How Accurate Are Melanoma Biopsies?

Biopsies for diagnosing melanoma aren’t as accurate as you may believe.
Biopsies for melanoma are not much more reliable than an 85 percent accuracy rate, according to chemistry professor Warren S. Warren, director of Duke University’s Center for Molecular and Biomolecular Imaging.
Warren headed the development of a laser-based tool that has the potential for diagnosing melanoma right in the dermatologist’s office.
This laser tool pumps tiny amounts of energy into a mole that a doctor may suspect is cancerous. The energy redistributes in skin cells, and this gets analyzed.
The Duke researchers discovered that a skin pigment called eumelanin is more prevalent in melanomas than in normal skin tissue.
Based on this, the researchers correctly identified the 11 malignant samples that were among 42 samples in the study.
The next step is to test the laser on thousands of archived slices of skin tissue.
Melanoma biopsies aren’t only less than reliable for diagnosing this disease, but are also capable of generating a false positive.
Warren says that even if the laser tool is only 50 percent more accurate than biopsy, it would actually prevent approximately 100,000 false-positive melanoma diagnoses; that is, normal tissue being diagnosed as melanoma.
A study in the Journal of American Academy of Dermatology (2010) says that pathologists would be in disagreement over whether or not a biopsy sample showed cancer … in 14 percent of biopsies.
A more accurate method of melanoma diagnosis is needed, says Warren, as false-positives result in expensive unnecessary treatments.
This laser tool is currently available commercially.
It just needs to be added to the microscopes that pathologists are already using to diagnose melanoma.
If you’re going to have a mole biopsied because your doctor ways it looks suspicious or because you’ve noticed it changing, you’ll want to inquire about the biopsy process — if the laser tool is in use.
Problem is, the cost to add the laser would be $100,000, but would more than offset the cost of unnecessary treatments for over-diagnosed cases of melanoma.
A more advanced step would be to develop the laser so that it can diagnose melanoma without the skin lesion even being removed from the patient.
This would be even more expensive than the tool being added onto a microscope, and this technology won’t be available for a few years, says Warren.
However, to get to that point, researchers plan on obtaining images of skin cancers grafted onto mice.
Conclusion: Standard biopsies of melanoma are nowhere near as reliable as people believe.
Currently, the technology exists to add the laser tool to microscopes for pathologists to more accurately diagnose melanoma. The full report is in Science Translational Medicine (Feb. 23, 2011).
In the meantime, make a habit of examining your skin every month, including behind the ears, between toes and on the bottoms of your feet, for suspicious lesions or moles.
And regardless of the reason you may ever have a mole removed, it should always be biopsied — even if it look perfectly normal and you want it removed for cosmetic reasons.
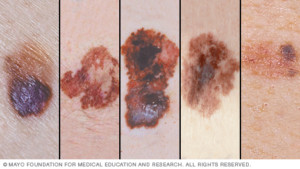
Examples of melanoma
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Peter Sobolev
Source: sciencedaily.com/releases/2011/02/110223151934.htm
Early Melanoma Detection: Mole Mapping Technology Helps Bring Peace of Mind
The earlier that melanoma is caught, the more likely you can be cured from this vicious cancer.
Most people are not aware of a groundbreaking technology that detects melanoma far earlier than any clinical exam can.
The technology is called digital dermoscopy, but this is a broad term, as this can refer to merely a hand-held device called a dermoscope that gives the physician a magnified view of moles.
A more in-depth version of “digital dermoscopy” involves a computer software program and serial photography of the patient’s moles.
Photos of moles, taken over a period of time, are taken, and then analyzed by the computer program to see if 1) they have endured changes over time, and 2) they have characteristics that, according to the computer’s database, resemble melanoma.
Digital dermoscopy with serial photography (around for about 10 years) is often referred to as “mole mapping,” though “mole mapping” is a broad term as well, and can simply refer to the patient’s crude drawing of his moles on a sketch pad.
I asked Dr. Theresa Pacheco, a dermatologist at the University of Colorado Hospital, about digital dermoscopy, aka mole mapping. UCH offers full-service digital dermoscopy including the computer software.
This technology is a godsend for people with many moles, and moles located in difficult-to-inspect areas like the back.
Elective removal of moles at increased risk for developing melanoma may make sense if the patient has only a handful of such moles.
But some people have literally hundreds of moles that require vigilant monitoring due to previous melanoma diagnosis, and/or nature of the moles (e.g., dysplastic).
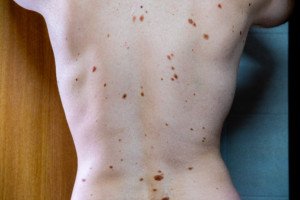
Many atypical moles. Shutterstock/Mikel Ugarte Gil
How effective is digital dermoscopy at viewing obscure areas like the scalp and genitals?
Dr. Pacheco: You can shave the hair or part the hair and still use digital dermoscopy to examine the lesion.
Basically, how does the computer software “detect” that a mole looks suspicious?
Dr. Pacheco: The computer program utilizes certain variables like ‘color,’ ‘symmetry,’ etc., that it utilizes to compute a score… our mole mapper rates each lesion as red (abnormal), yellow (quasi normal) or white (normal)…. but it is really up to the physician to determine whether a biopsy is warranted.
Does the device look at only moles (the moles that the dermatologist has determined for mapping)?
Dr. Pacheco: Yes.
Does the instrument also have the capability of detecting early melanomas in non-mole areas of skin?
Dr. Pacheco: No.
Basically how does digital dermoscopy work?
Dr. Pacheco: The mole mapper should be considered as a tool for use by a trained dermatologist — the dermatologist determines which moles to map….and ultimately which moles to biopsy to look under the microscope.
It is not possible (time) to map every square inch of the body.
We do take overview of body areas (trunk, arm, hand, etc.).
We know melanoma arises in existing nevi (but most nevi are normal) and equally in normal skin … so we focus on new moles, changing moles, symptoms associated with moles, etc. (“nevi” means moles).
Suppose a patient decides to have digital dermoscopy every month. Is there any medical impracticality to this?
I’d think that monthly digital dermoscopy would be superior to the patient’s own layman’s naked eye inspections, especially since the patient can’t possibly get an accurate view of his back; and that digital dermoscopy would take substantial guesswork out of self-exams.
Dr. Pacheco: Sure… but I usually recommend a baseline and then in six months. If moles are stable, I have them come back in a year.
Mole mapping has been hailed as highly effective for people with many moles/dysplastic nevi and a history of melanoma. However, what is your take on someone without “high risk” skin having digital dermoscopy done, say, once every six months, just for 1) peace of mind, and 2) superior detection over the layman’s naked eye, especially when it comes to viewing the back?
Dr. Pacheco: No system or doctor is perfect – so I am fine with patients requesting mole mapping. It does lessen the anxiety.
Although – usually after a couple normal/stable mole mapping sessions – they are fine with coming less often and letting me dictate control of their skin examination.
Can digital dermoscopy detect changes in a pre-existing mole before those changes can be detected with the most scrutinizing naked eye?
Dr. Pacheco: Yes.
In that case, what percentage of such early detection (when mole is biopsied and declared melanoma) are stage 0 or in situ? (very early melanoma)
Dr. Pacheco: I am not aware of statistical reports.
Are you aware of any technology on the horizon that will be able to scan the entire skin surface and thus detect malignant changes in their most rudimentary stages in non-mole areas?
No.
So if you are interested in the earliest detection of melanoma and are concerned about your risk factors, inquire about digital dermoscopy with serial photography to your dermatologist.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: molecheck.co.nz/mole-map.html
Digital Dermoscopy for Melanoma Detection: First Person Account

