Ripping Chest Pain: Get to ER ASAP! This Could Kill You

Ripping, Stabbing Chest Pain that Suddenly Occurs: Get to ER, Stat
A stabbing, severe kind of chest pain that suddenly comes on isn’t necessarily caused by a heart attack.
But this doesn’t mean it can’t be life threatening. It very well CAN be.
Think Aortic Dissection
“Stabbing or ripping chest pain always raises the specter of what we call ‘aortic dissection,’ says Dr. John A. Elefteriades, MD, William W.L. Glenn Professor of Surgery, and Director, Aortic Institute at Yale-New Haven, New Haven, CT.
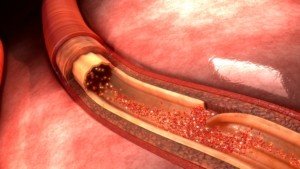
Schematic of an aortic dissection. Shutterstock/sciencepics
“Aortic dissection means internal tearing of the aorta, separating the inner from the outer layers of the aorta,” continues Dr. Elefteriades.
“This is exactly a ripping apart of the layers of the aorta, just as the term implies. This is a very serious condition that usually requires an immediate operation.”
Aortic Dissection Cannot Resolve on Its Own
This situation never self-corrects. It only gets worse; the course of it will lead to death 100 percent of the time … unless it is promptly treated—and treatment is always surgery (which may be open heart or endovascular).
Taking ground-up aspirin or a nitroglycerin pill would be useless in the event of an aortic dissection.
So would chest compressions, because the blood that should be pumped to the body’s organs is spilling out of the aorta and filling up the chest cavity.
An aortic dissection results in massive internal bleeding. Some patients will die within minutes.
However, there are others who have had a delayed visit to the ER visit, not realizing how serious their situation was, and because the dissection was of a slower nature, they survived despite delaying the ER visit by up to a few days.
But don’t assume that can be you, even if the pain kind of feels like it has subsided a bit. Don’t take any chances. Just get to the emergency room.
A “slower” dissection will ultimately lead to death if it is not surgically repaired.
So if you or someone you know has been complaining of agonizing or ripping chest pain, don’t wait another second in getting to the ER.

Formerly the chief of cardiothoracic surgery at Yale University and Yale New-Haven Hospital, Dr. Elefteriades is working on identifying the genetic mutations responsible for thoracic aortic aneurysms. He is the author of over 400 scientific publications on a wide range of cardiac and thoracic topics.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Freepik.com
Can Severe Persistent Chest Pain Be Caused by Cancer?

Persistent and especially severe chest pain usually gets people worrying about their heart, but this symptom can also be caused by cancer.
“Chest pain is abnormal and important and must be reported to a doctor,” says Dr. John A. Elefteriades, MD, William W.L. Glenn Professor of Surgery, and Director, Aortic Institute at Yale-New Haven, New Haven, CT.
“As everyone knows, chest pain felt under the breastbone can be a sign of angina or heart attack,” continues Dr. Elefteriades.
“Angina indicates that the heart is receiving inadequate blood flow due to arteries blocked by arteriosclerosis.”
Arteriosclerosis is hardening of the arteries from plaque buildup.
“Angina usually comes on with exertion or emotion. Women and men feel chest pain differently, as shown in the accompanying diagram (to come).
“Chest pain can also indicate an aneurysm of the aorta, the main artery of the body. This pain is usually non-exertional.
“If felt in the front, it indicates involvement of the ascending aorta in the front of the chest.
“If felt in the back (between the shoulder blades), it indicates involvement of the descending aorta in the back of the chest.”
An aneurysm is an abnormal enlargement of a blood vessel; the enlarged area is weak and prone to rupture or dissection — a life-threatening situation that requires immediate surgery.
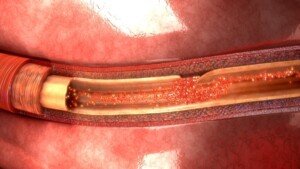
A tear in the inner lining of the aorta. Shutterstock
“Chest pain can also indicate that there is a lung cancer impinging on or invading the chest wall.”
As the tumor grows, it may spread to nearby structures, including the chest wall, causing discomfort or pain in the chest area.
This type of pain is often persistent and may worsen with movement or breathing.
Additionally, the pain can be accompanied by other symptoms such as persistent cough, weight loss, shortness of breath or blood in the sputum.
Can persistent chest pain have a non-serious cause?
Dr. Elefteriades continues, “Chest pain can also be benign, from inflammation of the costal cartilages, the soft bone that connects the ribs to the breastbone in the front of the chest.”
This is called costochondritis, and athletes who have this have been known to report that the pain is quite severe.
The pain associated with costochondritis, even though it has nothing to do with the heart, is typically sharp or aching and may vary in intensity.
It is often exacerbated by certain movements or pressure on the chest, such as coughing, deep breathing or physical activity.
The discomfort can also be tender to touch in the affected area, which is often found along the upper ribs.
“However, if you are having chest pain, you must report this and have it checked out,” urges Dr. Elefteriades. Especially if it’s persistent.

