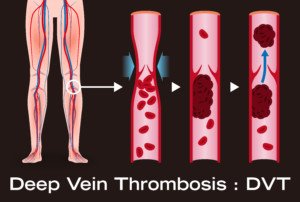
Can Fish Oil and Garlic Supplements Lower DVT Risk?
Find out what a DVT expert says about fish oil and garlic supplements as preventive measures.
A deep vein thrombosis is a pretty common condition in the general population, but there are those individuals who are at particularly high risk.
And those are people with multiple risk factors. Any one of the following risk factors, when combined with one, and especially two, of any of the others, puts a person at a noteworthy risk for a DVT.
- Smoker
- Obese
- Sedentary lifestyle, no regular exercise, excessive daily sitting
- Use of birth control pills
- Frequent air traveler, long flights, few walking breaks while on the plane
- Long distance truck driver who takes few walking breaks
- Recent joint replacement surgery
- Recent abdominal surgery
- Excessive bed rest for some other condition
- Pregnancy
The thicker that blood is, the more likely it will clot under the right circumstances, such as the risk factors above.
Aspirin thins out the blood, but it comes with side effects, namely stomach upset. It can also cause internal bleeding.
Fish Oil, Garlic and DVT Risk

Fish oil and garlic are natural blood thinners and anti-inflammatory agents.
Can they help lower the risk of a deep vein thrombosis?
“Yes, fish oil can have a protective effect [against deep vein thrombosis], as omega-3 fatty acids are known to reduce inflammation throughout the body,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
Inflammation Is a Precursor to DVT
“Inflammation to damaged cells lining veins can lead to thrombus formation,” says Dr. Lucas.
“Garlic is an effective blood thinner and may reduce DVT risk. These do convey some risk reduction, but small.”
Popping fish oil and garlic supplements doesn’t give you a pass for sitting in your truck’s cabin for five hours straight, or refusing to get up and walk around a little bit while on a long airline flight. Or to continue smoking.
Rather, fish oil and garlic supplements are an adjunct to an overall program that’s designed to prevent your blood from becoming thick and sticky, leading to a dangerous clot.
Fish oil contains omega-3 fatty acids that help reduce blood clotting by making platelets less likely to stick together.
Garlic has compounds that may help lower blood pressure and improve blood flow.
When used alongside a healthy diet, consistent cardio and resistance exercise, and other lifestyle changes such as keeping hydrated, these supplements can support cardiovascular health and reduce the risk of clot-related complications.
Fish oil supplements come in capsules, liquid and softgels.
Capsules are a popular choice due to their convenience and ease of swallowing, while softgels offer a similar benefit but are often easier to digest.
Liquid fish oil provides the option for those who prefer not to take pills, though it has a strong taste that some may find unpleasant.
Additionally, fish oil supplements can be found in flavored versions to mask the fishy taste.
Garlic supplements also come in various forms. The most common are garlic capsules or tablets, which contain powdered garlic or garlic extract and are designed to reduce the strong odor associated with fresh garlic.
Garlic oil supplements are another option, providing garlic’s benefits in a liquid form, usually in softgel capsules.
Additionally, there are aged garlic extracts available, which are often marketed as having fewer odor issues and potentially enhanced health benefits.
Any form of fish oil or garlic will help lower the risk of DVT.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Prolonged Desk Work Can Cause DVT: Tips on Prevention

Excessive desk work certainly can increase one’s risk of DVT, says Dr. Paul Lucas.
The human machine was not designed to spend all day sitting at a desk.
Unfortunately, that’s what many men and women must do to earn a living.
However, many people — once they get home from the sedentary workplace — continue with the excessive sitting.
“Excessive desk work certainly can increase one’s risk of DVT, as sitting for prolonged periods leads to stasis that poses a risk for thrombus development,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
Various studies indeed show that excessive sitting increases the risk of developing a blood clot in the leg.
“It is important stretch your legs, get up and walk for even a few minutes when doing this type of work,” says Dr. Lucas.
Prolonged sitting slows down blood flow, creating conditions that can be ripe for DVT formation.
“For every 30 minutes of sitting you should do these things to reduce that risk,” says Dr. Lucas.
