Can HIIT Improve Your Brain Health?

High intensity interval training (HIIT) is good for brain health, especially in middle-aged people.
This study on brain health finding comes from the Montreal Heart Institute (MHI) and was led by Dr. Anil Nigam.
HIIT involves brief, but power-based bursts of cardio activity, with a few or several minutes of casual pacing in between. HIIT can be done on any cardio equipment as well as outdoors in the form of flat land sprints, jogs up steep hills or dashing up moderately inclined hills.
Dr. Nigam’s study involved six adults who did high intensity interval training twice a week for four months using a stationary bike, and strength training twice a week.

Shutterstock/Seasontime
Prior to the exercise, the participants’ cognitive skills were assessed, along with brain oxygenation. Other vitals were also measured.
“Cognitive function, VO2max and brain oxygenation during exercise testing revealed that the participants’ cognitive functions had greatly improved thanks to the exercise,” says Dr. Nigam.
It’s no secret in the brain and exercise research community that exercise (including strength training) yields considerable benefits to brain health
Even if you’re in poor physical condition, you can still do high intensity interval training from a performance perspective.
I once had an overweight client who was a smoker and had peripheral vascular disease.
Walking was painful, but she had no problem pedaling a stationary bike with full force.
I’ve had other overweight clients use the elliptical machine as well as treadmill.
On the treadmill, HIIT can be done by someone of any fitness level.
A 3 mph walk on a 15 percent incline for an obese person can qualify as a high intensity interval segment, as this will drain them after 30 seconds.
Don’t cheat by holding onto the rails; swing the arms!
Nothing beats exercise, including HIIT, for improving brain health.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: ©Lorra Garrick
Source: sciencedaily.com/releases/2012/10/121029081211.htm
Signs the Brain Tumor in Your Dog is Progressing

Brain tumor progression in dogs…
This article explains what worsening symptoms to look out for if your dog has a brain tumor, including if your dog is receiving treatment for the brain tumor.
My parents’ dog was diagnosed with a brain tumor earlier this year, a few days after suffering a seizure.
In dogs over age 5 or 6, new onset seizures are strongly indicative of a brain tumor.
The first symptoms of a brain tumor will vary from dog to dog.
In the case of my parents’ German shepherd, the symptoms were:
Sudden compulsion to walk around the kitchen island and kitchen table counterclockwise; lost enthusiasm for playing fetch, including appearing disoriented; retching; an episode of vomiting; not showing previous excitement upon seeing familiar visitors; ignoring commands to come.
All of these symptoms appeared over a period of about one week, and then the seizure came; two days later an MRI revealed the brain tumor. The dog was given 3-9 months with treatment.
To make a long story short, after we realized that the dog almost died under the care of the diagnosing vet, we switched to an alternative vet who restored the dog to nearly normal as far as behavior.
We had hope, but my brother, a pharmaceutical chemist, pointed out, “But remember what we’re dealing with: A brain tumor is a brain tumor.”
We still had hope because the German shepherd was once again reconnecting with his family.
We saw his soul in his eyes; his bark was robust; he was interactive and responsive; and the pacing diminished, though never completely disappeared.
All along he was on potassium bromide (prescribed by the first vet, but advised by the alternative vet to remain on), an anti-convulsant.
Potassium bromide’s premier side effect is a wobbly gait and hind leg weakness.
However, this is supposed to disappear in several weeks.
But my brother said that it can last as long as the dog is on this salt solution.
The dog seemed perfectly normal for a while, save for a nearly complete loss of interest in playing fetch; and some pacing here and there.
And then one morning at 2 a.m. I was awakened by a big thud; the dog was having a seizure.
I had been staying with my parents to help them treat the pet (the administration of the meds was too overwhelming for my mother to handle alone, and my father was detached from the burden).
The dog had three more seizures within 24 hours. We took him to the alternative vet for a several-day stay for observation.
The dog was released declared in good shape (but realize that the vet clinic wasn’t laid out in a way to truly observe the animal’s behavior).
However, once back home, the pacing really picked up steam.
The dog had had two strep throat infections (the first was misdiagnosed by the initial vet, and the misdiagnosis nearly killed the GS), but only the second strep infection had him spitting up.
So when he began spitting up after returning from the several-day stay, I suspected yet another strep infection.
However, I didn’t see any other classic signs of strep infection in dogs (what are they?).
This alarmed me, actually, because if the spitting up wasn’t from strep, it had to be from the brain tumor.