Formerly the chief of cardiothoracic surgery at Yale University and Yale New-Haven Hospital, Dr. Elefteriades is working on identifying the genetic mutations responsible for thoracic aortic aneurysms. He is the author of over 400 scientific publications on a wide range of cardiac and thoracic topics.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
.
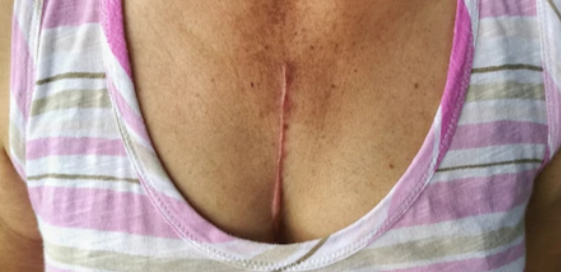
Top image: ©Lorra Garrick
Chest Pain with Hoarse Voice: May Be Cancer or Aortic Aneurysm
Have you been experiencing a hoarse voice and chest pain?
If your chest pain and hoarse voice seem to be connected to each other, and even if they don’t seem related, this can indicate a potentially life-threatening situation.
“A hoarse voice by itself just indicates voice box (larynx) or vocal cord problems, like inflammation, infection, or polyps–as we see with celebrities like Julie Andrews or Adele,” says Dr. John A. Elefteriades, MD, William W.L. Glenn Professor of Surgery, and Director, Aortic Institute at Yale-New Haven, New Haven, CT.
“The additional symptom of chest pain puts this in a different category.
“The nerves that operate the vocal cords, called the ‘recurrent laryngeal nerves,’ run (curiously) into the chest and around the arch of the aorta before ascending back to innervate the vocal cords.”
The aorta, the body’s largest blood vessel, branches off the heart and supplies the body with blood.
Dr. Elefteriades continues, “So, a combination of chest pain and hoarseness makes one think of space-occupying lesions in the chest in the vicinity of the recurrent laryngeal nerves.
“Such lesions could include aneurysms and tumors and cancers.”
An aneurysm is an abnormally enlarged blood vessel, sometimes referred to as dilated or ballooned.
The ballooned or enlarged portion is very weak and prone to tearing or rupture; there is a direct correlation between size of aneurysm and likelihood of tearing or rupture.
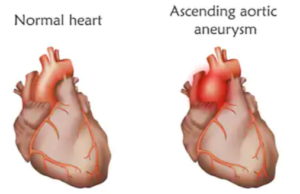
Shutterstock/Veronika Zakharova
“These lesions cause chest pain by compressing adjacent structures and impinging on intra-thoracic (in-the-thorax) nerves,” continues Dr. Elefteriades.
“These lesions cause hoarseness by stretching the recurrent laryngeal nerves, thus disturbing their function. This disturbance may be transient or permanent.
“Sometimes, with removal of the offending mass, vocal cord function can return to normal.
“The symptoms must be attended to, as not only is the hoarseness troublesome in itself, but an aneurysm or tumor or growth can be very serious and life-threatening.”
If you have chest pain with a hoarse voice, seek immediate attention:
An aortic aneurysm can rupture without warning; half of all patients with a ruptured aortic aneurysm die before they reach the hospital.

