Can Microscopic Colitis Diarrhea Deplete Nutrient Intake?

Wondering if the nutrients you eat go out with the diarrhea of microscopic colitis?
I sure was, after I was diagnosed and would see what appeared to be a lot of produce intake in my diarrhea.
So I was wondering if ingesting all the nutrients of the fruits and vegetables I juiced and also ate in whole form was being offset by “all the diarrhea.”
Bear in mind, however, that the diarrhea of microscopic colitis appears to be in a greater volume than it truly is, due to all the water that comes out with it.
Does the diarrhea of microscopic colitis cause the patient to lose nutrients?
“Microscopic colitis is a disease that affects the large intestine,” says Matilda N. Hagan, MD, inflammatory bowel disease specialist at The Center for Inflammatory Bowel and Colorectal Diseases, part of The Melissa L. Posner Institute for Digestive Health and Liver Disease, Mercy Medical Center in Baltimore.
“Malabsorption is not a typical part of this disease. The large intestine is primarily responsible for water absorption.
“Other causes of diarrhea that affects the small intestine can cause malabsorption where nutrients can be lost.”
In MC, the large intestine (colon) does not absorb water very well. As a result, the fecal matter that builds up gets mixed with a lot of water, causing the stools to be in the form of diarrhea once it’s voided, rather than in formed stools.
And if you can see fragments or bits of the fruits and vegetables you’ve recently eaten, that’s largely because the looseness or liquid nature of the diarrhea makes these undigested scraps easier to see, whereas with hard, formed stools, they are less visible.
So if you have microscopic colitis, feel free to eat all the nutrients you want without fearing that they are being voided out of you.
 Dr. Hagan is dedicated to collaborating with IBD specialists to discuss and explore advanced treatment options for the most complex inflammatory bowel disease cases.
Dr. Hagan is dedicated to collaborating with IBD specialists to discuss and explore advanced treatment options for the most complex inflammatory bowel disease cases.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Can Microscopic Colitis Cause Malabsorption?

