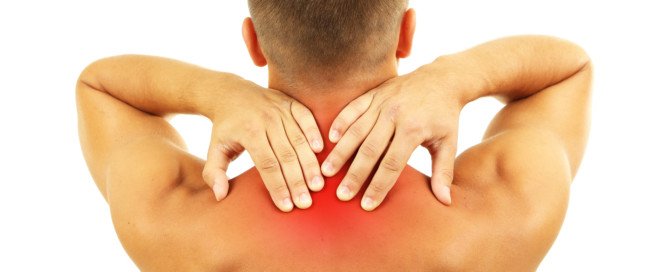
What’s It Mean When Collarbone Pain Comes from the Neck?
So your pain is in the collarbone or clavicle area, but it seems to be originating from your neck.
This doesn’t sound good, and it warrants a medical evaluation.
“Shoulder blade pain is most commonly indicative of a cervical problem, usually degenerative disc disease, sometimes spinal stenosis, or radiculopathy, which is more commonly known as a pinched nerve,” says Dr. Mark Galland, orthopedic surgeon, sports medicine specialist and physician at Orthopaedic Specialists of North Carolina.
“Cervical” refers to the neck area (cervical vertebrae). In degenerative disc disease, the spongy-like, shock-absorbing discs in between each vertebra are worn down.
Spinal stenosis is narrowing of the canal through which the spinal cord runs. Both situations can put pressure on nerves that come off the spinal cord.
Pain, tingling, numbness and weakness are all symptoms that can result.
Radiculopathy is when the pain, caused by nerve compression or pinching, radiates away from the source of the pinching.
So for a very common example, the pinching or compression of the nerve may be occurring in the low back (lumbar area), but the pain may be radiating down the leg.
Nerve compression in the neck area, likewise, can generate pain in the clavicle or shoulder region.
“Treatment options for this kind of pain include rest, physical therapy, a brief course of anti-inflammatory medication and a self-directed home exercise program,” says Dr. Galland.
It’s very crucial to stick with the physical therapy and home exercises.
“More significant pathology can be treated with a specialized injection called an ESI,” says Dr. Galland.
So if you have shoulder blade pain that seems to come from your neck, you should see an orthopedic specialist or sports medicine doctor.
ESI stands an epidural steroid injection, which often eliminates pain for up to three or four months.
Dr. Galland has authored many book chapters and papers in sports medicine. His advice and consultation have been sought by world-class athletes in track and field and Major League Baseball.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health.
.
Top image: Shutterstock/Africa Studio
Collar Bone Shoulder Pain but Full Range of Motion?
What can cause pain around the collar bone of your shoulder if the bone is not broken and you have full range of motion?
There are several possible causes of this situation.
“Nagging aches or pains around the collar bone may be caused by osteoarthritis of the acromioclavicular joint, also known as the AC joint; or the sternoclavicular joint, or the SC joint,” says Dr. Mark Galland, orthopedic surgeon, sports medicine specialist and physician at Orthopaedic Specialists of North Carolina.
The acromioclavicular joint is a key joint located where the acromion — a part of the shoulder blade (scapula) — meets the clavicle (collarbone).
It allows the shoulder to move and maintain stability. Movements include raising the arm, reaching overhead and rotating the shoulder.
What is osteoarthritis?
Osteoarthritis is a degenerative joint disease characterized by the gradual wearing down of cartilage between bones.
Cartilage is a smooth, flexible tissue that acts as a cushion and provides shock absorption between bones, allowing for smooth and pain-free joint movement.
In osteoarthritis, this cushioning layer deteriorates over time, leading to increased friction between the bones.
As the cartilage thins and wears away, bones may come into direct contact with each other, resulting in pain, swelling and decreased joint flexibility.
The reduction in cartilage reduces the joint’s ability to absorb shocks, which can exacerbate discomfort and contribute to further joint damage.
This condition can impact any joint — including the shoulder.
OA happens commonly to the knees, which is why people get knee replacement surgery.
It also occurs fairly commonly to the hip joint, necessitating hip replacement surgery.
However, shoulder replacement surgery is much less common because conservative treatments have a higher success rate than they do with OA of the knee or hip.
But if the osteoarthritis is bad enough (such as a bone-on-bone situation), and depending on the patient’s condition and medical history, an artificial shoulder joint may be an option.