Formerly the chief of cardiothoracic surgery at Yale University and Yale New-Haven Hospital, Dr. Elefteriades is working on identifying the genetic mutations responsible for thoracic aortic aneurysms. He is the author of over 400 scientific publications on a wide range of cardiac and thoracic topics.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Top image: Shutterstock/Andrey_Popov
Symptoms You Can Expect After Coronary Bypass Surgery
How can the coronary bypass patient know which are normal postoperative symptoms and which ones warrant a trip to the emergency room?
Is the line fuzzy here?
My mother had quintuple bypass surgery, and there were ongoing issues the first three weeks after surgery, including severe abdominal pain.
When I phoned the on-call doctor, he said to get her into the emergency room.
So I drove the 40 minutes down there, at around midnight.
After she got out of the car, she began collapsing. At the time, I thought it was a heart attack and had no idea what it really was (it turned out to be a sudden severe drop in blood pressure).
In the ER she was immediately tended to, and this included an ultrasound of her abdominal aorta (presumably to see if the severe abdominal pain was being caused by a rupturing aortic aneurysm).
The cause of the pain was never determined and my mother eventually made a full recovery.
Some select articles on coronary bypass surgery
Everyone who’s had CABG, plans on having CABG, or has a family member who’s had or is planning on having CABG, should read these articles:
- Vomiting after surgery
- Abdominal pain after surgery
- Chest pain after surgery
- Trouble breathing after surgery
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/virgo1957
Severe Chest Pain from GERD Can Mimic Heart Attack Feeling
The chest pain from GERD can feel just like the chest pain that occurs during a heart attack or one that’s about to occur.
GERD is a very common condition. Unfortunately, the chest pain that gastroesophageal reflux disease causes can be severe enough to mimic a heart attack, says Dr. Maxwell Chait, MD, gastroenterologist at ColumbiaDoctors Medical Group in Westchester County, NY.
Can an abdominal spasm be the only symptom of GERD?
Dr. Chait responds that the problem could be an esophageal spasm or “nutcracker esophagus.”
He adds, “These are true spasms of the muscle of the esophagus and can cause chest or upper abdominal pain that can be severe and mimic a heart attack.”
If you’re in the ER and report this symptom, you will have blood drawn to see if an enzyme called troponin has leaked into your blood.
The test for this is extremely sensitive and hence, extremely accurate in determining if you’ve had a recent heart attack or if you’re in the process of having one.
When cardiac muscle is damaged, troponin leaks from the tissue into the bloodstream.
But back to the abdominal spasm or a hiccup-like sensation…
Dr. Chait says that this can also “be associated with a sensation called water brash, which is the welling up of fluid in the mouth that one feels just before they vomit.”
He adds, “Both may be warning signs of GERD when it is associated with more severe problems such as esophagitis, gastritis, ulcer disease, etc.
“The spasm feeling also may not be related to the esophagus and actually be related to diseases of the gallbladder, stomach or pancreas.
“Either way, when someone gets these severe symptoms, they need further evaluation by their doctor.”
Severe chest pain or abdominal pain should never be ignored.
Though there are numerous non-serious causes, there are also quite a few serious causes.
Plus, you should never attempt to make a diagnosis; medical imaging can reveal a lot about what’s going on in the body, and that includes GERD.

