Vomiting During or After Exercise: Causes & Solutions

A doctor offers a very interesting cause of vomiting during or after exercise.
“That can happen when a person is very toxic, so when the circulation improves, then the lymphatics start moving and dumping toxins,” explains Carolyn Dean, MD, ND – Medical Advisory Board Member of the non-profit Nutritional Magnesium Association at nutritionalmagnesium.org.
“Vomiting is one way for the body to eliminate toxins.”
When I was a personal trainer, several of my clients upchucked a little towards the end of their workout session.
They were not what I’d call “physicalky fit” individuals. I worked them pretty hard, but kept a close watch on them to make sure they weren’t feeling sick.
The clients were beat towards the end of the exercise session, and only then did the vomit come.
My conclusion was that they hadn’t nourished and hydrated themselves well prior in the day.
In fact, one of these clients had nothing to eat all day prior to her evening workout with me.
Others reported having hardly eaten all day. This, combined with being out of shape or not being used to a strenuous workout, caused nausea, leading to vomiting.
A poorly conditioned person on the SAD (standard American diet) has a more toxic body than a physically fit person who’s been eating healthfully.
Additional Causes of Vomiting During or Shortly After Exercise

Shutterstock/MikeSaran
Motion sickness can lead to upchucking, such as the motion experienced when twirling around in a dance-based group fitness class, or even from some of the pivoting motions of a step aerobics class.
GERD (gastroesophageal reflux disease) can cause a queasy feeling from the acid jostling around as it refluxes back up the stomach and food pipe.
Exercise decreases blood flow to the cells of the digestive tract. A de-conditioned person is less able to tolerate this, and nausea can result.
Quite simply, improving one’s physical condition will resolve this issue.
There are those who can strenuously exercise on an empty stomach (morning workout) with little hydration, and not feel the least bit queasy.
Ending a grueling exercise session abruptly. A warm-down is important.
Then again, vomiting after abruptly ending a hard-hitting exercise session goes back to lack of conditioning.
A woman who doesn’t know she’s pregnant and exercises hard can also find herself vomiting at some point.
To avoid vomiting during or after exercise:
1) Take time to warm up; don’t dive into the workout full-force.
2) Par back on intensity to give your body a chance to get fitter.
3) Have some fruit or juice before the workout.
4) Have water before, and every 15 minutes, during the exercise.
5) Stick to a plant-based diet with strict limits on processed foods.

Dr. Dean, in practice for 35+ years and author of “The Magnesium Miracle,” is also a naturopath, nutritionist, herbalist, acupuncturist, lecturer and consultant.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Burning Lungs, Coughing after Hard Running: Benign Causes

There are several benign causes of burning lungs & coughing after hard running, and what’s “hard” is subjective.
“Burning in the lungs and coughing after hard running are likely due to magnesium deficiency,” says Carolyn Dean, MD, ND – Medical Advisory Board Member of the non-profit Nutritional Magnesium Association at nutritionalmagnesium.org.
“Magnesium makes muscles work properly, allowing calcium to cause muscle contraction and then pushing calcium out of the muscle cells to allow the relaxation phase.
“When there is a lack of magnesium, muscle cells in the bronchial tubes can go into spasm, tighten up and cause wheezing and burning and coughing.”
Try a magnesium citrate supplement in powder form. Follow directions; usually it’s one teaspoon twice per day.
Other Benign Causes of a Burning Sensation in the Lungs (with or without) a Cough after Running
Exercise-induced acid reflux. Wait 60-90 minutes after eating (even if it’s just an apple) before running and see what happens.
Exercise-induced asthma. This too is a possibility.
Being out of shape. Being de-conditioned can result in blood vessel constriction and excess mucus after you stop running, causing a burning feeling in the lungs and possibly a cough.
Solutions
See a physician if you suspect exercise-induced asthma. As for reflux, this may diminish over time as your body gets more physically fit.
In general, poorly conditioned lungs will “burn” after you do a level of running that you’re not used to.
This situation is quite common. And see how a magnesium supplement works.
