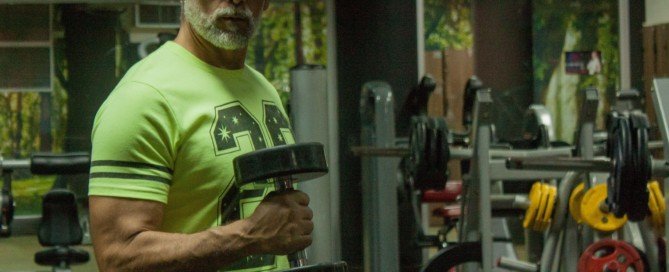Why Can Acute Stress Sometimes Cause Chest Pain?

Here’s a cardiologist’s explanation for how sudden stress can sometimes cause chest pain.
It can feel like a heart attack, especially when you remind yourself that there’ve been cases in which a heart attack indeed was set off by an acute episode of severe stress.
“Acute stress can lead to chest pain by causing the muscles of the chest wall, the back, the neck or the face to contract and tighten, leading to a sensation of pain,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“Acute stress can also raise your blood pressure which can place an increased burden on your heart, causing pain.
“When stress happens suddenly, the body is not prepared for it.
Even a normal response to stress can feel very abnormal.”
Do chest muscles spasm?
“Any muscles can spasm, especially when under stress,” says Dr. Denier. “The chest muscles can do this, causing pain. The diaphragm and the esophagus can also spasm which sometimes mimics heart pain.”
The esophagus’s composition includes striated and smooth muscle, so it definitely has the capacity to spasm.
“Acute stress and release of catecholamines can trigger spasm of the esophagus,” says Dr. Denier.
“Most often, esophageal spasm occurs while someone is eating or drinking something.
“It is more common in women and people with reflux disease or anxiety.
“Sometimes specific foods can trigger it.
“The important thing is that the symptoms can be exactly the same as a heart attack and should always be reported to your doctor.”
To minimize the harmful effect of stress on your heart, you should take up some form of intense exercise at least twice a week.
As for the benign chest pain, strength training and yoga would be a great combination to help keep the musculature less vulnerable to uncomfortable tensing up.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/tommaso79
What Does Chest Pain Only when Breathing Mean?

The good news is that chest pain only when breathing probably doesn’t mean a heart attack, but the real bad news is that it likely means that there is something else wrong with your heart.
Causes of chest pain only when breathing can involve the heart, though this does not necessarily mean a heart attack.
“Chest pain while breathing is called pleuritic chest pain and usually means there is inflammation involving the lining of the lungs and/or the heart,” explains Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
This is not related to a heart attack or clogged coronary arteries.
Dr. Denier continues, “When there is inflammation of the lining of the lung it is called pleurisy. Inflammation of the lining of the heart is called pericarditis.
“Both can follow an innocent upper respiratory infection or viral illness. This type of pain is worse on a deep inhale or with movement or lying flat.
“Both are relieved by anti-inflammatory medications and will go away once the inflammation is gone.”
These are not minor conditions. They DO need prompt medical attention. If you’re experiencing pain in the chest only when you breathe in — and it’s significant pain — get to the emergency room.
A Few More Causes of Chest Pain only While Breathing
Dr. Denier says, “Chest pain with breathing can also be caused by pneumonia which would usually also be accompanied by a cough and a fever.”
Unlike viral pneumonia, bacterial pneumonia doesn’t produce a fever.
However, a family member should never take the sufferer’s word for it that they says they “don’t feel warm.”
Take that person’s temperature yourself even if they insist, “I don’t feel hot.”
“Severe coughing can sometimes lead to a rib fracture which causes considerable pain with breathing,” adds Dr. Denier.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ShotPrime Studio
Which Side Chest Pain More Likely Means Heart Attack, Illness?
A cardiologist explains which side that chest pain is more likely to mean a heart problem or attack.
“Typically, left sided chest pain is more common in patients with angina and/or heart attacks,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“This is because the heart is located slightly more to the left of the chest.
“There are patients who experience right sided chest pain and truly have heart disease.
“This is called referred pain and can travel anywhere like the jaw or the arm.
“Women can have symptoms that are not typical of the usual angina and this includes right sided chest pain.
“Very rarely, we do see people with a heart on the right side of the body! This is why it’s so important to report any chest pain to your doctor.”
Chest pain on the left side of your chest can have benign causes, but you should report anything that concerns you to a cardiologist, with the idea that a cardiac problem can be ruled out.

