Gurgling from Stomach: Could this Be Acid Reflux?
Is that gurgling inside your stomach coming from acid reflux, cancer or what?
Now, gurgling from your stomach can be either annoying, embarrassing or scary (if you read somewhere that it could be a sign of cancer or even a brewing condition involving your heart).
Can Acid Reflux Cause a Gurgling Sound in the Belly?
“No — When your GI tract moves, it generally causes a gurgling noise,” says Jeffrey Fine, MD, chief of gastroenterology at the Medical Surgical Clinic of Irving.
“This is part of the natural digestive process and not due to acid reflux.”
What are the symptoms that acid reflux does cause?
The most common symptom of this very common condition is a burning or slightly abrasive feeling in the chest and/or upper abdomen.
However, the chest or abdominal discomfort from acid reflux isn’t always of a burning nature.
It can sometimes be described as a dull ache, strong ache or a pressure or heaviness.
The chest symptoms of acid reflux can mimic those of heart disease or of a heart attack.
Another common symptom of acid reflux is “burping” up a small amount of bitter tasting liquid after eating a meal — especially if you ate a lot of food in a short period of time.
The good news is that a gurgling stomach — either that which you can hear or only feel — is not cause for alarm.
The GI tract is supposed to move. The esophagus and intestines contract as part of the digestive process.
The esophagus and intestines are made of muscle, and muscle in the GI tract moves things along to get food digested. This movement is called peristalsis.
If you hear it, that’s normal. Whose stomach doesn’t gurgle sooner or later?

Dr. Fine has been in practice for over 30 years and specializes in digestive health, integrative medicine and food sensitivities.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Mix and Match Studio
Can HIIT Trigger Acid Reflux?

Are you wondering if high intensity interval training can bring on acid reflux?
“Yes. High intensity training can trigger acid reflux for some people, depending on what type of exercise the person is doing and how that person is wired,” explains Dr. Jeffrey Fine, MD, the chief of gastroenterology at the Medical Surgical Clinic of Irving.
“High intensity training can trigger acid reflux for some, depending on what type of exercise the person is doing and how that person refluxes,” says Dr. Fine.
Symptoms of Acid Reflux Brought on by High Intensity Interval Training
You may get a dull aching or burning in your upper abdomen.
If the acid reflux makes it higher up into your throat and mouth, you may start getting an unpleasant taste in your mouth.
This taste won’t be strong or sharp, but rather bland and dull. It may taste the way you’d imagine cardboard might taste. It may have a bitter quality to it.
It can come on within five minutes of your cardio exercise.
Dr. Fine explains, “Everyone is wired differently, neurologically speaking. Some people experience reflux only when lying down; others when sitting or standing up, and some experience it in either position.”
Can acid reflux be prevented during intense cardio training?
If you’ve been experiencing reflux symptoms as a result of HIIT, see what happens if you eat a small amount of food prior to the exercise, since an empty stomach can make you more likely to develop symptoms.
Many people perform HIIT on an empty stomach, namely to maximize the fat-burning effect.
But a small item of healthful food won’t disrupt this process.
Choose a something like a small peach, apple, banana, grapes or a little yogurt.
Another approach is to more gradually ramp your work intervals, to give your stomach a change to acclimate to the uptick in physical activity. This may result in less acid reflux.

Dr. Fine has been in practice for over 30 years and specializes in digestive health, integrative medicine and food sensitivities.
 Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified through the American Council on Exercise. At Bally Total Fitness she trained women and men of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/Razoomanet
Tiny Red Speck on Tissue Paper not Always Blood
Find out what that tiny red speck on your toilet paper after wiping yourself might actually be.
Recently after wiping myself after having a “number 2,” I noticed what appeared to be a very small, faint red splotch on the tissue paper.
I couldn’t get a good close-up of it with my contact lenses on (yes, I need an updated prescription).
I was sure I wasn’t imagining the red appearance—a faded red, not a bright red.
So I popped out the contact lens, and put the tissue paper up close to my unaided eye, while covering the other eye, for a good clear inspection.
The red speck appeared to be elevated off the tissue paper. Blood doesn’t do this. That’s not blood, I thought.
With my fingernail I lifted the red speck off the tissue paper and onto my finger.
It was several fibers from some kind of garment—obviously from the red sweat pants I had worn the day before.
Conclusion: Fibers from the red sweat pants had made their way into the entrance area of my anus.