Two of my personal-training clients, men in their 20s, experienced this lung burn after they worked out hard (high intensity interval training) on the elliptical machine, something they hadn’t done before.
Though this isn’t the same as running, it was still hard work that their lungs and GI tract were not used to.

Dr. Dean, in practice for 35+ years and author of “The Magnesium Miracle,” is also a naturopath, nutritionist, herbalist, acupuncturist, lecturer and consultant.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Tiny White Bump Inside Lower Eyelid, Painless
I asked my dermatologist what the very tiny white bump on the inside of my lower eyelid might be.
A “tiny white bump” on the inner lower eyelid can be a rather broad description.
But in my case, the very small white bump was about one and a half or so millimeters. It was painless, didn’t itch; I didn’t feel it in any way.
I noticed it when I one day slightly pulled down my lower eyelid to see if anything was where my lower eyelid meets the white of the eye, because there was an irritant in my eye.
I figured there was an eyelash there. That’s when I noticed a very small white bump, almost like a nodule.
For many months I’d periodically check it to see if it was changing in any way, and it always looked the same. This was reassuring.
Dermatologist
Finally when I saw my dermatologist for a routine skin check, I asked her what it was. She didn’t hesitate to say it was a cyst.
If you have any kind of white bump in your eyelid that’s causing symptoms, a scratchy feeling, swelling or is evolving especially, do not hesitate to see a dermatologist.
A dermatologist is more qualified to diagnose this than is an ophthalmologist — because it involves the skin, not the actual eyeball.
Now think about that for a moment. The eyelid is not part of the eye; it’s part of the skin. This includes the inner portion of it.
Yes, it’s right up against the eye, but that doesn’t change the fact that it is SKIN tissue. See a dermatologist.
“Diagnostically speaking, tiny white bumps in the lower eyelid are most likely to be either a hordeolum (stye) or chalazion,” says Tejas Patel, MD, a board certified dermatologist with AdvantageCare Physicians in New York.
“A chalazion is a noninfectious obstruction of the oil glands of the eyelids,” continues Dr. Patel.
“The benign cysts usually develop after abnormally thick oil gland secretions due to gland obstruction.
“A chalazion is usually not painful and usually develops further back on the eyelid than a stye.”
My cyst eventually disappeared on its own.
“A hordeolum (stye) is usually a pyogenic infection, most prevalently caused by staphylococcus,” says Dr. Patel.
“These benign cysts usually result from obstruction and infection of an eyelash follicle and adjacent gland. Styes are usually very painful.”
If you have a stye, applying a warm, moist compress for about 10-15 minutes several times a day can help loosen it, promoting drainage.
Gently massage the area with clean hands to encourage drainage. If there’s no improvement, consult with your dermatologist; don’t squeeze the stye.
A tiny white bump inside the lower eyelid is not likely to be something worrisome, but it’s always reassuring to get a benign diagnosis from your doctor.
 Dr. Patel treats all skin types and welcomes the most challenging skin problems. Dr. Patel specializes in both medical and cosmetic dermatology, and treats patients of all ages.
Dr. Patel treats all skin types and welcomes the most challenging skin problems. Dr. Patel specializes in both medical and cosmetic dermatology, and treats patients of all ages.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Why So Many Pulmonary Embolisms in Hospitals Are Fatal
Many pulmonary embolisms in hospital settings cause sudden death without symptoms, but many people die even when there are warning signs.
You may be thinking that it takes about four minutes for irreversible brain damage to occur when a patient has been deprived of oxygen (airflow blocked by a massive pulmonary embolism).
You may then be thinking that between symptom onset and death, medical personnel have four minutes to re-establish airflow.
However, people in hospitals have died from a pulmonary embolus even when there was more “brain time” involved.
In that case, the patient was still conscious and breathing (albeit very labored) after initial PE symptom onset.