I underwent serial digital dermoscopy at University of Colorado Hospital, and here’s what it’s like.
I finally decided to have serial digital dermoscopy done for melanoma screening, something I’ve been putting off for several years.
If you clicked on this article, you probably already know what serial digital dermoscopy is all about, as far as melanoma detection.
My insurance did not cover this, so be prepared in that your insurance may not cover it.
Serial digital dermoscopy is done at only a handful of facilities in the U.S., including at University of Colorado Hospital.
My dermatologist did not authorize the digital dermoscopy because I am not considered high risk for melanoma; thus, I paid out of pocket.
However, I also paid for some peace of mind, as this cutting-edge melanoma-screening technology has been proven to detect melanoma in its earliest stages.
I received a full-body skin exam from a third-year dermatology resident (University of Colorado Hospital is a teaching hospital), followed by a full-body skin exam by a dermatologist.
The doctor then decided to have three moles on my back imaged; no others.
Apparently, their digital dermoscopy is mostly for just the back, since this is the hardest-to-view area of the body.
The three moles on my back did not stand out from any of the moles elsewhere on my body (i.e., legs and arms).
However, I can’t view the back ones well, due to their location. Two of these moles are very small.
Apparently, the reason that larger moles on my leg were not included in the imaging was because I can readily inspect them.
After the doctor marked, with ink near them, the moles on my back, I was led to the room next door for the digital dermoscopy.
I stood, back facing a nurse, who was at a computer console. She placed an imaging device to the moles (I couldn’t see the device, of course, but it obviously recorded the image into the computer).
My Moles Were on the Computer Screen
She then showed me the 20-times magnification of each mole on the screen.
What a mole looks like, magnified 20 times, is entirely different than what it looks like to the naked eye.
In fact, the appearance looks a little scary because it is much less exact, less defined, more diffuse, and (in the case of a normal mole) full of spidery-looking configurations that dermatologists refer to as the “network” of a mole’s pigment.
The nurse pointed out that the squiggly lines or network were actually very normal, and that if the image showed instead a more dense, solid mass of brown, it would be concerning.
In the computer system was also a full image of my back.
The images of the three moles, plus the full image of my upper and lower back, will comprise the baseline images, so that 12 months from now, new images of the same areas can be compared: serial digital dermoscopy.
It will be easy to detect early changes in moles with a 20-fold magnification – changes that even a doctor’s highly trained naked eye will not be able to detect, and changes that even a doctor’s handheld dermoscope will not detect.
The procedure was brief and after the third mole was imaged, the nurse sprayed cleanser on my back to wipe off the ink. And that was that.
Paying out of pocket is worth the peace of mind that serial digital dermoscopy will bring to “mole-conscious” folks concerned about melanoma.
However, serial digital dermoscopy does not replace monthly home skin exams or the yearly clinical exam.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Why Small Dogs Should Be Walked Even if They’re Normal Weight

