Tanning & Teens: Skin Problems from Actinic Keratosis

Yes, that deep bronze or golden tan on your young body looks awesome, but here’s a big question:
Why would actinic keratoses ignore you when it’s time to aggravate an adult who used to worship the sun? And, actinic keratosis is PRECANCER.
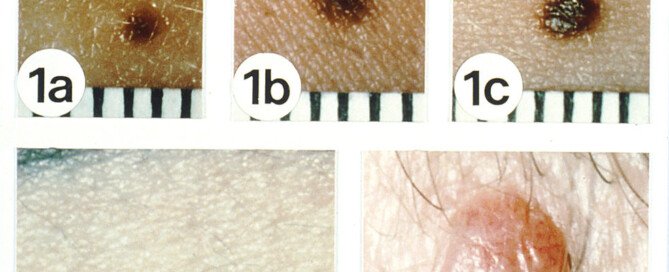
“Actinic keratoses are skin growths that occur from excessive ultraviolet ray exposure either from the sun or tanning parlor exposure,” says Dr. Janet Prystowsky, board certified dermatologist in New York, NY, with 30+ years’ experience.
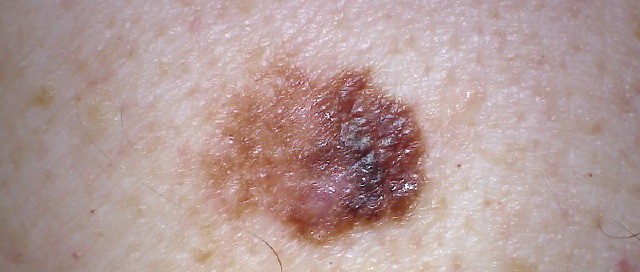
Getting these red, rough and scaly patches all over your skin is the result of lots of sun exposure during your youth and teen years.
I have three very tanned teen nephews and one golden-tanned teen niece, plus a few younger.
The three bronze tanned are 19, 17 and 14. The one teen, 14, and his 12- and 9-year-old siblings spend plenty of time in the sun every summer. The tanning is sowing seeds for getting actinic keratosis.
Teens may not care what happens when they’re older, but sometimes, your sun worshipping past will start to haunt you as early as in your 30s.
“Actinic keratoses do not occur early after excessive sun damage; typically patients are in their 40s or older,” says Dr. Prystowsky.
“Once they start showing up, however, it keeps happening and becomes a chronic skin maintenance concern requiring a dermatologist to guide through various treatment options.”
And though 40s may still seem like a long way from your current teen life, the time is NOW to start thinking how lousy things will be as an adult if your now tanned skin were potentially full of scars years later that may result (not always) from removal.
These red-pink, rough scaly lesions are sun damage and begin gradually, and may go unnoticed for a time, especially if located on the legs, back and feet.
Actinic keratoses are quite common, but the extent of developing these precancerous patches is quite variable.
An adult who always had a “healthy looking” golden glow as a teen may end up suffering from hundreds of actinic keratoses lesions by age 45.
If you’re a teen, is all the tanning worth it? Many teens avoid smoking, but then these same teens will bask in the sun and proudly show their dark tans.
Is the deep tan really worth it? It has been said that teens aren’t clueful enough to imagine their life years down the road. Do you think you’re this clueless? If not, then imagine how you want your skin to appear years from now.
Actinic keratosis is directly tied to sun exposure and tanning in youth, and has the potential to leave dozens and even hundreds of unsightly red marks all over one’s body.
“Treatment of actinic keratoses is advised because they can evolve into skin cancers called squamous cell carcinomas and possibly basal cell carcinoma,” says Dr. Prystowsky.
“If untreated and they have evolved into skin cancer, treatment is mandatory. If untreated, the skin cancers invade deeper into tissues and can have an adverse effect on local tissues as well as spread internally if neglected.”
Actinic keratoses are called precancerous lesions for good reason. Though only 5-10 percent of cases result in cancer and this typically takes years, it’s no picnic when it actually happens.
But even with those odds, who can actually feel secure having just been diagnosed with a precancerous lesion?
Pale skin is healthy and does not equate to poor health. DON’T FRY NOW and PAY LATER with actinic keratoses: precancer!