Heart attack symptoms

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
How Does Sudden Emotional Stress Cause Angina?

Sudden stress or anxiety has a specific way of causing angina or chest pain, even in healthy people.
A person who does not have heart disease (plaque buildup in the coronary arteries) can still experience chest pain as a result of anxiety or stress.
When a person has chest pain from a shortage of oxygen in the heart, caused by clogged arteries, this is called angina.
“Mental stress leads to the release of catecholamines in your body, hormones that help your body to protect itself,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“This is the body’s ‘fight or flight’ mechanism. Catecholamines cause an increase in your heart rate and blood pressure which increases your heart’s need for oxygen.
“Catecholamines can also cause your blood vessels to constrict.
“Sometimes the heart can pump so hard that it cuts off its own blood supply by squeezing the coronary arteries! All of these mechanisms can lead to chest pain.”
Non-angina chest pain from stress can cause chest pain as well.
In this case, muscle tension and shallow breathing, especially in the chest and shoulders, can cause the discomfort in that area.
Prolonged tightening reduces blood flow, causes fatigue and micro-spasms, and sensitizes pain nerves, producing chest wall pain without heart involvement.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Charnchai Saeheng
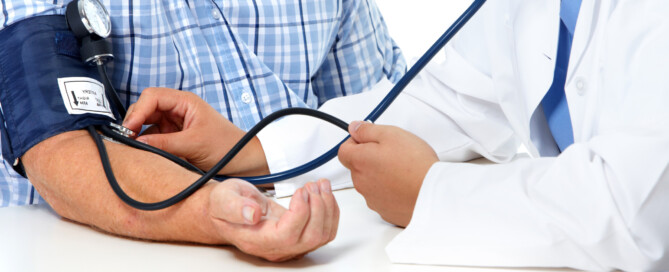
How Doctors Can Tell if High Blood Pressure in One Arm Is Serious

If your doctor finds that the blood pressure in one of your arms is high but not the other, this is serious and needs to be pursued.
“Doctors evaluate you based on many factors, not only physical findings,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“The first thing your doctor considers is your overall risk of any diseases such as cardiovascular disease,” she continues.
“There are risk factors known to put you at increased risk of a dangerous event like a heart attack or stroke.
“These risks include diabetes, high blood pressure, high cholesterol, smoking and a family history of early heart disease.”
A Study
“A study has shown that consistent readings of blood pressure with differences of 10-15 points between the two arms is a marker for increased risk of heart attacks and strokes.”
This is one reason why it’s so important to periodically take your blood pressure in both arms. It’s easy to do at your kitchen table.
“A new finding of a very large difference between the two arms would trigger your doctor to do further investigation with testing,” says Dr. Denier.
“The most sinister cause of differences in the blood pressure in both arms is aortic dissection or a tear in the aorta.
“It would be very unusual for someone to have this condition without other obvious signs and symptoms.
“The doctor would be looking for these signs very carefully even if he or she does not seem to be” having an aortic dissection.
The most blatant symptom of an aortic dissection is a ripping pain in the chest, which can radiate to the back.
But if you don’t have chest pain but still have big differences in blood pressure in your arms, see a cardiologist.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Alexander Raths
High Blood Pressure in One Arm: Serious Problem or Not?

Should your doctor be alarmed if you have high blood pressure in one arm and what does this mean?
“High blood pressure in one arm is something that is important to notice and report to your doctor,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“If your doctor seems unconcerned, it may be because he or she already knows you well and understands your medical conditions and what is normal for you. Do not assume this, of course.”
Have you discovered, using a home blood pressure gadget, that one of your arms has high blood pressure?
“It’s always wise to bring a finding that concerns you to your doctor’s attention,” says Dr. Denier.
“It’s common to see small differences in the blood pressure readings of each arm.
“Differences of 20 millimeters of mercury for the systolic or 10 mm Hg for the diastolic may be a sign of a health problem.
“This can be caused by narrowing of the blood vessels that travel to that arm.
“Other things that may cause this are chronic kidney disease, diabetes or atherosclerosis, all of which are risk factors for cardiovascular disease.”
My father has a history of having high blood pressure in one arm—not that high, but in the low range of what would be considered “high.”
He was told to take a reading daily and record the numbers.
He doesn’t have diabetes or chronic kidney disease, but he does have heart disease.
His coronary calcium score three years ago was 1195. Over time, the particular arm eventually began yielding readings under 140/90. His doctor was never alarmed over this.
Alert your doctor if you discover that the blood pressure in one arm is higher than the other.
Nevertheless, your doctor should know if you’ve uncovered this phenomenon via a home blood pressure gadget, to see what this finding may mean for your unique medical situation.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Syda Productions
What Blood Pressure Higher in One Arm Can Mean