My brother has had two small dogs (not fat, not even overweight) for a number of years and informed my mother that if she got a small dog, she wouldn’t have to walk it.
His exact words were: Small dogs don’t have to be walked.
Are you with him on this? And if so, is there a size cut-off? What if a small canine is part Chihuahua, part Golden Retriever? Hmmm.
It can get very confusing, trying to determine how small a dog needs to be to be exempt from being walked, and whether or not it’s a little overweight or moderately overweight, and taking into consideration its breed or mix of breeds — in order to require regimented walking for exercise. What a conundrum!
Whether or not your pet is overweight isn’t the issue; there are many other benefits to walking a small dog, says Dr. Liz Hanson, a doctor of veterinary medicine at Newport Animal Hospital in Newport Coast, CA.
Dr. Hanson points out that smaller breeds like the Maltese, Chihuahua and Pomeranian may be able to burn enough calories with normal activity inside the house to maintain a lean body.
But this doesn’t mean these small furry friends don’t need to be walked or given some form of outside exercise.
“Exercising your dog will help keep your small dog agile, limber and maintains good muscle tone which helps reduce arthritic pain as they get older,” explains Dr. Hanson.
“In addition, regular walks help keep your pet’s digestive system healthy and are beneficial to those with constipation issues.”
Does your small dog, that never gets walked because it’s trim, have unresolved constipation issues? Maybe it’s time to start taking Muffin for daily walks.
Or does little Princess bark too much? “Many small breed dogs have behavioral issues such as excessive barking, chewing, scratching and digging,” says Dr. Hanson.
“Walking your dog daily will help reduce and even eliminate many of these behavioral problems that often stem from boredom.”
Another reason to walk a small dog regardless of its weight is to help socialize it, says Dr. Hanson. “Smaller dogs kept mainly at home are often fearful of other dogs and people due to lack of exposure.”
Dr. Hanson notes that small breeds can be hyperactive; if your little pet has too much energy, chews furniture or jumps excessively, a regular walking program is just what the doctor ordered. This will help calm your pet down in the evening.
Do not let the absence of obesity or the presence of trimness guide you in whether or not to walk your small dog.
As you can see, taking a Pomeranian, Maltese or other tiny breed on regular walks can provide multiple benefits very unrelated to obesity or excess weight.
 Dr. Hanson grew up in Southern California, graduated from UC Davis and attended Colorado State University College of Veterinary Medicine. Dr. Hanson has worked in small animal general practice in Orange County for 15+ years. In her free time, she enjoys traveling, cooking, watching movies, and spending time with family and friends and her two dogs.
Dr. Hanson grew up in Southern California, graduated from UC Davis and attended Colorado State University College of Veterinary Medicine. Dr. Hanson has worked in small animal general practice in Orange County for 15+ years. In her free time, she enjoys traveling, cooking, watching movies, and spending time with family and friends and her two dogs.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Sudden Back Leg Weakness in Old Cats: 3 Common Causes