Microscopic colitis can cause numerous problems including tons of diarrhea.
Can it also cause food — even healthy food — to be malabsorbed, depriving you of nutrients?
“Malabsorption is not a classic feature of microscopic colitis since the disease affects the large intestine which handles fluid absorption,” says Matilda N. Hagan, MD, an inflammatory bowel disease specialist at The Center for Inflammatory Bowel and Colorectal Diseases, part of The Melissa L. Posner Institute for Digestive Health and Liver Disease at Mercy Medical Center in Baltimore.
She adds, “You can get dehydration from large amounts of watery diarrhea.”
Here’s why you might think that microscopic colitis can cause malabsorption:
You may see particles of undigested food in your diarrhea. This can include seeds and shreds of spinach and what appear to be fragments of grapes and strawberries. You may see grains of rice.
Seeing food in your diarrhea can lead to the conclusion that there’s malabsorption.
But what’s really happening is that, due to the looseness of the diarrhea, or its dispersability in the toilet bowl water, any undigested food is easily visible.
In formed, harder stools, however, fragments of fruit, olives, or seeds or grains of rice, will be well-hidden; you’d have to break apart the stools and examine closely to see undigested material.
Some Causes of Malabsorption
• Celiac disease. Interestingly, diagnoses of microscopic colitis is higher in the celiac population than in the general population, but no causative link between celiac disease and microscopic colitis has been identified.
It may simply be that having one autoimmune disease (celiac) raises the risk of developing another at some point in time (e.g., microscopic colitis).
• Severe pancreatic insufficiency
• Cirrhosis of the liver (caused by excessive alcohol intake)
• Gastroenteritis
• Lactase deficiency
• Abnormal motility due to diabetes or thyroid disorder
• Acute intestinal infection
• Crohn’s disease
There’s quite a few other causes of malabsorption, but rest assured, none of them are microscopic colitis.
 Dr. Hagan is dedicated to collaborating with IBD specialists to discuss and explore advanced treatment options for the most complex inflammatory bowel disease cases.
Dr. Hagan is dedicated to collaborating with IBD specialists to discuss and explore advanced treatment options for the most complex inflammatory bowel disease cases.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Simon Kadula
Acid Reflux vs. Esophageal Spasms vs. Hiatal Hernia
Do symptoms of acid reflux, esophageal spasms and hiatal hernia really overlap that much?
“There is a continuum of disorders that can affect the esophagus,” says gastroenterologist Larry Good, MD, who’s been in practice for 40+ years; has a private practice in Lynbrook, NY; and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
Dr. Good continues, “Patients often equate the presence of a hiatal hernia, the herniation of the stomach above the diaphragm, with GERD. This is not true.
“About a third of adults have a hiatal hernia and the vast majority of these patients do not have symptomatic heartburn.
“Adding obesity, diabetes mellitus and delayed gastric emptying to the presence of a hiatal hernia is a good recipe for heartburn.
“Symptomatic acid reflux occurs when the esophageal lining or mucosa becomes inflamed.
“The esophagus is lined with stratified squamous epithelium, so it is exactly like the skin. Imagine how your skin would react to being exposed continuously to hydrochloride acid!”
What really causes heartburn?
Dr. Gordon says, “Physicians have always believed that heartburn was primarily caused by acid injury to the esophagus.
“Medication [such as with PPI pills] is extremely effective in treating heartburn and in allowing inflamed esophageal mucosa to heal.
“There is, however, some recent evidence that this simple explanation for heartburn may not be entirely accurate.
“An allergic response to certain foods (unrelated to the typical food triggers for heartburn) may generate an inflammatory reaction in the esophagus called eosinophilic esophagitis, and that may presage many episodes of reflux esophagitis.
“Gastroenterologists are now seeing many patients with eosinophilic esophagitis and are studying the links between these conditions.”
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com
Why Does Heartburn Come and Go?
If you suffer from heartburn that comes and goes without any apparent cause, you should keep track of what you eat.
This tracking includes how much you eat and when, since food may very well be the trigger of your acid reflux.
“Classically, certain foods trigger reflux and symptomatic heartburn,” points out Gastroenterologist Larry Good, MD, who’s been practicing for 40+ years, with a private practice in Lynbrook, NY; and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
Types of Food that Can Make Heartburn Come and Go
Dr. Good says, “Fatty and fried foods, carbonated beverages, chocolate, mints and onions are typical triggers.
“Alcohol and caffeine are also frequent culprits.
“It takes about 90 minutes for the stomach to empty completely, so very large meals, especially if they contain the foods listed, taken just before bed will often precipitate nocturnal heartburn.
“Acidic foods like citrus juices can also provoke symptoms, especially if the esophagus is inflamed.”
Another reason for heartburn to come and go is when it’s being triggered by anxiety and stress.
Anxiety and stress, much like food consumption, can fluctuate throughout the day.
Their intermittent nature can be influenced by various factors, such as the occurrence of stressful events or changes in the individual’s mental state.
For instance, someone might experience heightened anxiety during a particularly stressful period at work or while facing personal challenges.
A particularly troublesome scenario arises when the physical symptoms of stress and anxiety, such as chest discomfort or heartburn from acid reflux, are exacerbated by both food intake and emotional strain.
This creates a double burden: the distressing physical sensations from acid reflux, which can be triggered or worsened by certain foods, and the additional strain from stress, which can also contribute to or intensify these symptoms.
In such cases, managing both the psychological and physiological aspects becomes crucial to alleviate discomfort and improve overall well-being.
Imagine what might happen if a person who’s prone to heartburn turns to reflux-triggering foods to deal with stress or anxiety!

