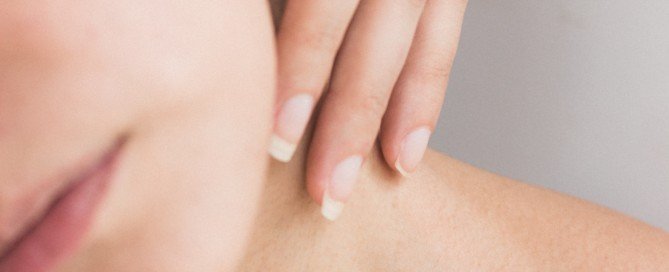
How to Check if Your Moles Are Getting Bigger
Here is a really simple way to tell if one of your moles is getting bigger — even a very tiny dot of a mole.
No apps required! You need only two simple items.
The first is a 3 x 5 index card.
Making Reference Dots for Mole Size Comparison
With a pencil, create a dot on the very edge of the long side of the index card. The size of the dot should be as close as possible to the mole.
This is the baseline dot that should replicate the size of the spot on your skin.
Use an index card, rather than regular paper, because the stiffness makes it easier to handle.
Place the edge of the card, that has the dot, against your skin as close to the mole as possible.
This is how you can compare the size of the dot to the mole, to see if you need to make it a tad bigger to match, or, start over and create the dot again to match the size.
The objective is to make a dot that’s the exact size (and shape, if applicable) to the mole. A bigger mole is less likely to appear as a perfect circle.
Duplicating the shape of a non-circular skin lesion will be challenging to the less-artistically inclined. If you can’t draw, do your best, as this is still a great home test.
Next, draw a second dot that’s a tiny bit smaller than the skin spot (or smaller than the baseline-drawn dot), on the edge of the card, near the baseline dot.
Finally, make a third dot, on the other side of the baseline dot, that’s a bit bigger.
Compare the Dots to See if Mole Is Bigger
You now have three dots. The middle dot is the same size as your mole. If you suspect it’s changing in size, all you need to do, to verify this, is place the edge of the card against your skin near the mole.
The closer the dot is to the edge of the card, the easier it will be to make a side by side comparison between mole and dot.
Without this reference point, it will be difficult to determine if your perception that a mole is changing in size is just your imagination. The index card method is objective and leaves nothing to imagination.
If the size of what’s on your skin begins matching the dot that’s bigger than the baseline dot, you know you’re not imagining that your mole has gotten bigger.
If after a week, the mole then matches the size of the baseline dot, this means that it has returned to its original size.
This is exactly what happened to me when I became concerned over a tiny brown spot. Because I was using the dot method, I knew it wasn’t my imagination that the mole had gotten bigger.
After several days of this, it then began matching the baseline dot that I had drawn, which reassured me that the increase in size must have been due to irritation. A biopsy later confirmed this.

 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Plantar Fasciitis Pain vs. Heel Spur: Symptom Comparison
“Plantar fasciitis is also commonly called ‘heel spur.’ but the two conditions are not the same,” says Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health.
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
“A true heel spur typically does not produce a high level of pain unless it presses on the soft tissue in the heel,” says Thompson.
“While plantar fasciitis and heel spurs can occur together, plantar fasciitis is usually the condition that produces the pain.”
The pain of plantar fasciitis can often be described as burning, or as “my feet are on fire.”
I’ve had plantar fasciitis, and it’s not the same kind of pain you might feel as part of a sprained ankle (which I’ve also had) or from getting hit in the ankle from something falling on it like a gym weight plate.
What’s a heel spur?
“Heel spurs are calcifications forming on the bone, that are typically caused by unusual or abnormal motion in the joints over time, excessive tension on the bone from a tendon, severe or repetitive trauma (everyday wear and tear), the aging process, conditions such as osteomyelitis (bone infection) and Charcot foot, and general inflammation (as in plantar fasciitis).”
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Can a Stress Fracture Cause Heel Pain?

