Sudden Onset Transient Double Vision: Get to ER

Just because your sudden-onset double vision disappeared after a few minutes doesn’t mean that the cause can’t kill you.
There are many causes of double vision (diplopia), but sudden-onset, transient double vision is a different animal and almost always points to an underlying, very serious problem.
For example, this is a possible symptom of a mini stroke (TIA: transient ischemic attack).
And though sudden-onset transient double vision may have a not-so-serious cause, such as something wrong with the eye rather than the brain, this doesn’t mean you should blow this off and pretend nothing happened just because everything returned to normal after a few minutes.
Get to the Emergency Room
A physician will administer the appropriate tests to see what may have caused this troubling symptom. NEVER think, “Oh, I’ll be fine; it’s gone now.”
Thinking like this could COST YOU. A transient ischemic attack is a warning sign that a massive stroke could be lurking just around the bend.
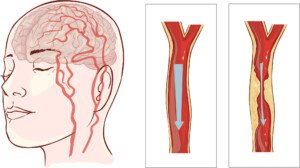
Blood flow in the brain is cut off in an ischemic stroke. Shutterstock/corbac40
Other possible causes of sudden-onset transient double vision are an actual stroke, diabetes and trauma to the head.
The ER doctor will start by taking a detailed medical history and performing a physical exam.
A neurological exam is usually next, as double vision can be linked to neurological issues – such as a TIA.
This involves checking your eye movements, reflexes and muscle strength.
Vision tests are also conducted to understand the nature of the double vision.
These tests might include tracking your eye movements and measuring how well your eyes focus and align.
Blood tests can help identify issues such as diabetes, thyroid problems or infections that could be affecting your vision.
If the initial tests suggest a more serious problem, imaging studies like a CT scan or MRI of the brain might be performed to check for tumors, bleeding or other abnormalities.
“If the symptom is truly double vision and the other causes you list are ruled out, then in otherwise healthy people a consideration would be myasthenia gravis,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“There is a simple blood test to check for this and one should see a neurologist to investigate this possibility.
“Myasthenia gravis is a condition which causes muscle weakness transiently. It can often be limited to muscles of the eyes.”
I’ll say it again: If your symptom lasted only a few minutes and you felt “fine” after that point, as though nothing happened, do not be tricked by this.
- A mini stroke, by definition, is transient.
- The next blood clot could be a full-blown stroke and permanently cripple you, if not kill you.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Erica Danger
Numbness in Tip of Middle Finger: Cause & Solution
If the tip of your middle finger has suddenly become numb, here is some reassuring news.
It’s hard to ignore numbness in the tip of your middle finger. However, the extreme locality of this should be a tip-off (no pun intended) that it’s benign and not a sign of MS or some other neurological disease.
I was inspired to write this article after I developed numbness in the tip of my middle finger.
It didn’t take long for me to connect the dots, though at first, I was stumped.
The day prior, I had placed a lot of pressure on it while doing bench dips at the gym with a lot of weight on my lap.
Below is what this exercise looks like.

Note the man’s left hand. Imagine the pressure against his middle finger as he pushes up.
When pushing up during this exercise against heavy resistance, one cannot help but press the middle fingertip really hard against the underside of the bench.
It’s nearly impossible not to do this. So how, then, might this cause numbness?
“There are two nerve branches that run along either side of our fingers,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“Numbness can occur with prolonged pressing or pressure against these small nerves, due to transient damage to the nerve.
“The medical term for it is ‘meralgia digitalgia.’” In a neurological disease, numbness would not be in such a tiny, pinpointed area in the absence of other symptoms.
If you have numbness in your middle fingertip, think very carefully what you’ve done earlier that day or the day before. I did, and at first, it didn’t come to me what I might have done to put pressure on it. Then I remembered the dips.
The fact that numbness is in only one finger and not the same finger in the other hand, in no way points to a disease! It’s quite common to exert force unequally when exercising under a heavy load.
What happens in meralgia digitalgia is that the pressure (in my case, pressure against the underside of the bench) compresses the nerve that supplies sensation to the skin surface of the fingertip.
In my case it took two or three days for the nerve to decompress and full sensation to return. There is no need for treatment other than patience.
It’s worthwhile to note that carpal tunnel syndrome can also cause numbness in the middle fingertip (my mother experienced this in both hands).
However, there will be other symptoms with carpal tunnel syndrome.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Seasontime
Can Cause of Numb Lips Be Serious Like ALS?

