How to Prevent Weight Gain from Caregiving Stress

Here’s a no-nonsense way to outright prevent gaining weight no matter how stressful your caregiving tasks are, no matter how demanding your charge is.
I’m an exercise and fitness enthusiast, and former personal trainer, who had the experience of “extreme caregiving” for my 80-something mother during her numerous serious medical situations (severe depression, quintuple bypass surgery, constant fainting episodes, two brain bleeds and a hip fracture).
Food Provides a Relief from Caregiver Stress
A caregiver will often turn to food for comfort (and thus gain weight); the mental angst can be unspeakable.
Another reason a stressed-out caregiver may gain weight is because the time required to keep up with a supply of healthful food, and then to prepare healthful dishes, is no longer present.
Convenience-eating translates to junk food eating. Feelings of powerlessness encourage the stressed caregiver to eat well-beyond the point of satiation, and weight gain happens.
During my first round of caregiving (my mother had knee arthroscopy followed by crippling depression) I subsisted almost entirely on junk food and ate like a horse, while staying with my parents to take care of her.
Alongside that, I was battling against my father’s poor judgment as far as what should be done with her (e.g., he kept denying that she had full-blown depression and hence, was an obstacle to antidepressant treatment).
There were many trips to IHOP, Village Inn and Perkins (my mother was too disabled to cook).
Whenever we went out for breakfast I’d order the same thing: French toast, drenched in butter and syrup. I had given up cardio exercise and gained weight (around 15 pounds), but had continued lifting weights.
A small amount of “stress weight” is one thing, but a LOT of weight gain (i.e., 15 or more pounds) doesn’t have to happen. Never take up smoking to prevent this!
- Do NOT quit exercising just because you’re seeking comfort through food!
- Do NOT quit exercising just because you’ve gained some weight.
Though I lived on large quantities of junk food, this was no excuse for ditching the weight workouts. I ditched the cardio, but the weight workouts were far more valuable.
The stressed caregiver needs to get away, and when possible, should use that time wisely: a gym workout will do much more good than a trip to a bar to “unwind.”
Gym workouts, rather than spending inordinate amounts of time on social media, will help prevent weight gain or at least help prevent more than 15 pounds of weight gain.

