “Wardell,” the PCP; X-rays show TKR okay. Doctor suspects spinal issues causing knee pain and recommends consult with neurosurgeon, especially since pain escalates in leg and back.
MISTAKES: My father waited six months to see a doctor; though the primary physician suspected an implant problem, he did not order two tests that could have revealed this: a bone scan and a Marcaine injection.
Making the issue trickier was that my father had spinal stenosis, which played a role in various diagnoses.
September 2010: Spine surgery recommended.
MISTAKE: Waiting another three months without aggressively pursuing possibility of a failed TKR.
October 2010: Non-invasive back surgery. This corrects the leg (quad) pain (which by then had developed in both legs) but the knee and low back problems remain.
February 2011: MRI.
MISTAKE: Letting another large chunk of time (four months) go by, during which the quad discomfort returned and bilateral knee pain continued.
The neurosurgeon who did the spine operation reviews MRI and sees no further reason for back surgery.
Recommends nerve pain block and visit to a physiatrist (MD who treats pain in nerves, muscles and bones).
March 2011: Physiatrist Dr. “Mueller” diagnoses nerve irritation and recommends continuation of exercises (all along my father had been doing various gentle leg exercises).
Later that month: A different orthopedic surgeon, Dr. “Switzer,” examines knees and hips via X-ray, revealing good TKRs but also hip osteoarthritis. Sharp hip pain had, indeed, developed over past few months. A pain block suppresses it.
June 2011: A Dr. “Seibold” says knee and quad pains could mean spinal problem.
MISTAKE: Letting three months go by without aggressively pursuing possibility of failed TKR. Remember, an X-ray is NOT the gold standard for diagnosing loosened implants!
Later that month: Hip replacement by Dr. Switzer.
September 2011: Visit with a Dr. “Martin” who sees no cause for leg/knee pain; sees no spine problem.
MISTAKE: Letting another three months lapse.
Later that month: Had EMG (nerve conduction study) by Dr. Mueller, showing some nerve damage, and MRI of low back.
MISTAKE: Waiting this long for an EMG; this test should have been recommended early on, even though ultimately, in my father’s case, it did not reveal the root problem.
October 2011: Dr. Martin sees no cause for knee pain and does NOT recommend further investigation!
WARNING: Beware of doctors who do not make referrals for further investigation of an unresolved problem.
November 2011: A clinic specializing in minimally invasive spine surgery performs endoscopic surgery; cost is out of pocket. Quad pains alleviated but knee problem persists.
PAIN UPDATE at this point: My father’s bilateral knee pain is worse, swelling continues; walking is more difficult despite pain blocks, NSAIDs, excessive rest, therapy exercises and ice packs.
February 2012: Dr. Switzer takes X-ray of hip implant; okay, thinks knee pain is related to hip bursitis.
March 2012: Returns to original TKR surgeon, Dr. “LaPiens,” who takes X-rays and orders blood test to rule out infection. Dr. LaPiens says implants might be loose.
MISTAKE: It should not have taken 26 months to finally hear this from a doctor!
April 2012: Bone scan.
MISTAKE: It should not have taken 27 months to finally get a bone scan!
Later that month, Dr. LaPiens confirms loosened TKR. Draws synovial fluid for infection check.
New primary care doctor recommends appointment with a new orthopedic surgeon, Dr. “Ganzelli.”
May 2012: Dr. Ganzelli disagrees with Dr. LaPiens’ diagnosis of loosened knee implant, and tells my father to see him again in three months, with no further recommendation for investigation!
MISTAKE: What does Dr. Ganzelli think might happen in the next 90 days, being that for nearly two and a half years, my father has been suffering from progressive knee pain?
June 2012: Acupuncture, which didn’t work. Dr. Switzer takes hip X-ray; okay; evaluates knees, blood test for infection and inflammation are negative.
PAIN UPDATE to this point: Every three months there’s been pain blocks (not always in same lumbar region) but they haven’t done much good.
August 2012: Primary doctor and Dr. Ganzelli say new X-rays of knees are okay; suspect allergy to metal part of implants; test for this is negative.
September 2012: Consult with neurosurgeon Dr. “Chung.” Diagnosis: lateral recess stenosis, recommends traditional back surgery (screws and bolts), 75 percent sure it will resolve knee pain.