As innocent as a numb lip may sound, some causes can be quite serious–can one be ALS?
There are a number of causes for numbness in a lip, says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
Dr. Geraci further explains, “Have to be careful here, as some of the causes can be signs of serious problems.
“I have to be sure to inform your readers that if they have these symptoms they should see a neurologist or their medical doctor.”
Before you panic, though, review your recent history to see if there could be a benign explanation.
Were you just out in the freezing cold?
Did you accidentally bite your lip recently?
Did you have dental work earlier and the Novocain has not completely worn off?
Sometimes the lip gets very numb from this anesthetic and it can last quite a while after the procedure.
Dr. Geraci continues, “One of the more common and benign causes is due to hyperventilation.
“During heavy breathing while exercising or during anxiety, carbon dioxide becomes decreased in the blood and this cause metabolic changes in the blood that are sensed by the nerve endings–lips, finger tips and toes.”
Serious Causes of Lip Numbness
One can be a TIA: transient ischemic attack. This is a “mini stroke” or blood clot that causes temporary symptoms.
If you suspect a TIA, get to the ER immediately, as a TIA is a harbinger of a full-blown stroke (30 percent of people who have a TIA have a stroke within one year).
However, if numbness in your lip is caused by a TIA, you’ll have other symptoms with it (one or more of the following: slurred speech, facial numbness or paralysis, confusion, visual disturbance, one side of body suddenly weak, numb, heavy or paralyzed).
Another possible cause is multiple sclerosis.
If you have a numb lip from MS, you probably have some other symptoms as well (e.g. muscle spasms, balance problems, fatigue, slurred speech and vision problems).
ALS does not cause lip numbness.
Some Other Causes of Lip Numbness
- leprosy
- seafood poisoning
- trigeminal neuralgia (facial nerve irritation; cause is sometimes unknown, but may be from the nerve coming in contact with a blood vessel, MS, aging, and rarely, a tumor; trigeminal neuralgia is also accompanied by facial pain)
- shingles
- arterial spasms (Reynaud’s disease)
- low blood sugar
- mineral deficiencies
- cosmetic/soap allergies and food allergies.
That’s a LOT of potential causes for numbness in the lip. However, if all you have is a numb lip, and NO other symptoms, chances are not likely that you have anything serious.
This statement, however, is not absolute, and if your lip numbness persists, see a doctor.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
What Causes INTERMITTENT Muscle Twitching?

This article is about the causes of intermittent muscle twitching (fasciculations), not spasms.
Intermittent muscle twitching (fasciculations) is not the same phenomenon as spasms.
If you’re wondering what can be causing intermittent twitching of your muscles, here is what Dr. Anthony P. Geraci, a neurologist, says:
“This is a short answer: Benign muscle twitches are due to unstable muscle fiber membranes, usually due to injury (as when we work out). The twitching is simply a random phenomenon.”
Dr. Geraci is associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
Thus, the intermittency, in and of itself, is no cause for concern.
And don’t let the term “injury” scare you.
Every time you exercise, you injure muscle fiber membranes.
They then repair themselves, and this is one way that exercise makes you stronger.
This injury is especially caused from intense weightlifting.
Benign fasciculations come in all sorts of flavors, shapes and colors, in that they can be occasional, intermittent for a few days or weeks, intermittent for many months, ongoing for a few days, and even ongoing for much longer periods of time.
Benign fascics can also occur in response to specific activities such as hiking, using the revolving staircase, chin-ups or bench pressing.
Thus, their occurrence is contingent on how often you do these triggering activities.
Other benign causes of common muscle twitching are fatigue, emotional stress or anxiety, and mineral deficiencies.
If you have fasciculations and no noticeable weakness or other concerning symptoms like slurred speech or falling seemingly for no reason — chances are pretty high that you do not have a neurological disease (i.e., despite the fascics, you can still knock off pushups, run up and down stairs, be on your feet all day at work without a hitch, etc.).
Note, however, that “benign fasciculation syndrome” typically comes with some cramping and/or exercise intolerance, though it is not progressive or capable of causing damage to your neuromuscular system.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Strength Tests for Foot Drop, Quads, Calves, Fingers