A veterinarian discusses three categories of causes of sudden hind leg weakness in a senior aged cat.
If your old cat has experienced sudden-onset weakness in its hind legs, there can be a serious medical cause for this.
Trauma As a Cause of Sudden Rear Limb Weakness in an Old Cat
Being hit by a car, falling from a height, or being accidentally struck or stepped upon can cause a senior cat’s back legs to suddenly become weak, says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
“With appropriate veterinary treatment, sometimes full control can be returned, but the first 24 hours are critical,” says Dr. Benson.
If you suspect trauma, get your cat medical attention as soon as possible.
Saddle Thrombus Can Cause Sudden Back Leg Weakness in Older Cats
A thrombus is a blood clot, which can be common in cats with heart disease.
Dr. Benson explains, “A blood clot dislodges from somewhere in the body, then lodges at the pelvic end of the aorta where the blood vessels split to go down the legs (an area known as the saddle), resulting in lack of blood flow to the legs.”
The aorta is the largest blood vessel and begins at the heart, distributing blood throughout the body with each heartbeat.
The condition is called feline aortic thromboembolism, and it’s very painful with an often poor prognosis.
“Treatment is aimed at dissolving the clot and controlling pain,” says Dr. Benson.
“Cats with cardiac disease are usually prescribed an anti-clotting agent to reduce the chances of an embolism like this occurring.”
Infection May Cause Sudden Hind Leg Weakness in an Old Cat
Infectious disease can arise from a number of sources that affect the brain, including tick-borne diseases, Cryptococcus, feline infectious peritonitis and taxoplasmosis.
As you can see, cancer is not on the list of sudden rear leg weakness in an older cat.
However, this list is not complete; it represents only the more common causes.
“As with many conditions, the prognosis improves the earlier it is detected, so bring your cat to the vet at the very first sign of any hind limb weakness,” says Dr. Benson.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/New Africa
How to Remove White German Shepherd Hair from Furniture

Anybody who’s ever had a white German shepherd (such as me) knows that these magnificent dogs shed quite a bit, and unless you keep up with this, there will be “hairs everywhere.”
Here are some ways to remove the hairs of a white German shepherd (they shed more than other breeds of GS) from your furniture.
Lint Roller
Always have these on hand. You can get them at discount bulk rates at Costco and Sam’s Club.
Just swipe the roller back and forth on your furniture.
For portions of furniture that sink down, that the roller misses when it rolls over, tear a fresh sheet from the tool and stuff it into the sunken area, scrunching it in there so that it makes contact and picks up the hairs.
Fabric Lint Brush
This tool will pick up white German shepherd hair when swiped in one direction, and then will deposit the hairs on the fabric portion of the tool.
The caveat is that you must then pluck off the clumps of hairs.
The plus is that there is no sticky, sometimes stubborn-to-tear-off sheets to deal with. These brushes are not disposable.

Rubber Brush
These come in different styles and shapes, and they do a good job at collecting the hairs of a white German shepherd that have found their way to your furniture.
This tool does not literally remove the fur, but it collects it into gobs that you can then remove with your hands.
Another way to remove hairs of a white German shepherd is to use a hand vacuum.
This works well in the corners of furniture where the seat cushion meets the back support.
Using specialized nozzle attachments will work in the areas that scrunched-up lint paper cannot effectively get to.
The key to keeping up with the shedding of a white German shepherd is to avoid skipping cleanup times.
To reduce the amount of shedding, you should brush your dog 2-3 times a day outside, and give the dog a bath once every few weeks.
A bath this often will not “ruin a dog’s coat.” The bath can be administered by simply sponging the white German shepherd with a sponge soaked in hypo-allergenic suds.
Then pour warm water from a bucket over the dog (several bucketfulls), at very close range so that it’s soothing.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top 5 Injuries BIG Dogs Get When Exercised Too Much

A veterinarian explains the most common injuries and problems that may affect a large dog when it’s exercised too much.
A large dog is prone to certain injuries or problems if he’s given too much exercise, such as being leashed to run alongside a bicycle over long distances.
Top 5 Injuries or Problems that Can Affect Large Dogs from too much Exercise
#1 Cruciate ligament tears: A tear of the cranial cruciate ligament (CCL) is the most common orthopedic injury to large as well as medium size dogs, begins Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
The CCL is analogous to our ACL in the knee.
A twisting or jarring motion is often necessary to tear or rupture the CCL. However, some large dogs are more vulnerable to this injury due to genetics, obesity or age.