Shutterstock/Sergey Nivens
I began suspecting that maybe the brain tumor was beating out the alternative treatment.
The dog occasionally staggered a little, and at one point swerved leftward into the washer as though a bit intoxicated. I thought, potassium bromide. Or…?
The next day, the pacing was even more jacked up; he spent a lot of time mindlessly pacing from one end of the house to the other.
However, the dog retained a few other resurrected behaviors that the brain tumor had initially knocked out, like giving a paw upon a visual command.
The next morning my mother found a pile of poop on the kitchen floor.
This was not normal; the dog was fully trained to bark when he needed to go out.
Later that day he urinated a little in the house. My brother thought it was a side effect of a sedative that the alternative vet had given him.
The dog had also paced nonstop for an hour between 6 am and 7 am.
Next day he waltzed over to his pillow and outright urinated in it, creating a puddle, then as he walked away, continued letting out urine, slipping on it.
Even if this was a side effect from a sedative, the dog should have known to stand at the door and bark, like he always had, to signal a need to go out.
I then admitted that the treatment was no longer working. Then hindsight began kicking in:
#1) The ongoing incidents of rear leg clumsiness and tipsy gait were not the potassium bromide; this was the brain tumor. “Ataxia” is a common symptom of brain tumor in dogs.
#2) Another common symptom of dog brain tumor is when the animal misjudges objects on the opposite side that the brain tumor is at, resulting in bumping into things.
The tumor was on the right side of the dog’s brain.
And I recalled how he bumped leftward into the washer; and how not too long before that, upon proceeding to jump into the backseat of the car, instead misjudged and jumped too far left, crashing into the frame of the car.
#3) The pacing the last few days of his life was nearly nonstop (literally) and quite fast, relentless, incessant.
#4) He wasn’t barking as much, and wasn’t interested in barking on command anymore.
#5) He lost interest in his family members. We were no longer his family; we were merely food dispensers.
#6) Incontinence
My brother and I told our mother, “It’s downhill from here. He’s no longer stabilized. He’s declining.”
Our suspicions were deeply confirmed after the dog got loose (thanks to lawn care worker who left our gate open), and would not come to me as I ran after him; would not come to my father when he intercepted him with the car and summoned him to jump in; and tried to bite me when I intercepted him at one point and tried to grab his harness.
Don’t let a great appetite fool you; a brain tumor in a dog can increase appetite.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: NC State University College of Veterinary Medicine
Housetrained Dog Pooping Inside House? Causes & Solutions

How aggravating IS it that your house trained dog is pooping around your house!
This infuriates many people into believing that their dogs pooped inside the house on purpose.
I asked dog trainer Zak George, host of Animal Planet’s 2009 “SuperFetch,” why a housetrained dog might poop inside the house on occasion.
First and foremost, George explains away two major misconceptions about “potty training regression” in canines:
1) “Accidents in the house are never punishable at any age for any dog,” and 2) Dogs never defecate or urinate in the house out of spite or revenge.
So even though that pile of dog poop is disgusting and ruins your carpet, remember: Maxie did not do it on purpose.
What is the usual reason a well-trained full-grown dog would start pooping inside the house at night while masters are asleep or during day?
And why would the dog poop in a forbidden indoor area like a bedroom?
ZG: There are three major logical reasons as to why a potty trained dog would start defecating in the house in an area that they are familiar with.
One, is that there may have been a change in their daily routine such as not being let out frequently enough or perhaps being fed at a different time of day than what they are typically used to.
If this is the case, then the pet’s routine should be amended, or should be given a few days to adapt to the new routine.
Generally speaking, a healthy adult canine should be let out every three to six hours depending on their food and water intake.
The second possibility is that there has been a change in environment. In this case the issue will typically last one to four days, or when the dog has realized that the new environment is “home.”
The final reason is that there could be a medical issue. Dogs, like humans, have varying degrees of stomach sensitivity.
It’s very common for them to have a loose stool, or worse, diarrhea, when they are eating a new food.
From my experience, these issues work themselves out within two to three days.
However, if the human parent has reason to believe there may be more to it, then a visit to the vet would be advised.