October 2012: Another ortho doctor, “Lichtenstein,” disagrees with Dr. Chung, saying he’s never seen knee pain result from spinal stenosis.
Later that month: Dr. Switzer gives Marcaine injection and more X-rays. An immediate relief of pain, following Marcaine injection, strongly points to failed TKR.
My father had instant pain relief and his walking was significantly improved. This effect wore off several hours later.
MISTAKE: Why didn’t any of the doctors (especially Dr. Switzer and Dr. LaPiens), recommend the Marcaine injection sooner?!
I asked this question to knee replacement surgeon whom I consulted specifically for this site; read his response.
PATIENT BEWARE: If you have persistent knee pain after TKR, you should suspect a failed implant and DEMAND a Marcaine injection! Also insist upon a bone scan. This is NOT the same as an X-ray.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/sasirin pamai
How to Do a Deadlift if You Have Golfer’s Elbow
Believe it or not, there IS a version of the deadlift that can be done if you have golfer’s elbow (medial epicondylitis).
I’ve had golfer’s elbow. Until the tendon healed, I couldn’t do deadlifts or anything that required a full-fledged grip. Or at least I thought.
If you have golfer’s elbow, you can perform the deadlift motion on a “dual cable cross” machine.

Lower the handles all the way to the floor, and set them close together (the machine must have this option) to duplicate the distance your hands would be on a barbell during a regular deadlift.
Even though you may have golfer’s elbow in only one arm, BOTH hands must be used identically in this exercise.
The medial epicondyle tendon is responsible for a gripping motion. Thus, golfer’s elbow interferes with gripping.
So instead of gripping the handles on the dual cable cross machine, you insert your entire hands through the loops of the handles, such that the strap portion of the handle (not the actual plastic handle) tugs against your wrists.
Again, BOTH hands must be positioned this way even if only one elbow is affected.
So if only one elbow is affected, you can’t grip one handle and “loop” the other; this will cause the looping side to be much shorter than the gripping side.
Palms may face towards you, towards each other or away from you (underhand loop).
Chances are, a neutral or overhand loop will cause pain, since the medial epicondyle is also responsible for wrist pronation. So use an underhand loop.
The strap portion will dig into your wrist. You might figure that gloves will solve this problem by creating a barrier, but depending on how much weight you’re pulling, the thickness of the gloves won’t be effective.
Instead, take a full-length Ace bandage and wrap securely around the wrist, then clasp it with a bandage clasp.
Place the band so that half is below the wrist crease and half is above (on the meaty portion of the palm).
Rotate the band so that the clasp is on the top portion of the wrist so that the cable strap does not accidentally knock it off.
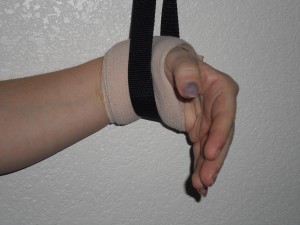
You will need to stand on some kind of perch. In my case, an 18-inch workout stool serves to mimic the range of motion that I’m used to with a barbell.
Get on the stool, squat to reach a handle, pull it towards you and insert your hand through the loop; repeat with other hand.
Position yourself as you would when setting up for a barbell deadlift, then straighten.
My deadlift stance fits perfectly on the standard 18-inch exercise stool. If your stance is wide, use a step-class stepper, adjusting the height with “risers.”
Unfortunately, this will be a hassle, as it will require quite a few risers, especially for six-footers.
The dual cross cable wrist deadlift will feel awkward at first, but it’s the next best thing if you have golfer’s elbow.
Believe me, I have experimented with everything possible. As long as you don’t feel discomfort, you will not aggravate your golfer’s elbow.
Initially use very light resistance to get used to this; do not make a dramatic jump in weight load.
You’ll need to experiment to figure out which weight load most duplicates your regular deadlift.
Don’t try the “grip by the wrist” maneuver on a Smith machine; I’ve tried it and it’s a no-go.
Alternative Modification for Deadlifts
Deadlifts with the barbell can be done if only one elbow is affected by golfer’s.
The good side grips normally, while the affected side grips the bar with a very tight middle, fourth and pinky finger — while the index finger is completely removed from contact.
The thumb grips as much as it can to keep the bar from slipping, but not as tightly as you normally would, as this may provoke the tendonitis and may also encourage the index finger to reflexively grip the bar.