“Massive PEs or saddle embolisms have a high risk for being fatal in any setting,” says Paul Lucas, MD, a surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
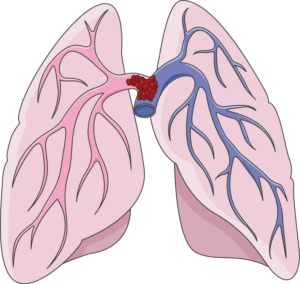
A “saddle” pulmonary embolism, plugging up the point at which the pulmonary artery branches off into each lung. Death can occur suddenly. Laboratoires Servier, CC BY-SA 3.0 /creativecommons.org/Wikimedia Commons
“Events occurring in a hospital, or at any site for that matter, require a trigger of a sequence of events to occur …. time of event to intervention,” continues Dr. Lucas.
“Although we would all like this to be instantaneous, it does take time. Every effort is made in these emergencies to expedite this.”
Treatment of Pulmonary Embolus Has Risks
“Keep in mind, you have to have a strong suspicion/diagnosis for this entity to just administer “clot busters,” as other things can have similar presenting symptoms,” says Dr. Lucas.
“You certainly don’t want to give ‘clot busters’ to someone whose symptoms are from that of bleeding.”
Here is what Steven Elias, MD, a vein specialist with Englewood Health in NJ, says:
“Before starting any therapy [i.e., blood thinners) that has significant risk such as intracranial bleeding (bleeding in the brain), most MDs would like a definitive diagnosis.
“If a patient survives a ‘massive PE’ and doesn’t immediately die, there is usually time for a CT scan which takes about 1-2 minutes.”
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Can You Get Deep Vein Thrombosis DURING Air Travel?
Two doctors weigh in on getting a DVT while on the airplane.
Perhaps you’ve heard of cases in which a person seemingly developed a DVT at some point after landing from air travel.
There are cases in which the patient becomes aware of leg pain and swelling while in a hotel or shortly after arriving back home.
“Yes, you can develop DVT during air travel, or any travel for that matter that requires long periods of immobility,” says Paul Lucas, MD, a surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
DVT Risk Factors Aboard a Plane
“The risk increases with the length of flight,” says Steven Elias, MD, a vein specialist with Englewood Health in NJ.
A very long trip in an airplane will encourage sleeping — which means very inert legs in a cramped space, unable to move about as they normally would when a person sleeps in a bed.
Dr. Elias adds, “The nature of air travel: immobility and dehydration secondary to cabin air low humidity add to the risk. DVT risk goes up significantly in flights longer than four to six hours.”
Shortest amount of time between takeoff of the airplane and DVT formation?
Dr. Lucas explains, “As far as the shortest amount of time to develop a DVT on the flight, that’s hard to pin down, and the reality is, it could be at any moment, but increased with the longer periods of immobility.
“Keep in mind though, the incidence of in-flight DVT is pretty low overall.”
Tips for avoiding a deep vein thrombosis while flying:
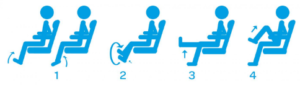
Stay hydrated, avoid liquor, get up every hour — no longer — and walk up and down the aisle
And, while seated you can regularly flex your feet up and down, which will stimulate blood flow in the calves. See the illustration below.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
Dr. Elias is a leading name in venous disease, minimally invasive vein disease therapy and clinical vein and wound research. Dr. Elias lectures about all aspects of venous disease nationally and internationally.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
How Common Is Headache in Chronic Subdural Hematoma?

Headache incidence varies depending on the age of the patient with chronic subdural hematoma.
A report in the Postgraduate Medical Journal states that the incidence of headache, as a symptom of chronic subdural hematoma, varies among different studies. The variance range is 14 percent to 80 percent.
The report points out that headache is less common a symptom in the elderly with chronic subdural hematoma than in younger patients. There’s a few reasons for this.
As the brain ages, it shrinks.
This is called age related brain atrophy. A shrunken brain means more intracranial space or room for the leaking blood to take up before pressure builds up on the brain (causing headache).
In a young person, there isn’t as much room for the leaking blood to fill, making headaches more likely as a first symptom.
This doesn’t mean elderly patients can’t get headaches from a chronic subdural hematoma.
In fact, my elderly mother’s first symptom complaint was of a horrible headache—later that day she was diagnosed with chronic subdural hematoma (from a fall six weeks prior in which she hit her head).