If you are experiencing shoulder pain that won’t go away, yet you still have a full range of motion, you should make an appointment with a physician whose specialties include the shoulder joint.
Many things can lead to persistent shoulder pain.
If the pain is worse when you move the joint in certain positions, or when you try to lift a weight over your head, this indicates a strong possibility of a musculoskeletal origin that does not involve a wearing down of the cartilage.
The collar bone may or may not be involved when the problem is musculoskeletal in origin.
If the rotator cuff is involved, there will NOT be full range of motion without pain.
Dr. Galland has authored many book chapters and papers in sports medicine. His advice and consultation have been sought by world-class athletes in track and field and Major League Baseball.
 Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health. Her writing focuses on fitness, health and medicine.
Lorra Garrick is a former personal trainer certified by the American Council on Exercise. At Bally Total Fitness she trained clients of all ages for fat loss, muscle building, fitness and improved health. Her writing focuses on fitness, health and medicine.
Old Cat Keeps Vomiting? 4 Causes, Solutions

An old cat can vomit for several reasons, some benign and some serious.
Cause #1 of an old cat vomiting
One cause can be diet, says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
An aging cat is less efficient at digesting foods that previously gave it no trouble.
“Your cat may have thrived on an inexpensive store-brand food for years, but poor quality proteins can get harder for older pets to break down,” says Dr. Benson.
The solution is a high-quality “senior pet” or “sensitive stomach” formula.
Aside from aging, older cats may develop allergies to certain food proteins, though this problem is more common in younger felines.
Switching your older cat over to a fish, lamb or a venison based diet may help alleviate vomiting.
Cause #2 of an old cat vomiting
Hairballs. An older can may lose more fur, meaning, more hairballs. “Using a hairball-specific diet or supplementing your cat’s diet with a lubricant like Laxitone (available from your veterinarian) can help ease hair through the GI tract,” says Dr. Benson.
What would be preferable, though, is to regularly brush your old cat with a special tool that helps remove the undercoat, like the Furminator (at pet stores).
Cause #3 of an old cat vomiting
Disease, and many, can cause this issue. Dr. Benson lists the following: cancer, GI ulceration, poisoning, ingestion of a foreign body, thyroid disease, kidney disease, pancreatitis and parasites.
And, just like in some people, stress can cause vomiting. A cat can be stressed enough to get sick.
“Your veterinarian will likely recommend a basic set of tests, including blood work, urinalysis (yes, even if your pet is urinating normally!), fecal testing and radiographs (X-rays), and may recommend additional tests like ultrasonography, GI-specific blood panels, endoscopy and/or biopsies,” explains Dr. Benson.
Cause #4 of an old cat vomiting
Feeding/eating patterns. Dr. Benson explains that cats that are “portion-fed at regular intervals may anticipate mealtimes and produce large amounts of gastric acid, which can cause them to throw up prior to food, or just after.”
If a cat gobbles up food, this too can cause it to upchuck. If you notice this pattern, try feeding your pet very small amounts of food when they “start to get vocal about mealtimes,” says Dr. Benson. Break their meal up into smaller portions.
“Overproduction of gastric acid can also be helped with some medications; your veterinarian will be able to help.”
If your older cat has been vomiting, don’t delay a vet visit by first trying home treatments; see the doctor promptly to rule out serious causes as soon as possible.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Gum Color Guide for Cat Owners

Here is a veterinarian’s guide for gum color in cats.
The color of a cat’s gums can tell a lot about your pet’s health.
Ideal Cat Gum Color
“When it comes to your cat’s gums, the key is to think pink!” begins Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
“A healthy cat’s gums are pink, neither too red nor too dull.”
However, a cat may have been born with black gums. In that case, says Dr. Benson, black gums would be this cat’s normal color.
If you have a kitten or are planning on getting a kitten, take good notice of the gum color.
In fact, take a few photos. You should know what the normal color usually is. If you have a cat and not a kitten, take a few photos anyways.
Knowing what the color normally is will assist you in spotting any changes that might mean a medical problem.
Cat Gum Color Guide
Dr. Benson explains: “Bright pink or red gums can be a sign of toxicity or dental disease; yellowish gums could point to problems with the liver.
“If your cat’s gums are looking blue, purple, gray, or whitish, this is an indication that blood is not circulating well in the peripheral circulation, which could be for a number of reasons, including cardiac disease, cancer, metabolic disease (kidney, liver disease), poisoning, shock and many others.”