Shutterstock/Sergey Nivens
What other reasons could account for a trained dog pooping around the house? Gastrointestinal ailment?
ZG: This may be a possibility. Whenever you have any questions about your dog’s health you should make a visit to the vet, just as you would take your son or daughter to the doctor if you suspected anything could be wrong.
Would age have anything to do with a housetrained dog one day up and pooping in the home?
ZG: The best thing to do is to keep an open dialogue with your vet, and if you think that age is affecting your dog’s behavior, then bring them in for a visit.
If the animal is trained to bark to get his master’s attention to be let out, why wouldn’t it bark first rather than just up and pooping inside the house?
Assume the canine normally barks when it wants to go outside to poop.
ZG: There are tons of variables to this. For example, does the dog have something wrong with his or her vocal chords? Is he or she sleep walking?
Maybe the dog is too ill to bark. Maybe the dog just doesn’t feel like barking.
Remember, dogs are living souls, and not computers that humans program.
If a human normally rings someone’s door bell upon arrival, but, for one reason or another, decides to knock instead, do we assume that the human needs to have this behavior analyzed? We could.
However, the more logical reason is that the dog’s mood is affected by something causing he or she to opt out of the usually habitual behavior.
What are the best fool-proof ways to correct the problem of a dog pooping inside the home?
Other than the obvious: no food after 6 pm; several play sessions in the evening to encourage voiding; letting the pet out before everyone goes to bed.
ZG: Like with humans, there is no “fool-proof” magic answer. If the problem persists and the above actions are taken, then there is most likely a medical issue.
If all medical possibilities are ruled out, spend lots of time outside playing fetch and experience life with them.
Praise them when they go potty outside and forgive them when they go in the house.
 Zak George is an American broadcaster and dog trainer known for various shows on the Animal Planet channel and “Who Let the Dogs Out?” for UK kids’ channel CBBC.
Zak George is an American broadcaster and dog trainer known for various shows on the Animal Planet channel and “Who Let the Dogs Out?” for UK kids’ channel CBBC.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Dogs Love Cucumbers, but How Much is Safe ?

Dogs, big and small, really do love cucumbers; they are nuts about them.
And let me tell you, I knew a white German shepherd who absolutely loved cucumbers. This dog was crazy about this elongated fruit.
The German shepherd belonged to my parents, and I’m the one who introduced him to the juicy, refreshing fruit.
The dog would eat a whole cucumber in just a few minutes.
This fruit seemed very safe for the dog to consume, as he never suffered any adverse effects from all the many cucumbers he had devoured.
And by the way, the cucumber IS a fruit, not a vegetable. It has seeds — making it a fruit.
This plant food is largely water, and the skin is loaded with phytonutrients (plant nutrients). It also has antioxidants.
Just because it’s not a protein food doesn’t mean a dog shouldn’t eat a cucumber. The cucumber, which is 90 percent or more water, contains no compounds that are toxic to canines.
In fact, according to 2.aspca.org/aspcablog, there isn’t even any data out on whether or not this fruit contains anything harmful to the canine species.
The ASPCA site does not encourage giving your pet “table food.”

However, cucumber should not be considered a “table food.”
It grows on a vine, not a table, and it’s not made in a factory.
Start by giving your dog small amounts of cucumber.
This will make a far healthier “treat” than giving your pet so-called doggie cookies that contain artificial flavors, chemical colorings and other additives.

Freepik.com, 8photo
Cucumber is also loaded with enzymes and is extremely low in calories — even a whole one.
Canines are omnivores, and there’s no reason a dog should not get some raw vegetables and fruit in its diet.
In fact, many dog foods contain vegetables, except they are not in raw form. Raw vegetation is the healthiest way to go.
Speak to your veterinarian about giving your dog cucumbers — which again, contain significant amounts of water — which is always good for your pet.
Cucumbers can also be sliced up and mixed in with dog food.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Dog Drinking Tons of Water Could Mean Serious Disease
You’d better be very worried if your dog keeps drinking tons of water and can’t seem to get enough.
Now, active dogs do normally drink a lot of water, but when this is done way too much, it can mean a serious disease in your dog.
I asked Dr. Michel Selmer, DVM, with The Caring Vet in NY, what would possibly make a dog drink tons of water other than playing a lot of ball in the hot sun.
“These clinical signs are non-specific and can be caused by many different diseases or conditions,” says Dr. Selmer.
“Usually it is the production of excess, dilute urine that results in compensatory increase in water consumption, but occasionally the condition is one of increased water intake that results in the production of large volumes of dilute urine.
“The following is not a complete listing of diseases that may result in increased thirst and urination, but it outlines the most common causes.”
Cause # 1 of dog drinking a lot of water: urinary/kidney/bladder conditions, and also conditions affecting the uterus, such as an infection.
Cause # 2 of heavy water drinking in a dog: hyperadrenocorticism, hypoadrenocorticism, hyperthyroidism, diabetes mellitus, diabetes insipidus. These are hormone related diseases.
“Liver disease, certain drugs, fever, pain and certain electrolyte imbalances may also result in increased thirst and urination,” says Dr. Selmer.

