Does Benign Multiple Sclerosis Actually Exist?

“While it is true that many people with multiple sclerosis have a ‘benign’ course, it is difficult to predict who will be in this lucky group,” says Dr. Kantor.
“There is a lot of controversy surrounding the classification of benign multiple sclerosis,” says Daniel Kantor, MD, director of the Neurology Residency Program, Florida Atlantic University.
Dr. Kantor explains, “While it is true that many people with multiple sclerosis have a ‘benign’ course, it is difficult to predict who will be in this lucky group.
“This is why many of us MS specialists see ‘benign multiple sclerosis’ as an after-the-fact diagnosis that can only be made retrospectively.”
MS occurs when the immune system turns against itself, and attacks the sheath that covers nerves and the nerves themselves. This disorder can come and go, yet also rarely leave people bedridden.
I’m a certified personal trainer and one of my clients had multiple sclerosis in remission; she was able to perform all sorts of workout routines.
Sometime after our sessions ended, I heard she had a relapse and was temporarily bedridden.
“There are probably many more people with multiple sclerosis than the 450,000 in the U.S. (and 2.5 million worldwide) commonly quoted,” says Dr. Kantor.
“Firstly, this is an old number from a study years ago; multiple sclerosis remains under-recognized and most people with MS live and die (after a normal life) with multiple sclerosis and don’t even know it.
“Most people with multiple sclerosis do extremely well and respond dramatically to the disease modifying agents (mostly injectables).”
Many famous people have MS, and perhaps the most famous contemporary person who has it is talk show host Montel Williams. Other famous people with MS include:
Neil Cavuto, Fox News Channel anchor; Lena Horne, actress/singer; Alan Osmond, one of the Osmond brothers; and Richard Pryor, comedian.
“There is another problem with the ‘benign’ multiple sclerosis category,” continues Dr. Kantor.
“Even if someone has no problem walking or feeling, they may have invisible symptoms that others don’t recognize or acknowledge.
“This can be very frustrating for the person with multiple sclerosis and they certainly wouldn’t call it ‘benign.’”
Symptoms of MS include: numbness or weakness in a leg or arm, usually beginning on one side of the body or both legs or both arms at the same time; vision problems (though rarely complete loss); pain; tremors and balance/gait problems; fatigue and dizziness.
When someone speaks of benign multiple sclerosis, perhaps they’re thinking in terms of mortality; MS rarely is fatal, and has been called the “best” nerve disease to have, since many other nerve diseases are terminal.

Dr. Kantor is also President Emeritus, Florida Society of Neurology.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Does Teen Obesity Cause Migraine Headaches?