In combination with her focus on early skin cancer detection and removal, Dr. Prystowsky provides a wide range of revitalizing and rejuvenating treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Are Flat Moles Safer than Raised or Equally Prone to Melanoma?
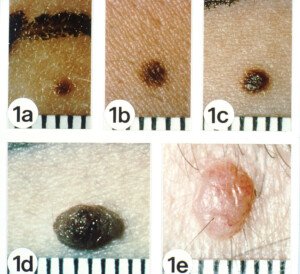
Have you noticed that some of your moles are raised, that is, clearly higher than the surface of the skin around them?
This doesn’t refer to moles that used to be flat and are now raised, but those that have always been this way—for as long as you can remember.
Perhaps you’re now wondering if these are more likely to transform into melanoma, a rare but deadly skin cancer if not caught in time.
So are raised moles more likely to develop into melanoma?
“NO,” says Dr. David Rahimi, MD, F.A.A.D., a board-certified dermatologist and cosmetic surgeon, and founder of Foreveryoung.net.
Dr. Rahimi explains, “The raised quality of a mole has nothing to do with its risk of malignant transformation or melanoma.”
Do you know your ABCDEs?
If you clicked on this article, you’re most likely familiar with the ABCDEs of checking lesions on your skin, so I won’t go into detail about this.
However, it’s reassuring to point out that Dr. Rahimi notes that the ABCDEs of screening for skin cancer do not mention anything about the “raised quality” of moles, birthmarks or freckles.
It’s crucial to get to know the natural marks and spots on your body so that, if they do begin changing in appearance, you’ll have a reference point.
Learn what’s normal for you. And have your skin checked by a dermatologist every year, even if this is not covered by your medical insurance.
Raised Moles Becoming Irritated
Depending on the location, a raised mole can receive recurring irritation from a piece of clothing.
This will not increase its malignant potential.
But if you decide to have a mole removed to avoid irritation or for cosmetic purposes, the rule of thumb is to always request that it be biopsied …
… not because it’s raised but because ANY mole that’s removed for ANY reason should always be biopsied.

Dr. Rahimi is the founder of Forever Young, Inc.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Black Area on Big Toenail: Melanoma or ??
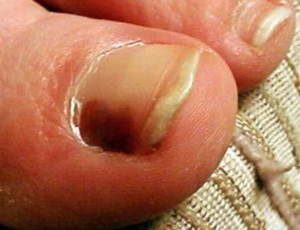
A black area or streak on the big toenail can have multiple causes, and one of them is melanoma.
What are all the things that a black spot or area on the big toenail can possibly mean?
“Fungus, bleeding under the toenail from trauma (talin Noire, runner’s nail), congenital mole, atypical mole, melanoma,” says Dr. David Rahimi, MD, a board-certified dermatologist and cosmetic surgeon.
What are the odds that this sign is melanoma?
Dr. Rahimi says, “Melanoma under the nail is very uncommon.
“I have seen four in 16 years of clinical practice. It is more common in patients with darker skin color: Asian, Hispanics and African Americans.”
Tell-tale features of melanoma?
“If the spot has been there for months, growing in darkness and size, and most importantly:
“Pigmentation in the proximal nail folds — meaning, the color is spilling into the skin portion of the nail. This is called the Hutchinson’s sign.”
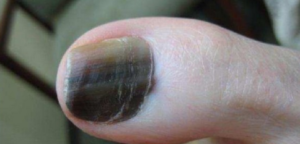
Hutchinson’s sign
NOTE: Melanoma in the toenail can occur even if the patient’s foot has had very little lifetime exposure to the sun.
Unlike other forms of melanoma that are typically linked to sun exposure, melanoma in the toenail may arise due to different factors, including genetic predisposition or other internal mechanisms that aren’t even fully known.
Diagnosis requires a biopsy, where a sample of the affected nail or surrounding tissue is examined for cancerous cells.
Unfortunately, there are no known preventive measures for the development of a melanoma in a toenail, whether it’s the big toe or the pinky.
What you can do is make sure you inspect your toenails and feet on a regular basis for any newly-developing dark spots, streaks, lines or smudge-like lesions.
Even if you habitually wear polish, at least make a point to give your toes a good view when it’s time to remove the polish.
Keeping your feet and toenails clean will also help in noticing unusual changes.
Always look at your feet! This includes between the toes and on the soles.
Have a dermatologist inspect your feet once a year.