If your dog drinks a ton of water, but otherwise seems healthy and has no symptoms like lethargy, poor appetite, constipation, vomiting, etc., then assume that you have one healthy, active pet that’s simply quenching its thirst.
“Rarely, a behavioral problem is at the root of increased drinking behavior,” says Dr. Selmer.
If your dog is frequently thirsty, don’t assume this requires any kind of discipline or retraining.
Give your dog filtered or treated water. It is not healthy for dogs to drink from puddles, water in a gutter, etc.
Your dog doesn’t need environmental toxins any more than you do.
 Dr. Selmer offers conventional Western plus holistic veterinary medicine, traditional Chinese veterinary medicine including acupuncture and herbal therapy, and integrative medical care for dogs and cats.
Dr. Selmer offers conventional Western plus holistic veterinary medicine, traditional Chinese veterinary medicine including acupuncture and herbal therapy, and integrative medical care for dogs and cats.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Brain Tumor in Dogs: How Rapid is Final Decline?

How rapid is the final decline in a dog with a brain tumor?
After my parents’ dog passed following a sudden rapid decline from a brain tumor, I consulted with Dr. Peter Gordon, DVM, Dipl. ACVIM (Neurology), with Boundary Bay Veterinary Specialty Hospital in Langley, British Columbia.
My parents’ dog had almost died at the hands of conventional treatment, and we had then turned him over to an alternative DVM cancer specialist.
However, the dog eventually had to be put down, despite the excellent treatment he had, and despite the raving reviews that other dog owners (whose dogs had cancer) had about this second doctor’s treatments.
At the start of the alternative treatment, my brother reminded us that a brain tumor is a serious condition.
The dog had improved considerably with the alternative treatment, and then literally out of the blue, he went downhill to the point where we decided it best to have him euthanized.
We were blindsided and stunned at this sudden, unexpected turn for the worse. We never saw it coming.
How rapid can brain tumor progression be in a dog whose treatment is no longer effective?
Dr. Gordon explains, “This is a difficult question to answer, as there are simply too many variables to consider. Primarily, the location and type of brain tumor will have a dramatic effect on how long a tumor will take to affect or re-affect a patient.”
“Very benign tumors in non-vital locations could take a long time (months) to cause clinical signs, as there is more room to grow, and loss of a non-life threatening function may not be initially noticed.
“Conversely, a very aggressive fast growing tumor, a tumor that is very close to a vital nerve center, or a tumor that has metastasized (spread) to more than one location within the brain will not take very long to create a life-threatening condition and may disable a patient within days to weeks.”
Our dog’s sudden reappearance of signs did not suggest a life-threatening course; but did suggest that this was the end, and that if we didn’t have him euthanized, then perhaps there would be an immediate life-threatening situation — for all we knew, the brain tumor was encroaching upon the brain stem.
Dr. Gordon continues, “Second, many times initial ‘symptoms’ are missed by the family, as a dog cannot describe a headache, dizziness, memory loss, etc.
“As such, the decline may seem ‘out of the blue,’ but in fact, the reported change only represents the final stages of a slowly developing deterioration.”
The vet tech for our dog’s original veterinary neurologist, who had diagnosed the animal, told me early on that eventually, there would be a noticeable deterioration, and that it would be “rapid,” perhaps over a matter of “a few days.” This was frightening to hear.