Are you an overeight or obese teen who suffers with migraine headaches? Ever wonder if your size might be contributing to this painful condition?
If you’ve been struggling to manage your food portions or choices of food in an effort to lose weight, you now have an added incentive.
And that is this: Excess body fat is clearly associated with migraine headaches.
And as if that weren’t enough, teens who smoke and don’t get much exercise also happen to be more likely to get migraine headaches.
So how much, then, are teens more likely to have migraine headaches when compared to peers who are of a normal weight, exercise and don’t smoke?
They are 3.4 times more likely to have frequent headaches.
Three Variables
1) Overweight, 2) Lack of exercise, and 3) Smoking.
The study showed that in teens with all three of these variables, 55 percent had frequent headaches.
Of teenagers without these negative factors, 25 percent had frequent headaches.
Teens who were only overweight were 40 percent more apt to get frequent headaches than teens without the negative factors.
Smoking teens were 50 percent more likely to experience frequent migraines..
Teens who exercised fewer than two days per week were 20 percent more likely to get frequent headaches than those who exercised a minimum of twice weekly and who were not overweight nor smokers.
These study results come from interviews of 5,847 teens age 13 through 18, part of the Nord-Trøndelag Health Study in Nord-Trøndelag county in Norway.
Nurses interviewed the teens about headaches, exercise and smoking, and took weight and height measurements.
Obesity and Headaches
“Obesity is a risk factor for migraine headaches because of the link with adiponectin,” says Dr. Tiff Jumaily, MD, a board certified pediatrician with Integrative Pediatrics and Medicine.
“Adiponectin is a hormone released from fat cells which modulates inflammatory mediators in migraines.
“Adiponectin is protective against dyslipidemia, insulin resistance and atherosclerosis.
“It releases IL-10, an anti-inflammatory cytokine, and inhibits pro-inflammatory cytokines.
“Greater concentrations of fat cells will inhibit the release of adiponectin which can increase the risk for migraine.
“Paradoxically, a sudden increase in adiponectin levels can also trigger migraine.”
Basic Weight Loss Tips for Overweight Teens
Increasing your exercise is a lot easier than quitting an addiction to smoking or cutting back on your favorite foods, though exceptions do exist.
A smoker may find it easier to just quit smoking than to take up exercise.
Nevertheless, exercising more will inspire healthier eating habits and suppress the craving for a smoke. The result will be weight loss.
Don’t worry that quitting smoking will cause weight gain. If you exercise and eat less junk food and more healthy food, you should not gain fat.
Spend less time sitting before the TV and computer if you’re concerned that quitting smoking will put on weight or increase your appetite.
Remind yourself that giving up smoking can mean no longer suffering from so many migraines.
Teens should remind themselves that exercise might be just the very trick to end migraines…or at least cut down the frequency.
Tips on Exercise if You’re a Teen Who Needs to Lose a Lot of Weight
You should find an aerobic type of exercise that you can stick to. This can be walking, inline skating, using a stationary bike, going up and down a staircase, doing step drills on just the bottom step of a staircase, or following along to exercise videos.
Keep well-hydrated to prevent the so-called dehydration headache.
And add in extra activity every chance you can get. For instance, walk the dog more frequently, for longer distances and at a faster pace.
Ask your parents to buy you some exercise devices such as a heavy ball, a few pairs of dumbbells and/or a set of resistance bands. There’s a ton of very portable exercise equipment sold online.
Ask your parents to get you a gym membership. Then start picking up some weights, jogging around the track if there’s one, and taking some group fitness classes.
If you can’t join a gym, you can still do home exercises such as the ones depicted below.

Lunge. Do it in one spot as well as walking.

Squat. Go up and down up to 20 times.
Yoga. You can start off with beginner poses and hold them for up to a minute.
Additional exercises at home: marching in place, jogging in place, leg kicks and swings, jumping jacks, knee pushups.
Losing weight is not about feeling imperfect.
It’s about improving your health and fitness, as well as reducing your experiences with migraine headaches.
The full report is in the online Neurology (August 18, 2010).
 Dr. Jumaily is a board certified pediatrician and fellow of the American Academy of Pediatrics. She has a thriving pediatric practice in Los Angeles, where she integrates allopathic medicine with integrative and holistic options to treat the whole child and help them thrive.
Dr. Jumaily is a board certified pediatrician and fellow of the American Academy of Pediatrics. She has a thriving pediatric practice in Los Angeles, where she integrates allopathic medicine with integrative and holistic options to treat the whole child and help them thrive.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Depositphotos.com
Source: sciencedaily.com/releases/2010/08/100818161445.htm
Can Left Side Neglect Be Temporary?