They remained there till the next day when a good wipe dislodged them and attached them to the tissue paper.
It had definitely looked like blood when it wasn’t close up and clear to my eye.
Next time you think you see a tiny speck of blood on the tissue paper after wiping yourself, get a really close, sharp look at it to see if it might instead be a few fibers of clothing material.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Anger Cause a Heart Attack or Stroke?

There really IS some truth to the saying, “If you don’t calm down you’ll have a heart attack.”
You’ve heard of extreme sudden fear causing a heart attack soon after, but can anger (which is a completely different emotion than is panic or fright), also lead to a heart attack or stroke?
Yes, says a study. The increased risk of heart attack or stroke, following an episode of anger, persists for up to two hours after.
The heightened risk, predictably, is much worse for people who have pre-existing risk factors for heart attack or stroke.
The study report says that high frequency of anger episodes increases the risk.
How does this all convert to numbers?
– In those with frequent outbursts of anger, five episodes per day would mean about 158 extra heart attacks per 10,000 individuals with low cardiovascular risk annually.
– The number of heart attacks jumps to 657 per 10,000 people in those who have a high cardiovascular risk.
“For people who already have issues with their heart or may have narrowed blood vessels supplying their heart, this [anger outbursts] can cause less blood flow to the heart and cause potential for heart attacks,” says Bethany Doran, MD, a board certified cardiologist and CEO of Enabled Health.
Nevertheless, a solid cause-and-effect relationship has not been established, when it comes to anger and heart attacks.
In other words, maybe people who frequently get angry are also more likely to have a high sodium junk food diet, smoke and/or not exercise.
On the other hand, mental stress drives up heart rate and blood pressure.
The so-called fight or flight response makes the blood thicken: nature’s way of protecting the body from bleeding out from the anticipated fight or escape).
The more that a person is in the midst of a stress response, the more often their blood is in a thickened state, which means it can clot more easily.
Problem is, modern man’s anger often takes place in a setting where he can’t fight or flee — such as at the workplace or stuck in a traffic jam on the way to an important appointment.
What can you do?
“Lowering risk factors for heart attacks by eating correctly, exercising and maintaining a healthy body weight can decrease risk factors for heart attack,” says Dr. Doran.
• Limit processed foods. Eat foods in their whole form as much as possible. For example, eat potatoes fresh from the produce section, not from a can.
• Keep sodium intake under 2,000 mg/day.
• Make efforts to lose excess weight via more exercise and portion control of food.
• If you smoke, quit. Limit drinking: eight ounces a day for men; four ounces a day for women.
• Do both aerobic exercise and strength training.
 Bethany Doran, MD, MPH, is a board certified cardiologist and CEO of Enabled Health, a hybrid in-person and virtual clinic that expands healthcare in rural areas and prevents readmissions for vulnerable patients managing chronic disease. Her work has been supported by grants from the NIH, American Heart Association and New York Academy of Medicine.
Bethany Doran, MD, MPH, is a board certified cardiologist and CEO of Enabled Health, a hybrid in-person and virtual clinic that expands healthcare in rural areas and prevents readmissions for vulnerable patients managing chronic disease. Her work has been supported by grants from the NIH, American Heart Association and New York Academy of Medicine.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Why You Suddenly Can’t Breathe for a Few Seconds

Do you have spells of “I can’t breathe!” that last maybe five or seven seconds?
Instead of allowing this to scare the pants off of you, see a doctor to get to the bottom of this frightening symptom.
My mother was having sporadic incidents in which she’d report, “I can’t breathe.”
Of course, she was able to breathe but said it was difficult.
She was not panting, winded or out of breath as one might be after running up a few flights of stairs.
The trouble breathing would last, as my mother said, “seconds,” and had no apparent trigger, frequently occurring when she was seated, or standing passively. Exertion did not bring it on.
If all your tests “come back normal,” it’s likely that the reason you have very brief episodes of difficulty breathing is anxiety related or a panic attack, even though right before the brief episode of breathing trouble, you weren’t thinking of anything worrisome.
Breathing Problems from a Panic Attack
“Panic attacks can cause a change in one’s ability to breathe,” says Walter Gaman, MD, FABFM, board certified in family medicine and the author of several award-winning books including “Age to Perfection: How to Thrive to 100, Happy, Healthy, and Wise.”