Freepik.com
Exercise can also include yoga, which may sound too passive, but a yoga class–if your gym offers one–will provide a unique challenge to your body. This beats unwinding with “a few drinks” any day.
My mother completely recovered, I moved back home, resumed cardio, stopped living on junk food, and quickly got my lean physique back.
Second Caregiving Stint: No Weight Gain
Less than a year later…another tour of duty…the quintuple bypass surgery. The ensuing four months were a nightmare.
Somehow, someway, I made the time to do all my shopping at Whole Foods and eat a plant-based diet with minimal junk food. I continued cardio and never missed a weight workout.
There were many trips to restaurants, and I almost always ordered something healthy like grilled salmon, broccoli and a salad.
I always had to go with my parents to restaurants because my mother was prone to passing out, and my father, being a senior citizen with recent back surgery, was in no condition to support 135 pounds of fainting weight.
Throughout the stress of this second round of caregiving, I dropped 10 pounds in its first 30 days, despite eating more food than usual.
The emotional strain was enormous (my mother was non-compliant), but the one thing that gave me a sense of control was eating healthfully and stopping at the point of satiation.
So you see, if you put your mind to it, weight gain from caregiving CAN be prevented. A few pounds are okay, but there was no excuse for my 15 pound weight gain during that first stint.
Caregiver stress is all the more reason why the individual should stick to a rigorous exercise regimen and make every effort possible to eat healthfully.
By not gaining weight, you will feel more in control amid what seems to be a very out-of-control environment.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: pexels-liza-summer
Why Grown Kids of the Super Obese Keep Bringing Food to Them
Why do the grown kids of the super morbidly obese who can’t even walk across a room keep bringing them giant portions of junk food?
Bringing enormous amounts of food to one’s 900 pound parent is like bringing caseloads of whiskey to someone with liver disease.
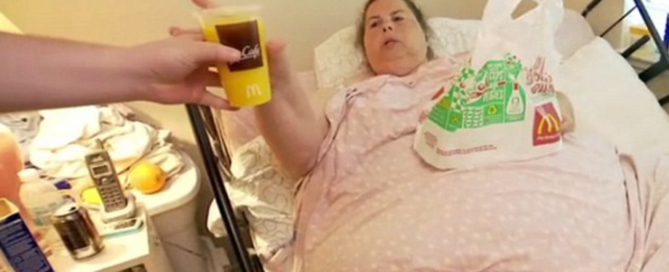
Renee Williams weighed about 900 pounds before she died, and the TV show depicting her life at this weight revealed that she lived with her two daughters, which made me wonder:
What enablers kept bringing this bedridden, essentially paralyzed woman all the food?
An online Daily Mail article (among other sources) notes that Williams would eat eight hamburgers in one sitting.
Her eldest daughter reported that Williams would eat till her stomach hurt.
Were her daughters participating in the enabling, bringing their mother some of the junk food she’d gorge on?
960 Pound Woman, Confined to Bed for Years, Didn’t Get that Way without Enablers
When I watched Williams’ story on TLC (“Half-Ton Mom”), the topic of who keeps bringing her so much food wasn’t dare broached, but the viewer could easily infer that Williams’ daughters were partially involved, simply because they were old enough to bring her food.
Presumably, at least one adult was part of the enabling process, since the daughters weren’t old enough to drive. It’s also possible that Williams received a large percentage of food from delivery people.
However, her oldest daughter, at the time of the TLC airing, was about 14 — old enough to take a stand against allowing excess food to get near her mother, who wasn’t even able to sit up in bed.
“It is common for adult children of addicts to develop their own addictive patterns,” says David Sack, MD, a psychiatrist specializing in addiction disorders, and CEO of Promises Treatment Centers in Malibu and Los Angeles.
“Many struggle with people-pleasing, an overdeveloped sense of responsibility, and fear of rejection or abandonment, which often manifests as codependency and enabling.”
Son Kept Taking Food Orders for Severely Morbidly Obese Mother
Another TLC program focused on a man about 19 who was shown leaving the house for and returning from food runs for his severely obese mother.
His mother was able to walk short distances in the house but not able to venture out shopping.
He’d bring her bags of candy bars, fastfood and other unhealthy items in alarming quantities, totally helpless at saying “No, I will not help you commit suicide!”
What’s odd is that it was not revealed what kind of stranglehold Williams had over her daughters, or what the second mother had over her adult son, that made it impossible for them to suppress the influx of food.
The mothers were never shown throwing temper tantrums or threatening to stop loving their kids.
Dr. Sack explains, “We often see adult children make excuses for a parent’s addiction or look the other way because they don’t want to disrespect or embarrass their parent, or perhaps they feel the parent has earned the right to behave as they please. Often, they’ve lost hope that change is possible.”
 Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Source: dailymail.co.uk/news/article-505198/The-half-ton-mum-Tragic-story-worlds-heaviest-woman.html
Morbidly Obese Reality Shows Ignore the Enabler Issue

Why don’t TLC shows about massively obese people confined to bed ever explore why their family members keep bringing them food?
Over the past several years there’s been quite a few TLC programs focusing on people weighing close to 1,000 pounds, showing gruesome footage of their gastric bypass surgeries and other unsightly details.
Yet not once spending some time visiting the enabling aspect of these situations — the enabling spouse or family member who keeps bringing tremendous amounts of food to their super obese loved-one who cannot get out of bed.
Is TLC afraid to broach the enabling component of super morbidly obese people?
Does TLC think that viewers would rather watch the surgeons slice away at grisly layers of fat to rearrange intestines — a most ghastly sight — than hear from the enabler why he or she is an enabler? These surgery scenes are extended.
The viewer doesn’t expect the enabler of super morbidly obese people to give a Freudian explanation; we just want to hear what they have to say — why they find it so difficult to just say no to the food addict.