Once a person develops left side neglect, will this usually be permanent or can it be a temporary condition?
Left side neglect is a fascinating neurological problem in which the patient lacks full awareness of his left side or part of the left side, as well as diminished awareness of inanimate objects that are leftward relative to wherever the person is in space at the moment.
My mother had left side neglect as a result of a chronic subdural hematoma on the right region of her brain that had resulted from hitting her head from a fall (in combination with being senior-aged and, most likely, the blood thinner she was on at the time).
Left neglect is more commonly the result of a stroke to the right area of the brain.
In the case of my mother, the problem was temporary.
But it had us unnerved when we realized the extent of it, after she was moved to a skilled nursing facility, a less-controlled, less-restricted environment than a hospital room where she spent just about all her time in bed.
If you clicked on this article, you already know what “left neglect” is, and most likely have been diagnosed with it, or know someone who has.
In the case of a stroke, left side neglect can be permanent, because a stroke is caused by oxygen depletion to brain cells, and once brain cells are starved long enough from oxygen, they cannot be brought back to life.
In my mother’s case, blood and cerebrospinal fluid were on the surface of her brain; the cells were still getting oxygen, but this fluid was creating a veil or fog over the cells, impairing neurological functioning.
As her body resorbed the fluid, the symptoms of the spatial neglect began disappearing.
The spatial neglect, at its worst, affected my mother’s ability to use a walker, maintain a linear walking path, and make turns without bumping the left side of the walker into baseboards.
Her left hand was orthopedically able to hold onto the walker, but it would keep slipping off because she lacked sufficient awareness of that side.
She’d end up trying to use the walker with one hand. But even when both hands were on it, she’d accidentally bump the walker into walls on the left side.
She was off the walker by evening; it was an impediment, actually, yet when she walked down the corridor, she had a tendency to veer to the right, and had no interest in anything to the left.
At the hospital in her room, seating for visitors was to her left, and often, she “ignored” me when I spoke to her when to her left, unless I raised my voice to call her name, and then she’d look at me as though suddenly hearing me.
I’d also get her attention by moving closer and more in front of her, though at the time, I didn’t know that this was the spatial neglect at work.
Currently, there is no sign of left side neglect in my mother, and the physical therapist who visited her home recently for an assessment, said that my mother didn’t need any home visits with a physical therapist, even.
Her left neglect did not disappear overnight, but there was a spike in improvement about 10 days after she was diagnosed with it.
When she came home from the nursing facility, she still had a tendency to drop things occasionally with the hand, but that problem soon disappeared.
At present, you’d never know that my mother once had a bizarre neurological phenomenon known as left neglect, also called spatial neglect.
In hindsight, I realize that left side neglect was at work prior to her second burr hole drain for the hematoma; at home she stated she wanted to lie on the futon in the dining room. From the kitchen this requires a left turn.
She exited the kitchen and began entering the living room, which is right. I had to physically steer her left into the dining room; classic left side neglect, fascinating phenomenon.
Left side neglect can be mild, moderate or severe. If you know someone with this condition, or have it yourself, there is hope, as there are multitudes of therapies to help overcome this condition.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: ncbi.nlm.nih.gov/pubmed/16408519
Top image: Shutterstock/Blue Planet Studio
Can Exercise Prevent Chronic Subdural Hematoma in Elderly?
Is it possible for exercise to prevent an elderly person from ever getting a chronic subdural hematoma?
“As we get older our brains shrink,” says Dr. David Beatty, MD, a retired general practitioner with 30+ years of experience and an instructor of general medicine for 20+ years.
“This happens to everyone, but happens quicker in some people than others.
“When the brain becomes smaller this leaves more space between the brain and the bones of the skull.
“This leads to stretching of the bridging veins and greater movement of the brain within the skull vault.
“To give an analogy. Think of a poorly packed box in the trunk of your car. The contents will rattle around more and be more likely to get damaged than if they were well-packed.
“Cerebral atrophy is not thought to be a reversible process, so it is crucial to prevent it where possible and to minimize its progression.”
Risk factors for chronic subdural hematoma include brain shrinkage (atrophy), old age, getting bumped in the head and daily use of blood thinners.
But one need not get bumped in the head, or be on blood thinners, to suffer a spontaneous chronic subdural hematoma.
The aging brain has a tendency to shrink, and so does the brain in people who never exercise.
An atrophied brain creates more space between the brain and the skull, which provides more room for a chronic subdural hematoma’s fluid to take up space – and hence create symptoms which require surgery to remedy.
To keep the brain healthy, Dr. Beatty recommends healthy lifestyle choices to reduce the risk of ailments that lead to brain atrophy.
These include avoiding smoking, minimizing alcohol intake, avoiding high blood pressure, and taking measures to prevent or remedy obesity.
“Exercise is another weapon in the fight to prevent cerebral atrophy,” says Dr. Beatty.
“It’s been shown that exercise increases blood circulation to the brain and slows the rate of cerebral atrophy.
“I think exercise may well have another benefit with regard to subdural hematoma prevention.
“Someone who is physically fitter is less likely to have the falls that cause the head injury which causes the subdural.”
Exercise and Brain Shrinkage