Dr. Rahimi is the founder of Forever Young, Inc.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Atypical Melanocytic Hyperplasia vs. In Situ Melanoma
Are atypical melanocytic hyperplasia and in situ melanoma one and the same?
“Yes, I consider them the same thing; it all depends who is reading the slides,” says Dr. David Rahimi, MD, F.A.A.D., board-certified dermatologist and cosmetic surgeon.
I was inspired to write this article because I read about a man whose biopsy result came back “benign.”
He asked to see the report a few years later and saw the phrasing “atypical melanocytic hyperplasia” and then “in situ melanoma.”
He was alarmed that he had been told it was benign.
Pathologist Dependent
Dr. Rahimi explains, “Newer microscopes and staining of the tissue allow a pathologist to look at individual cells and make a judgement call.
“Five skilled and experienced pathologists may look at the same slide and have two widely different interpretations ranging from mildly atypical to severely atypical.
“The two sides of the spectrum, normal and clearly melanoma, are easily identified.
“Everything in between is fuzzy and has been ‘interpreted’ by the pathologist.
“Also, often the specimen is ‘cut again’ for additional slides to be taken to a new doctor for a second evaluation.
“These second cuts or deeper cuts may look different (better or worse) and this often complicates the issue.”
And by the way, whenever you have a mole removed — regardless of the reason — be it for cosmetic purposes, or because it gets irritated from clothes due to its location, or you just have a funny feeling about the spot — GET IT BIOPSIED.
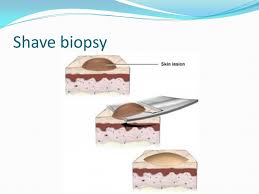
So what should you do when the biopsy report comes back?
Request to see the biopsy report of your mole or suspicious spot…immediately, and read it word for word.
“Atypical” refers to a cell that’s not typical.
“Hyperplasia” refers to excessive but benign growth; and “in situ” means very locally confined.

Dr. Rahimi is the founder of Forever Young, Inc.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/wavebreakmedia
Nodular Melanoma Can Spread in Just Days
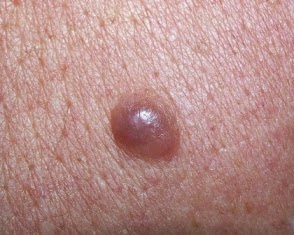
A dermatologist says, “Nodular melanoma can spread very quickly; within a matter of days or weeks.”
“A nodular melanoma can stay in the same spot for months and even rarely years; or spread into lymphatics and blood vessels very quickly.
“The consensus it that nodular melanoma does spread very quickly.
“In contrast, superficial spreading melanoma or melanoma in situ can stay in the same spot for years without spreading.”
What is nodular melanoma?
It’s a very rare form of skin cancer that grows more vertically than laterally or horizontally.
As the name implies, the growth looks like a nodule.
It typically presents as a raised, dark and sometimes irregularly shaped lesion, though it can also be reddish.
The rapid, downward growth can increase the risk of the cancer spreading to other parts of the body.
Shutterstock/Scio21
As mentioned, nodular melanoma is capable of rapid growth, meaning quickly growing in size — deeply penetrating downward into the skin’s deeper layers.
It can develop in regular skin or even within a melanoma of the superficial spreading type.
Nodular melanoma can occur in people with very dark skin, though this is exceedingly rare.
It’s not as associated with exposure to the sun as much as is the more common forms of this skin cancer, even though the most common locations are the normally exposed areas of the neck and head.
If you have a hard lump or nodular-shaped bump that’s new, and especially if it’s dark, black, itching, stinging or crusting, and if it seems to be growing or rapidly progressing, then get it checked out immediately. This includes a biopsy.

