Teaching Your Child to Refuse Candy from Strangers

Pedophiles often use candy to lure their child victims. Here’s how to teach young children to refuse candy being offered by a “nice” stranger!
A predator with half a brain will always have a bag of candy on him.
When teaching your child never to accept candy from a stranger, you should avoid the following mistakes.
Threats won’t work, such as, “If I ever find out you took candy from a stranger, I’m gonna (fill in the blank)!”
“Attempting to use a fear factor will only cause the child to be afraid of the parent, not the stranger,” says Dr. Shani Verschleiser, Founder and CEO of Magenu, a non-profit organization that creates and implements educational curriculums dedicated to empowering children in personal safety and awareness.
“It will also make sure that a child will never tell you if they actually are in a situation that is questionable or if they need help.”
In fact, most predators will use the tactics of telling children to keep secrets because their parents will be really mad at them, and these types of [threatening] comments [from the parents] reinforce to the child that the predator is telling the truth.
“In addition, giving a child this kind of statement doesn’t explain anything to the child in terms of what danger they are exposing themselves to.
“It only allows them to feel danger from their parent, which means if they feel they can ‘get away with it,’ and the parent will never find out, then they would still take the candy.”
“If you take candy from strangers, you’ll get fat!”
This tactic focuses on self-esteem, not the dangers of taking candy from strangers, says Dr. Verschleiser.
“A child who is told this comment really has no basis for why the stranger is dangerous; only that they are at fault if they eat the candy.
“In addition, if the child actually answers, ‘I can’t eat the candy because it will make me fat,’ as per the parent, the stranger can then just respond with, ‘Not this kind of candy,’ or, ‘It’s healthy candy,” or, ‘It’s low fat,’ etc. And then guess what: The child will be prone to taking candy from this crafty stranger!”
Tactics for Teaching Children not to Take Candy from Strangers
#1. Ask your child point-blank, “What would you do if someone you didn’t know offered you candy?” Include specifics (e.g., a man approaches you on the sidewalk. Hear out the response.
#2. If the response is “I’d take the candy,” or it’s vague, follow up with the question below.
#3. Ask, “Do you find it odd that a stranger would just come up to you out of the blue and offer you candy?” Then listen to the answer.
#4. Explain why it’s really bizarre, and hence, extremely suspicious, that a stranger would offer a child candy. Don’t just say, “A well-meaning stranger wouldn’t do that.” Explain WHY.
If you believe your child is old enough to be out and about alone (walking to a friend’s house, riding a bike in the neighborhood, etc.), then they’re old enough to be told about pedophiles, and that the next stranger who offers them candy may be a pedophile.
#5. Ask your child why they would think a stranger would want to give them candy. This will force them to reflect and analyze. Their analysis will force them to see this situation with more insight.
The child is apt to conclude, “Gee, that would be weird, a stranger picking me off the street randomly and wanting to give me candy!” This realization will strengthen the stranger danger radar.
#6. Explain, “You can never want candy bad enough that you’d take it from a stranger, when instead you can ask me for candy.
“If you think I’ll say no, ask anyways, because you know that eventually I’ll give you candy.
“If you’re tempted by a stranger’s offering, ask yourself if you want it badly enough to risk being abducted.
“If you want it that bad, run in the opposite direction and tell me what just happened.”
#7. Ask your child to tell you why they think a well-meaning stranger would require them to get into his car to have the candy. Again, this will force analysis.
#8. Ask why a well-meaning stranger wouldn’t first get permission from the parents. This will force analysis.
#9. Include role-playing in a variety of scenarios, using your kid’s favorite candy as a prop.
#10. Arrange for a trusted male friend, whom your child does not know, to pose as a predator and approach when you know the child will be alone.
Have your friend report to you what happened when this “stranger” offered your child candy, and discuss this with your child.
If you learn he or she took the offer, Dr. Verschleiser suggests the following:
“The candy lure by strangers needs to be combatted with the rule of never taking anything from anybody unless you okay it first.
“This applies to non-strangers as well because it happens to be a stage in the grooming process of predators.
“If you tell a child you can never take a present/candy, etc., from anyone including your brother/cousin/uncle, etc., without asking (me) first, then the rule applies to strangers as a given.”
 Dr. Verschleiser is a mother of three and is on a mission to educate teachers, parents and children about the topics of safety.
Dr. Verschleiser is a mother of three and is on a mission to educate teachers, parents and children about the topics of safety.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/epixproductions
Soucre: missingkids.com/home
How Effective Is Calcium Score Test at Heart Disease Prevention?