“So, push back your seat and stretch those legs. This is also important in air travel and prolonged car or train rides.”
In addition, stay well-hydrated! You may want to fill a pitcher with water in the morning, and then drink from that. This way it’ll be easier to track your water intake.
Remembering to get up every 30 minutes or so to exercise the legs can be cumbersome for people who are deeply absorbed in deadline work at a desk.
They should look into the idea of a treadmill desk. Many different makes and models are on the market.
If your employer won’t allow this, then have one set up at your house — either before the TV or for your computer.
If you have other risk factors for a DVT, such as smoking, obesity, lack of an exercise program or use of birth control pills, you really need to make a concerted effort to offset excessive sitting from desk work.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Can Chronic Stress Cause a DVT?
A vascular surgeon is asked if chronic stress can actually trigger a deep vein thrombosis.
“There is no real objective data on an association of chronic stress and DVT risk that I am aware of,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
However, Dr. Lucas says this: “Chronic stress can lead to elevation in blood pressure. This can result in damage to vessels leading to a setup for atherosclerosis, plaque buildup … and lead to heart attacks and strokes.”
Ongoing anxiety, persistently being “wound up” and “stressed out,” puts the body in a fight or flee mode.
To prepare for what the body thinks is an imminent fight or escape from danger, various physiological changes take place, including thickening of the blood to protect against bleeding to death. This proved handy for primitive man.
For modern man, this protective response can backfire; chronically thickened blood (chronic stress from job, finances, traffic jams, etc.) is more prone to clotting up.
Shutterstock/metamorworks
Chronic stress can lead to behaviors that put a person at high risk of a DVT.
- Overeating leading to obesity
- Excessive inertia, too much bed rest, prolonged cramped seating on a long airline flight or long vehicle drive
- Lack of exercise, sedentary lifestyle
- Smoking
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Compression Stockings Cause a DVT to Break Off?
A doctor answers the question if compression socks or stockings can trigger dislodging of a DVT.
Compression socks or stockings are well-known to people who have a medical condition that causes fluid retention in their legs.
This may be liver disease, kidney disease, or much more commonly, chronic heart failure.
The compression socks help push the backed-up fluid upward. Plus, they can reduce the discomfort that’s caused by the edema.
A person who has a medical condition that would cause enough fluid back-flow in the legs to necessitate the need for compression stockings is also a person who has a DVT risk that’s higher than that of the average population.
Complicating the issue is that if both of the patient’s legs are quite swollen at any given time, the swelling that’s caused by a deep vein thrombosis will not be as obvious as it would be in a normal leg.
And not all deep vein thromboses turn a leg red, hot or cause a calf cramp.
“Contrary to what most people believe, movement in general does not trigger a DVT to dislodge,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
“Dislodgment of a free-floating clot is more dangerous and prone to embolization at rest or with movement.”
Compression Garments
Dr. Lucas explains, “In the presence of DVT and unilateral leg swelling, mild compression garments can be worn to ease the swelling and offer support.
“They don’t squeeze the clot causing it to propagate or embolize.”
Lowering DVT Risk when You Have a Serious Medical Condition
One of the fastest ways to cut DVT risk is to quit smoking.
Another quick way is to take up exercise. If your legs hurt all the time due to your medical condition, then have a seat and do upper body strength training.
Drink six to eight cups of water a day and never sit for more than an hour nonstop.
If you’re obese, it’s time to start a safe weight loss plan.
Having a condition that warrants the use of compression socks does not give you a pass on taking measures to lower your risk of a DVT.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Lentpjuve
Does Psoriatic Arthritis Increase DVT Risk?
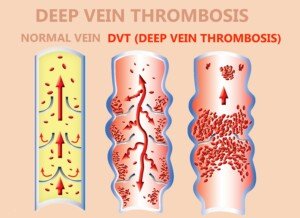
Find out what a doctor says about rheumatic disease’s relation to a deep vein thrombosis.
Psoriatic arthritis is an autoimmune disease that has no cure — only treatments — and for some patients, the flare-ups are resistant to treatments.