What can it mean when one arm has higher blood pressure than the other?
“Blood pressure readings come from the blood flowing through the vessels in the arm (or leg) which can be heard with a stethoscope,” says Donna Denier, MD, with The Cardiology Center with the Appalachian Regional Healthcare System.
“When readings are significantly different on both sides (20 systolic points or 10 diastolic points), it suggests that the flow of blood is different on the two sides,” continues Dr. Denier.
Blood Flow Differs on Both Sides of the Arm: Why Is This?
Dr. Denier explains, “Things that block flow in the arms are the same as those which cause blockage in the coronary arteries or other arteries in the body.”
This means that the arteries in the arm are clogged with the same fatty deposits or plaque that are involved with coronary artery disease.
“Diseases like chronic kidney disease and diabetes or conditions like high cholesterol or habits like cigarette smoking can all lead to blockage in the arteries anywhere in the body,” warns Dr. Denier.
“Finding it in the arms can be a warning that other vessels may also be blocked.”
If the blood pressure of one of your arms is higher than the other, you should undergo cardiac testing to see if your coronary arteries might have blockages.
One such test is the treadmill (or stationary bike) echocardiogram stress test. It measures blood flow through the three main coronary arteries during the exertion of exercise.
Home BP Measuring
• Before taking the measurement, make sure you have been seated and calm for five minutes.
• Do not cross your legs, not even at the ankles. They should be in a co mfortable, relaxed position and not up against anything. Keep them still, including your feet.
• The device’s cuff should be against bare skin, not clothes, for optimal accuracy.
• Keep the arm that’s being measured resting on a table, desk or the chair’s arm rest.
As innocuous as this finding may seem — that blood pressure is higher in one arm — you should report this to your doctor if you’ve discovered it with a home blood pressure device.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ kurhan
Chest Pain: Persistent vs. Intermittent vs. Sharp vs. Dull Ache

Here is what a cardiologist says about different kinds of chest pain like sharp, dull, persistent, intermittent.
How can the different types of chest pain—constant, intermittent, sharp and dull/achy be distinguished from each other?
“Chest pain that is intermittent and related to physical and/or emotional stress is more likely to be angina and related to the heart,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“With any intermittent pain, it’s important to look for the things that bring it on like exercise, eating or coughing.”
When a pain or ache of a come-and-go nature strikes, make a note of this: time, body position, recent foods eaten.
See if a pattern develops over time. For example, you may find that almost always, a particular type of brief aching in your chest occurs one or two days after your chest workout at the gym.
“Sharp pain is more likely to be inflammatory in nature, where dull pressure or tightness is more like cardiac pain,” says Dr. Denier.
Though a dull pressure or tightness is a common description in the symptom lists of gastroesophageal reflux disease, do NOT assume this is what you have before you’ve had your heart checked!
Though acid reflux is very common, so is heart disease.
Furthermore, a dull pressure or tightness in the chest, that isn’t correlated to food intake or related to acid reflux, is great cause for concern.
If it’s not heart related, it can still be potentially serious—like a bleeding ulcer in the upper esophagus.
“Persistent pain is usually not caused by the heart unless the person is having a heart attack.
“Angina comes and goes. Pain can be differentiated based on the other symptoms and findings that go with it and the risk factors for that particular person.”

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Oleg Golovnev
If You Upchuck for no Reason, Could It Be Caused by Angina?