“Holding breath or gulping for air can be a sign of other conditions, but when all other medical tests are within normal limits, a panic attack should be considered,” continues Dr. Gaman.
“Stress and anxiety are real and panic is caused by an over-stimulation of the fight or flight response within the body.”
My mother has congestive heart failure and an ejection fraction of 25 percent, but her cardiac nurse was more interested in the idea that fluid buildup (from the CHF) was causing the episodes of I can’t breathe.
“An older patient who has a known heart failure may experience an inability to breathe,” says Dr. Gaman.
“If the chest X-ray is normal, showing no fluid or enlargement of the heart, the shortness of breath could be caused by an SVT, supraventricular tachycardia.
“This is when the heart speeds up due to a problem with the electrical signals within the heart.”
My mother’s chest X ray was normal.
There was no weight gain and no edema.
Her other cardiac tests were normal: EKG, echocardiogram (though it did show weak left ventricle—the reason for the 25 EF), blood pressure, pulse, pulse-ox, chemical stress test.
Several years ago she had coronary bypass surgery.
If episodes of SVT had been occurring only while she was at home, making her suddenly “unable to breathe” for a few seconds, these transient events would not have been picked up at the ER.
She saw a pulmonologist who ruled out COPD. The pulmonologist did not believe that the very brief episodes of difficulty breathing were caused by a lung disease or even a heart problem.
When lung disease does cause problems breathing, the episode would not just suddenly come and go and last so briefly without any exertion or pattern; it would be more of a persisting situation.
Furthermore, my mother has no other symptoms that the doctor asked about, such as dizziness, fever, lightheadedness, tingling, numbness, nausea, visual problems or rashes.
The only symptom is the periodic sensation of “I can’t breathe.”
The pulmonologist said it’s probably either anxiety related or a vocal cord dysfunction.
And remember, a panic attack can occur in the absence of precipitating worrisome thoughts.
The “program” for panic attack often runs in the background—like a computer program running in the background—not readily apparent, but there.
“Anyone [young or older] experiencing a sudden lack of breath should seek medical attention,” says Dr. Gaman.
If you’re having episodes where you have trouble breathing, and it’s not related to exertion and seems to come on for no reason at all, and are brief (lasting only seconds), get your heart and lungs checked, but it’s probably panic attacks.
Get the more serious causes of trouble breathing ruled out first.

Dr. Gaman is with Executive Medicine of Texas and is with the Staying Young Radio Show 2.0 podcast.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ShotPrime Studio
Hydralazine (Apresoline): Is 300 Mg Daily an Overdose?
Here’s the scoop on accidentally taking 300 mg a day of hydralazine (Apresoline) instead of the prescribed 30 mg a day.
My mother’s cardiac nurse made a mistake which resulted in the pharmacist preparing her prescription for hydralazine (Apresoline) at 10 times the amount ordered by the cardiologist for high blood pressure.
About a month and a half after my mother began taking hydralazine, my father (who takes charge of all the medications) noticed a mistake:
The bottle said that each pill was 100 mg, but the dosing instructions on the bottle said to take one “10 mg” tablet three times a day.
Was this just a typographical error on the bottle, or were the tablets, that my mother had been taking at this recommendation for about a week, really 100 mg?
Well, when my father went back to the pharmacy to investigate, he compared the newly prepared, 10 mg pills to the ones in the 100 mg bottle, and they were smaller.
Initially she’d been taking just one 10 mg tablet a day. It was then increased to twice a day. Then the instructions came in for three times a day.
My father then noticed the 100 mg on the new bottle, but at first didn’t think much of it—until a week later when he just happened to notice the dosing instruction for “10 mg” three times a day.
So instead of 30 mg a day of Apresoline, my mother had been taking 300 mg a day.
My father said he was on “pins and needles” and refused to dispense to my mother any more of the pills, to clear the perceived overdose out of her system.
He called the cardiologist’s office—this was Friday. The cardiologist was out for the day.
I learned about this on Saturday and did some online research about hydralazine overdose.
I could not find how many mg of this Apresoline drug constituted an overdose, but was relieved to learn that 300 mg a day is actually a common prescription—after it gradually gets raised to this amount.
In fact, one site said 400 mg a day was sometimes prescribed, and one site even had it up to 800 mg.
Furthermore, the half life of hydralazine or Apresoline is three to seven hours, sometimes eight, meaning that half the amount of the drug is already cleared from the system in this time frame.