One thing that they might worry about is if psoriatic arthritis raises the risk of developing a deep vein thrombosis.
“Rheumatic disease doesn’t cause DVT,” begins Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
He continues, “It does, however, pose a risk for the development of DVT. In fact, a three-fold increase researchers have found.”
Risk Factors for a DVT in no Particular Order
- Birth control pills
- Smoking
- Pregnancy
- Sedentary lifestyle, no regular exercise
- Long airplane flights or vehicular travel with little movement in the legs
- Obesity
- Recent joint replacement or abdominal surgery
- Genetic clotting disorder
- Psoriatic arthritis
Dr. Lucas explains, “The biologic etiology of the elevated risk is a bit tricky. There isn’t anything definitive noted in the literature I looked up.
“There is speculation that there are increases and decreases in various liver proteins and factors that may convey the increased risk.”
What does this mean if you have psoriatic (or rheumatoid) arthritis?
If you have any of the aforementioned risk factors, see which ones that you can modify as much as possible.
Some of them are quite easy to modify, such as standing up and walking around for several minutes, at least once an hour, on a long airline flight or while at your workplace desk.
If you smoke, quit. Yes, just quit already.
Start a plan to lose weight if you’re obese. If you smoke and are also obese, at least you can instantly eliminate one of these DVT risk factors.
If you don’t exercise, it’s time to start. Psoriatic arthritis does not contraindicate exercise.
Finally, drink at least six, eight-ounce glasses of water a day, as dehydration can elevate the risk of a DVT in vulnerable individuals.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Solarisys
Swelling from DVT vs. Joint Replacement Fluid Retention
Is there a way to tell the difference, without imaging, between DVT swelling and post-surgical edema or fluid retention from a joint replacement surgery?
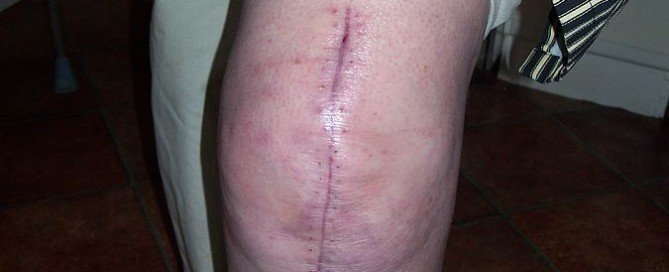
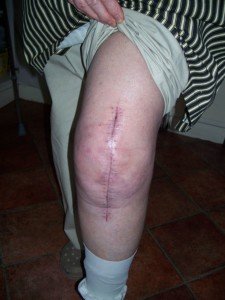
When a joint replacement patient views their affected limb for the first time free of any bandage or wrapping, the patient is bound to be in for a shock at how swollen the limb is.
If the patient knows some basic facts about deep vein thrombosis, they may start wondering if what they’re viewing is swelling from such a blood clot.
Joint replacement surgery is a major risk factor for a deep vein thrombosis.
But a knee or hip replacement will also cause par-for-the-course swelling.
“Swelling after joint replacement can be due to lymphedema, or reactive swelling due to the surgery itself,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
“Lymphedema can be caused by over-hydration during surgery, or by disruption or scarring of lymphatic channels near and around the soft tissues in the area of the surgery,” explains Dr. Lucas.
“Swelling may or may not be associated with a DVT. You cannot discern between them; you have to get an ultrasound to be sure that a DVT isn’t being missed.”
Your orthopedic surgeon as well as any other kind of doctor such as a vascular specialist simply cannot tell whether your swelling is from a DVT or the surgery itself.
However, the presence of other symptoms can definitely arouse high suspicion for a blood clot.
Based on other symptoms, your doctor will order an ultrasound of the limb.
Symptoms Suspicious for a DVT
- Unusual redness of the leg
- Excessive warmth in a part of the leg
- Cramping or pain in the calf, even though this area was not operated on.
- Sudden difficulty breathing (can mean a DVT dislodged and traveled to the lung).
- Sudden chest pain (another symptom of a blood clot traveling to the lung).
