Can a Microscopic Colitis Flare Occur Only Once?

While some people with microscopic colitis have it chronically “all the time,” is it possible that a lucky few might get a flare only once in their entire life?
I was inspired to cover this topic because I had microscopic colitis in 2010 and it resolved within eight weeks.
I registered with a microscopic colitis online community and posted that my doctor told me that microscopic colitis usually resolves in a few weeks.
One of the community members said this was laughable, and that it’s a chronic condition.
This reminds me of a pamphlet I read on plantar fasciitis, a painful heel condition.
The pamphlet said once PF gets to the point where you need custom-made orthotics, it will be a chronic condition.
Some months after getting my orthotics, the PF was completely gone and has never returned. That was years ago!
My point here is that it may seem that a condition, such as microscopic colitis, is necessarily chronic — that once you get it, you’ll get it again if it goes away — and again and again, back and forth throughout your life …
… or, you’ll have it continuously – because allegedly, there is no such thing as having a singular bout of microscopic colitis.
“The natural history of MC is quite variable and depends on the type of MC — lymphocytic or collagenous,” says John E. Pandolfino, MD, Director of the Esophageal Center, Northwestern Memorial Hospital, and Associate Professor, Division of Gastroenterology at Northwestern University.
“The lymphocytic type is associated with a better outcome and can resolve — although it may return.”
Very interesting, because my type, indeed, was lymphocytic. I’ve had several bouts since my diagnosis. Thus, for me, microscopic colitis is not a chronic condition. It’s a very occasional condition.
Dr. Pandolfino continues, “The collagenous variant is less likely to resolve, but still has a favorable outcome.
“Certainly, avoiding the inciting cause — such as a particular medicine (e.g., NSAIDs), will help the disease to resolve, and it is also possible that some patients will have a chronic problem that may require maintenance treatment.”
 Dr. Pandolfino’s practice covers a wide gamut of GI disorders including GERD, Barrett’s esophagus, benign and malignant tumors, swallowing disorders and esophageal disorders.
Dr. Pandolfino’s practice covers a wide gamut of GI disorders including GERD, Barrett’s esophagus, benign and malignant tumors, swallowing disorders and esophageal disorders.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Biting Hard Food Cause Jaw to Make Clicking Noise?

If you bite down on a hard piece of food with enough force like a cold chunk of solid chocolate, this can lead to a clicking noise in your jaw.
“It is not uncommon to see patients who come to the office stating that they had a prior minor jaw concern or no problem, until they bit down on a hard roll, granola bar, hard piece of chocolate, etc.,” says Donald R. Tanenbaum, DDS, MPH, a board certified TMJ and orofacial pain specialist, and author of “Doctor, Why Does My Face Still Ache.”
“When doing so they experienced a sudden slip of the jaw, heard a big crack, ‘saw stars,’ or ‘felt and explosion’….leading to pain, limited jaw opening, and/or a change in their bite.”
Biting Down on Hard Chocolate Causing Clicking Jaw
In my case, I was biting down on a cold chunk of solid chocolate and had to press my teeth hard, several times, to get it to fragment just once.
I did this two or three times, and after that, I realized that my jaw felt uncomfortable (though there were no sounds at that time), though the discomfort was gone within a while.
Several days later my jaw began clicking, though everything else was normal. The noise was soft.
“Essentially what happened is analogous to the athlete who, while performing, heard a big pop or explosion in their knee and were subsequently disabled, often with pain,” continues Dr. Tanenbaum.
Why Biting Down Hard Can Make the Jaw Click
“In both these scenarios there has been a gross failure of the supporting ligaments of the joint, allowing the cartilage to slip out of place wither partially or fully, leading in the TMJ to a click or a more profound limitation of motion.”
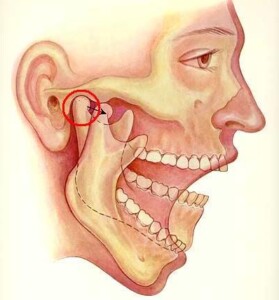
TMJ stands for temporomandibular joint, a ball-and-socket type of joint (like the hip bone is a ball-and-socket). The cartilage that absorbs the shock sits on top of the bone that moves.
“Picture your hand on a stick shift with the shift being the bone, the palm the cartilage and the fingers the ligaments which keep the cartilage in place,” says Dr. Tanenbaum.
“If the ligaments stretch or fail, the cartilage will slip forwards in the TMJ and become an interference to motion, leading to clicks which can be audible and painful.”
Though this problem can occur when frayed ligaments are ready to fail, says Dr. Tanenbaum, the noise in the jaw can also “occur randomly during a chewing event when the chewer was not anticipating resistance from food.”
Frankly, I was quite aggravated that I was having so much trouble fragmenting the chocolate, biting down hard with my back teeth while I was holding the piece in my hand.
“Reasons for ligaments to be frayed and unstable can include prior habits of tooth clenching and grinding, nail and cuticle biting, chronic heavy gum chewing, or past histories of trauma that may have made the ligaments unstable,” says Dr. Tanenbaum.
“Following pregnancies the TMJ ligaments can also be lax, and/or a person may have hypermobility of all there joints predisposing to this scenario.”
So if you hear a clicking, grating or grinding sound in your jaw, ask yourself if within the past few days you were biting unusually hard on some food.