What is TLC afraid of?
“Part of the problem is lack of awareness,” begins David Sack, MD, a psychiatrist specializing in addiction disorders, and CEO of Promises Treatment Centers in Malibu and Los Angeles.
“The public, and even the mental health field, has been slow to recognize that food can fuel addictive patterns in much the same way as drugs like heroin and cocaine.
“Just as family and friends can enable drug and alcohol abuse, they can become enablers to the food addict or compulsive overeater.”
TLC should devote an entire program to investigating enablers of obese family members who are confined to bed.
This would be far more intriguing than listening to the surgeon give commentary as he examines various folds of fat on the patient’s back.
“There also may be a reluctance to point the finger at people who, at least on the surface, appear to be trying to help,” says Dr. Sack.
“In many ways, obesity enablers are hostages and victims in their own right and require compassion and treatment just like the addicts they’re enabling.”
Nevertheless, I was so angry at Cheryl for becoming irate when a surgeon told her she had to help her 900 pound husband, Ricky Naputi, lose 100 pounds before he could qualify for surgery.
She stormed out of the room upon hearing this requirement.
But TLC didn’t explore why she reacted this way. It would have been LESS work for Cheryl to help Ricky lose weight — less food shopping, less food preparation, less cleaning, less money spent.
Why was she so mad? TLC owed viewers an explanation instead of leaving us hanging.
Maybe Cheryl was asked off-camera and refused to answer?
But what about the many other enablers? Do ALL of them refuse to share their insight about their enabling ways, yet have no qualms about revealing other issues such as no sex life or past sexual abuse?
Or perhaps some enablers have begged TLC to spend some time on the enabling issue, but TLC refused?
It’s anyone’s guess, because this component of the super morbidly obese lifestyle is kept well-hidden.
The only case I’m aware of in which the enabling was significantly focused on was the riveting case of Billy Robbins.
Much of the show centered on why his mother overfed him since childhood, such that by age 18, he weighed 800 pounds and spent most time in bed.
“Enabling is a topic morbidly obese individuals and their caretakers may be loathe to talk about because of the shame and confusion they feel,” says Dr. Sack. “They may avoid seeking help for fear of judgment from others.”
 Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Source: nydailynews.com/life-style/health/world-fattest-man-died-900-pounds-article-1.1353829
Enabler of Super Obese Family Member: Might YOU Become One?

Are you at risk of ever becoming an enabler to a family member who eventually gets so super morbidly obese that they can barely get out of bed or are even confined to bed?
They are being maintained in this condition by enablers (usually a spouse or family member) who keeps bringing them enormous amounts of junk food.
I’ve noticed that in every single case (and I’ve seen quite a few of these shows), the enabler is obese, often morbidly, but functional enough to be a caregiver/enabler.
I just can’t imagine that anyone who works out at a gym, has a physically fit body and eats mindfully could ever become an enabler such that eventually, their “enablee” gets too heavy to leave their bed.
You’ve heard of the “addictive personality” or “addictive brain.” Is there a such thing as an “enabler personality” or “enabler brain”?
Many women refuse to serve their husbands the amount of junk food they request; perhaps they are “anti-enablers”?
Though most functional obese people aren’t enablers, most enablers on the TLC shows are quite obese and don’t do any exercise.
It’s easy for me to believe, just based on the behavior of the enablers, that most were abused as children, or grew up in an emotionally corrupt household, stripping them of the capacity to engage in an emotionally and physically healthy adult relationship.
Inside the Mind of a “600 Pound Life” Enabler
“Anyone can become an enabler, but those with low self-esteem or who have difficulty saying no, expressing feelings, or setting and maintaining personal boundaries are most at risk,” says David Sack, MD, a psychiatrist specializing in addiction disorders, and CEO of Promises Treatment Centers in Malibu and Los Angeles.

More Risk Factors for Becoming an Enabler to a Super Obese Person
“Enablers believe they are bad or cruel if they don’t help and are afraid of what might happen if they don’t,” continues Dr. Sack.
“They feel compelled to take on other people’s responsibilities, sometimes out of guilt or fear, but also in an attempt to gain control.”
Enablers or those at risk put the needs and desires of others ahead of their own. This may sound noble, but when it leads to disaster, it’s destructive.
“In an attempt to protect themselves from victimization, they prefer to keep the peace than address the problem and deal with the potential fallout,” says Dr. Sack.
This begs the question: How extensive could the fallout be, when the bedridden food addict can’t get up and do anything?
What kind of frightening fallout was sweet, loving, 900 pound Renee Williams capable of inflicting upon her children if they stopped bringing her huge amounts of food?
“Most people learn codependent behaviors from their role models growing up, especially if they were raised in an addicted or dysfunctional home,” says Dr. Sack.
“Others may suffer traumatic experiences early in life, which contribute to low self-esteem, a fear of abandonment and other codependent traits.”
 Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Source: dailymail.co.uk/news/article-505198/The-half-ton-mum-Tragic-story-worlds-heaviest-woman.html
How Obese People Who Can’t Get Out of Bed Control Their Enabler