It’s been well-established that exercise prevents brain shrinkage in animal studies, and even human studies have demonstrated this.
There is a study that shows that moderate exercise over one year can increase the size of the hippocampus of the brain in older people.
This study, however, didn’t look at chronic subdural hematoma; it looked at spatial memory.
But the fact remains that exercise increased brain size, albeit only a particular portion of the brain.
The hippocampus study was carried out by researchers at the University of Illinois, University of Pittsburgh, Ohio State University and Rice University, and focused on older people who already had hippocampus shrinkage (atrophy).
The hippocampus is responsible for memory.
The study involved 120 inactive older subjects who did not have dementia.
They were placed in two groups: One group walked for exercise (40 minutes daily, 3x/week), and the other group simply did toning and stretching exercises.
Prior to the study, MRIs were taken of the subjects’ brains. MRIs were then taken six months into the study, and at the end of one year.
The group who exercised had a volume increase of the right and left hippocampus.
And get this: In the second group, the hippocampus decreased in volume! I.e., lack of exercise = brain shrinkage.
Another study showed that exercise increases the number of small blood vessels in the brain. (Radiological Society of North America [Dec. 2, 2008]; “Exercise Helps Prevent Age-related Brain Changes In Older Adults”)
If a brain has more small blood vessels, perhaps this can have a protective effect against a slow brain bleed, though there have been no studies specifically investigating this.
The bottom line, though, is that exercise is crucial for optimal brain function and integrity, and these benefits will extend into old age.
 Dr. Beatty has worked in primary medicine, surgery, accident and emergency, OBGYN, pediatrics and chronic disease management. He is the Doctor of Medicine for Strong Home Gym.
Dr. Beatty has worked in primary medicine, surgery, accident and emergency, OBGYN, pediatrics and chronic disease management. He is the Doctor of Medicine for Strong Home Gym.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Source: sciencedaily.com/releases/2011/01/110131153249.htm
Top image: Freepik
What If a Patient Pulls Burr Hole Brain Drain Tube Out?