Dr. Chait’s practice interests include digestive conditions such as colon cancer, gastrointestinal endoscopy and internal medicine. He has authored numerous publications in reputed journals.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
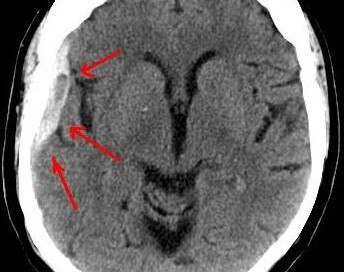
BRAIN BLEED from Concussion Can Mean Subdural Hematoma
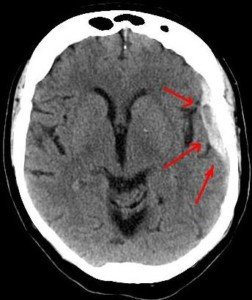
Bleeding in the brain, namely a subdural hematoma, can result from getting hit in the head or hitting your head in a fall.
“Traumatic brain injury (TBI) can produce hemorrhages (including subdural, epidural and subarachnoid) from the focal trauma to a particular area of the brain,” says D’Wan Carpenter, DO, a board certified physical medicine and rehabilitation physician with SIMEDHealth in FLA.
“In the case of subdural hematoma (SDH), the traumatic force causes shearing of the bridging veins which lie between the pia-arachnoid layer and the dura.
“There is an increased risk of subdural occurring from concussion/mild TBI in people with cerebral atrophy (generalized loss of brain parenchyma), a normal finding in the elderly.”
This is because there’s more room or space between the veins and the skull for them to be torn, whereas, in young people, this space is very tight (due to a bigger brain).
Younger people are far more likely to sustain an acute subdural hematoma — typically from vehicular crashes and sport-related impact (skiing, boxing, football).

“The findings of a SDH can occur immediately [acute], between three days and three weeks [sub-acute] or greater than three weeks [chronic],” says Dr. Carpenter.
“This is in part due to the fact that the blood flow through the bridging veins is at a low pressure.
“And this [sometimes] creates a slow leak of blood into the space between the skull and the dura mater.
“The severity of the TBI is typically related to the rate blood accumulates.”
An acute subdural hematoma is an emergency situation and has an 80 percent mortality rate.
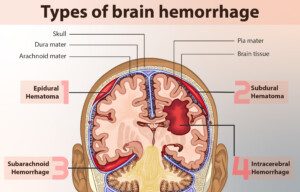
Credit: myupchar/wikimedia commons
With a chronic subdural hematoma the patient can go weeks, even a few months, before symptoms begin appearing.
This happened to my mother: Six weeks after fainting and then falling, hitting her head on the ceramic bathtub — she experienced her first symptoms.
One was weakness in a leg and a difference in the way she walked as a result.
She also experienced a major, persistent headache that she described as a “crown of thorns.”
 Dr. Carpenter is one of the nation’s top board-certified physical medicine and rehabilitation physicians, a national speaker, medical legal expert and independent medical examiner. She is founder and Chief Medical Officer of DJC Physical Medicine Consultants. Follow Dr. D’Wan on Twitter.
Dr. Carpenter is one of the nation’s top board-certified physical medicine and rehabilitation physicians, a national speaker, medical legal expert and independent medical examiner. She is founder and Chief Medical Officer of DJC Physical Medicine Consultants. Follow Dr. D’Wan on Twitter.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image credit: Lucien Monfils
How Healthy Are You? How to Check Your Urine