It’s been said that the super morbidly obese person is skilled at “manipulating” their enabler or caregiver.
What makes someone continuously bring huge amounts of unhealthy food to their loved-one who’s so obese that they’re confined to bed?
“As is the case with drug addiction, changes in the chemistry of the brain can cause people struggling with food addiction to manipulate others if that’s what it takes to get more of their drug (food),” explains David Sack, MD, a psychiatrist specializing in addiction disorders, and CEO of Promises Treatment Centers in Malibu and Los Angeles.
How does a bedridden person manipulate someone who can ambulate and drive?
“If the enabler tries to stop enabling, the food addict may use a number of strategies to elicit compliance,” begins Dr. Sack.
“They may use threats, guilt and heartbreaking pleas that are extremely persuasive, especially when used against someone who is codependent.”
Mysteriously, TLC, the cable channel that airs most of these types of shows, has failed tremendously at addressing the enabler aspect of the super morbidly obese.
The bedridden individuals, some weighing over 900 pounds, are shown as calm, sweet and loving, and rarely shown having any kind of meltdown, and when a little meltdown IS shown, it’s usually not related to being refused food, but for some other reason, such as not having lost weight.
Nevertheless, when a fit occurs due to not being given food, I just can’t figure out why it’s so hard for the enabler to ignore these little outbursts.
When my elderly mother was disabled from depression, it severely weakened her body.
I’ll never forget the time, in the middle of the night, she went to the bathroom to use the toilet.
I had gotten up to supervise in case she fell at any point. She was extremely non-compliant.
After she was done relieving herself, still sitting on the toilet, she told me to help her stand up.
I was sitting outside the bathroom, its door open, giving us a full view of each other. I knew she was capable of getting off the toilet if she put her mind to it.
I refused to be an enabler and remained seated. She got mad and demanded I come over and help her off the toilet seat.
My job was to supervise in case anything went wrong. Nothing more. I knew she could get up without my help.
Still on the seat, she looked at me fiercely and ordered me to help her up. “No,” I said. “I’m helping you by NOT helping you.”
Finally, she got up — and seemingly effortlessly. I then accompanied her back to bed (to make sure she didn’t fall). I just didn’t have it in me to be an enabler, despite my mother’s attempt to manipulate me.
I imagine that sometimes, super morbidly obese people make angry commands while in bed, using authoritative or pleading voices to manipulate their enablers.
The enablers, being already psychologically dismantled from childhood emotional trauma, are not able to oppose the demands or pleas.
Another possibility is that the enabler of the obese is the one in control:
Dr. Sack says, “Those who are morbidly obese are also vulnerable to being manipulated by the people around them, who may have their own unconscious emotional needs (for example, feeling better about their own situation or feeling needed).”
 Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
Dr. Sack is a sought-after media expert and has appeared on “Dateline NBC,” “Good Morning America,” “The Early Show,” and “The Doctors,” among many other outlets.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Whey Protein Benefit: Lowers High Blood Pressure

Whey protein may be a safe, cheap way to lower high blood pressure, a possible alternative to drugs that have side effects.
Lowering high blood pressure means cutting down on stroke and heart disease risk.
Whey Protein and Blood Pressure: Study
A study out of Washington State University found that daily consumption of whey protein resulted in at least a six-point reduction in average blood pressure of women and men who had pre-existing high blood pressure.
Though the 71 study participants were between 18 and 26 years, the study’s leader, nutritional biochemistry professor Susan Fluegal, says that older people with high blood pressure would probably get similar benefits from the whey protein.
Whey protein is low-cost and has not been linked to any adverse effects, says Fluegal in the International Dairy Journal paper.
In this study, results showed up in the first week and they lasted for the study’s six-week duration.
However, there were no results for study participants who had pre-existing normal blood pressure.
Whey Protein: Cause and Effect when It Comes to Lowering Blood Pressure
There may be a correlation between whey protein and a reduction in blood pressure readings, but a direct cause-and-effect has not been established.
“The Fluegal study and other studies supporting that whey protein can help reduce blood pressure have several variables that need to be researched further to ensure these findings are completely accurate,” says Dr. Keith Kantor, a leading nutritionist and CEO of the Nutritional Addiction Mitigation Eating and Drinking (NAMED) program, which treats substance abuse, mental illnesses and other illnesses.
Dr. Kantor explains, “I will say that the whey protein used in the studies was not sweetened — which results in less of an impact on insulin levels, resulting in less inflammation — which can help reduce high blood pressure if the person is consuming whey protein on a consistent basis.
“Whey protein is also very filling, which indirectly can reduce cravings and the consumption of processed and fried foods which both are linked to increased risk for high blood pressure.”
If you have hypertension, don’t assume that having a whey protein drink every day — all by itself — will knock it down.
Lower Your High Blood Pressure
Feel free to add whey protein (no sugar added) as a convenient break from meat, poultry and eggs. But to treat hypertension, you should do the following:
• Lower salt intake. Speak to your doctor about this.
• Increase intake of fruits and fresh vegetables.
• Replace refined grains with whole.
• Take up strength training and cardio exercise.
• Lose excess weight.
• Quit smoking or don’t ever start.
 Dr. Kantor has a PhD in nutritional science and a doctorate in naturopathic medicine, has appeared on CNN and Fox News Channel for his expertise, and has been an advocate of natural food and healthy living for 30+ years.
Dr. Kantor has a PhD in nutritional science and a doctorate in naturopathic medicine, has appeared on CNN and Fox News Channel for his expertise, and has been an advocate of natural food and healthy living for 30+ years.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Source:
sciencedaily.com/releases/2010/12/101208125624.htm
Low Blood Pressure: Symptoms, Dangers & How to Safely Raise