Here is what Dr. Benson explains: “Most dogs require surgical correction to get back on all four paws, and many benefit from pre- and/or post-surgical physical rehabilitation, just like humans!
A 2005 study estimated that Americans spent over $1.3 billion on canine CCL repairs in 2003.”
#2 Next is lameness. There may be no visible reasons for this, notes Dr. Benson. An X-ray may be done to detect any broken bones.
If the X-ray is normal, a vet will likely advise a limitation on movement, certainly exercise, and maybe give a course of pain relieving medication.
#3 The third problem that can affect large dogs are exercised too much is broken nails. “Broken nails are not uncommon in athletic dogs and can occur on soft ground or hard surfaces,” says Dr. Benson.
Your vet may have to remove the end of a broken nail. The biggest risk from this is infection of the exposed soft tissue inside the nail, says Dr. Benson.
He further explains: “Since licking and chewing at the nail plays a major part in this, dogs with broken nails will often need to wear an Elizabethan collar (‘cone of shame’), and the nail will need to be kept clean.
“Keeping nails trimmed helps to avoid this issue, but dogs with recurrent broken nails may have underlying problems that your veterinarian can help diagnose and treat.”
#4 Lacerations and cuts are also more likely to occur the more a large breed (or any size) dog exercises outside.
One day I saw a man walking his large dog across the parking lot that led to a mountain trail head.
The dog was prancing with each step because on all four feet were special “booties” to protect paws from insults from the gravelly trail.
These can help, since too much wear and tear on paws can lead to cuts, abrasions or irritation, especially in cold weather, adds Dr. Benson.
#5 Heat stroke: “Over-exertion can lead to hyperthermia, or heat stroke, which can be life-threatening,” says Dr. Benson.
“A dog’s normal temperature usually peaks at around 102.5oF, but when it rises to 105-110oF, this can lead to coma, organ dysfunction and even permanent brain damage or death.”
Watch out for the warning signs which can be subtle, such as a drunken-like gait, restlessness, excessive panting or drooling.
Large dogs (and small) need structured exercise, but too much of a good thing can cause injuries or other problems.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: avmajournals.avma.org/doi/abs/10.2460/javma.2005.227.1604)
Cat Poop Guide: Color, Consistency, Shape, Contents

Here is a complete guide to cat stools from a veterinarian: what different shapes, colors, consistency and other features might mean.
It’s very important that you get comfortable with the idea of inspecting your cat’s poops on a recurring basis, because the caliber of a cat’s stools can be indicative of any number of medical conditions including cancer.
Cat Poop Color
“I get less concerned with stool color than I do with consistency and contents,” says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
He says that color is often related to diet. A healthy cat stool should range from very light brown to almost black.
Cat Poop Consistency, Shape and Additional Features
Dr. Benson urges cat owners to keep a lookout for the following in their pet’s poops:
Consistency: Very soft stools (diarrhea) can be caused by many disease processes, and if this is a consistent finding in the litter box (or elsewhere!), or if your cat seems “off” and there is diarrhea, you should consult your veterinarian, explains Dr. Benson.
Very hard stools, such as small, hard balls rather than long, formed stools, can be “a more insidious marker of disease,” he says.
If your cat’s stools are hard, this can indicate any of the following: Underlying dehydration, kidney disease, diabetes, overactive thyroid, some forms of cancer and other conditions.
“Hard stools can also lead to constipation or GI blockage,” says Dr. Benson.

More Features of Cat Poops
“Blood, mucus, parasites and foreign materials can all also indicate changes or problems,” says Dr. Benson.
Blood: If you see fresh blood in the stools, this usually means an abrasion of the colon, often caused by colitis.
This can be a primary disease process, or secondary to other conditions like inflammatory bowel disease, explains Dr. Benson.
That’s not all. Fresh blood in the stools can mean there’s bleeding in the lower intestinal/rectal region, possibly from cancer. However, colitis is by far more likely.
Mucus: This gooey substance in a cat’s poop usually indicates colitis.
Parasites: Yes, it’s possible for the owner to see segments of tapeworm, the size of rice, in the poops of outdoor cats.
Dr. Benson urges you and your vet develop a regular deworming schedule.
“Every annual exam, make sure you bring in a stool sample to be examined by your vet, even for indoor cats.”
Foreign materials: Cats are capable of ingesting non-food items, such as grass, string, stones and even Christmas decorations, says Dr. Benson.
This cat poop guide won’t do you much good unless you commit to getting used to viewing your pet’s feces on a regular basis, and then following up with your vet if you see anything concerning.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Cat Keeps Licking Mouth: Sign of Cancer?