Dr. Gordon explains, “Third, treatment side effects can play a role in the ultimate survival time, as conditions like delayed radiation necrosis can occur after an initial ‘successful’ treatment and may result in further brain damage/deterioration.
“Fourth, the presence of brain tumors can trigger other conditions such as blood clots, bleeding, cysts, hydrocephalus or intracranial swelling (inflammation) that can develop quickly, compound the effect of the tumor and ultimately lead to the patient’s deterioration.”
Though I am not a veterinarian myself — based on logic, common sense and my knowledge of our dog’s situation and what the diagnosing veterinarian had explained at the outset — I’m concluding that intracranial swelling was what caused the sudden decline.
It wasn’t necessarily the brain tumor itself, but fluid, created by the mass, invading surrounding brain tissue, disrupting the dog’s cognitive functioning.
In theory, we could have had this fluid drained and bought some more quality time with the dog. But for how long?

The first vet’s treatment involved an anti-inflammatory (dexamethasone, which helped reverse inflammation caused by the cancer), and a diuretic (which helped drain fluid buildup from the tumor).
But the dexamethasone, according to the second, alternative vet’s comprehensive testing, had “shut down” the animal’s adrenal and thyroid glands, and had made the dog so hungry that he functioned as not much more than a perpetually famished life form constantly seeking out food.
The alternative vet took him off the dexamethasone, and for the next month and a half, we had pretty much our wonderful German shepherd back.
Until one morning at 5:45 a.m. when I was awakened (I was living with my parents to take charge of the dog’s treatments) by a horrible thud: the dog was seizing…and from that point on, deteriorated.
“As such, the location, type and number of brain masses would need to be known in addition to whatever treatment modalities had been used if one were to attempt to define a prognosis or plausible survival time line for a given patient,” says Dr. Gordon.
“With these sorts of variables involved, each case must be assessed and/or defined on an individual basis by your neurologist.”
If your dog has a brain tumor and seems to have made remarkable progress, don’t take it for granted! That awful turn could occur at a moment’s notice.
Do not become complacent and smug that your dog is cured just because he’s free of signs and looks “normal.”
Don’t put off taking those pictures of him or buying that special treat, and don’t put off hugging and kissing him because you think the “brain tumor is licked.”

Dr. Gordon has advanced training in intracranial and spinal neurosurgical techniques for the correction of intervertebral disc disease, cervical vertebral instability, spinal cord trauma/fracture, Chiari malformation and brain tumor resection.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
5 Signs Puppy Vomiting Is a Medical Emergency

A prominent veterinarian describes the 5 WARNING SIGNS your puppy’s vomiting means a medical emergency.
Throwing up is common in puppies. “Some of the minor causes of vomiting include intestinal or stomach viruses, parasites, and also dietary indiscretions (eating garbage or other irritating materials),” points out Dr. Michel Selmer, DVM, with The Caring Vet in NY.
Five Signs Vomiting in a Puppy Means Seek Immediate Medical Attention
“Bloat.” The puppy’s belly is sticking out and is repeatedly throwing up; also showing signs of extreme distress, panting, drooling and retching.
This condition is called torsion and affects large breeds. It can be especially brought on by exercising your dog very soon after it eats a full meal.
The dog’s or puppy’s stomach becomes swollen; the stomach organ twists, or torques.
This life-threatening condition requires veterinary help as soon as possible; it can kill your pet.
Look at your puppy’s vomit. If the vomit contains non-edible items, do not panic.
But if in addition your puppy is straining with its bowel movements, is distressed or retching, this can signal a medical emergency.
Is there blood in the vomit? This may mean a stomach ulcer or esophageal inflammation.
Do not delay medical treatment, including if the throwing up is forceful–even if the puppy has not recently eaten.
Vomiting is accompanied by other symptoms like refusal of food, lethargy, panting, diarrhea and other distress.
This may mean a systemic infection or poisoning, or Parvo, which can kill. See a veterinarian asap.
Repeated vomiting, even with no other symptoms, is alarming and warrants medical attention asap for your puppy (or grown dog).
Did you know that repeatedly throwing up can cause life-threatening dehydration?
Do not sit back and wait to see what happens! IT IS WHAT IT IS: A puppy is vomiting.
There are other symptoms or peculiarities. Your gut is telling you this isn’t right. Get immediate medical attention.
Don’t be like my massage therapist who waited to see “if it would get worse” in her large breed. It DID get worse: Her dog died from bloat.
 Dr. Selmer offers conventional Western plus holistic veterinary medicine, traditional Chinese veterinary medicine including acupuncture and herbal therapy, and integrative medical care for dogs and cats.
Dr. Selmer offers conventional Western plus holistic veterinary medicine, traditional Chinese veterinary medicine including acupuncture and herbal therapy, and integrative medical care for dogs and cats.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Sonsedska Yuliia
Rhinoplasty: How Painful Is a Nose Job; First Person Account