Summary: A cat’s gums can be the following colors: regular pink, black, bright pink, red, yellowish, blue, purple, gray and whitish. That’s quite a spectrum.
CRT Test
A veterinarian may perform a test called a capillary refill time, says Dr. Benson. The veterinarian presses on an area of the gum.
It momentarily turns a light pink or white while the blood is pushed out of the tissue.
The vet then counts to see how long it takes for the normal color to return. A normal capillary refill time is less than two seconds.
Takeaway
If you notice changes, see your veterinarian immediately.
“Because cats are very good at hiding obvious behaviors associated with disease, looking at things like gum color regularly can be a great way to check circulatory health,” says Dr. Benson.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Declawing Cat: Is Licking Paws Okay After Procedure?
A veterinarian discusses declawing your cat and your pet licking the paws afterwards.
You’ve had your cat declawed and are now noticing that your pet keeps licking its paws.
Should you allow this? Is it okay?
“No – most veterinary clinics will keep cats for observation for two to four days after a declawing procedure, to ensure that the cat is comfortable and not licking her paws,” says veterinarian Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
What’s wrong with a declawed cat licking its paws?
“Licking can introduce infection and open the surgical wounds where the claws were removed,” says Dr. Benson.
“Declawed cats require close observation, and most vets will send your pet home with special litter for at least the first week or two, so that small particles don’t get stuck in the wounds and delay the healing process.
“If you do notice licking once you bring your cat home, talk to your vet for tips on safe prevention.”
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Cat’s Paw Has Pinkish Red Growth: Cancer Possible

A veterinarian discusses cancer as a possible cause of a pinkish red growth in a cat’s paw.
Not all sinister growths on a cat are black or otherwise dark.
There is reason to beware of anything pink or reddish growing on your cat’s paw.
What can possibly cause a pink or reddish growth in a cat’s paw?
“Dermatological disease in cats is much less common than in dogs, but often tends to be more serious,” says Dr. Jules Benson, BVSc, chief veterinary officer with NationwideDVM, a pet insurer company.
“Skin growths are always suspicious for cancerous conditions like fibrosarcoma, or an autoimmune condition like eosinophilic granuloma complex (EGC).
“Your veterinarian will be able to take a biopsy (often just using a needle, initially), and the results of the biopsy will inform their opinion as to appropriate treatment options.”
Cell Pathology
“In some cases, isolated masses can be surgically removed with no further problems,” continues Dr. Benson.
“But the outcome very much depends on the type of cells that make up the mass and how the cells appear to be behaving.
“More aggressive cancers may have lots of forms of the same cell type, indicating rapid growth and activity, while cells that all look the same may indicate a more local and treatable form of disease).”
Two Other Cancers that Can Present As a Pink or Red Growth Involving a Cat’s Paw
- Squamous cell carcinoma. Older cats are usually affected by this sun-exposure-related tumor that may show as a reddish patch of skin covered with a scab in the early stages.
- Mast cell tumor. This is not usually aggressive.
A pink or red growth on a cat’s paw doesn’t always mean cancer.
- Eosinophilic plagues. These raised growths may appear “raw.”
- Indolent ulcer. These are pink and look like sores.
- Basal cell tumor. This small firm mass most often affects Persian, Siamese and Himalayan cats.
- Sebaceous adenoma. This resembles a wart.
If you notice any new pink or red growth on your cat’s paw or anywhere else, don’t hesitate to make an appointment with the vet.
 Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
Dr. Benson is regularly consulted by many media outlets including ABC, NBC, FOX, The Wall Street Journal and The New York Times to provide pet health advice to pet parents nationwide.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Sinus Problems Cause Pain in the Neck?

Sinus issues may cause neck pain … but only under a specific circumstance, says an ENT doctor.
*****
Neck discomfort can have numerous causes, including sleep position, a compressed nerve and even heart trouble.
Since the nasal passageways are rather near the neck, you might be wondering if there’s any chance that a problem in your nose could be related to pain in your neck region.
The answer is yes — but only under a specific circumstance.
“Neck pain cannot be from sinus problems unless you additionally have sinus symptoms,” says Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology (ear, nose and throat).