Knowing your calcium score just might save yourself from death by heart disease.
But it’s not as simple as an absolute number that applies to every single individual in the same way.
There are multiple considerations when it comes to your calcium score result.
When a celebrity dies in middle age from a heart attack, do you ever wonder if he or she had known their calcium score, would this knowledge have changed the trajectory of their lifestyle habits long-term and possibly prevented that heart attack?
Fact is, most people have never, and will never, have a calcium score test done. This includes the rich and famous.
Heart disease kills well over half a million Americans every year.
The most common type of heart disease is that of the coronary arteries (coronary artery disease, or CAD), and this can lead to heart attacks, chronic chest pain and shortness of breath (angina), heart failure, stroke and abnormal cardiac rhythms.
What is a calcium score test?
This non-invasive, 15-minute screening procedure can help present an overview of one’s heart health – within the context of other indicators such as the presence or absence of diabetes and obesity.
A CAT scan detects calcium deposits in the three major coronary arteries.
Calcium deposits strongly correlate with plaque buildup (blockages), and of course, plaque deposits correlates to coronary artery disease and cardiac event risk in the next three years.
It’s not recommended that a person have a calcium score test more frequently than every five years.
• The patient’s medical history is applied to the total calcium score.
• The number is then compared to patient databases for that individual’s gender and age to arrive at a final number.
• The lower the score, the less likely the presence of plaque buildup.
• A number of 150+ indicates excessive calcium deposits.
• Medical insurance usually will not cover the procedure, which can range from $70 to $350.
Effectiveness of Calcium Score Test
“A calcium score test is not a good test to determine prevention,” says Dr. Krishnan is with Pacific Heart & Vascular, a board-certified adult general cardiologist with advanced subspecialty training in interventional cardiology.
“The plaque volume is calculated and a risk score for future events has been calculated based on the number.
“Obviously the higher the score, the greater the chance for a cardiac event.”
But a very high score, such as 1,450, doesn’t guarantee a heart attack. An elderly person can live another 10 years after being told he has a calcium score of 1,450.
“It is also a long-term predictor of morbidity and mortality, but really does nothing for patients in the short-term,” says Dr. Krishnan.
“Many cardiologists can use it to guide further therapy in patients who fall in sort of a gray zone based on their risk factors.
“For example, an otherwise healthy patient with bad cholesterol numbers, who sort of exercises on an infrequent basis, could have a calcium score test performed — and the result can help guide whether he should be on further aggressive treatment such as aspirin or statin therapy.
“Patients who are low risk really would not benefit from this test and should continue maintaining a heart healthy lifestyle.
“Patients at high risk should be closely monitored and should be considered for more aggressive tests such as stress testing (along with heart medications).”
Fear of a Heart Attack Any Day After Getting a High Calcium Score Result
Dr. Krishnan explains, “In my practice I see a lot of patients who have been ordered calcium scores by other physicians, and they come to me quite anxious and paranoid at the results — thinking that they’re going to have a heart attack very shortly.
“I often end up having to reassure them that the best test for them to undergo in the short-term is a functional stress test to determine if there is any immediate coronary blockages.”
 Dr. Krishnan is with Pacific Heart & Vascular, where you can view his videos on heart disease and healthy living. He has numerous publications and often speaks at local and regional events.
Dr. Krishnan is with Pacific Heart & Vascular, where you can view his videos on heart disease and healthy living. He has numerous publications and often speaks at local and regional events.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Best Diet for Improving Congestive Heart Failure

If you’ve been diagnosed with heart failure, you’ll want to seriously consider changing your diet as part of your treatment.
A study from the University of Michigan Frankel Cardiovascular Center shows that after only 21 days on a particular diet, patients with heart failure had improvement.
The diet is called DASH: dietary approaches to stop hypertension.
This is not a gimmicky or strange diet; it’s quite sustainable and can drop high blood pressure (hypertension) as effectively as drugs.
“Our work suggests diet could play an important role in the progression of heart failure,” says Scott Hummel, MD, in the paper.
If you have heart failure, ask your cardiologist if it’s the type with preserved ejection fraction. This is the type that the study focused on.
Heart Failure Patients Who Changed Their Diet
The subjects were mostly in their 60s and 70s and kept food diaries, and also agreed to eat only the meals that were prepared by the University of Michigan Clinical Research Unit.