After a burr hole craniostomy for chronic subdural hematoma, a “drain” tube is left in the patient’s skull. This was the case of my mother.
She had a chronic subdural hematoma, and the drain tube that was placed in her head, after her second surgery, accidentally came out after she was shifting in her bed while propped up, and – according to her report – sat on the short tube, causing it to get tugged.
She immediately reported this to the staff via her nurse call button. If you clicked on this article, I needn’t explain to you what the burr hole drain looks like as it feeds into the patient’s head.
In the case of my mother, all that was there were small bandages, but the tube, as it entered the shaved portion of her head, was visible.
Will blood and cerebrospinal fluid spurt all over the place if the tube is pulled out (or comes out by accident, at least)? Not in the case of my mother.
I wouldn’t think any spurting would occur unless the burr hole tube came out the same day of the surgery.
In the case of my mother, it was tugged out on Friday; she had had the surgery two days prior on Wednesday. So by then, there wasn’t heavy draining.
I saw spots of a mixture of blood and cerebrospinal fluid here and there on the bed sheets, but nothing messy or alarming.
The burr hole is already draining in these cases, so if the tube comes out prematurely, of course the draining is going to continue.
But instead of the fluid draining into the tube, it will be “leaking” onto the scalp and will need someplace to go.
In this case, the fluid went onto the gauze that the nurse was sturdily applying to my mother’s scalp … after she paged the neurosurgeon for instructions.
Do not try to place the tube back in the burr hole! When the tube comes out, it immediately becomes contaminated! Instead, call the nurse if the patient already didn’t. Do not touch the hole.
When the nurse was applying compression, it was painful. Don’t panic if the nurse says that “brain juice” is coming out.
“Juice” means cerebrospinal fluid, possibly mixed with blood – which you already know is the objective of the draining in the first place when someone has chronic subdural hematoma.
You actually want this “juice” to continue to come out, because its collection in the brain is why the patient ended up having surgery in the first place.
As I watched the nurse maintain her compression on the burr hole, I asked how they were going to control the leaking.
She mentioned something about applying Vaseline which would create a barrier. Do we really want that, I asked, because the whole idea is to get the fluid out of the brain, not trap it in there with a barrier.
The nurse acknowledged my point, and then the neurosurgeon got back to her.
The final verdict was to wrap my mother’s head several times with a special wrapping, then have her lie on her side (the burr hole side against the pillow) as much as possible, so that gravity would allow continued draining.
A collection sheet was placed between her head and the pillow in case any fluid seeped through.
Why weren’t plans made to put in a new drain? This would require a sterile environment, i.e., another surgery in the OR, and also, the surgeon wasn’t available.
When my mother’s burr hole drain came out, it wasn’t an emergency situation. Again, the fluid is supposed to drain out anyways.
Next morning the bandages were removed and I was told that there had been minimal leaking, and the bandages remained off. Sutures were put in place.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Natalie Board
Antidepressant Losing Steam and Pooping Out? Solution

An antidepressant may work wonders initially but then may lose its punch and can’t keep up with the depression.
You may be on an antidepressant that’s been working wonderfully…
But then soon after you go on the prescription drug, it begins losing its full effect. It has pooped out: the “poop-out effect.”
The antidepressant that my mother was on for clinical depression seemed to start pooping out less than two weeks after starting it.
The drug was Cymbalta and the prescription called for 30 mg the first week, then 60 mg the second week.
Oddly, the doctor prescribed only 30 capsules with no refill authorization.
I consulted with my brother, who had been working in the pharmaceutical industry as a chemist for many years.
When an antidepressant poops out, this means it has lost its fire or power when it comes to subduing depression symptoms.
This doesn’t mean it’s lost all of its effect, but enough to cause concern in the patient and/or family members. The regression in my mother was noticeable.
With my mother, the poop-out effect took place on day 13 and day 14 of being on Cymbalta.
I assumed that she’d have to go up to 90 mg so that the drug could resume its full effectiveness.
I also wondered if her doctor would switch to a different drug, or, keep her on Cymbalta but add a second drug.
In the case of my mother, it turned out that the antidepressant hadn’t pooped out at all.
On day 15 she did great, and the next day we were in the doctor’s office.
The doctor explained that it takes a while for antidepressant drugs to take full effect.
Some days will be better than others, but as long as the overall picture looks good, then the drug is working.
On day 12, in the evening, my mother received some alarming news about a family member — a divorce, and I surmise that the shock had not sunk in that evening — until she went to bed.
Next morning she reported she hardly slept, having been kept awake thinking about the family member.
The second half of next day, my mother had what appeared to be the beginnings of a relapse into the depression. This repeated next day, and was worse.
But the day after, she was hopping. And I figured that the relapse had to have been related to news of the divorce.
Though my mother had setbacks, the drug was still working because without the antidepressant, she would have been debilitated, weeping and hardly eating.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Atrial Fibrillation, Elevated Troponin: How Much Heart Damage?
Can enough atrial fibrillation episodes, over time in someone with heart disease, cause cardiac damage that’s equal to a heart attack?
“Generally, A-fib does not result in significant heart damage,” says Dr. Simon Dixon, chairman of cardiovascular medicine for Beaumont Health System in Michigan.
You may already know that the higher the troponin level, the more damage that’s been done to the heart. The higher the troponin elevation, the worse the long-term prognosis is.
Over a certain level means a heart attack. Under that cut-off point, the result is deemed “indeterminate” or a “grey area.”
I wondered if a lot of “indeterminate” elevations of troponin, from atrial fibrillation in a patient with heart disease, would, over time, “equal” a heart attack.
So for example, suppose the elevations range from 0.11 to 0.30 – many of these over an extended period of time from episodes of A-fib that occur between sporadically and frequently.
Wouldn’t eventually all of these fractions “add up” to a heart attack?
Dr. Dixon explains, “Some patients have chronic low levels of troponin elevation (for example, 0.14 ng/mL).
“This can be ‘normal’ in some patients, or associated with disorders such as heart failure and kidney failure.
“This level of troponin elevation does not necessarily cause the same level of damage as a heart attack.”