There are quite a few causes of different urine color—including cancer. This is why you should regularly inspect your pee.
Guidelines for Checking Your Urine
Get in the habit of checking your urine. This does not mean you must obsess over it or become filled with anxiety whenever it’s time to relieve yourself.
Just make it a routine habit. The more you stick with the habit of checking your pee, the more in control you’ll be — and you’ll have less anxiety than if you were to go months between inspections.
Make a rule never to inspect your urine while using a public restroom. The lighting in public bathrooms is usually on the dim side.
The other reason is that the avoidance of checking (either on the toilet paper or in the bowl) in public bathrooms will help prevent becoming obsessive over this practice.
You urinate plenty of times throughout the day, so there’s plenty of opportunity to look at your urine. And this should be done in the controlled environment of your home.
It is best checked by voiding in a clear, clean plastic cup rather than trying to accurately view it as it enters the toilet bowl or while it billows out once in the toilet water.
There is so much more you can observe if it’s been collected in a clear and clean plastic cup.
However, this isn’t always practical (even at home). You need not collect your pee for every inspection.
But every day, for at least one voiding, the minimum inspection should consist of seeing what it looks like on the toilet paper, or as it streams out into the toilet bowl.
You’ll also want to view it in the toilet water. But make sure the toilet bowl is white and clean!
A dirty bowl, or one colored with cleaner or something else you may have dumped in there earlier, will hinder the accuracy of the inspection.
A good question is: How many times a day should you take a good look at your urine?
As many times as you feel at ease, but again, don’t become obsessive about it.
Daily checks are actually not even necessary, but checking in at least once a week can be easily maintained without leading to becoming overly attentive.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Twitching Muscles (Fasciculations): Your Headquarters for Answers

This site contains DOZENS of articles that answer questions about twitching muscles and benign fasciculations.
On this site you will find a WEALTH of information that addresses just about every conceivable question about twitching muscles, as well as perceived weakness, strength tests and the EMG test.
Below are links to some of these articles, but many more await you; just type into the search box (upper right of any page) what you’re seeking answers to, and see what comes up in the results!
Click on the body part that’s been twitching:
- Toes — whether it’s the pinky, big toe, several toes, etc.
- Stomach — lower, middle or upper abdomen or the entire stomach area.
- Thumb — sometimes the entire thumb moves, and this is hard to dismiss.
- Lip — it could be just the upper lip, or the lower or both, or the corner.
- All over — the twitching can be anywhere on the body and multiple areas going at the same time such as the back of the upper legs, the calves, the triceps, the eyelid, a finger … anywhere where there’s a muscle.
MORE Articles on Fasciculations Plus Other Related Concerns
It’s amazing how weak a person can feel when they start believing they have a fatal disease such as amyotrophic lateral sclerosis.
Suddenly, their leg or arm feels weak. There are ways for a medical professional to screen for true weakness (clinical) and that which only SEEMS real (perceived weakness).
ALS weakness compared to perceived weakness
There are so many ways to test the strength of your foot to “rule out” foot drop
But some strength tests for the foot are very ineffective, while others are slam-dunk effective.
Sometimes a person with health anxiety will try to do the wrong kind of strength test.
If you know the right kind to do — ones that are very telling — you will gain more insight and quite possibly LOADS of reassurance.
Strength tests you can do for foot drop
Shutterstock/MRAORAOR
Some men and women will focus on their tongue and no other body part.
And sometimes the tongue is part of a fear that involves other body parts such as the hand or leg.
One of the aspects of twitching muscles that freaks people out is when they are visible.
If it can be seen, it can surely be felt. But if the twitch can be felt, it’s not always visible.
What does visibility actually mean when it comes to a twitching muscle? It’s all here: All about visible fascics
Anxiety is a leading cause of benign fasciculations (muscle twitching with a harmless cause).
Are you stressing about bills lately? How about an impending major car repair?
What about stress in your marriage or relationships, or anxiety about issues at the workplace?
Whether the anxiety is acute or chronic, it can affect the body in many worrisome ways.
Exercise or vigorous physical activity, as well, can cause residual or lingering fasciculations.
For instance you may end up with a real “thumper” in your quad a few hours after going at it on your gym’s revolving staircase.
Several hours of hiking can easily bring it on — and not while you’re hiking, but after you get home and are relaxed in front of the TV or computer.
This is when your muscles will find it best to start worming or thumping around.
A combination of anxiety and exercise can create ripe conditions for lots of twitching that will get your attention.
Exercise, anxiety and the relation to twitching muscles.

