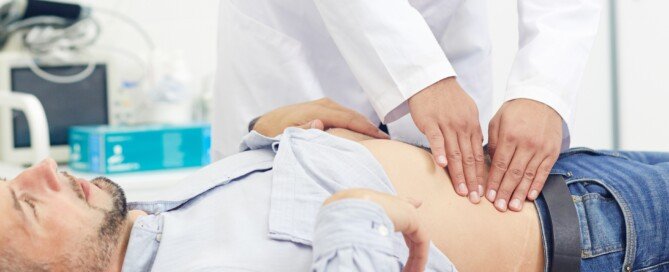
Do Asymmetrical Legs Mean ALS?

Are you panicking about ALS because your legs are uneven or not symmetrical?
The body is NOT symmetrical. This applies to more than shape and muscles. Examine the moles on your lower leg.
Do you have the exact same pattern of moles on your other leg? One calf is probably bigger than the other, too.
Gee, I see this ALL the time in someone walking ahead of me wearing shorts.
Like you have a dominant arm, you also have a dominant leg. There is no reason to worry about ALS.
The dominant leg may have more dents in the calf, reflecting slightly more toned muscles and/or less fat (not atrophy!).
As a former personal trainer, I’d see this all the time in my clients as well as other gym patrons.
If your less dominant calf has more dents, this does not mean muscle atrophy.
Don’t panic over ALS. It means natural asymmetry, which may be the result of maybe a little less fat there.
(The less fat between skin and muscle, the more muscle definition you’ll have.)
Assurance if You’re Worried About ALS
“Mild muscle asymmetry is usually not of concern, especially without associated weakness,” says John Whyte, MD, board certified internist in Washington, DC, and author of “Is This Normal? The Essential Guide to Middle Age and Beyond.”
Or maybe your “non-dominant” leg is more dominant than you think!
For example, suppose your right leg is stronger than your left, as far as push-power.
This, however, does not mean that your left leg can’t be superior in some other aspect, such as balancing on one foot or taking off in a leap.

Freepik.com;yanalya
“Our bodies are not bilaterally symmetrical,” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
He continues, “An old trick from the pre-Photoshop days was to take a straight-on photograph of someone’s face, cut it down the middle, reverse one side and put the two versions of one side together, producing an image which did not resemble the original person. Even identical twins have subtle differences.”
Though Dr. Leavey references the face here, keep in mind that the face is full of muscles.
He adds, “If you are right handed, your right arm will be a bit more developed from the increased use over years. Similar changes are in the legs.”
If you’ve been panicking over ALS, you may want to monitor your blood pressure, as anxiety can raise it.

Dr. Whyte is the chief medical officer of webmd.com. Prior, he was the chief medical expert for almost a decade at Discovery Channel.

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Source: webmd.com/brain/tc/amyotrophic-lateral-sclerosis-als-topic-overview?page=2
Sleep Paralysis Following Lucid Dreams: Why I Embrace This