The diet conformed to the DASH plan, which limits daily sodium to 1,150 milligrams and has other parameters as well.
The DASH diet is high in important minerals like magnesium and potassium.
Dietary Changes Can Help People Manage their Chronic Heart Failure
“The diet itself is simply a balanced diet that is extremely low in sodium due to its lack of processed foods,” says Dr. Keith Kantor, a leading nutritionist and CEO of the Nutritional Addiction Mitigation Eating and Drinking (NAMED) program, which treats substance abuse, mental illnesses and other illnesses.
“Congestive symptoms can be improved and lead to long-term disease management if the diet is followed exclusively.”
Dash to the DASH Diet to help improve management of chronic heart failure.
 Dr. Kantor has a PhD in nutritional science and a doctorate in naturopathic medicine, has appeared on CNN and Fox News Channel for his expertise, and has been an advocate of natural food and healthy living for 30+ years.
Dr. Kantor has a PhD in nutritional science and a doctorate in naturopathic medicine, has appeared on CNN and Fox News Channel for his expertise, and has been an advocate of natural food and healthy living for 30+ years.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com, peoplecreations
Source: sciencedaily.com/releases/2013/09/130924153628.htm
Are Heart Attacks with No Chest Pain Less Severe?

Is there a link between how mild or severe chest pain is, and how mild or massive a heart attack is?
Heart attacks often come with chest pain, but some come without or with just a little bit of discomfort.
It should not be surprising that for many people who’ve suffered a significant or massive heart attack, the chest pain was either mild or non-existent.
“Your body is often not good at identifying heart pain because it has not had any practice,” says Christopher J. Hanifin, PA-C, who was previously a physician assistant in open heart surgery with Cardiothoracic Surgery of South Bend in South Bend, IN.
Hanifin explains, “Think about your thumb. You have spent your whole life touching it, twisting it, burning it, hitting it with a hammer, slamming it in the door, and getting splinters stuck in it.
“When something is wrong with your thumb, your body knows just what is going on.
“Contrast this with your heart. At least during your first episode, your nervous system has no experience identifying heart pain.
“When you start to have a heart attack, your body can have a hard time figuring out what is going on. The pain can radiate to either arm, your neck, your jaw and even your teeth.”
Study Shows No Connection Between Absence of Chest Pain and Severity of Heart Attack
A paper published in a Sept. 2013 JAMA Internal Medicine details a study of over a thousand women 55+ who had heart attacks – but reported no chest pain.
Dr. Louise Pilote, senior study author, urges people to get away from the perception that heart attacks usually mean an “older man clutching his chest.”
There are other symptoms to be acutely on the lookout for, such as shortness of breath, weakness and rapid pulse.
The so-called Hollywood Heart Attack creates the illusion that this event necessarily comes with enough pain to make someone clutch or grab their chest.
In the study, 20% of women suffering a heart attack did not experience chest pain. And, absence of chest pain was not associated with less severe heart attacks.
Don’t ever think, “Well, if I’m having a heart attack, it’s only mild because I don’t have any chest pain with this shortness of breath.”
The absence of chest pain may mean fewer symptoms altogether, but this does not mean that the disease state itself is less severe.
An exact diagnosis cannot be made based on presence or absence of symptoms.
“Another important factor to consider is that some patients who are at increased for heart attack generally have decreased pain sensation,” says Hanifin.
“Diabetes is a big risk factor for coronary artery disease.
“It’s pretty well-known that diabetics need to check their feet regularly and carefully because they can develop sores and injuries and not have the associated pain. The same thing can happen with heart pain.”
 Christopher J. Hanifin, PA-C, is currently Department Chair and Assistant Professor, Department of Physician Assistant, Seton Hall University, NJ.
Christopher J. Hanifin, PA-C, is currently Department Chair and Assistant Professor, Department of Physician Assistant, Seton Hall University, NJ.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/uzhursky
Source: sciencedaily.com/releases/2013/09/130916204742.htm
How Accurate Is a Stress Test for Women’s Heart Disease Detection?
A treadmill stress test to determine the presence of heart disease in women is not as accurate as you may think.
If you’ve always imagined that all a woman needs to do, to find out if she has clogged coronary arteries (heart disease), is to take a treadmill stress test so that doctors can see if there’s restricted blood flow during exercise — think again.
Maybe one day it will be that easy, but currently, it’s nowhere near it.