Dr. Rahimi is the founder of Forever Young, Inc.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can a Benign Mole Get Bigger, Change Color and Shape?
Warning signs for skin cancer include changing shape and colors in a pre-existing mole, as well as getting bigger.
However, can a benign mole undergo such changes?
I was motivated to write this article after seeing a photo of a large mole on a person’s back that was on a website for digital serial dermoscopy.
The serial images showed the mole changing and getting bigger in size, but the diagnosis ultimately was benign. This was quite surprising.
What a Doctor Says …
I then read a post in a thread about melanoma and moles, and the poster said that she had a mole that had become irregular in shape and multi-colored, but that the biopsy said it was benign.
- How can this be?
- Could a lab error be involved?
- How does a mole behave this way yet be benign?
- Let’s exclude some causes of changes in moles such as pregnancy and rubbing from clothes.
- I presented these questions to Dr. David Rahimi, MD, F.A.A.D., a board-certified dermatologist and cosmetic surgeon.
Dr. Rahimi explains, “Moles may change and still stay benign. Only a small percentage of moles in a predisposed person become malignant. Pathology could also have underestimated the degree of atypia.”
Atypia refers to cells that are not typical and thus more likely than typical cells to ever become cancerous.
If some of your moles have been identified as being atypical, you can always request that they be removed and biopsied for peace of mind, though sometimes a dermatologist will be the first to make this recommendation.

Dr. Rahimi is the founder of Forever Young, Inc.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Point Fr
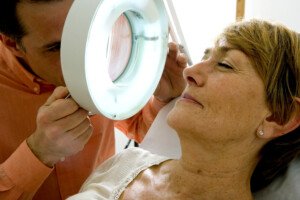
Skin Cancer on Scalp: Prevention Tips for Bald Men

Here is the bald man’s complete guide by a dermatologist on skin cancer prevention and detection on his scalp.
“Non-melanoma skin cancer is extremely common on the scalp in bald men,” says Dr. Joel Schlessinger, MD, board certified dermatologist and cosmetic surgeon with a private practice in Omaha, NE.
“Even melanoma is common there, and it is extremely important to guard against sun exposure if and when possible by wearing a hat (preferably brimmed) and sunscreen.”
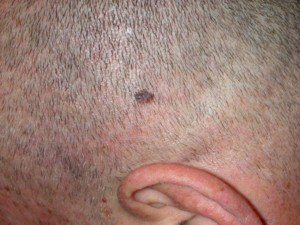
Melanoma
As a bald man, you may be hesitant to cover your pate when outdoors if this is the style you enjoy.
“Often the skin cancer can start off as a precancerous lesion called an actinic keratosis,” says Dr. Schlessinger.
A head full of actinic keratoses lesions is quite unsightly. Treatment for these red and pink, scaly splotches can leave scars.
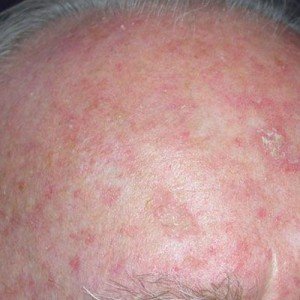
Actinic keratosis
But often, there’s no treatment because the bald man either doesn’t realize he has these lesions, or, he sees them but thinks they’re just a natural part of the skin’s aging process.
He may not even mind them that much, depending on how many or big they are.
But Dr. Schlessinger explains, “Over time it can progress to be a more significant issue, and if left untreated can develop into squamous cell carcinoma [a skin cancer].
“Other skin cancers such as basal cell carcinoma can also appear on the scalp.”
How often should bald men inspect their scalp?
“Men should inspect their scalp monthly if possible. If there is still hair present that makes it difficult, it’s possible to ask a hair stylist to take a look,” as part of the monthly routine. A partner or parent can also take a look.
Dr. Schlessinger continues, “If there are any suspicious areas they should be evaluated and possibly even biopsied.
“Skin cancers such as basal cell and squamous cell carcinoma tend to bleed if irritated, so that is a symptom to heed.
“Bald men should always apply sunscreen before leaving their home, but the important thing is that they should reapply every two hours while outside, so don’t leave home without a tube to replenish your sunscreen!