That heel pain that’s been bothering you lately just may indeed be caused by a stress fracture.
“Fractures and bruises can create pain in the heel,” says Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health (IPFH.org).
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
What Is a Stress Fracture?
Quite simply, it is a tiny crack in a bone. The injured part of the bone is not severe enough to displace the bone; a cast is not required for healing.
However, a walking boot or brace may be needed to provide support, reduce pressure on the bone and limit movement.
This helps the fracture heal properly by preventing further stress or injury.
It also reduces pain and allows for safer, more comfortable mobility during recovery.
The bones of the lower leg and foot are the most vulnerable to a stress fracture. These, of course, include the heel area.
Physical activities that, in particular, can give rise to this kind of injury include jumping, running, basketball, volleyball, gymnastics and figure skating, among others.
But ANYONE can get a stress fracture in the foot.
Thompson explains, “The calcaneus is the primary bone in the heel. Although an actual fracture of the calcaneus is relatively rare, it can be very painful.
“A fracture occurs most often as a result of a severe blow to the heel area, such as a fall from a height or some other serious trauma.
“Calcaneus fractures are often serious and need to be attended to quickly.”
Thompson further explains, “Less severe stress fractures can also be responsible for heel pain, but are typically not as painful as more serious fractures.
“Bruises can also occur as the result of blows to the heel area, and while they can be painful, they are not as serious as fractures.
“Those who are particularly vulnerable to heel bruises are participants in sports that require repetitive jumping and landing on the feet.
“This includes volleyball, basketball and distance running.”
Other sports that include jumping are that of track field events, high intensity interval training involving workout boxes or stools, and parkour, which is a form of running that involves leaping over obstacles.
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/KlaraBstock
Why Your Heels Hurt Like Mad Stepping Out of Bed
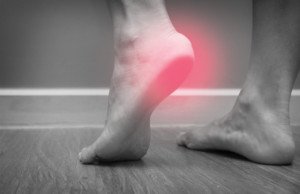
Do you dread getting out of bed every morning due to really nasty heel pain?
Does it almost feel like you’re stepping on hot coals?
“A sharp burning pain in the heel area is one of the most telltale signs of plantar fasciitis,” says Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health (IPFH.org).
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
“Plantar fasciitis is inflammation of the plantar fascia, the dense band of fibrous tissue that functions as the main support for the arch of the foot,” continues Thompson.
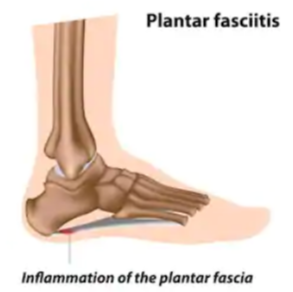
Shutterstock/By Alila Medical Media
“Plantar fasciitis is most frequently caused by a sudden increase in the level or intensity of activities, overuse, faulty biomechanics (for example overpronation, high-arched feet or other gait-related issues), being overweight, extended periods of standing on hard surfaces and poorly designed footwear.”
I used to have plantar fasciitis in both feet, having developed at the same time.
The trigger was walking on my heels, on a treadmill, wearing hiking boots.
I wanted to break in the boots for extended hikes, and perhaps I got bored just walking on the machine.
So I decided to walk on my heels to target more of the anterior tibialis muscle in the front of the lower leg.
Though I was really into fitness, the risk of plantar fasciitis from walking on my heels didn’t occur to me.
“The sudden pain one experiences when first stepping out of bed in the morning is typically a result of the affected foot’s having been in a relaxed, plantarflexed position (pointing downward) during the night,” says Thompson.
“When the foot is tensed and stretched into a dorsiflexed position (heel down, toes up) to bear weight when the person gets out of bed, it stretches and tears the already inflamed plantar fascia away from its attachment point on the calcaneus (heel bone), causing the sudden and intense pain.”
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Top image: Shutterstock/catinsyrup
Why Feet Hurt After Sitting: Circulation Problem, Solution
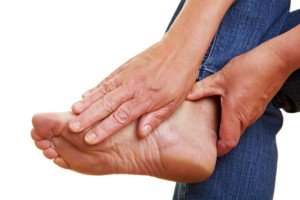
There is a cause of hurting feet after sitting that may surprise you.
Are your feet in pain or sore after you’ve been sitting for a while, such as while using a computer, at the workplace or relaxing in front of the TV?
“If your feet don’t normally hurt when you are walking or moving about, the most likely cause is that the blood in your feet and legs has not been circulating vigorously while you were sitting,” says Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health (IPFH.org).
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
“The human body is designed for movement; and periods of prolonged standing or sitting have a negative effect on circulation in the legs,” says Thompson.
Prolonged sitting also has a negative effect on the heart, according to research that was reported in Current Cardiovascular Risk Reports, 2008
“The veins in the feet and legs that carry deoxygenated blood back to the heart have to work against gravitational pull,” says Thompson.
“These veins have valves that help the blood flow upward, and there is a ‘pump’ mechanism in the calf muscles of the legs that assists in that upward flow.”