For obvious reasons, you will need to work with a lower weight. Never lift a load that elicits elbow discomfort, no matter how light.
Put your ego aside and lift whatever light weight is required to avoid causing any discomfort.
This light load may actually be light enough to eliminate the thumb as well, so that you’re gripping with only the middle, fourth and pinky fingers.
Very gradually, work up from this baseline light load as the tendon heals. This may take many months.
At some point, you’ll need to reintroduce your thumb on the golfer’s elbow side due to the increasing load as the tendon heals.
Do this ONLY if there is no elbow discomfort.
This alternative technique works — I speak from experience. But it requires patience!
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/Andrey_Popov
Should You Avoid Flip Flops? Yes, They Can Hurt Your Feet

There’s a very unsuspecting explanation for why sometimes feet hurt even though you haven’t sprained or twisted anything or worn high heels.
Next time you think of showing your bare feet in public with flip-flops, heed the warning from a doctor that this kind of footwear can hurt your feet.
The more socialized form of health care in the UK makes it easier to track the source of hairline fractures and sprains in feet:
The National Health Service there estimates that $62 million are spent every year on the treatment of 200,000 flip-flop related injuries! That’s a LOT of foot pain.
“There are limited statistics about injuries related to flip-flops because people aren’t always certain an injury is directly related to wearing the sandals,” says podiatrist (foot specialist) Dr. Alan Berman, DPM, of Somers Orthopaedic Surgery & Sports Medicine in New York.
Many people who wear flip-flops don’t care that their feet and toenails are unsightly, but maybe what Dr. Berman has to say about foot pain will make them think twice about wearing flip-flops in restaurants, at work, gyms, church, classes and while shopping.
If you still think your feet are nice to look at, or if you don’t care what people think, and thus you still intend on wearing flip-flops, at least take mind of Dr. Berman’s tips to help prevent foot pain relating to “tongs.”

Wear flip-flops only for short periods.
They offer no arch support, shock absorption or heel cushioning (says the American Podiatric Medical Association), and thus are beneficial only for basic protection from hot surfaces and in helping prevent athlete’s foot in public showers.
If your feet have been hurting you lately but you don’t recall tripping or twisting a foot during sport, consider it’s because of wearing flip-flops for extended periods.
Furthermore, it’s obvious that this type of footwear can make it easy to turn an ankle or stumble.
And you certainly can’t run very hard if you find you have to make a mad dash (e.g., running across a parking lot in the rain).
Avoid sport in flip-flops.
Dr. Berman says, “People who ran or jumped in flip-flops and suffered sprained ankles, fractures, and severe ligament injuries have required surgery.”
I see people wearing these things on hiking trails and while using cardio equipment!
Don’t wear flip-flops to cut the grass.
For obvious reasons, avoid wearing them when doing yard work.
Flip-flops can cause a litany of foot problems.
The following foot ailments can result: plantar fasciitis (painful heels), hammer toe, shin splints and metatarsalgia (causes pain in the ball of the foot).
In order to prevent tongs from slipping off your feet, you must scrunch your toes with every step to keep a grip on the tong.
This disrupts the natural gait pattern of the foot, and has a ripple effect up the lower body:
Natural stride is shortened, preventing natural “locking” of the foot, forcing the leg and hip muscles to work harder (no, this is NOT the same as exercise!), resulting in suppression of other muscles.
This chain reaction then leads to the aforementioned ailments.
Keep the rubber off the metal.
Flip-flops can actually lead to car accidents because they impair a driver’s control if they come off the foot and lodge under the brake or gas pedal, according to the American Automobile Association.
Make sure your driving footwear is not so loose that it pops off and interferes with the pedals.
 Dr. Berman has been in practice for over 25 years and provides both surgical and state-of-the-art nonsurgical care to his patients.
Dr. Berman has been in practice for over 25 years and provides both surgical and state-of-the-art nonsurgical care to his patients.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Chest Pain but Normal Test Results: What’s Next?
Find out what you should do if you have chest pain but “all the tests” are normal.
Many people have chest pain but the cardiac tests come back normal. Chest pain is the No. 1 reason for emergency room visits.
Most of these patients are told that their chest pain is not related to their heart.