“It is a known fact that stress test has 50% sensitivity and specificity for detecting CAD in women younger than 60 years of age due to the phenomenon of false positive test,” says Asim Cheema, MD, who’s board certified in internal medicine, cardiovascular diseases and interventional cardiology by the American Board of Internal Medicine. Dr. Cheema is with Your Doctors Online, an online doctor chat site.
Dr. Cheema also adds, “The exact cause/mechanism of false positive test in women is unknown but likely related to hormones (progesterone).”
Let’s Look at a Study
A study in the Dec. 2012 issue of The American Journal of Cardiology reports a promising conclusion to researchers’ investigation of treadmill stress tests identifying heart disease in women.
However, the percentages aren’t exactly super high, as you’re about to find out.
The report points out that many physicians don’t put a lot of faith in the accuracy of the exercise treadmill test (ETT) in detecting women’s heart disease.
Nevertheless, the researchers, from UC Davis, discovered that the exercise treadmill test can accurately predict heart disease in women over age 65.
Though this sounds great, it’s not too impressive for women under age 65.
The paper notes that the predictive efficacy of the treadmill stress test was enhanced by two particular EKG indications.
The exercise treadmill exam includes an EKG reading. If the exam detects signs of heart disease, then more invasive and definitive procedures are warranted, such as the catheter angiogram.
This is actually the gold standard in identifying blockages, but it’s very invasive and carries with it the risk of stroke and heart attack.
The study involved 111 women who reported chest pain and whose treadmill results were “positive.” These women underwent catheter angiograms.
The Results
Half the women had heart disease (determined by the catheter angiogram).
When the results were broken down by age, the percentage went up to 68 percent for women over age 65, and down to 36 percent for women 35 to 50.
The percentage for the older women may not seem impressive, but to the researchers, it’s a mark of a successful procedure.
What about the EKG?
Two indicators, called the ST-segment depression and the ST-segment recovery, turned out to be important to the ETT’s diagnostic value.
For women over 65, longer ST-segment recovery time yielded an 80 percent prediction rate of heart disease.
Tips for Reducing the Risk of Coronary Artery Disease for Women and Men
• Don’t stress about the small things in life. Practice stress management.

• Realize that just because you “feel” beautiful doesn’t mean you practice heart-healthy habits.
Make sure you’re at a medically acceptable weight.
• Do both strength and cardio exercise.

Shutterstock/Nata Kotliar
• Don’t assume your heart is healthy just because you weigh 120. If you smoke, quit. If you eat a lot of processed foods, cut back, especially on high sodium foods.
• Avoid trans fats, limit saturated fats, and eat more “good fat” foods like olive oil, seeds, nuts and fish.

Your Doctors Online offers a free 7 day trial where you can ask a doctor questions online and get answers in minutes from anywhere 24/7. Learn more here. Dr. Cheema teaches and provides supervision to graduate students at the Institute of Medical Sciences, University of Toronto.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: ©Lorra Garrick
Source: sciencedaily.com/releases/2012/12/121206153646.htm
Why You Should Wear Earplugs at Ball Games & Other Sports
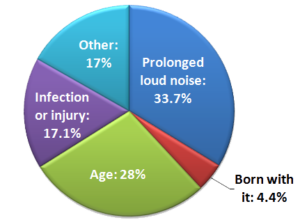
Hearing loss causes; which is No. 1?
The screaming at ball games and other sporting events is literally deafening, yet very few people think to wear earplugs at these events. You’re ruining your hearing.
The loud screaming, hollering and cheering at ball games and other sporting events not only can cause hearing loss, but just one game can damage hearing.
There are sporting events that have been studied for the very purpose of hearing loss from the loudness.
“To provide an example of one such event, a study of noise levels produced at an NCAA arena has shown that one-third of the participants tested over the course of three home games for the Murray State Racers were exposed to noise levels above the OSHA noise exposure limit of 85 dB for an average of eight hours,” begins Rivka Strom, AuD, CCC-A, chief audiologist at Central Hearing LLC in NY.
“OSHA is the Occupational Safety and Health Administration, and they set noise exposure limits for levels based on a timing factor,” continues Strom.
“The effect of noise induced hearing loss (NIHL) are potentially serious — and while spectators may realize these events are loud, they may not realize they are dangerous to the ears. Ear protection is a MUST at these events!”
One Sporting Event Is All It Takes to Damage Hearing
This is the finding from a study by Bill Hodgetts (U of A’s Faculty of Rehabilitation Medicine) and Dr. Richard Liu (Faculty of Medicine and Dentistry).