However, symptoms of an overdose can be the following: faintness, passing out, muscle aches, ankle swelling, chest pain, rapid heart rate.
My mother had none of these. But then again, 300 mg a day is a standard prescription amount.
However, a patient is never jumped from 30 mg a day to 300 mg a day overnight, either.
On Monday morning my parents received the phone call they were waiting for, and the cardiologist’s office told her there was no problem with the 300 mg accidental dosing, and that ironically, the doctor will probably want to go up to 300 mg a day over time anyways.
Hydralazine is a vasodilator—it opens up blood vessels so that more blood could flow through the body.
Lesson learned: Always make sure that you KNOW the dose that the doctor has prescribed, or that the doctor has changed (increased or decreased).
Make sure that this number MATCHES what’s on the prescription bottle.
Read the prescription bottle very carefully, even if you need a magnifying glass.
Have the pharmacist recite to you what the prescription is for. This is your right as the consumer!
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/daizuoxin
Sources:
drugs.com/dosage/hydralazine.html
rxlist.com/apresoline-drug.htm
drugs.com/sfx/hydralazine-side-effects.html
webmd.com/drugs/drug-8662-hydralazine+oral.aspx
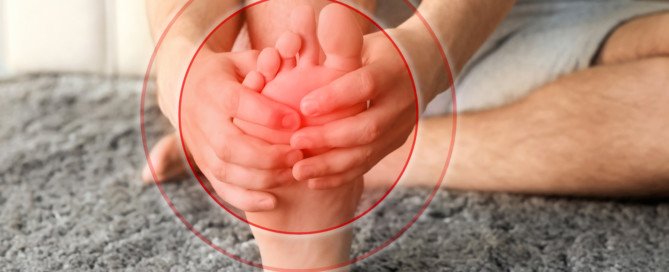
Pain in Ball of Foot when Cycling: Causes, Solutions
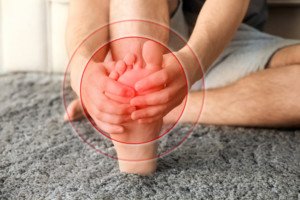
A doctor explains that there are several possible causes to a pain in the ball of the foot when cycling.
This can occur while riding outdoors or while using a stationary bike.
There are several possible causes of pain in the ball of your foot when pedaling a bike.
“Pain in the ball of the foot, especially when cycling, can be due to several issues,” says Nere Onosode, DPM, of OrthoCARE, which specializes in all elements of orthopedic medicine including foot, ankle, knee, hip and shoulder care.
Footwear
“The simplest solution is usually the most missed. Addressing the type and size of shoes used to ambulate and/or ride is important.
“Full length arch supports with forefoot padding can help alleviate pain at the ball of the foot.”
Make sure that your footwear is designed for cycling, or at least, exercise.
Don’t assume that an indoor “exercycle” doesn’t count as enough exercise to warrant proper footwear.
In other words, avoid wearing sandals or flip-flops while pedaling (people have been known to do this).
As for arch supports, these are sold online and at drug stores; no prescription required.
There are many varieties, and you may need to try several different versions before finding the right ones.
Musculoskeletal Causes
Dr. Onosode explains, “From a musculoskeletal standpoint, it could be a bone issue from crowding of the metatarsals that make up the ball of the foot, or entrapment of nerves that run in between those.”
You may even have a hairline fracture of a metatarsal bone, which an X-ray would likely show.
A hairline fracture of a metatarsal bone is a small, often subtle crack in one of the long bones in the foot, which can occur due to repetitive stress or trauma.
This type of fracture is typically characterized by a thin, non-displaced crack that may not always be visible on standard X-rays but at least can be detected with advanced imaging techniques if symptoms persist.
Dr. Onosode adds, “Also, inflammation of the bursa can cause pain. If the pain is related to inflammation, a simple OTC anti-inflammatory pills can help resolve that.”
Bursitis occurs when one of the small fluid-filled sacs that cushion bones and tendons becomes irritated or inflamed.
This condition commonly affects the bursa located at the base of the toes or under the heel.
The inflammation can result from repetitive stress, improper footwear, or direct trauma.
Treatment can also include ice. In some cases, physical therapy or injections may be recommended to reduce inflammation and alleviate discomfort.
In summary, pain in the ball of your foot should not happen while cycling.