What are the symptoms of LOW blood pressure, how dangerous is this and how is it treated?
“Many people have ‘low’ blood pressure and are perfectly healthy,” says Susan L. Besser, MD, with Mercy Medical Center, Baltimore; Diplomate, American Board of Obesity Medicine and board certified by the American Board of Family Medicine.
“Assuming there is no reason for sudden low blood pressure — like dehydration, trauma, severe medical illness [e.g., right-sided heart failure] — if you are not having any symptoms, there is no need to be concerned about it.
“The most common symptom is fainting when you change position (like from lying down to standing).
“The treatment is to be sure you are well-hydrated and to add some salt to your diet (salt makes your blood pressure go up).” But don’t go overboard on the salt/sodium, either.
“There are prescription medications also, but you must talk with your doctor about that.”
Symptoms of Persistent Hypotension
In addition to dizziness or feeling light in the head, the suffer may experience any of the following: fatigue, blurred vision, nausea, trouble concentrating and even passing out.
The symptoms of a sudden drop in blood pressure can be caused by other conditions, but they are:
- Altered mental status, confusion or the appearance of being “totally out of it,” especially in the elderly
- Cold, clammy or moist skin
- Rapid shallow breathing
- Rapid weak pulse
This is a life threatening situation. The body is not getting enough blood. If the person has a pre-existing condition, namely chronic heart failure, a sudden drop in blood pressure is truly an emergency situation.
Many medical conditions and even prescription drugs can drop blood pressure.
The key issue, again, is how the patient feels despite the low blood pressure. For example, in a very fit, athletic individual, a BP reading of 90 over 67 may be normal.
But for an unhealthy, sedentary person whose BP is normally 130 over 80, a sudden drop to 90 over 67 could make them faint or feel ill.
Treatment for Low Blood Pressure
This depends on the cause, which a doctor can determine.
In the event of a more persistent low BP vs. an acute severe drop, the usual treatments include drinking more water, wearing compression stockings and taking a prescribed medication which can boost blood volume.
You should have a home blood pressure device and regularly take readings — after you’ve been sitting relaxed for five minutes.
 Dr. Besser provides comprehensive family care, treating common and acute primary conditions like diabetes and hypertension. Her ongoing approach allows her the opportunity to provide accurate and critical diagnoses of more complex conditions and disorders.
Dr. Besser provides comprehensive family care, treating common and acute primary conditions like diabetes and hypertension. Her ongoing approach allows her the opportunity to provide accurate and critical diagnoses of more complex conditions and disorders.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com/jcomp
Aortic Aneurysm: Are Pull-ups Safe to Do?
A leading aortic aneurysm repair surgeon answers if pull-ups are safe for patients to perform.
People who are diagnosed with an aortic aneurysm are typically warned that they must avoid straining with heavy weights.
This directive comes with a lot of ambiguity and is open to very subjective interpretation.
One hundred pounds sounds heavy, but to a trained powerlifter, it’s a walk in the park.
But what if a powerlifter is diagnosed with an aortic aneurysm?
Aortic Aneurysm, Pull-ups and Muscle Failure
The directive of do not strain with heavy weights would definitely apply to someone, diagnosed with aortic aneurysm, who is doing a set of pull-ups and keeps cranking them out, straining to get in those last two repetitions.
Straining is obvious because the last few reps are slow and labored, as opposed to knocked off with ease.
No matter how easy someone makes pull-ups look, he or she has a limit, when they begin approaching the so-called muscle failure, and the routine just becomes super nasty; pull-ups to muscle failure are a real bear.
A person with aortic aneurysm, even if he (or she) has been knocking off pull-ups for years and is in tip-top shape, must end their days of pushing to the limits with this compound exercise.
Percentage of the Rep Max
To make this easy to describe, suppose an athlete’s rep max with pull-ups is 12. He starts feeling the heat at around rep 8. It’s a royal strain to complete 12.
If he has aortic aneurysm, would it be dangerous for him to complete, say, seven reps?
After all, this would be before he begins entering the straining zone. Seven, for this particular athlete, isn’t all that difficult.
“Yes, a percentage of maximal effort is a good way to look at exercise,” says Allan S. Stewart, MD, a cardiothoracic surgeon at HCA Florida Mercy Hospital in Coconut Grove.
The amount of recruitment of additional muscle groups is what causes the increase in catecholamine surge and consequently, the increase in blood pressure delivered to the weakened aorta.”
A pull-up recruits a significant amount of muscle fibers; it’s a classic compound exercise. Seven reps out of the 12 rep max would be 58 percent of the maximal effort.