They measured noise levels at games 3, 4 and 6 of the Stanley Cup finals against the Carolina Hurricanes in 2005.
Don’t let that past date fool you; their findings still stand strong.
Results of Sound Level Meter Testing
It took under six minutes to achieve the maximum allowable daily dose of noise volume.
To put another way, every fan without earplugs got socked with about 8,100 percent of their daily noise dose.

The paper adds that fans aren’t the only ones at risk for hearing loss at sporting events; athletes and employees are as well.
One must wonder how damaged the hearing is of that brawny hockey player who proudly sports his permanently disfigured nose.
The study report points out that usually, fans’ ears will recover after one or two games.
But do you have season tickets or otherwise attend frequently? Whatever hearing loss you eventually develop will be connected to these games.
Who’d ever get caught dead wearing earplugs to a sporting event?
One woman posted in an etiquette forum that she nonchalantly popped in earplugs when the woman behind her began screaming blood curdles every time her team scored.
We all want to have fun and root for our teams. But must you sound like Fay Wray when she sees King Kong for the first time?
The woman with the earplugs never even turned to look at the screamer, yet the screamer became offended at the sight of someone in front of her putting in earplugs and began hurling obscenities.
Though the reaction by this nutcase is the exception, you should not hesitate to pop in earplugs. In fact, put them in as you take your seat rather than after the fact.
Just like you’d wear sunscreen to protect your skin while at the ball game, a cap to shield your eyes from glare, mittens to keep your hands warm, a scarf over your nose, and so on, why should earplugs be excluded from your arsenal of body protection?
Never mind what strangers, or even your own camp, might think.
You may need to loosen one or both plugs to fully understand conversation with your group amid a generally noisy atmosphere, but when conversation is finished you can just push the ear plugs firmly back in to protect your hearing.
The study appears in the 2006 Canadian Medical Association Journal.

Dr. Strom is a member of the American Speech Language and Hearing Association and has received several awards including Brooklyn College’s Excellence In Audiology Award.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Sources: sciencedaily.com/releases/2006/12/061206095322.htm; etiquettehell.com/smf/index.php?topic=112801.0
Supplement Pills Stuck in Chest Feeling: Solutions

Here’s how to prevent getting that pills stuck in chest feeling after taking several supplements at once.
Have you found that often, if not always, whenever you take your usual “handful” of supplement pills, that soon after, it feels as though they are stuck in your chest?
The stuck pill sensation can be described as being behind the breastbone (sternum) or somewhere in the esophagus — which is actually behind the breastbone.
The way to prevent the sensation that a cluster of supplement pills are stuck somewhere behind your breastbone or in your chest is to keep your head lowered a bit while swallowing the nutritionals.
This seems counterintuitive to the traditional way of swallowing a pill: tossing the head back while swallowing with the water.
Somehow we’ve been led to believe that tilting the head back will assist in getting something down the throat.
I was doing some online research into the issue of that stuck feeling in the esophagus, as this had been occurring to me (I take numerous supplements daily).
Tossing the head back narrows the passageway through which pills and food travel, and lowering the head, on the other hand, opens up the passageway more — thus creating an easier path for incoming pills to slide down.
If this still seems like it would cause you to choke, think of it this way:
When you eat food — meat, cereal, candy, a crunchy salad, munchies, a sandwich, a milkshake, soda — do you toss your head back every time you swallow a mouthful?
Of course not. Typically, when people eat, their head is straight ahead, or even tilted down somewhat, as in when they’re eating and reading a book or magazine at the same time! Yet they don’t choke.
Certainly you’ve eaten while your head was tilted downward, such as while looking at your computer keyboard, at your smartphone, etc., without gagging on the food.
Though a pill is a harder item that doesn’t get pulverized and pureed by our teeth and saliva before it slides down the throat, the principle still applies that keeping the head lowered while swallowing will help that supplement (capsule, gel cap or tablet) go down more efficiently.
So next time you take your supplement pills, keep your head lowered for every swallow.
For best results, drink some water ahead of time to lubricate the passageway, and make sure you drink a big glass of water (or fluid) with your nutritional supplements for optimizing the prevention of that stuck in the chest feeling.
Two More Solutions
“Feeling of pills stuck in the esophagus happens when the supplements are passed into the esophagus but are not moving into the stomach, causing discomfort and chest pain,” says Natasha Fuksina, MD, an internal medicine and obesity specialist who combines traditional, integrative and functional medicine to restore health and function.