Shutterstock/Hurst Photo
Eating a big piece of emotionally-soothing chocolate cake right before bedtime is the last thing a person with acid reflux problems needs to do.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Thomas Foldes
HOW Does Lexapro Trigger GERD?
Lexapro can trigger GERD, but just how does this happen?
Lexapro is an antidepressant drug, but it can also help reduce anxiety.
It belongs to a class of drugs called selective serotonin reuptake inhibitors (SSRIs).
Among the possible side effects to taking Lexapro is that of gastroesophageal reflux disease.
How Lexapro Leads to GERD
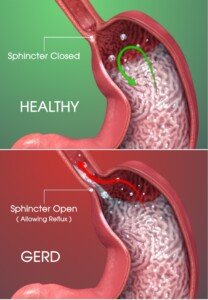
“Lexapro and other antidepressants can relax the lower esophageal sphincter and promote heartburn,” explains Larry Good, MD, a gastroenterologist who’s been in practice for 40+ years; has a private practice in Lynbrook, NY; and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
Dr. Good continues, “Many medications can have similar effects, and doctors should take a very careful medication history when evaluating patients with heartburn.”
Since Lexapro can relax the lower esophageal sphincter, there is something that you can do to help manage the acid reflux — at least overnight.
Scientific Animations, CC/BY-SA/Attribution-ShareAlike 4.0 International
Relief for Acid Reflux from Lexapro
When you’re lying in your bed, with your body horizontal, the sphincter becomes more relaxed.
Gravity’s vertical effect is not present to help keep the stomach’s acidic juices contained where they belong: in the stomach.
So while you’re asleep, the acid refluxes upward, getting past that weakened sphincter, and makes its way up the esophagus.
It may even reach the throat, causing throat related symptoms when you awaken: a bitter or unpleasant taste in your mouth; a cough; a scratchy throat; a hoarse voice.
Drinking water won’t help because the problem is that your vocal cords have been contacted by acid reflux.
The water will go down the esophagus, not having any effect on the vocal cords.
What you can do is prop your torso up a bit to bring some gravity into the equation.
Do not eat within three hours of bedtime, since eating close to bedtime can contribute to overnight acid reflux.
For daytime management, avoid foods that give you heartburn, and avoid eating a lot of food at one sitting.
If the GERD from Lexapro cannot be managed with these natural approaches, do not quit taking this antidepressant unless your doctor gives you instructions to do so.
Your doctor may also prescribe a drug to help control the acid reflux.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Esophagitis Cause of Chest Pain vs. Heart Attack

Uh oh, chest pain from heart attack vs. esophagitis can be “very difficult to distinguish,” says a gastroenterologist.
“Esophagitis, inflammation of the esophagus, can cause severe chest pain,” says Gastroenterologist Larry Good, MD, in practice for 40+ years and with a private practice in Lynbrook, NY, and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
Why can the severe chest pain of esophagitis mimic that of a heart attack?
Dr. Good explains, “The esophagus, heart and airways are all served by the vagus nerve which can send signals to the brain from these organs.
“This is called six dermatone pain, corresponding to the sensory innervation of the organs in the chest cavity.
“Because of this, it can be very difficult to distinguish between pain that derives from the heart, the esophagus and the lungs.”
Wow, that’s scary. You’d think that nature would have devised a way for the brain to tell the difference, to be able to interpret pain signals unique to the heart, to the esophagus and to the lungs.
Instead, chest pain from esophagitis and the heart (and lungs) can feel the same across the board.
What makes this more frightening is when patients know that there’s no reason for them to have a low risk of heart attack.
You don’t have a low risk for heart attack if any of the following apply to you:
You lead a sedentary lifestyle. You’re obese. You smoke. You have diabetes. Your diet is mostly ultra-processed foods, even if you’re not overweight.
You have untreated sleep apnea. You have uncontrolled high blood pressure.
So when that chest pain strikes — which may actually be esophagitis in that person — they fear the worst. So what should you do?
How about getting a complete cardiology exam…before your next or first incidence of unexplained chest pain? See what a cardiologist says about your heart. If you have chest pain history, also see a gastroenterologist to discuss esophagitis.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/ PrinceOfLove
Can GERD Breathing Problems Suffocate You to Death?

GERD breathing problems can lead to feelings of suffocation and serious lung issues.
Ever feel that the breathing problems from GERD could suffocate you to death?
Sorry to say, but the very medical condition that is so often presented with amusement in TV commercials can actually cause very serious problems involving breathing that, if not managed properly, can be life-threatening.
This doesn’t mean that every time you develop heartburn or some other milder symptom of GERD, you should panic and grab the phone in preparation of dialing 9-1-1.
But a chronic GERD sufferer needs to be well-aware of just what acid reflux disease is capable of.
Many patients already know that acid reflux can reach the throat, causing breathing problems—and in some cases, a suffocating feeling.
“The most feared complication of esophageal problems is aspiration, the passage of gastric contents into the lungs,” begins Larry Good, MD, a gastroenterologist who’s been in practice for 40+ years, with a private practice in Lynbrook, NY, and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
Dr. Good explains, “This can cause severe lung injury. Severe, chronic reflux can cause a variety of upper airway and lung problems including sore throat, hoarse voice, voice fatigue, laryngeal injury, cough, pneumonia and lung abscess.
“These can contribute to many breathing problems including asthma and worsening of COPD.”
COPD is not actually caused by GERD, but what Dr. Good is saying is that severe, chronic reflux can aggravate pre-existing chronic obstructive pulmonary disease.
If you’re familiar with “LPR” – laryngopharyngeal reflux – then you know that the sensation of difficulty breathing can be a symptom.
However, you won’t literally suffocate to death right on the spot from LPR or from the GERD that affects structures below the throat.
So despite all the serious possible fallouts of GERD, such as a lung abscess or pneumonia, it’s not something that’s going to one day strangle and suffocate you while you’re sleeping or eating and kill you right then and there.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: George Rudy
Can Lifting Free Weights Cause GERD?