I’ve never understood why sleep paralysis scares so many people and why they say they “suffer” from it.
Since childhood (though I can’t pinpoint if it was grade school or junior high), I’ve experienced sleep paralysis. Note that I say “experienced” rather than “suffer.”
However, why is it that when I experience sleep paralysis…every single time without fail…it follows a lucid flight dream?
Every single time. Now this doesn’t mean that every single time I have a lucid flight dream, I enter into sleep paralysis. But it’s the other way around.
The paranormal explanation is that the lucid flight dream is not an actual REM stage dream at all, but an out-of-body experience (astral projection).
Paranormal enthusiasts would explain that the sleep paralysis that follows is that of my astral body returning to my physical body.
It takes a few minutes for the “fit” to complete, and hence, the sleep paralysis. Hmmm.
I can pop in and out of sleep paralysis during a brief time window that follows the first episode. I’ve always enjoyed tinkering around with it.
There’ve been times when it felt as though the upper half of my body was inside my body, but my legs were sticking outside my body.
There’ve also been times that it felt that I was hovering horizontally five feet above my body, but every time I’ve opened my eyes, I was inside my body.
As for opening my eyes…I’m able to do this during sleep paralysis, but only for several moments; they become too heavy to keep open.
How I Know I’m Not Dreaming About Sleep Paralysis
I know I’m not dreaming these experiences because I’ve verified them by noting the precise configuration of bed sheet wrinkles and the position of my arm and hand.
When I pop out of the sleep paralysis and open my eyes…everything appears as it had during the paralysis.
This also goes for the exact time. For example, I might note it’s 8:02 a.m. during an episode of sleep paralysis. When it concludes and I open my eyes, it’s 8:03 or 8:04.
When I’m in sleep paralysis, I try to astral project, and thus far, have not succeeded, though I still seriously wonder if the lucid flight dreams are actual out-of-body excursions.
Astral Projection
What makes these “dreams” highly suspect for astral projections are the following key features:
#1. The flights are amazingly vivid and realistic, as though they are actually happening. I swear, I know exactly what it feels like to fly above a canyon or mountain range.
#2. In almost every flight dream, there are no other people present. It’s just me and the beautiful nature I’m flying over. Why aren’t there any characters in these dreams?
In my non-lucid dreams or lucid non-flight dreams, there are always other characters involved. Funny how they’re almost always absent in the lucid flight dreams.
#3. While I’m having a lucid flight dream, I can induce sleep paralysis. I can’t explain how I do it, but I just do it.
#4. If I’m having a lucid non-flight dream, I never think of inducing sleep paralysis. The phenomenon is the farthest thing from my mind. Instead, I’m caught up with the story in the dream, no matter how bizarre it is.
This suggests that the lucid flight dream is, in fact, an out-of-body experience, during which my mental faculties are NOT muddled by the dream state.
Once I’m in sleep paralysis, I cannot get back into the dream, but when the sleep paralysis wears off, I can pop back into the paralysis as long as I attempt that within a few moments.
Otherwise, if I wait too long, the opportunity expires and I’m fully awake.
Are there elements of lucid flight dreams that suggest they’re just dreams?
#1. It’s always daylight, even though sometimes when I have these experiences, it’s in the middle of the night when it’s dark (unless my out-of-body episodes somehow always end up in a distant time zone?).
#2. Sometimes interaction with characters precedes the flight, even though once I’m in flight, no characters exist 99 percent of the time.
There have been lucid flight dreams in which, while I was airborne, I did see people on the ground (though this is very rare).
So if this is an astral projection…who were those characters? They certainly didn’t come across as spirits—just run-of-the-mill dream characters.
#3. If these are out-of-body experiences, why is the part when I’m leaving my body and viewing it in my bed bypassed?
In other words, the astral projection involves teleportation rather than manual exiting of my body.
All that being said, I enjoy sleep paralysis and you should too. It’s cool and far out!
If you’re scared of sleep paralysis, ask your doctor if this is a symptom of a medical condition.
If sleep paralysis continues to frighten you, take better care of your body. If you have a fit, strong body, you’ll be less likely to fear having a disease that causes paralysis.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Minoxidil 5 Percent Stains Hair Gray: Solutions
It’s not your imagination; minoxidil 5 percent can stain your hair gray.
Based on my experience, the 5 percent minoxidil solution “turns” whatever hair it comes in contact with a grayish color.
The new hairs that have come in are my natural color, so I’m not saying that this drug makes the regrowth gray.
And the “gray” isn’t the same as a true gray hair. It’s some kind of staining that’s not well-documented in the medical literature.
A good shampoo gets rid of most of it, but it will return if you keep using the 5 percent solution—at least in my case, this is what happened.
My hairdresser thought I had gray hairs coming in; she seemed skeptical when I told her it was the 5 percent minoxidil.
I’ve been using the drug on my temples where there’s been some hair loss, and I must say, the new hair is coming in wonderfully. I have my solid hairline back.
The fix for the staining problem was for me to stop using the 5 percent so much and rely more on the 2 percent.
Even though the 5 percent is marketed towards men, there’s no reason why women can’t use it.
But it does come with more potential side effects.
In my case it was the gray staining, but also aggravating itching. The 2 percent solved the staining problem outright and doesn’t itch as much.
And by the way, sponging the gray area with water will not get rid of it.
You may want to use the 5 percent to kick start the regrowth, but then once the regrowth occurs, use the 2 percent for maintenance.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
ALS Anxiety, Muscle Atrophy and Twitching Conquering This Stress

Constant muscle atrophy checking is a common experience with people who are plagued by an obsession they might have ALS, a deadly, incurable disease that results in muscle atrophy.
ALS is very rare, striking about 5,600 Americans yearly, so why would anyone be consumed by fear of ALS and perform constant muscle atrophy checks?
If you found this article, you know exactly why, so I’ll cut to the chase.
Once you reach a point where you are constantly checking the suspect body part in the mirror or without a mirror, for signs of muscle atrophy, your mind must be retrained or reprogrammed.
This will not occur overnight, but it CAN be accomplished. Checking for muscle atrophy often takes place in front of a mirror.
But often, sufferers will do this without a mirror if the suspect area is on a hand, foot or calf.
The first step in overcoming the compulsion to continuously check for muscle atrophy is to realize that the body is not symmetrical.