Dr. Tanenbaum’s practice focuses on facial pain, TMJ disorder and sleep-related breathing disorders. He is the past president of the American Academy of Orofacial Pain and takes a multidisciplinary approach to his patients’ care.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Are TMJ Disorders Always Painful or Can They Be Painless?

A TMJ disorder expert explains if this is necessarily painful, or if this can present with no pain at all while still causing movement problems.
Is it possible to have a TMJ disorder (known as TMD or temperomandiular joint disorder) without actually feeling any pain?
“The symptoms can be pain (what brings most to the office), clicking, popping and locking, limited motion or bite changes,” says Donald R. Tanenbaum, DDS, MPH, a board certified TMJ and orofacial pain specialist, and author of “Doctor, Why Does My Face Still Ache.”
Dr. Tanenbaum continues, “Therefore, not all concerns relate to pain. Some relate to not being able to open their mouth wider than one finger’s width, or jaws locking open or in a closed position but without pain.
“Others cannot bring their teeth together in a normal fashion. Pain is a function of inflammation primarily in the joint itself or the associated muscles.”
Muscle Problem, not Bone Problem
Dr. Tanenbaum adds that for most people who’ve been told they have a TMJ disorder, their joint is actually fine, and they just have muscle pain.
“Problematic muscles can lead to pain, and restricted motion, along with bite changes.
“The pain can be in the jaw region or referred to the teeth, ears, eyes and facial regions.
“So at times the location of the pain is not the source of the pain.
“Muscle pain may be due to inflammation or chemical changes such as the accumulation of lactic acid due to muscle overuse, which can occur due to habits or emotions.”
In other words, a person who holds their teeth in a clenched position during moments of anger or stress, may end up with pain or aching in the muscles that control this motion.
The muscles in the jaw are like the muscles anywhere else in the body: prone to soreness and aching from overuse.
“Most people without pain but with some joint noise or limited jaw motion do not come in for care, though women more commonly come looking for an answer.
“Men virtually never come unless they really hurt or their jaw is locked.”

Dr. Tanenbaum’s practice focuses on facial pain, TMJ disorder and sleep-related breathing disorders. He is the past president of the American Academy of Orofacial Pain and takes a multidisciplinary approach to his patients’ care.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/diy13
Can Grating, Clicking Jaw Noise Be the Only TMJ Symptom?
What’s really going on if your only symptom is a grating or clicking sound in your jaw when you chew, open or close it?
Is your jaw suddenly clicking or making a grating sound, but everything else is fine?
What does it mean (TMJ problems?) if your only symptom is annoying sounds coming from the hinge part of your jaw when you open and close your mouth, and chew?
“TMJ problems or TMD, temporomandibular disorders, are essentially orthopedic problems involving the joint itself (the TMJ) and the associated ligaments, cartilage, tendon and muscles,” says Donald R. Tanenbaum, DDS, MPH, a board certified TMJ and orofacial pain specialist, and author of “Doctor, Why Does My Face Still Ache.”
- Symptoms thus can vary and include pain, noise, limited motion, soreness, joint instability and problems with bite.
- Pain can be present continually or only when moving the jaw.
“So, if joint noise is present it suggests some type of alteration in the anatomy of the joint leading to instability, friction or interference, ultimately giving rise to noise which can be a click, pop or grating,” says Dr. Tanenbaum.
“As with all joints in the body, joint noise can be present without pain or disability.”
Perhaps you hear a grating, crunching, popping, clicking or crackling sound in your knee joint when you bend the knee, even though there’s no pain or instability.
The same process may be occurring in your jaw if it makes noise in the absence of pain, soreness or disability.
Theirry Canuel, CreativeCommons
I recently experienced a grating noise in my jaw when opening and closing my mouth, when chewing, and when shifting the jaw horizontally, but absolutely no pain; it felt perfectly normal and moved normal.
At first it was vague, just a little clicking here and there, for a few days, not enough to get my attention.
Then next day the jaw noise got my attention because it was more pronounced, impossible to ignore when eating.
I thought that maybe aggressive mouth-opening to floss my teeth had finally caught up with me.
Then I remembered: Several days prior I had bitten down on a very hard piece of food, on the same side where the noise in my jaw was occurring.
Clicking or grating noise in the jaw “may reflect adaptive changes that have occurred over the years, but not always related to disease and certainly not always indicative of future progression,” says Dr. Tanenbaum.
“Noise in the TM joints can occur due to dryness and friction, altered shape of the articulating bones, shift in the position of the protective cartilage, muscle fatigue or foreign bodies.
“Each of these scenarios will lead to certain noise patterns and character.”
So what does it mean if there’s grating or other noise in the jaw when moving it, but no pain and no limited motion or trouble chewing?
Dr. Tanenbaum explains, that “that person likely does not have an active problem, but rather, a sign (not symptom) that suggests that the architecture of the joint has changed. Most of the time no treatment would be advised.
“Approximately 30 percent of the population has TMJ noise and a large proportion have no other symptoms.
“Grating noise in particular can represent dryness which may come from persistent clenching which forces moisture out of a joint.
“It may also be the end result of a degenerative process causing changes in the shape of the TMJ and the generation of a grinding sensation.”
Dr. Tanenbaum says that biting down on a hard piece of chocolate can cause a TMJ problem.
Guess what: The hard piece of food that I had bitten down on was a very hard block of dark chocolate, straight from the refrigerator!
And I’ll admit, I bit down multiple times to get at it, and it was uncomfortable on my bite.
I finally had to microwave the block. It took over five weeks for the noise in my jaw to disappear with no treatment other than to avoid eating things like carrots, apples and hard chocolates.