Years ago I had nose surgery, a.k.a. rhinoplasty or “nose job,” and there was some pain involved.
I had a deviated septum and a past mild fracture, so a nose job was in order. It’s not pretty recovering from rhinoplasty.
But a nose job actually has little pain because painkillers dull the pain.
Thinking of getting a rhinoplasty? I say get your rhinoplasty. Mine left no scars.
My nose used to be bulbous and crooked. The fracture was either from karate, volleyball or both.
The hardest part of a rhinoplasty may be finding a plastic surgeon you can trust. I remember lying on the gurney and being given anesthesia.
Next thing I knew, I was lying with my eyes closed and sensed that the surgery was over.
My nose was packed tightly with something and I had to breathe with my mouth open.
The first week following a nose job is terrible. Though painkillers numb the pain, other things happen.
Because my nose was packed tightly with wads of some kind of material, I had to constantly breathe with my mouth open.
The sensation of the tight packing was NOT like a mere stuffy nose from the common cold. It felt like cement was jammed up both nostrils.
As a result, I was not able to sleep for longer than 20 minutes at a time, because I’d be awakened by a very dry mouth from breathing with my mouth open.
During my waking hours, I had to always have with me a little plastic saucer to cough and spit out chunks of blood and other body tissue that were leaking down my throat from my nasal passages.
Because my nostrils were packed solid, the big gobs of blood could only go down my throat and then get coughed up and out of my mouth.
The taste and sensation were horrendous, and I would cough and spit it up.
I remember being in a store, holding the saucer, when an “attack” of blood suddenly occurred.
Right then and there, I coughed chunks of blood and solid matter into the saucer, and some lady witnessed this. She kept staring.
The packing stays in for a whole week following surgery. This means that for a week, you can’t taste any food or beverages.
A few days after the nose job, my face began looking as though I had been beaten.
There was extensive bruising under my eyes, and my eyelids were swollen and bluish-purple-green. My nasal area was swollen and partially bandaged.
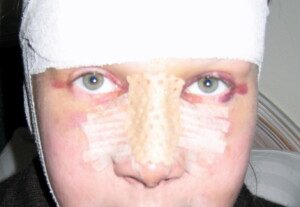
Three days postop rhinoplasty (not the author). Alison Cassidy, CC BY-SA 3.0/creativecommons.org/licenses/by-sa/3.0/ Wikimedia Commons
After the bandages come off, you’re not out of the woods. I had to massage my nose several times a day, apply a cream, and gently push my nose upward so that it would further mold into the shape that I wanted: ski slope shaped, slightly upturned.
I can honestly say I have a great nose. Most people, at least in my opinion, have a lousy one, one that turns downward; the tip being lower than the nostrils (a la Paris Hilton !).
The plastic surgeon said that the surgery fixed things so that my “snozz” will never turn downward as I get older. After all, the nose never stops growing.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/FREEPIK2
Diseases that Can Make You Smell Cigarette Smoke

