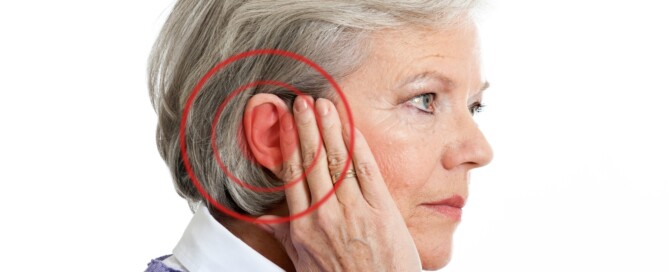
Can Tinnitus Be Higher Tone than What You Can Hear for Real?
Can a person hear a tinnitus (sine wave tone) at a higher frequency than what he can hear in real life?
So let’s look at it this way: Suppose a hearing test determines that you can only hear at 11,000 Hz, but the tinnitus that rings in your ears against your will matches a tone of 13,000. (more…)
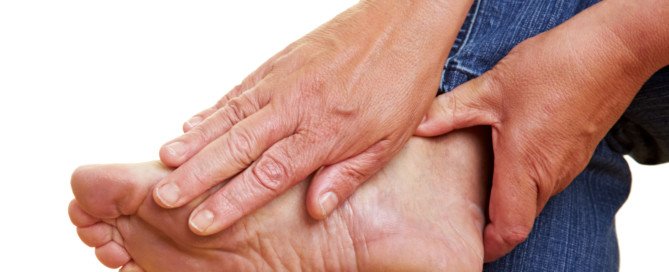
A Slightly Numb Big Toe Can Be Caused by Diabetic Neuropathy
You may have diabetes and the numb feeling in your big toe can be caused by diabetes, but it may also have other causes unrelated to blood sugar levels.
Neuropathy has causes other than diabetes, even though you may have seen ads for diabetic neuropathy. (more…)
Ears Get Cold Outside Jogging even in Warm Weather?
Do your ears always get cold outside even in 75 degree weather, especially if you’re hiking, jogging or even walking?
For some people, wearing a cap of some sort to keep the ears warm is necessary, even in what would be considered warm weather. (more…)
Conquer that Mad Racing Heart Every Time You Use a Staircase

So your heart pounds like a demon every time you walk up a flight of stairs?
First of all, make sure that a cardiologist finds nothing wrong with your heart.
The doctor must clear you for a form of exercise called interval training, because this will likely cure you of that frightening racing heart that occurs every time you go up a flight of stairs. (more…)
Can More Frequent Urination Be a Symptom of Perimenopause ?

You aren’t imagining it: There may very well be a link between perimenopause and more frequent urinating than usual, including those overnight trips to the bathroom.
How many voids per 24 hours define urinary frequency?
“Although there is no absolute number of daytime voids that is ‘abnormal,’ urinary frequency is typically defined as more than eight voids/24 hours,” says R. Mark Ellerkmann, MD, Director, The Urogynecology Center at Mercy Medical Center, Baltimore.
“However, many things can influence the degree of urinary frequency — how much one drinks, what one drinks, whether someone is on a diuretic, etc.”
So right off the bat, you may want to ask yourself if perimenopause has been making you consume more fluids, though thirst is not a symptom of perimenopause.