Strength Tests for Foot Drop, Quads, Calves, Fingers
As a former personal trainer, I have designed some brilliant strength tests that should give any healthy person loads of reassurance that they are healthy.
Of course, always consult with a neurologist for a medical evaluation if you’re experiencing troubling symptoms.
But in the meantime, try out these strength tests if your “hot areas” are the foot, quads, calves and/or fingers.
Strength tests can be a fabulous way of giving you the very reassurance that you so desperately need to feel that you’re healthy — that everything’s going to be just fine!
Strength Tests for the Following
Think you have foot drop? Foot drop is literally that: a dropped foot — due to the inability of the muscles to hold it up.
This is evident when walking. The affected foot will feel as though it’s dragging or limp, or not as perky as it used to be.
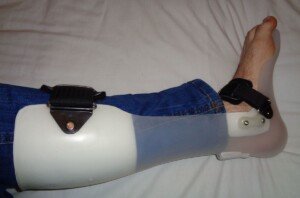
An ankle-foot orthotic (AFO) for true foot drop. Source: Foot drop Pagemaker787 CreativeCommons
Many conditions, including ALS, cause foot drop. However, there are strength tests that, if you can pull them off, will be mighty reassuring that your motor neurons are just fine. Check them out: Foot Drop
Some people with health anxiety have taken to focusing on their quad muscles or entire upper leg.
There are strength tests that target the quadriceps muscles, and if these muscles are weak due to a motor neuron disease, you will not be able to conduct these drills without knowing that something is very wrong. So check them out. Quads
Another hot area of focus among those with health anxiety is the lower leg or calves. I have some dandy strength tests for those.
Fingers and/or the entire hand are also a common area of focus.
It is so easy to see if your fingers are truly suffering from clinical weakness by conducting some straightforward strength tests. Here they are. Fingers
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Why Don’t Websites Say ALS Tongue Twitching Can’t Be Felt?

Those who fear ALS would benefit by knowing that bulbar-onset tongue twitching cannot be felt by the patient.
Bulbar-onset ALS tongue twitching cannot be felt by the patient, but are there web sites that make note of this?
How does one discover or come to the conclusion that their tongue is twitching?
Sometimes they just happen to see what appears to be a twitch when maybe applying lipstick or flossing their teeth.
Being that few people have a habit of looking at their tongue in the absence of any perceived worrisome or annoying symptoms, perhaps we should conclude that most people who report tongue twitching initially began feeling something that they concluded were fasciculations.
When a person hunts enough on the Internet for information pertaining to tongue twitching, they will come across a lot of instances in which “tongue twitching” and bulbar-onset ALS are in the same sentence.
Mayo Clinic even lists twitching of the tongue as a symptom of ALS.
Why don’t any of these sites point out that bulbar-onset fasculations CANNOT BE FELT?
I posed this question to Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
Dr. Geraci says, “I am not surprised that medical sites never point this out: It is a huge complaint I have with the medical profession; they always write about disease and symptoms from THEIR point of view and not the patient’s experience.”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Why Can’t ALS Patients Feel Their Tongue Twitching?

Though tongue twitching can result from bulbar-onset ALS, the patient never feels the fasciculations.
When a person has bulbar-onset ALS, one of the symptoms can be a twitching tongue.
These fasciculations look like worms squirming under the tongue, says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
Despite this appearance, the patient cannot feel the fasciculations. Why is this? Dr. Geraci explains:
“I think probably people who have tongue fascics don’t notice them because they are a relatively late symptom, even if the ALS is bulbar.
“By that time, the patient will have some tongue weakness which leads to difficulty eating and speaking — THIS is what they notice.
“We use our tongues so frequently that it would be difficult for someone to actually feel fascics apart from the background normal tongue movements.”
How often does the person with ALS experience their tongue twitching?
“The squirming is subtle and sporadic,” says Dr. Geraci.
He adds, “The sensory nerves are indeed feeding that info centrally.
“But we have mechanisms in our brain to filter out sensory inputs.
“And my guess — this has never been studied — is that the brain suppresses those inputs because it is focused on other ‘duties’ of the tongue like eating and speaking.”
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
What Bulbar Tongue Twitching Really Looks Like