To another person who isn’t as strong, seven reps could be this person’s rep max, in which case, he should do only two or three.
Dr. Stewart continues, “Working to failure is better accomplished with dumbbells than with a straight bar or with pull-ups — places where it is difficult to assess the strain mid-rep and also difficult to stop without a spotter.
“It is much safer to exercise with specific muscle groups, lighten the weight, and work towards failure.”
Guidelines for Doing Pull-ups with Aortic Aneurysm
In summary, treat pull-ups as you would with any other kind of lifting: Avoid anything that makes you strain, grunt, groan or really struggle. If that’s just one pull-up, then don’t do it.
If you’ve been doing 50 pull-ups and that’s your rep max, and then learn you have an aortic aneurysm, you can still do pull-ups, but not 50 anymore.
Probably not 40. Which number rep is that entrance into the next level of difficulty? Stop short of that transition.
If you find yourself slowing down with the tempo, this means you’re entering the straining zone. Stop. Don’t go there.
Play it safe by quitting several reps before it even gets difficult (the levels are challenging, difficult, and then straining).
By doing submaximal pull-ups, will you lose strength? Yes. You can do 10 sets of three pull-ups if your rep max is seven or eight.
If the RM is higher, you can do more than three in a set, but don’t venture into the straining zone. If the tempo is slowing down, you’ve overshot the boundary.
Research into the danger of doing pull-ups with aortic aneurysm is nonexistent, but putting stress on a weakened great vessel means that you place yourself in danger of an aortic dissection or rupture. Play it safe.

A pioneering aortic disease surgeon for 20+ years, Dr. Stewart has performed 5,000+ open heart surgeries and is the developer of a hybrid endovascular procedure for treating complex aortic aneurysms. In 2013 Dr. Stewart was recruited to lead the Center for Aortic Disease at Mount Sinai Hospital, later promoted to Associate Professor of Cardiovascular Surgery.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lifting Weights with Aortic Aneurysm: Detailed Guidelines

Are you fed up with the vague, non-descript guidelines of weightlifting for thoracic aortic aneurysm?
Finally, here are guidelines that you can make sense out of.
A diagnosis of a thoracic aortic aneurysm doesn’t mean you must give up lifting weights.
There are several problems with the standard guidelines or “restrictions” for people with a thoracic aortic aneurysm, when it comes to lifting weights.
Weightlifting guidelines for those with a thoracic aortic aneurysm attempt to be a one-size-fits-all template.
Vague Guideline #1: People with thoracic aortic aneurysm should not lift more than half their body weight.
The problem here is that obese people (with thoracic aortic aneurysm) who’ve never done strength training get a free pass for lifting a lot of weight, while lightweight but muscular, strong people who’ve been training all along (and then learn they have thoracic aortic aneurysm) get “punished” for being lightweight.