If you’re scheduled for joint replacement surgery, expect to see a lot of swelling the first time you see your bare skin. The puffiness can last for several weeks.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Dave Haygarth
Cause of DVT Weeks after Joint Replacement Surgery
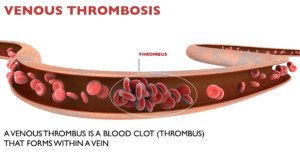
Shutterstock/Naeblys
The “grace period” for DVT development after joint replacement surgery is 90 days, but why so far out if by then, the patient is walking?
Three months out from a knee or hip replacement surgery, a patient who has recovered well might be walking a few miles a day.
Despite that, the risk for a deep vein thrombosis is still present.
“Hard to say why one may get a DVT weeks after joint replacement surgery,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
“Obviously, being sedentary is the main reason, but poor joint movement, lack of flexion ability….anything that may contribute to stasis [inertia] will be a risk….scar tissue, post-op inflammation/swelling within the knee space,” explains Dr. Lucas.
My father has had four joint replacement surgeries. For the fourth one, he was on Coumadin for only 10 days post-op.
Interestingly, the medical literature, in general, says that a patient is at increased risk for DVT up to 90 days after knee or hip replacement surgery.
DVT Risk Following Joint Replacement Varies from One Patient to the Next
Dr. Lucas says, “Some people have a hypercoagulable state [more prone to clotting] that they are not even aware of, and the insult of surgery triggers the DVT.
“Usually these people don’t get DVT unless another risk exposure presents, like surgery or a traumatic injury, etc.”
DVT Symptoms to Be on the Alert for
- Soreness, tenderness or cramp in the lower leg that is not relieved with rest.
- A cramp or other discomfort can also occur in the upper leg and pelvic area.
- The affected area appears suddenly bigger or swollen.
- The affected area may be reddisn/pinkish. It may also be pale or blanched.
- It may be exceptionally warm to the touch.
- In some cases, the affected vein can be felt by a finger, but this usually doesn’t happen.
- If you suspect you have a deep vein thrombosis, you need to get to the ER as soon as possible, even if the pain is only minor. A DVT can dislodge, travel to the lungs and become life threatening.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Naeblys
How Long in Length Can a DVT Be?

A doctor explains how long a DVT can measure in length; no wonder a breakoff can cause a massive fatal pulmonary embolism.
Perhaps you’ve always thought that a DVT, a blood clot in a deep vein, is the size of a BB, just a little bit of sticky blood matter inside a vein, only a centimeter or so long.
Length of a DVT
“In terms of length or extent of a DVT, they can range from those that are very focal (a couple of mm only) to extensive clot throughout the length of the leg, and even into the iliac veins and inferior vena cava,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
In other words, a deep vein thrombosis can extend the length from the foot all the way to the heart, all in one vessel, that extends this length, and merges into the inferior vena cava, a major vein that transports blood from the lower body to the heart where it’s reoxygenated and recirculated.
A DVT that’s almost the entire length of the body has the potential for huge bits of it to dislodge.
And in seconds it can plug up the pulmonary artery where it splits off into each lung, causing near-instant death from a massive or “saddle” pulmonary embolism.
Length of Most DVT’s
“Obviously, most clots aren’t that extensive, but it’s important to note that they certainly can be,” says Dr. Lucas. “They can cause a myriad of symptoms from pain only, to swelling, or a combination of them.”
There are other, more benign causes of pain and swelling in the leg, but Dr. Lucas warns that if you have these symptoms and there’s no simple explanation (e.g., no recent hard run up a hill), you should at least think about a blood clot as a possibility and get the leg examined.
Both pain and swelling, especially in the lower leg, are worrisome, says Dr. Lucas, but not diagnostic for a DVT.
“In fact, no physical examination finding is accurately diagnostic of a DVT, but suspicion should be rendered. About 2-5 percent of people experience a DVT within their lifespan.”
It’s not true that the longer in length a DVT, the more prominent the symptoms will be.
A person can have a DVT that extends from foot to hip and not have symptoms, since in about half the cases, these blood clots present with no symptoms.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Naeblys
You Suspect DVT; Ultrasound Negative; What’s Next Step?
Find out what testing you should insist upon if you suspect a DVT but the ultrasound turns up negative.