Dr. Tanenbaum’s practice focuses on facial pain, TMJ disorder and sleep-related breathing disorders. He is the past president of the American Academy of Orofacial Pain and takes a multidisciplinary approach to his patients’ care.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik/wayhomestudio
Angina Symptoms in Men Compared to Women
Women and men are so different and this includes with angina symptoms.
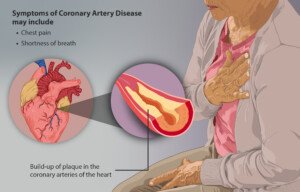
Angina is when the heart muscle does not receive adequate blood flow (and therefore oxygen), as a result of narrowed coronary arteries.
The resulting classic symptoms are chest pain and shortness of breath, especially upon physical exertion or emotional stress.
“Both men and women experience angina (chest pain or discomfort) due to blockage in the coronary arteries that supply the heart muscle,” says Gordon A. Ewy, MD, Director Emeritus, University of Arizona Sarver Heart Center.
A myocardial infarction is when blood flow fails to reach heart muscle due to a completely blocked artery, thereby damaging the tissue.
Dr. Ewy says that men are more likely to have an MI as their initial symptom of heart disease.
“In men, atherosclerosis (combination of cholesterol, scar tissue and inflammatory cells) causes angina by narrowing the coronary artery,” says Dr. Ewy. For women it’s different.
“In women, angina is often due to blockages caused by coronary spasm, in which the muscles in the coronary artery contract, making the artery smaller in one area and limiting blood flow to the heart muscle,” explains Dr. Ewy.
A CT coronary angiogram is used to detect blockages in large coronary arteries.
myupchar. com
This imaging test can therefore miss the problems that cause women’s angina.
“As a result, many women with positive stress tests and angina previously were told there was nothing wrong with their hearts because their coronary angiograms were normal.”
What’s even scarier is that the gold standard for identifying coronary artery blockages, the invasive catheter angiogram, may actually miss blockages in the smallest of the heart’s vessels.
So how can such small-scale, but significant, blockages be detected?
Dr. Ewy says by sophisticated MRI cardiac chemical stress tests. Angina is just harder to detect in women versus men.
Symptoms of angina in men differ than those of women.
“Recent studies have shown that unlike angina in men, most often characterized by chest or left-arm discomfort, angina in women often presents as weakness, fatigue, shoulder, stomach or back pain or shortness of breath,” says Dr. Ewy.
What about treadmill stress tests?
They are more likely to generate false positives in women (the identification of a blockages that’s non-existent).
Dr. Ewy explains: “While 25 percent of men with angina suffered heart attacks within five years, heart attacks occurred in only 17 percent of women with angina.
“In all studies of heart attacks due to total or near-total blockage of a coronary artery, 75 percent were men and 25 percent women.
“Thus, the classic heart attack is three times more common in men; yet, when women do have a heart attack, their mortality rate is higher.”
 In the area of research, Dr. Ewy has made significant contributions to the defibrillation and resuscitation of patients with cardiac arrest. He is board certified in internal medicine and cardiology and has authored over 400 publications in medical journals.
In the area of research, Dr. Ewy has made significant contributions to the defibrillation and resuscitation of patients with cardiac arrest. He is board certified in internal medicine and cardiology and has authored over 400 publications in medical journals.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Dry Cough with White Phlegm: Causes, Treatment
An ear, nose and throat doctor explains what causes a dry cough with white phlegm, and what you can do.
“The most common cause of a dry cough with occasional white phlegm is acid reflux,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology; one of her specialties is sinus surgery.
“Acid from the stomach comes up and irritates the back of the throat,” continues Dr. Silvers, and “this causes the throat to swell, tickling the cords and causing a dry cough.”
A person can have acid reflux and not necessarily experience heartburn or other discomfort in the stomach or chest.
“The mucous drips in the back of the throat causing post nasal drip,” adds Dr. Silvers.
“This mucous is protecting the throat from the acid which will otherwise cause throat ulcers.
“It is this mucous that the individual with acid reflux may cough up periodically.”
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Aaron Amat
Trouble Breathing Your Through Nose? Should You Worry?