Overactive Bladder
Dr. Ellerkmann says that usually, complaints of urinary frequency come with additional symptoms:
• Urinary urgency (“sudden, compelling desire to pass urine which is difficult to defer”)
• Nocturia – getting up in the middle of the night to relieve oneself more than once
• Urge related
“The constellation of these symptoms provide for a clinical diagnosis we refer to as overactive bladder or OAB (defined as urgency, often with frequency and nocturia, with or without urge related urinary incontinence),” explains Dr. Ellerkmann.
Severity does increase with age, but perimenopause typically occurs in a woman’s 40s. Urge related incontinence is more common in women.
“Urge incontinence increases with age, from 17 percent of women older than 45 years to 27 percent of women older than 75 years of age.”
The Perimenopause and Urinary Frequency Connection
“Perimenopause is defined at that period of time leading up to menopause,” says Dr. Ellerkmann.
“Many physiological changes occur during the perimenopausal time period as levels of circulating hormones — estrogen, progesterone and testosterone — fluctuate and levels slowly decrease.
“The effects of estrogen on the urogenital tract are well-known, as these tissues (the vaginal and peri-urethral tissues/bladder) are very rich in estrogen receptors.
“As circulating estrogen levels decrease and become less consistent, vaginal and peri-urethral tissues become less well-lubricated; they become thinner and less elastic and less well-vascularized [stocked with blood vessels].
“It may be that the loss of estrogen can adversely affect the bladder, but whether the hormonal changes of perimenopause are directly related to symptoms of urinary frequency is difficult to say.”
Solutions to Increased Urinary Frequency from Perimenopause
Dr. Ellerkmann says that some studies support the use of supplemental vaginal estrogen cream in both periomenopausal and menopausal women to partially alleviate symptoms of overactive bladder.
Dr. Ellerkmann also explains, “Excluding organic causes that might cause overactive bladder symptoms (bladder cancers, stones, bladder prolapse, infections, foreign suture or mesh from urological surgery) or medications (diuretics) or behavior (excessive consumption of liquids), the most common inciting causes of urinary frequency and urgency are consumption of known dietary irritants — the most common of which are caffeinated beverages, tea, artificial sweeteners, carbonated beverages, citrus juices, tomatoes, chocolate, sodas.”
Dr. Ellerkmann is board certified in both OB/GYN and female pelvic medicine and reconstructive surgery. He specializes in the treatment of urinary incontinence in women of all ages.
is board certified in both OB/GYN and female pelvic medicine and reconstructive surgery. He specializes in the treatment of urinary incontinence in women of all ages.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Feel Like You Must Pee Really Bad after a Pap Smear ?

Did your Pap smear make your bladder feel full enough to burst, like you had to pee a whole gallon?
So after the doctor is finished with the Pap smear, having removed the speculum and completed the digital exam, you’re left lying immobile because it feels that your bladder is suddenly filled to the hilt with urine.
But you know there can’t be any urine in there because:
• You relieved yourself right before the exam.
• You didn’t even have a drop of water prior to the exam.
• The preceding day you went light on the water.
You induced dehydration to lessen any bladder discomfort from a Pap smear, but this time, the urge to pee was overwhelming. What could cause this?
“The only comment I would have on this question is that (depending on the examiner and the patient) a pelvic examination (speculum placement, bimanual examination) can possibly irritate the vaginal tissues and may cause a patient to have transient overactive bladder symptoms,” says R. Mark Ellerkmann, MD, Director, The Urogynecology Center at Mercy Medical Center, Baltimore.
The severe urge to pee after a Pap smear has nothing to do with the actual buildup of urine in the bladder.
#1 Urine comes from the kidneys.
#2 A Pap smear cannot magically make urine fill up the bladder.
#3 It’s only an illusion.
The vagina is also very close to the urethra, so any handling of the vagina could irritate the urethra, simulating an urge to void.
And all of this is what you must remind yourself for your next Pap smear, especially when it’s completed and you’re lying there very still, feeling as though at any moment you’re going to leak.
Give this sensation five or so minutes to pass. Just lie there and breathe deeply, eyes closed. Tell your doctor why you want to just lie there, then do it.
Dr. Ellerkmann adds, “It is highly unlikely that a pelvic examination increases the risk of a urinary tract infection — often responsible for transient OAB symptoms — or any trauma to the pelvic floor.
“It is just that pressing and palpating (feeling) the bladder and uterus can cause a sensation of ‘needing’ to go.”
Dr. Ellerkmann is board certified in both OB/GYN and female pelvic medicine and reconstructive surgery. He specializes in the treatment of urinary incontinence in women of all ages.
is board certified in both OB/GYN and female pelvic medicine and reconstructive surgery. He specializes in the treatment of urinary incontinence in women of all ages.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Here’s Why It’s Hard for Type 1 Diabetics to Get Pregnant
The high blood sugar of type 1 diabetes doesn’t interfere with GETTING pregnant, but instead causes another problem once a woman IS pregnant. (more…)
Why Does Diabetes Cause Shiny Skin on the Lower Legs?