So if you sit for prolonged periods, such as at work, driving long distances, in an airplane or just reading a book, “the lack of muscle activity in your legs may cause insufficient return flow of the blood, causing it to ‘pool’ in your feet and legs,” continues Thompson.
“When you stand up, the extra blood in the feet and legs has to be circulated back up the legs, which may create higher than normal blood pressure in the area, which in turn may cause you to feel pain.”
How can one avoid this?
“The best way is to stand up frequently if you can, and to flex the feet, move the legs and in general avoid sitting still for prolonged periods.
“This is especially difficult on long plane flights, and is especially important to avoid if possible due to the potential danger of blood clots related to prolonged sitting and varying air pressure in airliner cabins.”
Heel or Arch Pain After Sitting
This will almost always be caused by plantar fasciitis, an inflammation of the ligaments that run the length on the underside of the foot.
However, if you have this condition, you’ll also very likely experience it when up and about, not just when sitting, and particularly during exercise or sport.
You’ll also probably feel pain or burning under your feet the moment you get out of bed in the morning.
Plantar fasciitis has nothing to do with poor circulation.
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Top image: Shutterstock/Robert Kneschke
Pain in Feet After Sitting May Be Arthritis or Fibromyalgia
Don’t dismiss arthritis or fibromyalgia as possible reasons your feet hurt after sitting, even though you may have read that a likely cause is plantar fasciitis.
Here is what Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health (IPFH.org), has to say about the cause of feet hurting after prolonged sitting:
“Another, less likely reason for pain in the feet after sitting for a while is arthritis or a connective tissue problem such as fibromyalgia.
“Both can cause you to feel pain when you put weight on joints that have been inactive for extended periods of time.”
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot discomfort.
The Effects of Obesity
In addition to the above causes, obesity can lead to painful feet when seated and after standing following prolonged sitting.
This is due to increased pressure, inflammation and conditions that can be caused or worsened by obesity such as plantar fasciitis (pain in the heel or sole) or swollen ankles.
Extra weight strains foot structures, leading to aching, tenderness and swelling, especially after inactivity when blood flow changes.
This added stress can damage tissues, weaken arches and contribute to structural problems.
How can this problem be prevented?
In addition to working on weight loss of you’re overweight, Thompson explains that you should “try to avoid sitting for prolonged periods of time, and/or move the feet and legs while seated to help stimulate circulation.”
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Burning Pain in Arch of Foot: 3 Possible Causes
There are three very likely causes of burning pain in the arch of one’s foot.
“If the burning pain in the arch is toward the heel area on the plantar surface (underside) of the foot, a likely cause is a heel spur or plantar fasciitis,” says Bob Thompson, certified pedorthist, executive director, Institute for Preventive Foot Health.
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
“Plantar fasciitis is inflammation of the plantar fascia, the dense band of fibrous tissue that functions as the main support for the arch of the foot,” continues Thompson.
Causes of plantar fasciitis, says Thompson, are:
• Sudden increase in exercise intensity
• Overuse/overtraining involving the feet
• Faulty biomechanics (e.g., walking on one’s heels, gait abnormality from flat feet or high arch)
• Poorly designed footwear
• Standing for too long
• Being overweight, especially morbidly obese
Second possible cause of burning pain in the arch:
This would be posterior tibial tendonitis. “Tendonitis is inflammation of a tendon,” says Thompson.
“The posterior tibial tendon runs through the area on the medial (inside) area of the ankle and into the arch area.
“This type of tendonitis can occur due to injuries related to falls and athletic activities that put stress on the posterior tibial tendon (as basketball, soccer and tennis).
“Other causes include overuse, degeneration from conditions such as rheumatoid arthritis, diabetes or hypertension and obesity.”
Third possible cause of burning pain in the arch of the foot:
That’s a strained muscle. “The flexor digitorum longus muscle runs along the medial side of the foot in the arch area; and a strain in this muscle can produce burning pain in the arch area,” says Thompson.
“As in other conditions, strains can occur due to overuse and vigorous activities that include running, jumping and throwing, especially if the participant is not well-conditioned for those activities.
“Other causes include fatigue and insufficient or improper warmup before vigorous physical activities.”
Treatments that Will Help Relieve a Burning Pain in the Arch of Your Foot
Initial treatment for plantar fasciitis — perhaps the most common cause for burning in the arch of the foot — typically involves avoidance of the offending activity, ice application and over-the-counter anti-inflammatory medications (NSAIDs).
Stretching exercises for the Achilles tendon and plantar fascia, along with strengthening exercises for the foot and lower leg, can help heal this often burning condition.
Before exiting your bed every morning, spend one minute pulling your toes towards yourself, each foot, to stretch the plantar fascia, which will have tightened up overnight. See the image below.