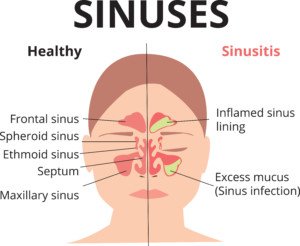
What are the typical sinus related symptoms?
Shutterstock/Ekaterina Siubarova
Sinus symptoms classically consist of a headache (that often feels like a stress or tension type of headache), pressure or aching behind the eyes or across the forehead, nasal congestion, and, says Dr. Silvers, facial pressure (a common symptom of sinus problems) or discomfort in the upper teeth.
“You would not have isolated neck pain with the sinuses as a cause with no other symptoms,” says Dr. Silvers.
So if your only symptom is an ache in your neck, then you need to keep seeking out the cause if it persists despite, for instance, changing pillows or how you sit before the computer, or with a warm compress to help heal strained muscles.
Other Sources of Neck Pain
“Neck pain can be muscle, bone or nerve related,” adds Dr. Silvers. “Our necks are very sensitive and can be sore with stress, sleeping funny and even holding our heads in an awkward position after a while.
“Anything that causes chronic pain elsewhere in the body can also manifest itself in the neck based on how we carry ourselves and how we sleep.”
A new exercise can cause isolated neck pain, such as tilting the head upward during the exercise, which pulls at the frontal neck muscles.
A muscle spasm or a persistent ache from the exercise can result later on in the day or even the day after.
Persistent neck pain with no explainable cause (such as from prolonged bending of your head backwards from belaying your climbing partner) warrants a visit with a doctor and likely an MRI, as the pain can be caused by a pinched nerve or other problem.
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Sneezing, Sniffling after Exercise: Causes & Solutions

Find out what an ear, nose and throat physician says about sniffling and sneezing after exercise.
Do you find you must sneeze and/or have the sniffles following exercise? Even indoors?
This may occur soon after you completed your training on a stationary bike, elliptical machine, revolving staircase or treadmill.
Or, the sniffling and/or sneezing may begin starting up right after your group fitness class, martial arts class or staircase workout.
And you know it can’t be allergies if this happens indoors.
“Vasomotor rhinitis is the medical term for a runny nose,” begins Dr. Stacey Silvers, MD, of Madison ENT & Facial Plastic Surgery in NYC, who is board certified in otolaryngology (ear, nose and throat).
“Triggers in younger people can be eating spicy food, walking in cold weather and exercise. Runny nose causes sniffling and can be more constant with age.”
Allergic rhinitis is another term; does your sneezing or sniffling occur after only outdoor exercise?
Pollens in the air or even environmental pollutants can be causes.
Do the annoying symptoms occur most after you’ve hiked among wildflowers?
“An anticholinergic medication like Ipatropium bromide can dry up a runny nose and be used on an as-needed basis,” says Dr. Silvers. “This is a prescription from your physician.”
What about a runny nose during aerobic activity?
In my case, it kept happening when I was inline skating. The solution is to treat the symptom.
Every so often on the trail there was a trash can off to the side.
I’d have tissue paper in my fanny pack, and when it was time to give my nose a good blow, I simply cruised over to a trash can, blew, then deposited the used tissue paper into the can.
Then I’d take off for another round of inline skating.
It’s possible that pollen contributed to the runny nose., especially since once I stopped this fun form of aerobic exercise, the runny nose ceased.
 An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
An NYC expert in ear, nose and throat care, Dr. Silvers has been named among America’s Top Physicians and Surgeons in facial plastic surgery and otolaryngology numerous times since 2003. Dr. Silvers is an expert in the field of minimally invasive rhinology, resolving patients’ breathing and sinus problems with simple in-office procedures.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Vladimir Gjorgiev
How Soon after Total Hip Replacement Can you Cross Legs?
An orthopedic surgeon provides guidelines to crossing legs after total hip replacement surgery.
For many, crossing the legs is second nature.
The tendency to want to do this will be strong even after a cross-legging person undergoes a total hip replacement surgery.
If this is a strong habit for you, and you plan on having a total hip replacement — or have just had one — you’re going to have to give up this habit for a while.
How Long to Refrain from Crossing Legs After a THR
“Some surgeons will limit leg crossing after total hip replacement for six weeks,” says Marc W. Hungerford, MD, Chief of Orthopedics at Mercy Medical Center and Director of Joint Replacement and Reconstruction at Mercy.