“The etiology for chest pain is not always the heart, but it is so important to be sure it is not the heart!” says Dawn Kershner, DO, a cardiologist at MedStar Union Memorial Hospital, Baltimore, MD.
Dr. Kershner continues, “Chest pain can be caused by numerous GI problems, musculoskeletal — like a pulled or inflamed muscle/joint — pulmonary embolus,” which is a blood clot in the lung that can kill within minutes.
“As a cardiologist, I make sure the chest pain is not cardiac and then start looking for the non-cardiac cause.”
Do not delay; if you are having chest pain, you do have a choice: Sit or lie there wondering if it’s your heart preparing for an attack, or — you can head to the emergency room to get it checked out.
If the incident passes and you’re still alive, do not assume it’s nothing to worry about.
Make an appointment with a cardiologist and get tests done.
Now what if all the tests are normal?
This includes blood tests, EKG, echocardiogram, Holter monitor and “stress test.” A stress test can be via exercise or chemical.
After these normal test results, if you continue having chest pain, and also have other symptoms (e.g., sweating, nausea, jaw pain, back pain, labored breathing) that are well-known as being part of many heart attacks or signs of severe coronary blockage, then you need to:
- Ask your doctor about a CT angiogram.
A CT angiogram is non-invasive and will show if you have blockages in your coronary arteries.
 Board certified in internal medicine/cardiovascular disease, Dr. Kershner treats abnormal EKG and abnormal stress test among many other cardiac conditions.
Board certified in internal medicine/cardiovascular disease, Dr. Kershner treats abnormal EKG and abnormal stress test among many other cardiac conditions.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Why Some Athletes Have Higher Resting Heart Rate

Find out why it’s a myth that all athletes or gym rats have a low resting heart rate.
Do you work out hard at the gym and even do high intensity interval training, yet are mystified over your relatively high resting pulse?
A normal resting heart rate for the general population is between 60 and 100.
A muscle-building enthusiast who also does high intensity interval training, and even some miscellaneous cardio jaunts such as lengthy hikes, may still find he or she has a resting heart rate in the 70s or even low 80s – which seems high for an athlete.
What’s the reason some athletes have a higher resting heart rate?
“Most ‘athletes’ are weekend warriors or those who run daily or work out; but they are not necessarily career athletes,” says Dr. Sameer Sayeed, a cardiologist at ColumbiaDoctors of Somers, NY.
“Their level of exercise is greater than the general population who doesn’t exercise or just does light walking.
“But their exercise is not enough to cause the very low resting heart rates associated with more career athletes like Olympians or marathon runners who train every day, all year-round, and are so well-conditioned that their hearts develop the features of an athlete’s heart, with a stronger, thicker muscle and larger chamber for higher blood flow and the low resting heart rate from such severe endurance.”
Tennis great Bjorn Borg was reported to have had a resting pulse of 38, though that’s been refuted, and it was likely more like 50-60.
Many marathon runners, who are not professional caliber, report a resting heart rate in the 40s and 50s.
I asked Dr. Sayeed if the really low resting heart rate is associated usually with elite endurance athletes, and he said it is. “They do severe training daily for months to years,” he adds.
What about hardcore gym athletes who strain and severely tax their bodies with heavy weight workouts?

Though a powerlifter or bodybuilder will strain through sets that leave their heart pounding at the end, this type of training simply cannot be compared to running for two hours straight.
“They are not doing severe training like a marathoner or Olympian,” says Dr. Sayeed.
The “severity” in this case refers to how much the cardiac muscle is taxed, not how much weight the bones and skeletal muscles can move.
Serious marathoners may run 10-15 miles every day, and at a painful, nonstop pace.
Whereas the powerlifter or bodybuilder is painfully active only for a fraction of that time, even though a gym workout may last two hours. Most of that training time is spent resting.
High intensity interval training will help lower resting heart rate and has several advantages over long-distance running, for those whose goals are related to fitness and fat loss rather than completing marathons.
An athlete or hardcore gym enthusiast may have a relatively fast resting pulse due to factors that raise resting heart rate, such as ongoing stress and anxiety, caffeine, medications and smoking (yes, some gym enthusiasts actually smoke).
Finally, overtraining can elevate the resting pulse.
Signs of overtraining also include moodiness or irritability, ongoing fatigue, trouble with sleep, failure to progress, or even regression with performance.