Plantar fascia stretch. Freepik.com/yanalya
Arch supports are recommended during exercise or sport.
If conservative treatments don’t work, then physical therapy, corticosteroid injections or shockwave therapy may be considered.
Rarely, if other treatments fail and symptoms persist, surgical options may be explored.
Treatment for posterior tibial tendonitis includes rest, ice and NSAIDS.
Physical therapy is important for stretching and strengthening to improve flexibility and support for the tendon.
Custom insoles or arch supports can provide additional stability and relieve pressure on the tendon.

In more severe cases, a brace or walking boot may be used to immobilize the foot and allow healing.
If conservative treatments do not provide relief, corticosteroid injections are an option.
In rare cases, surgical intervention might be necessary.
For a flexor digitorum longus muscle strain, avoid the offending activity and apply warm compresses. Gradually resume activity as the burning in your arch begins subsiding.
To further reduce burning pain in the arch of your foot, or to help prevent any burning from developing or recurring — work on losing weight if you’re overweight.
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Top image: Shutterstock/Denis Val
Can Burning Feet Be Caused by a Serious Disease?
Don’t blow off that burning in your feet. This can mean a life-threatening condition.
Don’t assume that feet don’t show symptoms of serious disease.
“Burning feeling in the feet can be an indication of neuropathy (nerve damage),” says Bob Thompson, certified pedorthist, executive director of the Institute for Preventive Foot Health (IPHG.org).
A pedorthist is a medical professional who specializes in designing footwear and devices to alleviate foot pain.
“Since this is a serious condition, anyone who experiences a burning or tingling sensation in the feet should see a physician immediately,” continues Thompson.
“Neuropathy is most commonly associated with longstanding cases of type 1 or type 2 diabetes.”

Perhaps you’ve heard the term diabetes neuropathy, and maybe you’ve even seen print magazine ads for medications to alleviate the symptoms, which are often depicted as a burning pins and needles sensation.
Neuropathy, which as mentioned can cause a burning in the feet, has other causes besides diabetes.
These are, says Thompson, “nerve injuries (especially in the lower back), pressure on the spinal nerves from a herniated disc, lack of blood flow to the feet, often because of artery problems, multiple sclerosis, seizures, strokes or transient ischemic attacks, and a number of other systemic issues.”
If you’ve been experiencing burning in the feet that clearly doesn’t seem related to recent excessive activity such as trail running, an all-day hike, an extra strenuous step aerobics class, plyometric (jumping) drills or first-time inline skating, make an appointment to see a doctor.
“If the burning sensation is located between the toes or is accompanied by itching, it is likely due to athlete’s foot,” says Thompson.
“Feet may also burn as a result of alcoholism, Charcot Marie Tooth (a nerve disorder), or certain vitamin and mineral deficiencies.
Simply being in ill-fitting footwear including sneakers all day long — even without a lot of walking — can cause a sensation of mild burning, though this would dissipate by end of day once the shoes are off.
“Burning in the feet is also often associated with certain chemotherapy drugs,” says Thompson.
 Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
Robert Thompson is a nationally recognized speaker on the topics of preventive foot health and soft tissue injury prevention.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss and keeping it off, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss and keeping it off, muscle building, fitness and improved health.
.
Top image: Shutterstock/Africa Studio Foot Pain
Twitching Muscles: Strength Tests for Quadriceps
Here are reliable strength tests for the quadriceps if twitching muscles have you scared.
As a former personal trainer, I’ve come up with excellent ways to test the strength of your quadriceps muscles.
Strength test # 1
Get up from a sturdy, non-rocking, non-deep chair — or weightlifting bench — with just one leg.
This will not be possible for many healthy people, but if you can do it without using your hands, this should be really reassuring.
Don’t despair if you can’t do this; again, it’s inherently difficult, and should not be attempted from a low chair.
This quadriceps strength test is basically for athletes or well-conditioned gym enthusiasts, but feel free to give it a try.
If you can’t do this, you can still use it as a strength test in terms of progress over the next few weeks.
Progress is reassuring, because it means that the muscle is healthy and getting stronger with repeated attempts.
Strength test # 2
Hop up a flight of stairs with both feet at the same time.
At the top, expect to be winded if you’re able to bound up nonstop. This is a strength test for your quadriceps, not a test of cardiovascular stamina.