Difficulty breathing through the nose can be a pretty frightening experience when you swear you don’t have typical nasal congestion.
What may initially come to mind is the onset of a heart attack, since most people know that the so-called shortness of breath is a common symptom of a heart attack — as well as chronically clogged coronary arteries.
Breathing Problem: Trouble with the Nose
“Shortness of breath” is not the same as the sensation that despite deep breaths, you’re just not getting in enough air.
Trouble breathing that feels as though it’s originating in the nasal passages is probably exactly that: an obstruction in the sinuses or nostrils.
“The causes of nasal obstruction are two: structural and congestion,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology; one of her specialties is sinus surgery.
“Most people have a combination of both,” continues Dr. Silvers. “Structural causes are a deviated septum (which everyone has to one extent or another).
“The septum is simply the cartilage and bony wall that separates the right nostril from the left nostril. It is the tent pole which holds up the nose.
“The second structural blockage can be large adenoid tissue. The adenoids are the ‘tonsils’ behind the nose; they are lymphatic tissue which typically gets smaller as a person ages.
“If enlarged into pre-teen, teen years or adulthood, they can affect the nasal breathing and quality of life and may need to be removed.
“The third structural blockage can be nasal polyps. These form from severe allergies and are an overgrowth of the mucosa in the nose forming single or multiple nasal polyps.
“Congestion, most typically, can be caused by allergy or a virus. This is when the tissues in the nose swell as a response to allergy or viral nasal inflammation.
“Structural blockages can be surgically corrected. Congestion causes need medications.”
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Vladimir Gjorgiev
Hoarse Voice Causes: from Cancer to Reflux to Enlarged Aorta