Shutterstock/LightField Studios
According to this guideline, a 280 pound obese man gets to work out with 140 pounds, while a 160 pound highly trained man gets limited to 80 pounds, even though the 160-pound, muscular man may be significantly stronger than the 280-pound fat man!
In fact, the very heavy man may struggle and strain with just 90 pounds, while the smaller man easily hoists half the big guy’s weight: 140 pounds!
Which man, then, will have the greater blood pressure spike and thus strain his aorta more? The 280-pound, weaker man!
“Obviously, these recommendations are guidelines, and cannot be universally applied,” says Allan S. Stewart, MD, a cardiothoracic surgeon at HCA Florida Mercy Hospital in Coconut Grove.
“Fit people would have more ease in lifting heavier weights, but they are also the ones who are more likely to ignore the guidelines.
“Deconditioned people usually won’t lift 50 percent of their body weight, or they wouldn’t be deconditioned!”
Vague Guideline #2: People with thoracic aortic aneurysm should not lift more than 50 pounds.
Gee, does this mean it’s okay, then, for someone with a thoracic aortic aneurysm to lift 40 pounds – over his or her head – 20 times in a row?
A highly trained person with recently diagnosed thoracic aortic aneurysm may find it easy to lift 40 pounds over his head 20 times (no straining at all, and thus, no aortic root strain).
Whereas a deconditioned patient must strain just to push 40 pounds up only once. This guideline is way too ambiguous.
This vague guideline also doesn’t distinguish among different kinds of lifting.
For instance, a leg press of more than 50 pounds (e.g., 80 pounds) is very easy even for deconditioned people. So why should this be prohibited?
Whereas, a dumbbell bent-over row of 45 pounds would require most untrained women to strain – to do even one repetition, yet according to this guideline, it’s acceptable!
Dr. Stewart explains: “Isolated arm work, like dumbbell curls, will impose little strain on the root. The rule of thumb is that if you are stressing your core (things that make you go Hmmm!), it’s straining your root pressure.”
So if dumbbell curls are okay, does this mean it’s safe for women with aortic aneurysm to curl a 45 pound barbell (less-than-50-pound-rule), even if they must strain to get the reps out?
According to the International Registry of Acute Aortic Dissections: Patients often ask exactly how much weight it is permissible to lift.
Unfortunately, it is not possible to provide a blanket answer to that question, as it all depends on the patient’s size, muscular strength, physical fitness, and how the weight is actually lifted.
Rather than try to define a numerical limit, it may be more appropriate and useful to explain that patients can lift whatever weight they can comfortably lift without having to “bear down” or perform the Valsalva maneuver.
So if you can curl a 100-pound barbell without straining, the absence of straining is your clue that this resistance is not dangerous to your aortic root.
In other words, avoid anything that makes you strain, grunt, or want to grunt or moan.
Vague Guideline #3: Very frightening to those newly diagnosed with a thoracic aortic aneurysm who are weightlifters is when they hear, “Don’t lift more than 10 pounds.”

According to this rule, a highly trained individual, strong as a bull, but recently diagnosed with a thoracic aortic aneurysm, is now rendered prohibited from lifting his or her own baby and even a large watermelon!
The 11-pound bowling ball becomes a 9-pounder. Don’t move the ficus plant; don’t place the 15-pound dog in the car or handle a 12-pound suitcase.
Athletes or even sedentary people, newly diagnosed with a thoracic aortic aneurysm, will exclaim, “This can’t be real!”
A rule this strict is given because it virtually guarantees there will be no aortic dissection triggered by heavy lifting, and it’s easier for a cardiologist to be this strict than to open up the floodgates for endless questions that would result from broadening the restriction to 50 pounds or half one’s body weight.
Vague Guideline #4: People with aortic aneurysm should flat-out avoid lifting weights.

This restriction is the easiest for a physician to administer.
It minimizes patient questions about hypothetical scenarios involving weightlifting exercise or lifting weights on the job, and reassures the doctor that the patient was given the safest recommendation possible – should a dissection occur.
Dr. Stewart says, “. . .the variability (in guidelines) results from an ignorance about the contribution of weight bearing to the risk of dissection.”
Dr. Stewart adds that “the only real data comes from studies on athletes with normal aortas, where a pressure catheter was placed in the aorta during lifting.
“It was demonstrated that lifting an excess of 50 percent of one’s body weight puts a supra-physiologic stress on the root.
“It seems fairly obvious, that if the root is already diseased, then a supra-physiologic load would be bad.
“No correlation has ever been found, however, that weightlifting will lead to dissection.
“What does seem intuitive, though, is that subjecting a weak piece of pipe to high pressure, will further increase the weakness of the pipe until it breaks (or in the case of the aorta, dissects).”

A pioneering aortic disease surgeon for 20+ years, Dr. Stewart has performed 5,000+ open heart surgeries and is the developer of a hybrid endovascular procedure for treating complex aortic aneurysms. In 2013 Dr. Stewart was recruited to lead the Center for Aortic Disease at Mount Sinai Hospital, later promoted to Associate Professor of Cardiovascular Surgery.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/Mladen Zivkovic
Aortic Aneurysm: Is High Intensity Interval Training Safe?
A leading aortic disease surgeon explains about aortic aneurysm and high intensity interval training cardio.
If you’ve been diagnosed with an aortic aneurysm and have always been a fitness enthusiast, you’re likely wondering if high intensity interval training (HIIT) is safe.
Medical literature has very scant information on the safety of cardio for people with aortic aneurysm.
Apparently, there have been no studies on the risk of aortic aneurysm dissection in people who engage in high intensity interval training.