Depositphotos.com
And speaking of the quads — the quadriceps muscles — this area of the body is a common hotspot for fasciculations.
Often, they can be felt while a person is sitting at their computer or watching TV.
Strength tests for this particular muscle group are almost endless, but there are several key movements that are excellent for testing strength and neuromuscular control.
Here are strength tests you can do at home.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/sdecoret
Tongue Problems: Twitching, Stiffness, Soreness
This muscle (yes, the tongue is a muscle) has caused unspeakable anxiety in many men and women —
— to the point where they’ll spend huge amounts of time every day examining their tongue in a mirror, and also “testing” its strength by pressing it against the insides of their mouth.
These “checks” can go on all day, beginning shortly after getting out of bed in the morning.
Before the face is washed, hair is combed, etc., the afflicted individual begins examining his or her tongue in a mirror.
After a certain number of checks, he’s convinced nothing is wrong. Then upon proceeding to do the next thing (brush hair, rinse face, shave, what-have-you), he’s suddenly reeled back to the mirror and just has to get in more tongue checks.
Can’t Get Enough Tongue Inspections
The tongue is not just a muscle — it’s an ugly muscle. There’s no such thing as an attractive tongue.
Its inherent unsightliness doesn’t help calm the nerves or those with health anxiety.
They’ll think it’s swollen, or maybe they’ll swear it’s atrophied.
They’ll begin seeing that one side is smaller than the other, or that there are “dents” in it that mean a deadly neurological disease — a killer disease that I won’t mention here, but you know what I’m referring to.
Sometimes the frequent tongue inspections involve how well a person can move it inside the mouth.
Other times it’s about how this muscle feels inside the mouth.
- Is it stiff?
- Is it rigid?
- Is it hard?
- Can it press harder on one side than the other?
- Can it curl?
Check out these very helpful tongue articles if you’re in desperate need of reassurance:
- Take control of your tongue twitching terror
- Is there a way at home to rule out Bulbar onset?
- Causes of a stiff tongue
- Causes of a sore tongue
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Vladimir Gjorgiev
Muscle Weakness Strength Tests for Peace of Mind

What your panicky self really needs right now are some strength tests to see if your muscles are truly weak or to see if your problem is the so-called perceived weakness.
What is perceived weakness?
This term used to primarily refer to the observation of moral deficiency in another individual.
Times have really changed since the advent of Dr. Google.
Perceived weakness has come to be strongly associated with falsely believing that one has a new-onset weakened portion of a limb and even a single finger.
They may suddenly develop this perception during a workout when one arm is noticeably “weaker” than the other during a bench press, dumbbell press or some other lift involving two arms.
This can trigger going down a rabbit hole.
A trigger can also be the tasks of daily living. For example, something falls out of your hand like a notebook, a spoon, a pen, your child’s little stuffed animal, a bag of chips — anything that you might be carrying throughout a normal day in a hand.
This then sets off the idea that the hand has become weak — due to a motor neuron disease.
When one’s mind starts going in these directions, “strength tests” will invariably follow.
If you’re a gym rat, many of these tests will take place in the gym or wherever you do your workouts.
If you’re not into lifting weights, these inspections of strength in that “weak” part of your body will take place usually at home, but sometimes also on the job.
These can be any kind of physical exertion that you can possibly imagine.
For instance, if you believe your left arm is weak due to a new disease, you may find yourself trying to pick up the vacuum cleaner with one hand.
Or picking up your dog repeatedly, or repetitively picking up a box of books from the floor.
The strength tests that ensue, when one develops perceived weakness and a fear that this is the beginning of a neurodegenerative disease, can be quite elaborate and/or unrealistic.
Here are strength tests for various body parts:
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.