Lifting free weights CAN cause GERD, but wait till you learn which particular weightlifting exercises can especially do this!
Lifting weights, of all things, can actually bring on GERD, which stands for gastroesophageal reflux disease, also called “heartburn” in layman’s terms.
“The pathophysiology of GERD is a complex relationship between gastric contents, gastric emptying, lower esophageal sphincter [LES] pressure and esophageal mucosal resistance to acid and other irritants,” explains Gastroenterologist Larry Good, MD, who’s been practicing for 40+ years, with a private practice in Lynbrook, NY; and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
How can lifting free weights cause GERD?
“The essential requirement for GERD to occur is for intragastric pressure to exceed LES pressure,” continues Dr. Good.
“Therefore, anything that increases intragastric pressure will cause reflux of gastric contents into the esophagus. Straining of any kind will contribute to GERD.
“For example, squats or standing military presses with free weights dramatically increase intra-abdominal pressure and can worsen symptoms of GERD. Bench pressing, on the other hand, will not.
“Likewise, exercises that lower the head below the level of the abdomen can precipitate reflux symptoms or even regurgitation of gastric contents, because the force of gravity can exceed the resting LES pressure.”
Weightlifting moves in which the head is lower than the abdomen include inverted rows (if the feet are propped high enough) and elevated-foot pushups.
“Obese individuals are particularly susceptible,” says Dr. Good, to GERD being caused or aggravated by lifting weights—when they perform the particular movements that can bring on the symptoms such as squats and standing overhead presses.
Does this mean give up the very weightlifting moves that trigger your GERD?
Keep doing them if they are important for your fitness and physique goals. Nobody ever got sick from weightlifting-induced acid reflux.
But you should avoid other triggers for GERD such as liquor, caffeine and spicy foods. And don’t go overboard on the post-workout meal.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com Racool_studio
What Should Diabetics Eat After Strength Training?

With all the advice out there on what to eat after strength training, what should diabetics eat?
“Post-workout refueling wouldn’t be much different from someone who doesn’t have diabetes,” says Alison Massey, MS, RD, LDN, registered dietitian and certified diabetes educator with over 10 years of experience in various community and clinical settings.
That’s very interesting, because there’s a lot of disagreement among fitness experts, nutritionists, dieticians, competitive physique athletes, exercise physiologists and medical doctors about just what a person should eat following a session of strength training.
Certainly, the intensity (or lack thereof) of a strength training session would factor into just what you should eat afterwards.
For instance, a meal following 90 minutes of brutal weightlifting would need to be bigger than the meal that’s required to subsidize a 45 minute, medium-force workout.
Massey advises diabetics to monitor their glucose during a strength training session and after.
A low reading mid-workout, for example, will necessitate consumption of a quick-acting carbohydrate like juice or candy.
Carbohydrates should be eaten soon after strength training, whether you’re diabetic or not.
With the carbohydrates should be a clean source of protein (e.g., tuna salad or whole chicken, not deli meat).

The carb source should be healthy, too (whole potato, brown rice, quinoa, and if you must have bread, make it whole grain—and the fewer the ingredients, the better).
The muscle building community recommends 20-35 grams of protein following strength training, but again, this is controversial and depends on multiple variables such as the individual’s goals, intensity and how much muscle they want to gain (or maintain).
Massey says that low fat milk can be part of a post-workout meal for diabetics. In fact, studies support milk as a good post-workout beverage.
Though milk is low in carbs, it’s “insulinogenic,” meaning, it promotes the process of insulin shuttling blood sugar (from eaten carbs) to insulin receptor sites on muscle cells.

















