Vomiting can definitely be related to a problem with the heart, including angina.
“Angina can lead to vomiting, and it is one of the important signs of a heart attack,” says Donna P. Denier, MD, of The Cardiology Center with the Appalachian Regional Healthcare System.
“Vomiting can be a response to any pain. It is caused by stimulation of the autonomic nervous system.
“When it occurs in the presence of chest pain, it is very concerning.”
Two days before my mother underwent emergency quintuple bypass surgery, she had a few episodes of light vomiting, following an episode of difficulty breathing. Two days later she had chest pain.
After her second ER visit in three days she was diagnosed with unstable angina, and that evening had the bypass surgery.
“Other signs to look for are sweating, pale cool skin. These are all signs that someone may be having a heart attack.
In some patients, such as women and diabetics, nausea and/or vomiting may be the only symptom of the heart in need of oxygen.”
HOW does angina lead to vomiting?
“Vomiting in the presence of chest pain is caused by increased activity of the autonomic nervous system,” says Dr. Denier.
“The ANS is stimulated when a person is under severe stress and suffering from pain.
“Internal organs can become stressed when they do not get enough oxygen and that can trigger the ANS leading to nausea and/or vomiting.”
Two Main Types of Angina
Angina pectoris is chest pain resulting from reduced blood flow through the heart.
The stable type means that the problem occurs in response to physical exertion or emotional stress like anger.
Unstable angina refers to reduced blood flow at rest, for no apparent reason.
This can even occur while someone is asleep, and then the chest pain wakes them up.
In such a case, it’s not likely they’ll be awakened by the need to vomit.

Dr. Denier has been practicing medicine for over 20 years and is board certified by the American Board of Internal Medicine – Cardiovascular Disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/InesBazdar
Bodybuilding Guidelines after Heart Bypass Surgery (CABG)

Straight from a cardiologist, here are the guidelines for bodybuilding after having heart bypass surgery, a.k.a. CABG.
CABG stands for coronary arterial bypass grafting, and there are two kinds of patients when it comes to bodybuilding:
1) Those who wonder if they can continue bodybuilding after they recover from the heart bypass operation, and
2) Those who’ve hardly ever touched weights, but would like to take up bodybuilding once they fully rehabilitate from their CABG.
“Assuming the patient underwent cardiac rehab successfully, he should be able to perform strenuous activities including weightlifting,” says Pilar Stevens-Cohen, MD, FACC, Department of Cardiology, South Nassau Communities Hospital.
“Even a patient who has sustained permanent damage from an MI [heart attack] or has heart failure following CABG, should be able to begin strength training. The physical limitation would be based on symptoms only.”

So if you’ve been into bodybuilding all along, then you can resume it without a hitch — once you have completed your post-op cardiac rehab program.
“Assuming the patient is fully revascularized with no residual blockages that were left unaddressed, there is no limitation,” says Dr. Cohen-Stevens.
In case you’re wondering how a bodybuilder would wind up needing heart bypass surgery in the first place, consider the following:
Some bodybuilders hardly ever, if at all, do structured aerobic exercise. Next, steroid use can damage coronary arteries.
But in non-steroid users, you must consider a lack of aerobic exercise, and a diet that promotes systemic inflammation (which can lead to heart disease).
Not all bodybuilders have Zen-like diets or are faithful to cardio-centric exercise. Remember, their goal is physique sculpting, not running long distances.
If you’ve had (or will have) heart bypass surgery but have never done any bodybuilding, but would like to take up this endeavor, then once you complete your cardiac post-op rehab regimen, your biggest issue will be the orthopedic element of strength training.
That is, you don’t want to rush into lifting heavy weights simply because this can strain untrained tendons and muscles.
The biggest limitation, then, in the novice is that of an out-of-condition musculoskeletal system.
So though your heart may be doing just fine and may be ready for some more serious strength training, your rotator cuffs or low back structures may require a slower entry into more serious weight lifting.
Dr. Steven-Cohen also explains, “Patients should keep in mind that not all coronary disease is revascularized, and CABG is not ‘all new arteries,’ and you may not be completely symptom-free.
“We are able to open moderate to large size vessels that have a significant blockage (> 50%) with symptoms.
“Disease in smaller vessels or diffuse disease, may not be addressed with a stent or bypass.
“It is possible to have symptoms because of these blockages that would require titration of medication and may limit ability to exercise.”