Six weeks — yes. That may seem like along time to abandon a habitual seating position. But you really should do this.
Dr. Hungerford explains, “Bringing the hip across the body midline and rotating it could cause the hip to dislocate.
“The restriction is usually in place for six weeks until the tissues around the hip have healed.”
This guideline applies whether a person has an elective THR due to degenerative joint disease (osteoarthritis in the hip) or due to a fractured hip from an accident.
And it doesn’t matter if you’re a man or a woman. The new hip needs a chance to settle in.
What about crossing the legs after a total knee replacement?
“There is usually no restriction to crossing the legs after TKR,” says Dr. Hungerford.
However, after a TKR, you should not do deep squats or sit on your heels (common positions for gardening). And this rule is in place for all time following the surgery.
The need for elective total hip (and knee) surgery is caused by the reduction of cartilage between the bones.
In some cases there is no cartilage; the X-ray shows bone-on-bone contact. Crossing one’s legs does not cause the hip cartilage to wear down.
 Dr. Hungerford was the first orthopedic surgeon in Maryland to perform MAKOplasty, a minimally invasive partial knee procedure powered by the RIO® Robotic Arm Technology.
Dr. Hungerford was the first orthopedic surgeon in Maryland to perform MAKOplasty, a minimally invasive partial knee procedure powered by the RIO® Robotic Arm Technology.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik
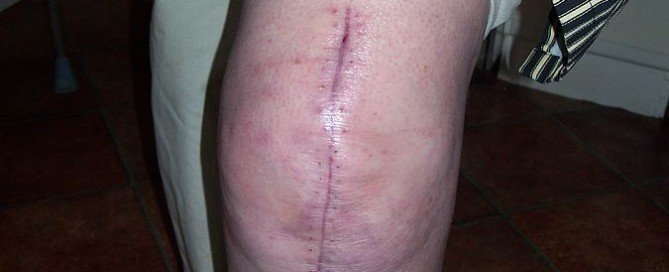
Why Swelling of Surgical Leg (TKR) Goes Down Overnight
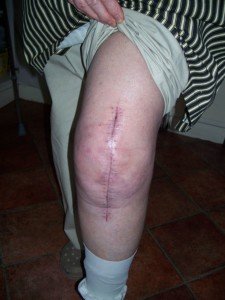
An orthopedic surgeon explains why swelling of the surgical leg (total knee replacement) goes down overnight and then seemingly balloons up after awakening.
Following a total knee replacement, the patient may notice that the initial swelling subsides as the hours after the surgery pass.
But then, come next morning, the leg looks bigger than ever, all puffed up.
The patient may then be alarmed over the possibility of a blood clot (deep vein thrombosis).
A DVT is an alarming problem because at any moment, a piece of the blood clot (or the whole thing) could dislodge and in seconds get into the lungs and cause a life threatening pulmonary embolus.
Swelling after a Total Knee Replacement
“Swelling is a function of circulation and fluid pressure,” begins Marc W. Hungerford, MD, Chief of Orthopedics at Mercy Medical Center and Director of Joint Replacement and Reconstruction at Mercy.
“After a total knee replacement the circulation to the knee is increased because of the body’s healing response.
“When you are standing or sitting during the day, the leg is in a dependent position and the pressure in the blood vessels is increased.
“When sleeping at night, the leg is at the same level relative to the rest of the body and the pressure decreases. This allows the pressure and swelling to go down.”
But then once you’re awake — and up and about — you may see that the leg appears to be swelling more.
Following TKR, the patient is urged to get up and about as soon as possible, not only to help prevent a blood clot, but to hastily get the joint acquainted with its new device. The sooner the better.
Nurses will check both legs of the patient throughout the day to make sure that the swelling is par for the course rather than suspicious for a DVT.
Over 600,000 total knee replacements are performed in the United States every year!
Each year, over 600,000 total knee replacement surgeries are performed in the U.S.
The knee joint is the most unstable joint in the human body.
Adults of any age can be affected by osteoarthritis, though it’s most common in older people.
 Dr. Hungerford was the first orthopedic surgeon in Maryland to perform MAKOplasty, a minimally invasive partial knee procedure powered by the RIO® Robotic Arm Technology.
Dr. Hungerford was the first orthopedic surgeon in Maryland to perform MAKOplasty, a minimally invasive partial knee procedure powered by the RIO® Robotic Arm Technology.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.