A neurologist describes what bulbar-onset ALS tongue twitching actually looks like.
If you’re scared that you might have bulbar-onset ALS because you see your tongue twitching when you look at it in the mirror, you may be shocked at what you’re about to find out.
For the topic of what tongue twitching in bulbar-onset ALS really looks like, the expert source is Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
Dr. Geraci explains, “Twitching of the tongue is a tricky subject, and that is because the vast majority of people who think their tongue is twitching are actually experiencing something else with their tongue, which could include:
“Tingling, numbness, some rare nerve disorders (many of which are treatable; inflammatory neuropathies), and very rarely dystonia, which is a problem that stems from the brain and not the tongue muscle itself.”
Dystonia is involuntary muscle contractions.
Dr. Geraci says that the only real cause of tongue twitching is ALS, and that “benign fascics never affect the tongue.”
But hold on! Before you panic, recall that Dr. Geraci described the ALS twitching as “quivering.”
Just what does this quivering actually look like?
Dr. Geraci explains, “The quivering is very impressive in ALS; it looks like a bunch of worms squirming around just beneath the surface.
“It is much more pronounced than the normal movements we see when we stick out our tongues.”
WORMS?! Is this what you see when you inspect your tongue for hours every day?
Or do you see very brief “jerks” in specific areas, jerking that looks like twitches?
When something jerks briefly, the word in the English language to describe this is a twitch.
People see the jerk, call it a twitch, and then think they might have ALS.
“People with ALS are never aware of the tongue twitching, NEVER,” says Dr. Geraci.
So if benign fascics never affect the tongue, then just what is that twitching you see in the mirror?
Let’s look at a great analogy:
Suppose you’re nervous as sh— and are told to stand on one leg and hold the other out at some crazy angle.

What are the odds that your outstretched leg will NOT be perfectly still?
The entire unit will be tremoring. This will occur even if you’re not nervous; it’s a sustained muscle contraction; the leg is not in a relaxed state.
There will be subtle movements, no matter how hard you try to keep the leg still.
When you examine your tongue for twitching, it’s stuck out; it’s in a state of sustained muscle contraction – even if it’s poking out just a little. Add anxiety to this, and what do you get?
Dr. Geraci explains, “So, to address the anxiety, if they see twitching they are seeing the normal muscle movements of the tongue — like standing on one leg, we can’t ever really get the tongue to relax when we look at it.”
I sent Dr. Geraci a YouTube video of a twitching tongue.
Every so often in the video, there appears to be a very brief fascic in one area of it. I asked, “What’s going on with this man’s tongue?”
“The answer here gets a bit complicated,” says Dr. Geraci. “Because it is so difficult to really hold the tongue in a state of complete rest, one can’t say if the twitches on the video are fascics or an actual motor unit contraction (the motor unit being the nerve connected to the muscle fiber).
“If the motor unit sends an impulse, the twitch will occur, but that is a function of the fact that even though the tongue SEEMS to be at rest, that man had to stick it out and therefore by definition he is using the muscle and it is NOT at rest.
“So the answer I would say is that yes, a person can feel a twitch or movement of the tongue.
“But unless they are many in number — hence the quivering — it is likely that they are seeing normal contractions of the muscles from its nerve because they just can’t keep the muscle at rest.
“That is one reason we do needle EMG on the tongue; the needle can discriminate between little contractions and fasciculations.”
Dr. Geraci also says that “it is incredibly rare for tongue twitching to be the first symptom a patient would have” in bulbar-onset ALS.
“If you think you are having twitching, gently stick your tongue out in front of the mirror and look at it.
“Twitches (from ALS) will make the tongue look as though it is quivering.
“If you see this, the best advice is to have your doctor or a neurologist take a look.”
Remember, the “quivering” looks like worms squirming under there, and despite this creepy description, the ALS patient with bulbar-onset will “never” feel this quivering or twitching.
Here’s an article explaining why the ALS patient with bulbar-onset NEVER feels their twitching.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/MCarper
Causes of Twitching in Neck and Shoulder Muscles
A neurologist explains what may be causing twitching in your neck and shoulder muscles.
Have your neck and shoulder areas been twitching lately?
“For almost everyone – particularly young healthy persons — a simple twitch of a muscle anywhere in the body is completely normal and nothing to worry about,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
This could very well be the case of “Nedo,” a strength training enthusiast who posted about his shoulder twitching in a bodybuilding forum.
One person suggested dehydration was a cause, but Nedo reported that the shoulder twitching continued after drinking a gallon of water a day.
A twitching shoulder can be caused by dehydration, caffeine, magnesium deficiency, stress and exercising, including after an absence from exercise.
Lactic acid builds up from exercise in the muscle cell, says Dr. Geraci.
As this occurs, “a chain of events takes place that injures the cell and destabilizes its cell membrane. Normally, the membrane is kept stable by the single nerve fiber attached to it.”
Exercise affects the “chemical soup” inside a muscle fiber that sets off an “electrical impulse, referred to as depolarization,” says Dr. Geraci.