“This condition is known as diabetic dermopathy, characterized by thinning, shiny, friable skin due to microvascular changes in the small blood vessels in the skin,” says Jenepher Piper, a family practice nurse practitioner for Maryland Family Care for 25+ years and a former nurse with Home Care Nurse for Johns Hopkins Home Care.
“This is similar to the changes that occur to the retina of the eye (diabetic retinopathy).”
It is unknown what the underlying mechanism is of diabetes dermopathy, according to a report by the British Journal of Diabetes.
Despite the appearance, with can be mottled and include shiny sections, this condition does not cause symptoms.
The skin lesions do not require treatment.
If you notice what seems to be this condition on your legs, even if it doesn’t appear to be shiny, and your last checkup did not show diabetes or you were not tested for it, you should get retested!
Patients suffering from conditions such as coronary artery disease, obesity and diabetes turn to Nurse Practitioner Piper to help them best manage their overall health.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Source: bjd-abcd.com/index.php/bjd/article/viewFile/24/63
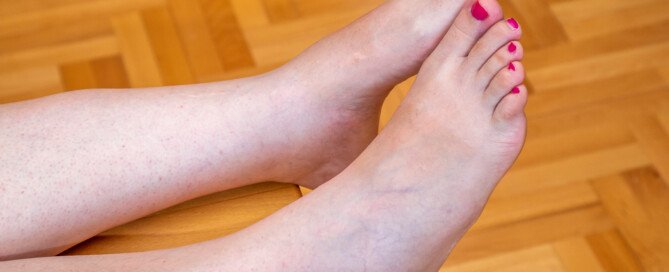
When Those Scary Sock Indentations Don’t Mean Edema

Discovering you may have edema, thanks to worrisome indentations in your skin caused by socks, is pretty unnerving.
That’s because edema can be caused by problems with the heart or kidneys. (more…)
Just What IS “Cloudy” Urine? Its Appearance and Color

The term “cloudy urine” comes up often on medical sites, but there’s no description of just what this is.
It’s open to subjective interpretation. To some people it can mean a milky colored urine.
To others it may bring to mind a cloudy color, kind of grey-like.
And to other people it can mean a murky quality to their light orange urine – the orange being from dehydration.
“Cloudy” is an overly broad term.
“Cloudy urine refers to urine that is not clear but uniformly opaque, like a cloud,” says Jenepher Piper, a family practice nurse practitioner for Maryland Family Care for 25+ years and a former nurse with Home Care Nurse for Johns Hopkins Home Care.
You may still be able to see through this type of excrement if it’s in a clear plastic cup.
It may also be cloudy enough or solid-looking enough that you would not be able to see your finger on the other side of the plastic cup.
“Cloudy urine doesn’t imply any change from typical urine color, light to dark yellow,” says Piper.
In other words, the murkiness can be present in any color on the urine spectrum, from clear/pale yellow to medium yellow to dark yellow to yellow-orange to light orange to orange (these colors are determined by hydration levels).
Urologic Oncologist’s Description of Cloudy Urine
“‘Cloudy’ urine can describe a wide variety of urine,” says Michael Herman, MD, director of urologic oncology at South Nassau Communities Hospital in Oceanside, NY.
“It can range from urine that is just slightly translucent to flakes of sediment in the urine to urine that looks almost milky it is so cloudy.”
There are many causes of the so-called cloudy urine, and some of the non-cancerous causes can still be serious.
Patients suffering from conditions such as coronary artery disease, obesity and diabetes turn to Nurse Practitioner Piper to help them best manage their overall health.
Dr. Herman’s interests include reducing the over-diagnosis and over-treatment of prostate cancer by utilizing the latest biomarkers and imaging techniques. He is at the forefront of treatment and research of urologic cancers.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.