“The goal is avoid high stress on the aortic root,” says Allan S. Stewart, MD, a cardiothoracic surgeon at HCA Florida Mercy Hospital in Coconut Grove.
“To this end, the goal is to minimize the adrenaline rush.
“When looking at blood pressure during cardio, the biggest impact is in the first 10-15 minutes of exercise.
“To ameliorate that stress, I tell my patients to ramp up slowly. More specifically, I advise that runners start with a 15 minute mile and then gradually start to increase the speed.
“Cyclists similarly, should begin with a 12-14 mph speed for 15 minutes on flat ground before taking a steep hill.
“There is little in the way of hard scientific evidence to support these recommendations, but the goal is to allow for the body to acclimate to intensity.
“I do not advise anyone with an aneurysm meeting the criteria for repair, to do level 7 or above in intensity.”
In short, a person whose aortic aneurysm is less than 5 cm can safely do high intensity interval training – but the following criteria must be met:
The patient must also have a tri-leaflet aortic valve; must not have a connective tissue disorder; and must not be experiencing symptoms from the aortic aneurysm!
So does this mean that it truly is safe for a person with aortic aneurysm, to engage in high intensity interval training?
Here is what another aortic disease surgeon, Dr. Eric Isselbacher, says in a 2005 issue of the journal Circulation:
Aerobic exercise is generally safe, provided the patient does not have a hypertensive response to exercise.
Consequently, should a patient wish to engage in vigorous aerobic exercise (eg, running or biking), it is prudent to obtain an exercise treadmill test—on β-blockers and/or other baseline antihypertensive medications—to assess the physiological response to exercise and ensure that the systolic blood pressure does not rise above 180 mm Hg.
Minimizing blood pressure response will minimize stress on the aortic root.
According to Dr. Stewart, it can be safe for one with aortic aneurysm (not meeting repair criteria) to reach an intensity level of 7 and above – out of an intensity scale of zero to 10.
Ten means your fullest effort over a 30-second or less period of time.
Think of running up a hill as fast as possible. Level 10 high intensity interval training workouts can also involve pedaling, stepping and jumping.

Level 10 leaves you feeling battered and unable to talk.
Level 9 also produces compete breathlessness within 30 seconds, but a tiny portion of you feels you could have gone a wee bit faster or harder.
So how can high intensity interval training be safe for someone with aortic aneurysm?
Assuming that the patient meets the criteria mentioned previously, does not have a hypertensive response to cardio, and slowly ramps up, as Dr. Stewart advises, high intensity interval training will not strain the aortic root in one who has an aneurysm.
Don’t let the extreme tachycardia (increased heart rate), that follows a high intensity interval training segment, be misleading.
Panting forcefully to recover oxygen levels will not pressurize the weakened vessel wall of someone with aortic aneurysm.
The stress of high intensity interval training is on the lungs.
Dr. Stewart adds, “Sustained cardio is fine. It is not the length of the exercise, but how it commences that causes the difficulty.”
So how should one with aortic aneurysm commence high intensity interval training?
Do a 10-15-minute, slow ramp-up. Using a treadmill as an example, suppose your HIIT maximum speed is 10 mph (for 30 seconds), alternating with slow walking.
You will do a very brief run at 5, 6, 7, 8 and 9 mph preceding it – after you’ve warmed yourself up for 10-15 minutes with walking that escalates to a 4 mph pace.
To minimize a blood pressure spike, each submaximal speed interval will be preceded by a 10-second, 5 mph jog. E.g., when it’s time to run 8 mph, run first for 10 seconds at 5 mph, then run 15 seconds at 8 mph.
That 5 mph for 10 seconds will act as a bridge between the recovery walks and the speed intervals.
When you get to 10 mph, add another bridge: After the 10-second, 5 mph jog, run 5 seconds at 8 mph, and then jump to 10 mph for no longer than 30 seconds. After concluding any speed segment, always slow down gradually!
Yes, this is a lot of fussing around with the treadmill’s controls, not to mention the added burden of those bridges on your max efforts, but if you have a thoracic aortic aneurysm and want to safely do high intensity interval training, you must take precautions.