“Even on cloudy days there is sun and that sun will cause cancers if there is no protection.
“Hats are a perfect way to protect, but they should not be ball caps, as that way the ears are left out to the elements.
“A wide brimmed hat should be used to protect, rather than a ball cap for this reason.”
What is the most common cancer on the scalp of bald men?
“Generally, the squamous cell carcinoma is the most common form of skin cancer in bald men, but basal cell carcinoma is a close second,” says Dr. Schlessinger.
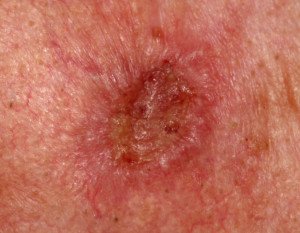
Squamous cell carscinoma. Shutterstock/Dermatology11
“Melanoma and a few less common skin cancers can also appear on the scalp.
“We are seeing an epidemic of skin cancer on the scalp as we see more sunlight and less protection from the ozone layer.
“The good news is that sunscreens are improving, but they need to be reapplied each 80 minutes if in water or sweating.
“Additionally, hats such as Tilley Hats, contain sun protection that will last for the entire duration of activities.”

So if you’re part of the bald is beautiful camp, this means taking excellent care of your scalp to always be ahead (no pun intended) of skin cancer.
And by the way, these guidelines apply to men with darker skin as well.
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/andrimka
Are Moles on Toes High Risk for Melanoma?
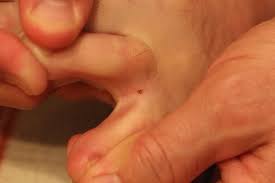
Many people assume that a mole on a toe is more likely to become melanoma, or, already is this deadly skin cancer.
“Moles on toes (and fingers) can be more concerning but aren’t usually melanomas,” says Dr. Joel Schlessinger, MD, a board certified dermatologist and cosmetic surgeon with a private practice in Omaha, NE.
“On the other hand (no pun intended!), they do tend to change more commonly and can turn into melanomas if they are exposed to the sun or tanning beds frequently.
“As a dermatologist, I always recommend my patients show me their hands and feet during a mole exam, as they can often be overlooked, especially when moles are between the webs of the toes.
“Anecdotally, I have seen a melanoma on the toe of an 18-year-old!
“It was caught when it was small enough that it wasn’t necessary to amputate, but if it had gotten much larger my patient would have lost his toe.”
What is meant by “they tend to change more commonly?”
“Moles on toes and fingers tend to be a little more likely to change from good to bad over time, so there is good reason to be concerned if one of these moles starts to turn darker over time,” says Dr. Schlessinger.
“Even those moles that are relatively ‘normal’ looking may be worthwhile showing to a dermatologist.
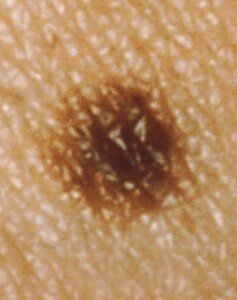
Common mole, 2 millimeters. Cancer.gov
“One of the reasons I suspect that moles on the hands and feet are bad actors is that people simply don’t examine these areas.
“For this reason, I always examine these areas when my patients come in for mole exams, even if my patients doubt there are any issues.
“It is shocking how many we find when we take the time to look!
“It is important to make sure your dermatologist takes the time to examine all areas of the body, including your hands and feet.
“Take off your shoes and socks if you are in the dermatologist’s office for a mole check.
“Also, make sure you lift up your feet so the dermatologist can examine them, and wiggle your toes so they reveal moles between the toes, if present.”
Prior to checking your feet, toes and between your toes for moles or any new spots, make sure that your feet, including between the toes, are thoroughly cleaned.
After all, a stubborn speck of dark debris can look very much like a suspicious mole.
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Itching Be the ONLY Symptom of Melanoma?
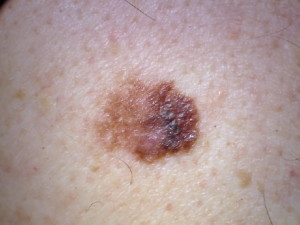
Perhaps you already know that an itching mole is a possible symptom of melanoma.
But what most medical sites do not say is whether or not this itching is almost always, or usually, or sometimes or rarely accompanied by other symptoms of a cancerous mole or lesion—such as crusting, bleeding, darkening or an increase in size.
“While itching is occasionally something that my patients relate as the symptom that brought them in for a mole or even a melanoma, it is very uncommon, actually,” says Dr. Joel Schlessinger, MD, a board certified dermatologist and cosmetic surgeon who has a private practice in Omaha, NE.
“That is why melanoma is so scary, as there can be no symptoms at all other than the changes in color. Moles, on the other hand, do tend to have times that they itch and even bleed.
“Interestingly, I have often seen patients who have presented with a very significant melanoma and they go so far as to state that they didn’t come in because it wasn’t itching ‘yet’.
“The important thing to remember here is that itch as a symptom that might be worth listening to is a very poor way to decide whether or not to see the dermatologist for a suspicious mole.
“While it may be a part of or reason to suspect that a mole is changing to be irritated, it doesn’t often correlate with the onset of a melanoma.”
If you suspect that a mole is itching, first be sure that it’s actually the spot that’s presenting with this symptom.
In other words, perhaps there’s a tiny bug bite only a centimeter away from it that’s the source of the itching.
Or maybe there’s some other irritant very close by that was caused by a stiff tag on your clothes.
But if you’re sure it’s the mole, the itching more likely than not has a benign cause if the spot otherwise looks normal, unchanged, non-evolving.
The irritation may have been caused by clothing.
Nevertheless, it won’t hurt to have a dermatologist examine it; don’t sit back and think, “Well, I’ll just keep an eye on it to see if it starts changing color or getting bigger before making a doctor appointment.”
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Does Melanoma Risk Disappear After a Certain Age?