Dr. Dixon specializes in the treatment of acute and chronic coronary artery disease, with research focusing on pioneering treatments to save heart muscle in patients having heart attacks.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/megaflopp
Why Can A-Fib with Heart Disease Cause Troponin Elevation?

There’s a specific reason why an episode of atrial fibrillation can elevate troponin levels if you already have heart disease.
Troponin is a protein enzyme that leaks from heart muscle when that muscle sustains damage, such as from a heart attack or blunt chest trauma.
But an episode of atrial fibrillation — an abnormal heart rhythm – -can also cause a leak of troponin, which of course, means that some damage to the cardiac tissue has occurred—but not nearly as much as would occur from a heart attack.
In a person whose only condition is A-fib, an episode of this cardiac arrhythmia won’t cause a rise in troponin.
But if someone has severe coronary artery disease, it can. In severe coronary artery disease (or “heart disease”), the arteries that supply blood to the heart are at least 70 percent blocked with plaque.
This leaves a small diameter through which blood gets through, and can cause symptoms, usually shortness of breath with only mild exertion, and/or chest pain.
Atrial Fibrillation + Heart Disease = Rise in Troponin
“Patients with coronary artery disease are more likely to have a troponin elevation because the blockage in the artery limits the ability of the heart to increase blood flow to the muscle during the AF episode,” says Dr. Simon Dixon, chairman of cardiovascular medicine for Beaumont Health System in Michigan.
When a patient’s troponin test result is elevated, another one should be taken several hours later to see if the numerical result is higher.
The test may be repeated a few more times to see when the number stops rising and starts coming down.
If the patient has not exhibited any sign of a heart attack, such as chest pain or pressure, clammy skin, nausea, jaw or arm pain, or shortness of breath, but they have atrial fibrillation, then the reason for the elevated troponin will not likely be that of a heart attack.

Dr. Dixon specializes in the treatment of acute and chronic coronary artery disease, with research focusing on pioneering treatments to save heart muscle in patients having heart attacks.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/designer491
Does Every Episode of Atrial Fibrillation Damage the Heart?
In someone with coronary artery disease, does every episode of atrial fibrillation mean damage to the heart?
Damage to cardiac tissue can result from an episode of atrial fibrillation in a person with coronary artery disease.
Not all people with CAD experience A-fib, and not all people who have periods of atrial fibrillation have coronary heart disease.
Arial fibrillation is a rhythm disorder that increases the risk of blood clots that can lead to a heart attack or stroke.
In fact, A-fib is a major risk factor for a massive stroke, which could be fatal.
This arrhythmia is characterized by a sudden increase in heart rate — but it’s not a steady rate. It jumps all over the place.
This erratic beat can be felt in the pulse with fingers to the wrist.
The numbers on a heart rate screen will be jumping all over the place.
Atrial fibrillation and coronary artery disease can exist in the same patient, and there are times when an event of atrial fibrillation results in a mild elevation of troponin, the protein enzyme that leaks from the heart muscle—indicating that damage was sustained.
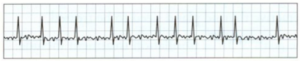
An EKG showing A-fib
Does every incidence of A-fib in someone with coronary artery disease necessarily damage the heart?
“Most episodes of AF do not cause the troponin to be elevated,” says Dr. Simon Dixon, chairman of cardiovascular medicine for Beaumont Health System in Michigan.
“This depends a lot on the heart rate during episodes as well as other factors such as blood count and the extent of coronary disease.”
Thus, if someone with heart disease has several A-fib episodes per week, this does not necessarily mean that the patient’s heart gets damaged (as revealed by elevated troponin) every time.
“Atrial fibrillation can occur in episodes (paroxysms) or be present all the time (permanent),” says Dr. Dixon.
“Most patients with AF do not sustain muscle damage unless the heart rate becomes quite uncontrolled, or there are other medical factors such as fever, low blood oxygen level or low blood count.”