“This can be alleviated by swallowing small amounts of warm liquids, sometimes with a small amount of soft food, which can help propel the stuck pills into the stomach.”
Second, you may want to consider spreading the intake of all of your supplement pills throughout the day rather than as a bunch in one sitting.
 Dr. Fuksina is the founder of astraMDhealth, which includes telemedicine. Double board certified in internal and obesity medicine, she focuses on a personalized approach, including metabolism and genetic makeup, to customize treatments and preventive care.
Dr. Fuksina is the founder of astraMDhealth, which includes telemedicine. Double board certified in internal and obesity medicine, she focuses on a personalized approach, including metabolism and genetic makeup, to customize treatments and preventive care.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/sirtravelalot
Noise Sensitivity ADHD: Real Illness or Product of Culture?

One of the symptoms of ADHD, according to WebMD, is the following:
“Easily distracted by irrelevant stimuli and frequently interrupting ongoing tasks to attend to trivial noises or events that are usually ignored by others.”
This describes me perfectly. However, this does not mean I have ADHD or some kind of problem or neurological issue.
People who’ve been diagnosed with “noise sensitivity” or “hypersensitivity to noise” due to ADHD would find that, in certain environments (e.g., out in the country), their alleged problem would be non-existent.
In a culture replete with relentless auditory stimuli, seems like the oddballs are people who CAN ignore it all.
If your coworker keeps repeatedly tapping their pen on the desk, or keeps making clucking and smacking sounds with endless gum chewing, and you find this disruptive to your concentration, WHO really has the problem?
Not you! This is an issue of being considerate vs. inconsiderate, not who might have ADHD (or ADD).
Some years ago I was repeatedly distracted by ongoing giggling of a young woman who was being taken on a tour of my workplace. For all I know, nobody could stand it.
But even if I’d been the only one, this doesn’t make me noise sensitive or ADHD.
Instead of wondering why I’d be the only one distracted by ongoing giggling (nobody was telling funny jokes; it was merely a tour), the better question is why was this woman giggling at everything?
Let’s look at some culture-based noises that people who’ve been diagnosed with ADHD are driven “crazy” by:
- loud high pitched beeps from vehicles backing out
- motorcycle engines and men fooling around with their car motors
- clocks clanging every hour
- ticking clocks
- hums from various machines (computers, lighting fixtures, ventilation, refrigerators, copy machines)
- chairs squeaking
- bus and car brakes shrieking.
What’s ADHD “noise sensitivity” today was non-existent 100 years ago.
The website for the Environmental Protection Agency identifies noise pollution as a real problem:
Noise pollution adversely affects the lives of millions of people. Studies have shown that there are direct links between noise and health.
Problems related to noise include stress related illnesses, high blood pressure, speech interference, hearing loss, sleep disruption, and lost productivity.
Noise Induced Hearing Loss (NIHL) is the most common and often discussed health effect, but research has shown that exposure to constant or high levels of noise can cause countless adverse health effects.
What about noise that’s been around since the beginning of time? That would be loud laughter, shrieking and screaming children, noisy eating, knuckle cracking, whistling and humming.
I once finally told a coworker that his incessant whistling was very annoying. This doesn’t make me ADHD. Brazen, maybe, but not ADHD.
More power to those who can tune out rude people.
But this doesn’t mean that others have ADHD or “noise sensitivity.” Like the EPA says, noise pollution is real.
I don’t consider myself ADHD just because I wear ear plugs at Whole Foods Market where piped in music blares and toddlers scream nearby, or at the gym where attention-seeking men smash metal weight plates into each other.
I don’t want noise induced hearing loss. This doesn’t make me ADHD.
I’m no more ADHD for wearing ear plugs to preserve good hearing than someone is for wearing sun block to protect their skin, or avoiding cigarette smoke to protect their lungs. Being health conscious does not make you ADHD.
The criteria for ADHD has been expanded over the years, and some of this involves how one reacts to noise.
If my reaction to unnecessary and offensive sounds (e.g., neighbor keeps revving up his thundering car engine over a 30 minute period just to play around with it, versus revving up a malfunctioning engine for a few minutes to get it going so he could drive to work) means I probably have ADHD, then that’s fine with me because it also means I’ll have great hearing well into old age since I make efforts to avoid loud or shrieking sounds.