Can you be too old to get melanoma?
Is it true that if you have never gotten melanoma by a certain age…you’ll probably never get it?
If this is true, how is it that advancing age is a risk factor for melanoma?
“Dermatologists used to see about one melanoma a year and perhaps two if they had a very busy practice,” explains Dr. Joel Schlessinger, MD, a board certified dermatologist and cosmetic surgeon with a private practice in Omaha, NE.
“Now, they routinely see 12 or more a year and the melanomas straddle every age, including 80+ year olds!”
I know a man who, when he was 89, a dermatologist performed a skin exam, pronounced everything as being normal, and told him he probably would never get melanoma if he’d lived this long without ever developing it. I thought, “What?!”
Why are more melanomas being diagnosed including in the 80-something year-old group?
Dr. Schlessinger explains, “The reason for this is that the sunlight exposure has become stronger over the years with the ozone layer becoming depleted.
“Additionally, as sun habits have changed, older individuals have now been exposed to recreational sun much more than in the past and that leads to increased risk for melanoma.
“That doesn’t mean that they have as many melanomas as younger individuals, but it does mean that every age needs to protect and be aware of skin changes.
I find that moles on older individuals are often benign (no risk) but that when I see a melanoma in an older individual it tends to be more aggressive.
“Additionally, with the advent of newer medications for conditions such as rheumatoid arthritis and conditions such as multiple sclerosis that can actually make melanomas more likely, it is important to be checked more thoroughly by your dermatologist.
“Additionally, it is important to protect your skin, whatever age you are!”
 Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
Dr. Schlessinger, founder of LovelySkin.com, has 25+ years of experience treating many skin conditions including melanoma. He’s founder of the Advanced Skin Research Center, a clinical facility that investigates new medications and treatments.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.