One of my articles on DVT is about Staci Stringer, who was told she did not have a DVT even though her calve was swollen and so painful that it was “hard to walk,” she says.
This sounds unbelievable, but it happens: An ultrasound will be negative for a DVT, even though there is one, and the patient just knows that the procedure missed it.
If you ever suspect a deep vein thrombosis but the ultrasound technician says there’s “nothing,” and a doctor says “go home,” count to 3, then remember the following:
“As the director of our vascular lab, I make sure that my techs are very well-versed in venous ultrasound,” says Paul Lucas, MD, surgeon with the Vascular Center and director of the Vascular Laboratory at Mercy Hospital in Baltimore.
“A true vascular lab will examine the entire leg in question, both above and below the knee.
“Some ultrasound departments will only rule out a DVT to the level of the popliteal vein, i.e.. to the knee.”
The popliteal vein is in the back of the knee, and a blood clot in this vessel can cause pain behind the knee.
The reason that some ultrasound departments run the transponder only up to the knee, says Dr. Lucas, “is the low embolization risk for a DVT in the tibial veins.”
Tibial refers to the larger of the two bones in the lower leg.
“If you need an ultrasound done to rule out a DVT, a certified/accredited vascular lab is the place to go.
“Vascular technologists only do vascular studies, whereas an ultrasound tech in some places will do all types of tests. Experience means a lot here.
“If however, a DVT is ‘missed.’ a repeat ultrasound exam may be warranted. If you suspect the DVT may be at the pelvic level or higher, a CT scan may be useful.
“It is possible to have a negative test and within days a repeat could be positive–and it really might not have been there on the first go-around.”
Read more about Staci Stringer.
 Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
Dr. Lucas leads a team of vascular surgeons and technologists who specialize in the diagnosis and treatment of patients with diseased blood vessels.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Shaynepplstockphoto
Causes of DVT in Absence of Risk Factors & Clotting Disorder

Find out what can possibly cause a DVT when there’s no risk factors and no clotting disorders.
A DVT is a deep vein thrombosis: a blood clot in a vein deep in the body, usually in the leg, but sometimes also in the hip area.
In some cases of these blood clots, the patient seemingly did nothing to bring it on (such as being a smoker and sitting cramped in an airplane for several hours)
Additional DVT Risk Factors
Risk factors for a DVT are quite numerous and include prolonged immobility from any kind of traveling, joint replacement and abdominal surgery, birth control pills, hormone replacement surgery, obesity, lack of regular exercise, elderly age, pregnancy and dehydration.
And of course, blood clotting disorders raise the risk.
However, people have been known to get a DVT who have none of the risk factors and who test negative for clotting disorders, leaving the patient, who may even be a young lean gym rat who can’t sit still, baffled.
“In some cases the cause of a DVT is never found,” says Darren Klass, MD, clinical instructor of interventional radiology at the University of British Columbia and the Vancouver Coastal Health Association.
Dr. Klass explains, “In young healthy patients with no risk factors, mechanical compression of the left iliac vein by the right iliac artery in the pelvis may cause a spontaneous DVT. This entity is called May-Thurner syndrome.”
A person may never know they have May-Thurner syndrome until a deep vein thrombosis develops.
“A similar entity exists in the chest, where the subclavian vein (continuation of the vein from your arm) may become compressed by muscle or bone in the chest and cause a DVT,” says Dr. Klass. “This is called Paget-Schroetter syndrome.”
In this condition, repetitive and strenuous upper body activity (swimming, gymnastics, wrestling) is often linked to the deep vein thrombosis.
“Young patients with DVT with no risk factors will be investigated by their physician and these entities excluded,” continues Dr. Klass.
“Other more benign causes may simply be due to dehydration; patients who do not keep their fluid intake up may become dehydrated, which makes the blood more susceptible to clotting.
“In these cases often the dehydration is corrected long before the clot is discovered, and the cause is never found.
“These cases are very few and often a cause can be found after extensive investigation.”









 Dr. K
Dr. K
