Serious diseases can make you smell cigarette smoke even though nobody is smoking.
Smelling cigarette smoke or something burning can be a sign of a major illness. However, phantom smelling (be it cigarette smoke, burning rubber or something foul) is more common than you would think — and is usually nothing to be alarmed about.
Nevertheless, it is important that you get checked out by a physician who understands smell.
You should keep in mind that benign conditions, not just serious disease, can make you smell cigarette smoke or burning rubber, says Jordan S. Josephson, MD, FACS, ear, nose and throat specialist; director of the New York Nasal and Sinus Center, and author of “Sinus Relief Now.”
Smelling cigarette smoke or something burning, in the absence of burning rubber or someone puffing cigarettes, is called phantosmia.
This is smelling something foul when nothing is around to actually be causing the odor.
So what are the serious diseases that can cause phantosmia?
Dr. Josephson says, “A tumor of the brain or the olfactory nerve can also cause phantom smells, decreased or absent sense of smell (hyposmia), or bad sense of smell (known as parosmia).”
Brain tumors in these locations are not the only alarming conditions that can lead to smelling cigarette smoke or burning rubber in the absence of these compounds.
Dr. Josephson explains, “We do know that this sensation can be related to neurologic problems such as a stroke, seizure disorder or epilepsy.
“The patient may not even be aware that they are having a seizure, epilepsy or a stroke because this (smelling cigarette smoke) may be the only symptom.
“If a brain tumor is the cause, it could be an aesthesioneuroblastoma.
“A brain tumor that would cause you to smell cigarette smoke or burning material would usually be located in the temporal lobe of the brain.”
Dr. Josephson adds, “If you suffer from recurrent or increasing episodes of parosmia [or phantosmia], then it is important for you to have this looked into by a board certified ENT doctor and/or a neurologist.”
The exam should include a CT (CAT) scan and a smell test.
If you occasionally smell rubber burning or cigarette smoke for no apparent reason, don’t panic and don’t assume you have a serious disease.
This problem is common and is often the result of many possible benign or non-serious causes including sinus infections which can be recurrent or recalcitrant.
The time to see a doctor is if the phantosmia or parosmia is persistent or frequent, and especially if it worsens. Make sure you see a board certified ear, nose and throat doctor, also known as an otolaryngologist, who understands the nose and sinus.

Dr. Josephson has taught hundreds of physicians the technique of functional endoscopic sinus and nasal surgery, and was an instructor on the faculty at the Johns Hopkins Medical Center.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Pixabay/Alexas Fotos
Brain Tumor Can Cause Smelling Something Bad that’s Not There
Prenatal Vitamins vs. Regular Vitamins: What’s the Difference?

Is this just a gimmick or is there TRULY a difference between regular vitamins and prenatal vitamins? Isn’t a vitamin a vitamin? After all, aren’t all supplements the same?
I went as far as wondering if the word “prenatal” simply referred to when the vitamins were being taken (“prenatal” meaning prior to the baby’s birth), as opposed to a special type of supplement.
I’ve always thought that the only difference between supplements was whether or not they were organic/natural or synthetic.
“Many people do consume prenatal vitamins when not pregnant,” says Randy Fink, MD, Director of the Center of Excellence for Obstetrics & Gynecology in Miami, FL.
“Many women feel they see a recognizable benefit to their hair and nails from the prenatal, and ‘prenatals’ are also marketed for women in the pre-conception period.
“But is there a difference between the prenatal vitamin and a standard multivitamin?”
The term “prenatal,” when applied to supplements, actually refers to a particular composition of the supplement, rather than a time period for taking the supplements.
Thus, there is indeed a difference in the makeup of prenatals when compared to regular, conventional supplements.
Dr. Fink explains, “The prenatal vitamin will contain slightly different doses of some of the micronutrients when compared to a multivitamin.
“For instance, folic acid and iron levels are higher in prenatal vitamins. Zinc levels are typically higher in prenatal vitamins, as is the level of vitamin C.
“But prenatals contain less vitamin A, as high doses can be toxic to a developing fetus.”
The term “micronutrients” refers to vitamins and minerals in general. (“Macronutrients” refers to carbohydrates, fat and protein.)
Iron and zinc are valuable minerals — needed for optimal functioning of the body, especially a body that is carrying a baby.
Before supplements were formulated in a laboratory, women who were pregnant somehow managed without prenatals, right? Well, perhaps not.
After all, before modern medicine, the infant mortality rate was exceptionally higher than it is today. In fact, during ancient times, it was very high.
This is why the life expectancy for primitive man has typically been calculated to be exceedingly low: The infant mortality rate is factored in, which markedly brings down the average!
In addition to the high infant mortality rate during earlier times, the rate at which women died in childbirth was far greater than it is today. Nevertheless, the human species survived and proliferated.
It’s conjecture whether or not the consumption of prenatal vitamins could have made a major difference for women before the advent of modern medicine.
However, if your OBGYN recommends prenatals, it’s wise to take this advice; supplementation according to the physician’s guidelines certainly won’t harm a pregnant woman.














