The Postgraduate Medical Journal then notes that the second reason is that in the elderly, there’s an “earlier onset of confusion,” and this “attracts medical attention before the development of headache” in elderly patients.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Monkey Business Images
Source: bmj.com/content/78/916/71.full
Chronic Subdural Hematoma Symptoms: Young vs. Old Patients
Yes, there tends to be differences in symptoms of chronic subdural hematoma in young patients vs. elderly.
A report in the journal Injury points out differences in symptom presentation of chronic subdural hematoma in young patients (under age 40) and elderly (over age 75).
Young Patients with Chronic Subdural Hematoma
The researchers observed particular characteristics of symptoms: a higher incidence of headache, and a higher incidence of vomiting, along with a shorter time span between initial trauma and corrective surgery.
Elderly Patients
They tended to have symptoms relating to change in mental status, deficits in motor control and larger collections of blood in the brain.
Pertaining to the patients in this analysis, there was no statistically significant difference in the rate of surgical complications.
Just what is a chronic subdural hematoma?
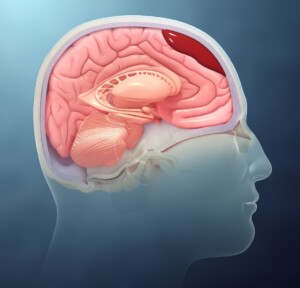
Depiction of a subdural hematoma. Scientific Animations, CC/BY-SA/Attribution-ShareAlike 4.0 International
A chronic subdural hematoma is a type of brain injury where blood collects between the brain’s surface and the dura mater, the outermost layer of the protective coverings of the brain.
It’s significantly more common in people over 65 vs. middle age and especially younger adults.
Unlike an acute subdural hematoma, which occurs suddenly due to trauma and involves rapid bleeding, a chronic subdural hematoma develops over weeks or months.
This slower progression happens when small veins between the brain and the dura mater are torn, often due to minor head trauma or even spontaneously, particularly in individuals with weakened blood vessels or elderly people on blood thinners.
Brain shrinkage due to age is the primary reason people over 65 are much more likely to suffer from a chronic subdural hematoma.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/wavebreakmedia
Source: injuryjournal.com/article/S0020-1383(02)00020-7/abstract
Soft Plaque Rupture, Chest Pain, Low Heart Disease Risk?

Can chest pain in a physically fit person with low heart disease risk be caused by a soft plaque rupture?
“Recent literature suggests two different kinds of plaque: calcified plaque which is considered more stable and less likely to rupture; and soft plaque which is considered to be more lipid-laden and more likely to rupture,” says Monica Reynolds, MD, a cardiologist with ColumbiaDoctors Medical Group in White Plains, NY.
The coronary calcium score test measures only the calcified plaque, and the amount is converted to a numerical value.
There is a strong correlation between numerical value and likelihood of heart disease and near-future cardiac events.
However, in a person with a low or zero calcium score, or, to put another way, very little “sludge” in their coronary arteries, it’s not impossible for them to experience a soft plaque rupture.
After all, the soft plaque in a fit, nonsmoking athlete with a healthy lifestyle is just as “unstable” as the soft plaque in a sedentary, diabetic, junk-food eating person with high blood pressure.
The classic cause of cardiac chest pain other than heart attack is a condition called angina.
This is when blood flow in the coronary artery is temporarily restricted, causing chest pain (and sometimes shortness of breath).
Usually there’s a trigger, namely physical exertion and/or high-charged emotions.
But I wondered about chest pain from a soft plaque rupture that resolves after a few minutes, something that might explain a sudden unfolding of chest pain for no reason (no physical exertion) that then goes away after a few minutes or so.
Obviously, a rupture is more likely to happen in a person with a ton of soft plaque versus in someone with a small amount. But having a small amount of soft plaque doesn’t guarantee no rupture.
How do you know if that recent chest pain was a soft plaque rupture?
Especially if you have low risk for heart disease?
“As with any biological system, there really is no ‘rule’ – only trends,” explains Dr. Reynolds.