Shutterstock/Syda Productions
“This is the basic process that leads to muscle fiber contraction.” This fiber contraction is the twitching.
What if both the neck and shoulder are twitching?
“I see some patients who tell me about twitches of neck or shoulder muscles,” says Dr. Geraci.
“Advice on this subject would be lacking if I didn’t discuss the possibility that the ‘twitch’ is something else.
“Neck muscles generally are not stressed or worked out” from exercise, “so something else could be going on.
“Muscles of the shoulder can have twitches just from bench pressing for example, but from a neurologist’s point of view, neck and shoulder muscles can, in some instances, be considered as one anatomical unit.
“Two conditions should be considered if neck and shoulder muscles are ‘twitching.’ One possibility is that the person is having tics.
“Tics are brief jerks of groups of muscles and generally will therefore move a limb or the neck, sometimes ever so slightly that you would call it a twitch.”
Tics in adults can be caused by sleep deprivation or stress, or have no known cause.
Dystonia (involuntary muscle contractions) is the other condition, says Dr. Geraci, that can ever so slightly move a muscle in the neck that it seems like a twitch.
He explains that “dystonia can be caused by a brain tumor, Parkinson’s disease and Huntington’s, but two points:
“Exceedingly rare in brain tumor, and the other two are manifest diagnoses before dystonia sets in.
“In young people with neck dystonia it is practically always cervical dystonia alone.”
Back to neck twitching, Dr. Geraci says, “Benign tremor is fairly common and usually is inherited, so you would start by thinking about your parents and grandparents. Did they have twitching or movements of the neck or arms?
“The most common example of dystonia is something most people have heard about: writer’s cramp.
“Dystonia can be difficult to diagnose, especially in its early stages, even for a neurologist.
“It can cause the muscle to contract, again usually in groups and therefore one might notice movement of the limb or neck.
“The movement in the neck can be so subtle as to look like a brief twitch or even a rhythmic tremor.”
Dr. Geraci recommends having a neurologist examine you if you’re having excessive movements or twitching in the shoulder or neck muscles.
Tics and cervical dystonia are treatable, so early diagnosis is important.
 Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
Dr. Geraci is also the director of neuromuscular medicine at Northwell Health in New York.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: forum.bodybuilding.com/showthread.php?t=947596&page=1
Why You Get Paralyzed During Sleep and Why It’s Harmless
Don’t be frightened of “sleep paralysis,” but instead, embrace it!
Have you awakened in the morning to find that your body is totally paralyzed?
I have! And I love it!
“Almost everyone has had the experience of being jerked awake just as they are falling into light sleep,” says Anthony P. Geraci, MD, associate professor of neurology at Donald & Barbara Zucker School of Medicine in New York.
“It feels as if someone has shaken you awake. These jerks are common and a normal part of the earliest stages of sleep and they are called hypnogogic myoclonic jerks.
“Not to worry – these occur as a part of the center of your brain, called the thalamus, starts to shut down your motor system.
“This occurs as a protective mechanism, and in fact we are essentially paralyzed during about 75 percent of normal sleep.”
Sleep Paralysis Is Normal
It’s believed by researchers and physicians to be a protective mechanism against physically acting out our dreams.
However, it’s only fair that I mention that those who are authorities on out-of-body experiences (astral projection) believe that sleep paralysis is either the astral body re-entering the physical body, or, it’s a launching pad for an astral projection.
Now you can be a skeptic, but here’s a phenomenon that I can’t explain with my OWN sleep paralysis:
Every single time I have sleep paralysis, it follows a lucid flight dream! I find it extremely odd that my SP has never, ever followed a regular dream.
These lucid flight dreams of mine are spectacular in terms of imagery and experience, and I always feel that these excursions actually happened.
I have been told by those who’ve had out-of-body experiences that these are astral projections. I’d sure like to think so.
I can pop in and out of SP once it runs its course (a few or several minutes). If I wait too long to pop back into it, the window of opportunity for this closes.
Bottom line: Sleep paralysis does NOT mean anything is wrong with your body.
Dr. Geraci adds that myoclonus jerks do not happen during deep sleep.
“They can happen to some people during light sleep stages such as REM (rapid eye movement), but if you experience these occasionally, just roll over and go back to sleep.
“You’re just fine and these movements have nothing to do with your muscles.”