Shutterstock/Vadim Martynenko
Begin slowly at first, as agility is required, and non-athletic people risk stumbling. Go one slow step at a time. With both feet, jump to the next step and collect your balance.
Proceed at a comfortable pace. If both quadriceps are normal, you will feel an equality in your legs, rather than one noticeably deficient relative to the other.
If you’re sloppy doing this, the thing to look for is equality or bilateral ability.
Non-athletes will struggle with this, but if their muscles are healthy, the struggling will be equal in both legs, or bilateral.
Practice this daily; a person with healthy muscles will experience progress.
Strength test # 3
Dash up and down a staircase or outdoor steps.
Did one quad’s “weakness” cause you to stumble and fall?

Athletes or exercise enthusiasts can try all sorts of things for quadriceps strength tests, such as jumping up and down exercise stools; performing barbell and dumbbell squats; deadlifts; leg presses and leg extensions.
If you can perform these with the same amount of weight you’ve always used, and especially if you’re making gains as far as mount of weight lifted, this should be extremely reassuring.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Freepik.com
Cause of Sudden Arm, Leg Weakness on One Side of Body

The cause of sudden weakness of an arm and leg on one side of the body isn’t necessarily a stroke.
If unexplained arm and leg weakness are happening to you, ask yourself if, in the past few months, you bumped your head or fell and hit your head — or in some way, got banged in the head — even if at the time there were no symptoms.
Dr. Irene Gatti de Leon began experiencing weakness in her right arm and leg, seemingly out of the blue.
Two months prior, she had slipped on some ice and hit her head, but at the time was able to shake it off and didn’t give it a second thought.
Two months later, when she began having weakness in her arm and leg, she didn’t make the connection.
She wasted no time getting an MRI, which revealed a chronic subdural hematoma — a large one compressing her brain.
“Chronic subdural hematoma develops over the course of weeks and sometimes, if the size is small, can cause no symptoms,” says Natasha Fuksina, MD, an internal and integrative medicine specialist who combines traditional and functional medicine to restore health and function.
“However, as the pressure from the bleeding increases it can cause symptoms such as headache, dizziness, personality changes and even progress to the weakness of the arm and leg the opposite side of the body (contralateral side).
“In severe cases, subdural hematoma can cause loss of consciousness and death if the pressure it exerts on the brain is extremely high.”
Sudden Arm and Leg Weakness on One Side: Not Always a Stroke
My mother passed out from a sudden blood pressure drop while standing at the bathroom sink, and on the way down, hit her head against the porcelain bathtub.
She wasn’t even conscious as she fell, so thus couldn’t even help break the fall.
When I heard that awful thud (I was on the lower level), I immediately knew what happened and flew up the stairs.
Unlike the Dr. Gatti de Leon case, my mother had a brain scan that very day — but it showed no subdural hematoma; it was normal.
Six weeks later she had sudden weakness in both legs, particularly the left.
If a chronic subdural hematoma is ignored, with the patient thinking that sudden arm or leg weakness is from stress or working too hard, the patient risks permanent disability — similar to that suffered from a stroke.
“The brain is covered by three layers of coverings (meninges) – dura, arachnoid and pia,” says Dr. Fuksina.
“A subdural hematoma is a collection of blood outside of the brain — between the outermost layer (dura) and the middle layer (arachnoid).”
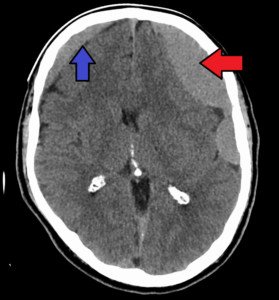
Subdural hematoma. James Heilman, MD
An acute subdural hematoma is immediately life-threatening, since the bleeding is rapid.
A chronic subdural hematoma leaks blood very slowly over time, which is why the patient can go weeks without symptoms, and then literally awaken one day with significant arm and leg weakness.
Neurological symptoms should never be ignored.
If you have sudden or even gradual weakness of an arm and leg, especially on one side of the body, seek immediate medical attention; insist on a brain scan.







 Dr. Fuksina
Dr. Fuksina
