Dr. Dixon specializes in the treatment of acute and chronic coronary artery disease, with research focusing on pioneering treatments to save heart muscle in patients having heart attacks.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/TippaPatt
What’s the Elevated Troponin Range from A-Fib Episodes?

An episode of atrial fibrillation can elevate troponin, but what would be the typical range of this elevation?
Atrial fibrillation (A-fib) is a serious heart rhythm disorder that can have significant consequences if left untreated.
While some patients may not experience symptoms, A-fib poses a major risk due to the potential for blood pooling in the heart.
This stagnation increases the risk of ischemic stroke, particularly in individuals over 65 and those with additional stroke risk factors, such as a family history or smoking.
Additionally, A-fib can lead to elevated levels of troponin, an enzyme released by the heart when the cardiac muscle is damaged.
Elevated troponin levels indicate that the heart is under stress or experiencing damage, further complicating the management of A-fib and its associated risks.
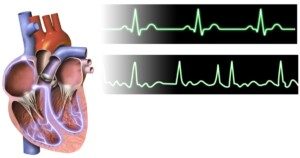
Atrial fibrillation. BruceBlaus
“Some patients with atrial fibrillation develop a fast heart rate (rapid ventricular rate) in the setting of infection, bleeding or other medical conditions,” says Dr. Simon Dixon, chairman of cardiovascular medicine for Beaumont Health System in Michigan.
One such medical condition is coronary artery disease: buildup of fatty deposits inside the arteries.
These arteries supply blood to the heart muscle, and when plaques accumulate, they narrow and harden the arteries, reducing blood flow.
When an episode of A-fib occurs, says Dr. Dixon, “the heart muscle needs greater blood supply to provide oxygen and glucose [blood sugar].
“At times, however, the ‘demand’ outstrips the ‘supply,’ resulting in damage to the muscle (especially on the inside wall of the heart, or subendocardial layer).
“Generally the troponin elevation in these cases is small, for example, 0.1-2.0 ng/mL (the upper limit for the normal range of troponin in our hospital is 0.06 ng/mL).”
This troponin range is called “indeterminate,” because it can have numerous causes other than an episode of atrial fibrillation, but this range isn’t high enough to arouse the suspicion for a heart attack.
Troponin elevation of unknown origin is far more common in elderly people, but should always be followed up.
Age of Patient with Elevated Troponin
The younger a person is, the more significant an elevated result is.
In the younger adult population, elevated troponin levels are less likely to be attributed to age-related conditions and more likely to indicate acute or significant cardiac issues, such as a heart attack or severe heart inflammation.
In contrast, older adults may have elevated troponin levels due to chronic conditions or age-related changes in heart function that are less immediately alarming.
Therefore, in younger adults, an elevated troponin level typically means a more urgent investigation to find out what the cause is.

Dr. Dixon specializes in the treatment of acute and chronic coronary artery disease, with his research focusing on pioneering treatments to save heart muscle in patients who are having heart attacks.
 Lorra Garrick has been covering medical, fitness and cyber security topics for many years, having written thousands of articles for print magazines and websites, and this includes as a ghostwriter. She is also a former ACE certified personal trainer.
Lorra Garrick has been covering medical, fitness and cyber security topics for many years, having written thousands of articles for print magazines and websites, and this includes as a ghostwriter. She is also a former ACE certified personal trainer.
.