Dr. Sayeed performs echocardiograms and stress tests at the Midtown Manhattan and Westchester offices at Columbia Doctors. He is also trained in cardiac CT imaging.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Source: runnersworld.com/community/forums/training/marathon-race-training/low-heart-rate
Knee Replacement Revision without General Anesthesia?

An orthopedic surgeon discusses anesthesia options for knee revision surgery.
Are you wondering if general anesthesia is absolutely necessary for knee revision surgery?
After all, this is quite unnerving, being that a tube is stuck down your throat (intubation) and a mechanical device breathes for you.
Good News
“Knee revision can be done under regional (spinal, epidural, femoral/sciatic block) with sedation, depending on the efficiency of the surgeon and the skills of the anesthesiologist,” says Henry Boucher, MD, clinical instructor of Adult Reconstruction, Medstar Union Memorial Orthopaedics, Baltimore, MD.
“There is some controversy whether the DVT/PE rates are lower with regional some studies show), but it is a commonly held belief,” adds. Dr. Boucher.
Reasons why a patient should have general anesthesia for knee revision surgery (or primary replacement).
Dr. Boucher explains, “Contraindications (to regional anesthesia) include elevated risk of bleeding (use of anticoagulants); certain cardiac conditions (severe aortic stenosis) where a drop in blood pressure due to proximal migration of the spinal would be very risky; some patients with extensive spinal surgery.”
Why would some surgeons prefer general anesthesia for knee replacement or revision surgery in a patient without any contraindications?
Dr. Boucher explains, “Some surgeons are reluctant to agree to regional because of 1) the time it takes to place and 2) time to achieve proper anesthesia.
“The flip side is that it can save time at the end of the case since there is no lengthy wakeup.
“Sometimes the spinal does not take—which then requires general—or requires extra time to set up even in the best of hands.
“Some anesthesia providers feel the same way and may be more comfortable with general.
“Efficiency and willingness to do regional is certainly related to the skill of the anesthesia provider.”
This has me thinking that the surgeon and anesthesiologist don’t consider what’s best for the patient in terms of blood clot risk, which includes the DVT becoming a life-threatening pulmonary embolus.
Dr. Boucher says, “Regarding DVT/PE, there is research that both supports and refutes lower rates in regional anesthesia.
“It is true that DVT/PE are major medical complications after knee replacement, but in my opinion the more pertinent risk factors are the patient’s comorbidities and post-op immobility rather than type of anesthesia.”
Dr. Boucher’s specialties are hip and knee surgery, replacement and revision, and sports medicine surgery. He has been the recipient of the Golden Apple Award for teaching excellence multiple times.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Non-Surgical Treatment of Failed Total Knee Replacement
Could there be any nonsurgical alternatives to knee revision surgery for a failed TKR?
After all, revision surgery involves just as much recovery time as the original operation.
Furthermore, knee revision surgery is more complicated than the original procedure, because the defective parts must be removed.
And there’s no guarantee that the revision won’t eventually become loosened or failed either.
Loosened Knee Replacements Can’t Repair Themselves on Their Own
“A loosened implant requires surgery to correct,” says Henry Boucher, MD, clinical instructor of Adult Reconstruction, Medstar Union Memorial Orthopaedics, Baltimore, MD.
There is just no way around this. The alternative is to live with pain, and the pain from a failed knee replacement will get worse. Your only recourse, unfortunately, is the revision surgery.
However, isn’t there anything that a person can do to take the edge off the pain if they decide not to have the knee revision surgery?
“For patients not willing or able to undergo surgery, a hinged brace and assistive device — cane, crutch, walker — can can help with comfort,” says Dr. Boucher.
Don’t confuse this with pain relief. The pain of a failed total knee replacement can be so significant that walking with these assistive devices will still be painful.
And even prescription painkillers will not be enough to make life bearable for some patients unless they decide to live their life out of a scooter or wheelchair.
In short, there are no non-surgical treatment alternatives for a failed or loosened knee replacement.
Warning Signs that Your Knee Replacement Implants Are Loosened
• Soreness, and especially a severe degree of pain, long after normal postop pain should have disappeared.
• Signs of an infected knee joint: fever, muscle aches, chills.
• Stiffness in the joint or a limited range of motion.
• Swelling or puffiness due to excess fluid in the joint.