A hoarse voice can have many causes, and this includes acid reflux, laryngeal cancer and an aortic aneurysm.
Have you been bothered by a hoarse voice lately that doesn’t seem to have a cause such as excessive yelling or a cold?
A hoarse voice in the morning is normal, but what about in general?
“Many things can cause hoarseness,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology; one of her specialties is sinus surgery.
“Laryngitis (viral inflammation of the vocal chords); vocal cord nodules or polyps; long-term smoking irritates the vocal cords causing chronic swelling; vocal cancer, and very commonly acid reflux,” continues Dr. Silvers.
“Acid from the stomach comes up and irritates the back of the throat, causing it to swell. This swelling affects the quality of the voice and causes hoarseness.”
Acid reflux is also known as GERD: gastroesophageal reflux disease.
A thoracic aortic aneurysm, though not a likely cause of a hoarse voice can still cause a hoarse voice.
An aneurysm is a dilated (enlarged) or ballooned portion of an artery.
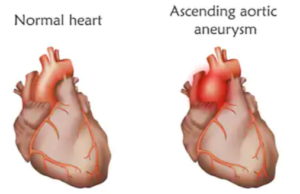
Shutterstock/Veronika Zakharova
The nerve that innervates the vocal cords passes near a section of the ascending aorta, the great vessel (largest in the body) that branches out from the heart.
If part of this vessel, in this location, is enlarged or bulging, it could make contact with the nerve.
So if you’re a nonsmoker and an ENT doctor tells you your vocal cords look normal, that you don’t have GERD or an infection, you haven’t been doing any shouting, yet the hoarseness just won’t go away, it may be time to visit a cardiologist.
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Aaron Amat.
Source: stanfordhospital.org/healthLib/greystone/heartCenter/heartConditionsinAdults/thoracicAorticAneurysm.html
Foul Taste in Back of Throat: Causes, Solutions
If you suffer from a foul taste in the back of your throat, read what this ear, nose and throat doctor has to say about this annoying problem.
Have you been suffering from a foul taste in the back of your throat, even though this cannot be explained by anything you’ve eaten or otherwise ingested?
“Foul taste in the throat can be from: chronic sinus problems, acid reflux or tonsil stones,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology; one of her specialties is sinus surgery.
Tonsil stones can result, says Dr. Silvers, from the buildup of mucous and old food in the tonsil cavities.
These tonsil stones, also known as tonsilloliths, are small, calcified formations that develop within the crypts or crevices of the tonsils.
Over time, these materials can become trapped in the tonsil’s natural folds and pockets, where they gradually undergo a process of mineralization.
As the debris continues to collect and the stones increase in size, they can contribute to discomfort, bad breath and a sour or foul taste in the back of your throat.
As gross as this sounds, the good news is that it’s not a serious issue such as cancer.
Sinus Infection
“A chronic sinus infection can have a sour tasting mucous that can drip in the throat; more severe foul taste is noted with an acute infection,” contiues Dr. Silvers.
Acid Reflux
“Acid reflux causes stomach acid to come up, causing many patients to experience a sour taste and bad breath.”
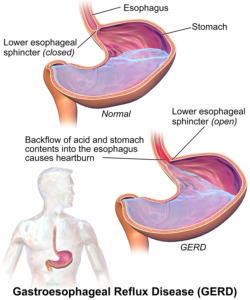
Acid Reflux. Image: BruceBlaus
Another cause of a foul taste in the back of the throat can be stress and anxiety.
Dr. Silvers says that stress is a major contributing factor to the issue of acid reflux. When you get stressed out, this triggers a cascade of responses in your body.
One of these responses includes an increase in stomach acid production.
The body’s stress response can lead to elevated levels of hormones such as cortisol, which in turn can stimulate the stomach to produce more acid than usual.
As the production of stomach acid increases, the likelihood of acid reflux also rises.
When the acid levels become too high, the lower muscle at the bottom of the esophagus, that adjoins the stomach, may not be able to hold back the acid.
The result? This acid gets past the muscle and into the esophagus. But the refluxed acid can also get up into the throat, leading to that foul taste in the back and even in the mouth itself.
When acid travels up to the throat and causes symptoms (including a lump feeling, cough and burning sensation), this is called laryngeal-pharyngeal reflux (LPR).
Hiatal Hernia
The annoying symptom of a bad taste in the throat can also be caused by a hiatal hernia, which can cause or aggravate GERD and LPR.
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/puhhha
Constant Throat Clearing: Causes, Solutions

An ear, nose and throat doctor explains causes of constant throat clearing, and what can be done about this.
Constant throat clearing isn’t just a nuisance to you if you suffer from this, but it’s also a nuisance to all the people around you who hear it.
“Chronic throat clearing is from acid reflux,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology; one of her specialties is sinus surgery.
“Acid from the stomach comes up and irritates the back of the throat,” continues Dr. Silvers. This results in swelling.
“The mucous drips in the back of the throat causing post-nasal drip,” continues Dr. Silvers.
“This mucous is protecting the throat from the acid which will otherwise cause throat ulcers.
“The mucous is annoying, however, and causes an individual to clear their throat constantly, or intermittently to speak, depending on how bad the reflux and how much protective mucous is produced as a result.
“Stress is a big contributing factor to acid reflux,” adds Dr. Silvers.
“Stress will increase the production of stomach acid and the acid can reflux up.”
The more acid in your stomach, the more refluxed acid there will be if the conditions are ripe for reflux in the first place, such as having a weak lower esophageal sphincter (LES).
The LES is normally tight and keeps acid in the stomach where it belongs.
Tourette’s syndrome can also be a cause of the constant or frequent clearing of the throat.
Symptoms of Tourette’s syndrome can be very mild and are often misdiagnosed as other conditions.
Tourette’s syndrome is a neurological disorder characterized by repetitive, involuntary movements and vocalizations known as tics.
These tics can range from simple motor tics, such as blinking or head jerking, to more complex movements and vocalizations like making sounds and repeating words or phrases.
The onset typically occurs in childhood, with symptoms often becoming noticeable between ages five and 10.
It’s also not impossible for autism to be a cause of frequent throat clearing in the absence of a cold, allergies or acid reflux.
In this case, the behavior would be what’s known as a stim: self-stimulatory behavior or repetitive movements — usually for self-regulation. This cause, though, would be at the bottom of the list: possible, but highly unlikely.