There’s normal and necessary noise (lawn mower, carpet steam cleaner, crying infant or injured young child), and then there’s intrusive and unneeded noise (letting toddlers and preschoolers scream in stores, raucous laughter in the workplace, adults screaming over petty things, incessantly barking dog).
If you want to protect your hearing from harm and be a healthier person, this doesn’t mean you have “noise sensitivity” or ADHD.
UPDATE: In March 2022, the author of this article was diagnosed with Autism Spectrum Disorder — but not ADHD.
Though the autism explains getting distracted by irrelevant sounds that would not be noticed by other people, and finding some non-loud sounds to be very annoying — the desire to protect one’s hearing in loud environments to avoid future hearing loss is not indicative of a neurodivergent mind.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: ©Lorra Garrick
Sources: webmd.com/add-adhd/guide/adhd-symptoms; womenwithadhd.com/forum/topics/sensitivity-to-repetitive; epa.gov/air/noise.html#health
Cough Is Getting Worse: What Does an ER Exam Involve?
If you have a worsening cough, get to the emergency room because it can be serious; here’s what’s involved.
When my mother developed a cough with phlegm that sounded horrible — and after several days was only worse — I took her to the ER, suspecting pneumonia.
My mother was taken to a room in the ER, and soon the doctor appeared. The doctor asked her many questions.
If you go to the ER with a cough, the doctor will ask a lot of questions.
This includes if you have symptoms other than the cough such as fever or chills.
This helps guide the doctor in suspecting viral versus bacterial pneumonia.
“If a cough is rapidly worsening, it is crucial to seek medical attention promptly,” says Alice Benjamin, a clinical nurse specialist, and chief nursing officer and correspondent for nurse.org.
She explains, “Early intervention can lead to earlier diagnosis and initiation of appropriate treatment.
“Delaying medical care can allow the condition to worsen, potentially leading to more severe complications and a more challenging recovery.”
Pneumonia, which can be life-threatening at any age, isn’t the only potentially serious problem of a cough.
Benjamin points out that it may also be caused by congestive heart failure and lung cancer, though bronchitis can also be the culprit.
The doctor ordered a chest X ray for my mother, then had the nurse come in and give her a five minute albuterol treatment, in which she breathed into and out of a hand-held tube device that expelled vapors.
Vitals were taken, but a blood test was not taken (though lab tests are typically taken).
The doctor seemed very sure that the coughing was either from pneumonia or bronchitis.
In fact, after listening with a stethoscope, he said he heard wheezing, which he thought was likely caused by bronchitis.
The chest X ray showed “a little” pneumonia. The doctor then prescribed an antibiotic called Levoquin.
She was given one 500 mg pill right there (about 10 pm), then discharged with an albuterol inhalation pump.
The ER visit wasn’t that long, but of course, length of stay will depend on how busy the emergency room is, and whether a patient gets “bumped” by an incoming patient with a more serious presentation.
The ER facility need not be a hospital; it can be an urgent care facility, which is fully equipped to deal with cases of pneumonia.
I’ve taken my mother to an urgent care facility as well for a worsening cough.
An ER visit for a bad cough is well-worth the time investment.
A bad cough that goes untreated can turn out to be pneumonia, which the Centers for Disease Control says kills about 50,000 Americans a year.
“Visiting the emergency room for a rapidly worsening cough, especially for individuals over the age of 65, is important for several reasons,” says Benjamin.
“A rapidly worsening cough can be a sign of respiratory distress, which may result in decreased oxygen levels in the blood.
“Hypoxia (low oxygen levels) can be particularly dangerous for older adults and can lead to confusion, dizziness and organ damage.
“ER staff can quickly assess oxygen levels and provide appropriate interventions.”
Older adults are also at higher risk of developing serious complications from respiratory infections, but younger adults are not immune to this outcome, either.
“The ER is equipped to evaluate and manage these types of emergencies promptly,” says Benjamin.
 Alice Benjamin, APRN, is Chief Nursing Officer & Correspondent for Nurse.org. In addition to being a clinical nurse specialist and family nurse practitioner, she also has 20+ years of experience in critical care and emergency medicine, and gives podcasts on health.
Alice Benjamin, APRN, is Chief Nursing Officer & Correspondent for Nurse.org. In addition to being a clinical nurse specialist and family nurse practitioner, she also has 20+ years of experience in critical care and emergency medicine, and gives podcasts on health.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ Stockbakery
Sources:
my.clevelandclinic.org/heart/disorders/aorta_marfan/aneurysm_aorta.aspx
cdc.gov/Features/Pneumonia/
Cause of Blackout in Seemingly Healthy Elderly

Do you know an elderly person who blacked out for no apparent reason, with no history of fainting?