“Obviously, those with risk factors TEND to develop more extensive coronary disease sooner than those without risk factors. But no one is guaranteed not to get coronary disease.”
Heart Attack & Plaque
“Many years ago, it was felt that most plaque builds up gradually over years until it eventually reaches a critical mass in obstructing the blood flow and the patient develops symptoms,” says Dr. Reynolds.
“More and more, however, we have come to appreciate that plaque buildup is not really a smooth process but can be described as a series of small ‘eruptions’ followed by healing.
“A small bit of plaque in an artery ‘ruptures’ and exposes the undersurface to the bloodstream where platelets and other clotting factors are stimulated to repair the rupture.”
- What happens when you pick off a scab?
- The scab is replaced by an even bigger scab.
“In a similar way, when the ruptured plaque is repaired, the new plaque is a little larger,” continues Dr. Reynolds.
“With repeated ruptures, the plaque can eventually reach critical mass and cause symptoms which prompt a cardiac workup and can lead to elective catheterization and stenting.
OR – the rupture can lead to such a vigorous platelet and clotting factor response that the artery goes from having mild non-obstructive plaque to total occlusion [blockage] in a matter of minutes.
“An acute rupture is now considered the mechanism for many of the patients who present with an acute heart attack or unstable angina.”
What are the odds that any given chest pain can be a soft plaque rupture?
This question applies to chest pain that doesn’t have an apparent trigger.
For example, mild chest pain can result from the motility of fecal matter building up through the large colon.
Some of the large colon runs in the upper abdominal area, so if a good chunk of BM is being transported through, it can cause mild chest pain.
The chest pain will gradually vanish, and then you’ll realize you have to do a big No. 2.
Acid reflux causes chest pain. Does it occur only when you lie down? That’s a tip-off, though acid reflux can hit when you’re upright.
Does “chest pain” occur only upon exhalation or inhalation? It’s likely a strained muscle or inflamed cartilage.
What about occasional chest pains that come out of the blue?
“Could it be plaque rupture and angina?” says Dr. Reynolds. “Maybe …. but I wouldn’t start with that. Each person is unique. Each comes with his/her own set of risk factors.
“Life is full of aches and pains. The overwhelming majority are NOT life-threatening. Common sense must prevail or we will be spending every waking hour in the hospital ER.”
Dr. Reynolds regularly sees patients for chest pain. “Very rarely is it ‘classic angina’ – it is usually some atypical presentation.
“Each time a patient comes in for an evaluation of chest pain, I do a complete history and get a good description of the pain.
“I do a physical exam and check the EKG. I assess the risk factors. If there is a moderate risk for heart disease, I will refer for a stress test and sometimes (not often) in patients with atypical pain, the stress test is positive.
“Those patients often go on to have a cardiac catheterization and some get a stent.
“And guess what – it is not uncommon that the patients with really atypical pain [who underwent stenting] come back to my office a few weeks later and STILL HAVE THE PAIN.
“Why? Because the pain wasn’t cardiac to begin with, but we just happened to find some coronary disease because, guess what – coronary disease comes with age!”
Kick Back the Soft Plaque
“Bottom line – do not walk around in a state of overwhelming anxiety about what might pop up around the next corner,” says Dr. Reynolds. “Eat right. Exercise. Don’t smoke. Enjoy life.
“Anxiety can only make everything worse – raise your BP and cholesterol, age you faster and maybe even accelerate heart disease. No one is immune to heart disease. But you must keep this in perspective.”
A hardcore overhaul of dietary habits can reverse soft plaque buildup.
Add rigorous exercise and you’ll reverse any heart disease even faster.
Think of all the exercise people did before machines took over.
 Since 1992 Dr. Reynolds has practiced clinical cardiology at ColumbiaDoctors Medical Group, one of the largest multi-specialty practices in New York State.
Since 1992 Dr. Reynolds has practiced clinical cardiology at ColumbiaDoctors Medical Group, one of the largest multi-specialty practices in New York State.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Hriana
Do Doctors Give too Many Tests for Heart Disease?
What does a cardiologist have to say about the belief that doctors order too many tests for heart disease?