If it doesn’t go away despite icing, self-massage and taking a break from the exercise, see a doctor.
 Nere Onosode, DPM, is a Doctor of Podiatric Medicine and board qualified by the American Board of Foot and Ankle Surgery.
Nere Onosode, DPM, is a Doctor of Podiatric Medicine and board qualified by the American Board of Foot and Ankle Surgery.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Africa Studio
DVT Prevention after Joint Replacement: Portable Compression
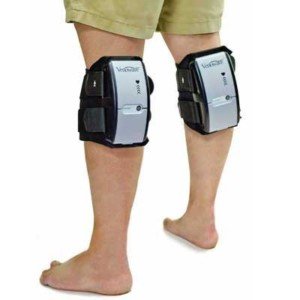
DVT (blood clot) prevention after joint replacement surgery can be done with a portable compression device that straps onto the legs.
The standard of care following joint replacement surgery is to send the patient home with a prescription to take a powerful blood thinner drug to prevent the development of a DVT: deep vein thrombosis.
Sometimes the surgeon will instruct the patient to take only aspirin.
Whether the patient takes a prescription blood thinner (Coumadin) or aspirin depends on the surgeon’s viewpoint on these two drugs as well as the patient’s medical history and other unique factors.
However, there is a third way to help prevent post-op blood clots following joint replacement surgery.
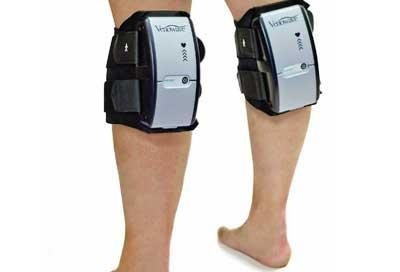
Portable (Mobile) Compression Device
The Shiley Center for Orthopaedic Research and Education at Scripps Clinic has conducted research and the report is in a 2015 issue of Journal of Bone and Joint Surgery.
The conclusion of the study is that a portable, strap-on compression device is just as effective as blood thinners in the prevention of a DVT.
The patient can easily walk around with the device on (walking would be limited by the joint replacement surgery itself, however, as the patient heals from the operation).
The device can be used by patients at their home for 10 days, or even longer, following joint replacement surgery—in place of a blood thinner, to stave off a blood clot formation.
Patients should inquire about this device to their surgeons prior to the operation.
Blood Thinners vs. Compression Device
“The risk of bleeding with blood thinners has to be weighed against its benefit in preventing blood clots,” says Dr. Paramjit “Romi” Chopra, MD, founder of the Midwest Institute for Minimally Invasive Therapies (MIMIT), an interventional radiology and endovascular therapy practice.
“Long-term use of blood thinners is not recommended if patients are mobile and at lower risk of DVT once they resume their usual level of activity.
“Lower extremity compression devices, including portable sequential compression devices and even compression stockings, can reduce the risk of DVT.
“They may be a better option in patients at higher risk for bleeding, such has patients with history of GI bleeding.”
Dr. Chopra combines his Eastern roots and 30+ years’ Western experience to unify the best of both worlds at MIMIT to treat venous disease, peripheral artery disease and musculoskeletal disease.
combines his Eastern roots and 30+ years’ Western experience to unify the best of both worlds at MIMIT to treat venous disease, peripheral artery disease and musculoskeletal disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Source: sciencedaily.com/releases/2014/02/140214152050.htm
Percentage of Liver Disease Patients with Bad Body Odor
Find out the percentage of people with liver disease who have bad body odor.
What percentage of patients with liver disease have the bad odor?
What’s really odd is that when I do a search on “causes of change in body odor” or “causes of foul body odor,” liver disease is on the list.
But when I do extensive searches on “symptoms of liver disease,” not one of these sites, including esteemed sites like Mayoclinic.com, lists body odor as a symptom.
So just what is that percentage?
“It’s a small percentage, less than 10%, maybe even less than five percent,” says Jeffrey Fine, MD, chief of gastroenterology at the Medical Surgical Clinic of Irving.
“A patient will only have that distinctive odor when they’re in liver failure, and most patients with liver disease do not progress that far.”
Why is the percentage so small?
Dr. Fine says, “We can speculate that this is because the only liver disease patients who experience this symptom are the ones in liver failure and that is a small percentage of patients.”

Dr. Fine has been in practice for over 30 years and specializes in digestive health, integrative medicine and food sensitivities.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.