An elderly person apparently blacks out and falls. First of all, you need to determine — if possible — that they actually passed out while upright, versus lost their footing or a knee buckled and then fell.
I’d been staying with my elderly parents to care for them; my mother was experiencing severe pain from a herniated disc, and my father had just had knee revision surgery.
The knee rehabbing was going good; my father got around on a walker. Though there was a lot of post-surgical pain, he was stable with the walker.
Then a THUD! in the Middle of the Night
Eight days after the surgery, I heard a thud at 3:30 in the morning; my mother called out to me.
I dashed into my parents’ room and found my father prone (stomach down) on the floor, shoulders and head in the bathroom.
His surgical knee was over the walker, which was lying on the floor.
I removed it from under the leg, and my first thought was that the knee surgeon goofed up; the hardware suddenly loosened.
I got on my knees and within seconds realized my father was disoriented and belligerent (not his nature), and not responsive to my simple commands to alter his body position so that I could better assist.
He was holding his stomach off the floor; only his forearms, knees, thighs and feet were making contact, and he was stuck in this position.
I immediately knew that this fall had not been broken consciously as he went down, because:
1) He had altered mentation, indicative of a significant whack on the head, and 2) He had a purple and red “goose egg” hematoma on his forehead, indicative of a hard fall.
Based on his body position, he had fallen forward. Because the walker had been under his leg, this meant that, just prior to the fall, he had slumped forward over the walker, body weight crumbling on top of it as he pitched forward, knocking the device over as he fell over it.
Sleuthing 101: He’d had a blackout while standing, while using the walker to get to the bathroom.
He had passed out, then fallen. The knee could not have given way; otherwise, he would have supported himself on the walker and remained upright.
Knee pain would not have made him fall over the walker and end up prone on the floor, walker under leg. Pain would have simply made him safely shuffle back to the bed.
The floor was clear of obstacles; tripping was ruled out. He had blacked out.
Why would a seemingly healthy elderly person black out?
I also considered that my elderly father didn’t actually black out, but instead, became so dizzy or lightheaded that he fell forward, still conscious but not grounded enough to break the fall. I suspected a narcotic painkiller contributed.
I also suspected his high blood pressure drug, Lisinopril, which can cause fainting as a side effect.
It was more than a coincidence that a fainting spell occurred in that tiny sliver of time during which my elderly father got up in the middle of the night to use the bathroom; I suspected a big blood pressure drop caused by medications.
Emergency room personnel suspected a “cardiac event” because a blood test revealed that his troponin was elevated.
He was admitted to the cardiac unit. The follow-up troponin test yielded no upward trend, so heart attack was ruled out.
The doctor suspected one of three things:
1) A combination of dehydration, physical stress from the recent knee surgery, Lisinopril side effect and Flomax side effect.
My father had been taking Flomax for quite a while, and the doctor said it causes dizziness in 30 percent of patients.
2) Heart rhythm disorder, or 3) Heart valve problem.
A heart rhythm and valve disorder were ruled out with tests. Blood sugar was normal, ruling out diabetes. CT scan of head was normal.
The diagnosis of exclusion, then, for why my elderly father blacked out, was “the perfect storm” of recent knee surgery stress, lack of hydration, Lisinopril and Flomax.
The doctor took him off the Lisinopril and Flomax.
A week out from the blackout, he continued to sometimes experience the “room swirling” upon sitting up from a back-down position on his bed.
Takeways from a Medical Doctor
“To prevent from having a fainting episode, it’s important to make sure you maintain a good hydration status,” says Amber Robins, MD, a board certified family medicine physician in NY.
“A good way to tell if you’re hydrated is by looking at your urine. If it is yellow, this means that you may need to drink more fluids.

Shutterstock/gritsalak karalak
“Keep in mind that you can also overdo your hydration which could lead to other medical issues.
“This is where speaking to your primary care doctor about your particular medical conditions may be most appropriate.
“After a knee replacement or any surgery, a patient may also be on pain medications. For some, this can lead to feelings of dizziness which could lead to having a fall.
“Again, I would suggest talking with your doctor to discuss a regimen that may be best for you.”
Remember, if an elderly family member has had surgery, hydration is super important.
However, clear with the surgeon just how much water a day the patient should be getting.
And make sure that the family member is taking any medications in their proper doses.