Believe it or not, something as seemingly innocuous as mouth licking can be a sign of cancer in a cat, says a veterinarian.
Your cat has been licking its mouth a lot lately, and at first, you thought this was just part of your pet’s meticulous grooming, but you now are wondering if this could be a sign of cancer.
Most Common Cause of Excessive Mouth Licking in a Cat
Without a doubt, the most common explanation for why a cat frequently licks its mouth is dental disease, says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
“Red, swollen gums, bad breath, difficulty eating and frequent licking can all be signs of gingivitis (inflammation of the gums) and periodontal disease (inflammation of the structures supporting the teeth, including gums, bones and nerves),” explains Dr. Benson.
How can you help prevent such a problem? Make sure you take your cat to see the vet on a regular basis, advises Dr. Benson.
This should include dental check-ups and at-home dental care to help reduce the chances of any kind of periodontal disease developing.
Cancer
Now, if your cat shows one, a few or all of these symptoms, don’t assume it’s probably dental disease, because these same clinical signs — including mouth licking — could mean cancer, says Dr. Benson.
“By far the most common oral tumor in cats is squamous cell carcinoma,” he says.
According to Veterinarypartner.com, this cancer usually affects older cats, with the average age of diagnosis being 12.5 years.
The website lists the following as risk factors: sun exposure, use of flea collars, persistent consumption of canned food, and, believe it or not, smoking on the part of the owner.
In fact, if the owner smokes one to 19 cigarettes a day, the risk jumps up four times.
“Early recognition is the key to maximizing the chances for successful treatment, though the prognosis is always guarded in these cases because the cancer often spreads very quickly,” says Dr. Benson.
This cancer is treatable only when caught early.
Don’t wait till your cat is constantly licking its mouth to get comfortable examining its mouth on a routine basis or to look into protecting your cat with pet insurance policy that covers cancers as standard, advises Dr. Benson.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: veterinarypartner.com/Content.plx?A=2722&S=2
Can Diarrhea in a Cat Be Caused by Cancer?

Diarrhea in a cat can have many causes, and a veterinarian warns that cancer can actually be a possible cause.
Has your cat been experiencing diarrhea lately and you’re beginning to wonder if this could be a symptom of cancer?
Causes of Diarrhea in a Cat Include Cancer
“Yes, diarrhea can be a clinical sign of cancer, particularly gastrointestinal (GI) lymphoma,” says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
This cancer is the most commonly diagnosed type of cancer in U.S. cats, and in fact, comprises 20 percent of all cancers in U.S. cats. The risk spikes once a cat reaches the age of 7 years.
However, pet parents should be aware that symptoms of this cancer can mimic symptoms of benign conditions, as well.
“If there is a suspicion that cancer could be the cause [of the diarrhea], your veterinarian may have to conduct several tests to determine the root cause,” says Dr. Benson.
“Inflammatory bowel disease [another possible cause of diarrhea] and GI lymphoma (a form of cancer) often appear so similar, even at a cellular level, that full-thickness excisions from the intestinal wall are often needed to distinguish between them,” explains Dr. Benson.
Benign Causes of Diarrhea in Cats
Diarrhea is a common symptom and usually, it does not mean cancer simply because there are so many other causes.

Dr. Benson says these causes include food intolerances or allergies, internal parasites, metabolic disease or primary GI disease like inflammatory bowel disease (IBD). High fiber content can also cause some diarrhea.
Dr. Benson advises: “Because diarrhea can rapidly result in dehydration, it’s important to have your cat evaluated by a veterinarian within 24 hours of first seeing signs of GI upset, or sooner if your cat appears visibly sick or lethargic.”
Treatment Expense for Cancer
“Diagnosing and treating GI disease, especially GI cancer, can be a long, difficult and expensive process, which is why many veterinarians recommend pet insurance that covers cancers as standard,” says Dr. Benson, “to help cover these unforeseen costs.”
He notes that pet insurance has to be in effect before your cat or dog starts to show any kind of GI distress, diarrhea or other symptoms, in order for coverage to be available.
It’s a wise idea to start the insurance policy while your pet is healthy.