These tests include stress tests and angiograms.
There are also various blood tests related to diseases of the heart.
“Recent data has confirmed that we are over-testing our patients,” says Monica Reynolds, MD, a cardiologist with ColumbiaDoctors Medical Group in White Plains, NY.
“Regular echocardiograms and stress tests in patients with low risk profiles and atypical symptoms do NOT prolong life or improve quality of life.”
A low risk profile might be a man or woman under age 45 who does not smoke, does not have diabetes, does not have high blood pressure and is not overweight.
Another example of a low risk profile is a 55-year-old man who has always been an exercise enthusiast, has none of the problems mentioned above, is only a little overweight and has no family history of early-onset coronary artery disease.
What about stenting in patients with blocked arteries but no symptoms?
“In fact, stenting arteries that are partially blocked but have not caused symptoms does NOT prolong life or improve quality of life,” adds Dr. Reynolds.
The CT Angiogram
This non-invasive but radiation-emitting procedure involves looking at the inside of coronary arteries via the use of a contrast dye that lights up blood vessels on an imaging screen.
The CTA can view soft plaque buildup inside the arteries. Soft plaque is unstable in that a piece of it can break off and block blood flow or trigger a clotting mechanism that obstructs blood flow in the heart.
Dr. Reynolds explains, “CT angiograms looking for soft plaque is of very debatable use in a patient with a low cardiac risk profile and only atypical symptoms.
“Patients are better served by changing their diet, exercising more, and taking medications when necessary to reduce cardiac risk.”
 Since 1992 Dr. Reynolds has practiced clinical cardiology at ColumbiaDoctors Medical Group, one of the largest multi-specialty practices in New York State.
Since 1992 Dr. Reynolds has practiced clinical cardiology at ColumbiaDoctors Medical Group, one of the largest multi-specialty practices in New York State.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ Satyrenko
Does Spinach REALLY Cause Black Stools?

Here’s a detailed look at black stools being caused by spinach.
Have you recently looked into the toilet bowl and noticed that your poops were black?
Did you panic?
Did you realize you recently ate spinach?
Spinach may cause stools to appear black. However, in my experience, I have another explanation.
I juice a lot of spinach, enough to sometimes make an 8 ounce glass of juiced produce that includes fruits and greens.
Drinking all that deep green from the spinach can have a striking effect on the color of your stools.
One day I noticed my BMs were nearly black — not like the color of coal, but near black enough to grab my attention.
I had ingested a larger-than-usual amount of spinach.
With a spoon I removed some of the BM, brought it towards the light above the sink and closely inspected it with my eyes.
The stool matter, turns out, was NOT black. It was very, very dark green. I mean REALLY DARK GREEN.
Have you ever seen a blackish-green car? It was kind of like that.
“Spinach contains iron,” says Lawrence Hoberman, MD, a board certified gastroenterologist and creator of EndoMune probiotic products.
“Large servings can cause the stools to be dark, but generally not black.”
Do not let this experience stop you from eating spinach!
Spinach is one of the healthiest-for-you vegetables.
It’s packed with essential vitamins and minerals like vitamins A, C and K, as well as folate, and of course, the iron.
This superfood is also rich in antioxidants, which help protect your cells from damage.
Also, it contains fiber, which supports digestive health.
Plus, spinach is super low in calories, making it an excellent part of a weight loss plan.
So next time you see what appears to be black poops in the toilet bowl, remove some with a spoon and give it a close visual inspection under a good light source to see what color it really is.













 With 40+ years’ experience, Dr. Hoberman is an expert in probiotics. He has extensive first-hand experience treating a variety of digestive health issues and has seen the dramatic results probiotics have had on his patients. endomune.com/meet-dr-hoberman
With 40+ years’ experience, Dr. Hoberman is an expert in probiotics. He has extensive first-hand experience treating a variety of digestive health issues and has seen the dramatic results probiotics have had on his patients. endomune.com/meet-dr-hoberman
