Check out the benign asymmetry in this woman’s upper arms. Freepik.com, drobotdean
The body is not symmetrical.
Your dominant arm, especially its upper part, will almost always appear bigger than the non-dominant arm.
This is how you should think, rather than, “Why does my non-dominant arm appear smaller than my dominant arm?”
The more you perform muscle atrophy checks, the more apparent muscle atrophy you will find.
You know that old saying? “If you look hard enough for something, you’ll find it”?
Think way back, perhaps during childhood, when you just happened to realize that one side of your body did not look like the other.
What happened after that? Did you panic? Did you obsess and spend huge amounts of time every day checking for muscle atrophy?
Or did you think nothing of it after one and a half seconds?
So what’s different NOW?
“Our bodies are not bilaterally symmetrical,” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
“An old trick from the pre-Photoshop days was to take a straight-on photograph of someone’s face, cut it down the middle, reverse one side and put the two versions of one side together, producing an image which did not resemble the original person.
“With computer graphics you can do this, which used to take hours, in seconds.
“Even identical twins have subtle differences. If you are right handed, your right arm will be a bit more developed from the increased use over years.
“Similar changes are in the legs, where you may be ‘right legged’ or ‘left legged.’ We are not ‘cookie cutter.’ Deal with it.”
Even bodybuilders and physique athletes, who fight for “perfect symmetry” for their posing routines, often can’t nail it.

More asymmetry
At first glance the bodybuilder above seems to be perfectly symmetrical. But keep looking.
His right arm (or left from your view) has a dent just below the insertion point of the deltoid, midway between the biceps and triceps. No such dent is visible on his left arm.
A bulge appears above his right armpit that’s absent above the left.
Note the dent under his left collarbone. It’s missing on the right side.
To someone with health anxiety, this man might have ALS. But he’s a strong, fit bodybuilder!
Every time you enter your bathroom to relieve yourself, brush your teeth, even comb your hair, do NOT turn on the light.
Flipping on the light will encourage checking for muscle atrophy.
Always wear socks to discourage checking feet for muscle atrophy.
If you start spotting “dents” in the suspect area, ask yourself where on earth you got the idea that “dents” are a sign of ALS.

Engaging the quad muscles brings out the “dents.” Shutterstock/Jasminko Ibrakovic
Panic over dents is quite common in people who spend inordinate amounts of time performing muscle atrophy checks, yet, where in the ALS literature does it state that dents are a symptom of ALS?
Nevertheless, there is an explanation for dents: not enough body fat to conceal muscle topography!
Open a bodybuilding magazine. You’ll see tons of dents in the athletes because they hardly have any body fat between the muscles and skin.
They are dent city. Think of dents as muscle definition. Isn’t that what everyone wants? Some nice definition?
A person’s six-pack abs are full of dents! Dents are good!
Keep reminding yourself that NOWHERE in the annals of medicine does it state that the human body is supposed to be symmetrical.
Check for muscle atrophy on other people. You’ll find it everywhere and on everyone:
Check the bare legs of someone walking ahead of you. One calf is almost always bigger.
Or one thigh might be a little more curved.
One hip might be a little higher.
Check another person’s arms. You’ll see lack of symmetry there, too.
It is perfectly normal for one foot to be bigger than the other! In fact, I asked a podiatrist (physician who specializes in foot/ankle/lower extremity conditions) about this.
“In regards to patients who present to my office with a foot problem that only affects one foot, it is not uncommon to find that one foot is a different size,” says Alan L. Bass, DPM, Medical Director, NEMO Capital Partners, LLC.
“Many times problems such as plantar fasciitis, forefoot pain, jamming of the joints of the foot is caused by improper shoe gear due to the fact that the patient is wearing a pair of shoes of one size, but one of the foot is a different size, either length and width,” explains Dr. Bass.
 Dr. Bass is with Central Jersey Foot & Ankle Care, and is a Fellow of the American College of Foot and Ankle Orthopedics and Medicine. basspodiatry.com/our-foot-doctor
Dr. Bass is with Central Jersey Foot & Ankle Care, and is a Fellow of the American College of Foot and Ankle Orthopedics and Medicine. basspodiatry.com/our-foot-doctor

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Frank11
Muscle Twitching: Is It ALS, Anxiety or BFS? Best Information!
Is Twitching More Likely ALS just Because a WHOLE Toe Jerks?
The Kind of Woman a Controlling Man Wants

A control freak man who’s prone to violence wants only a certain kind of female victim.
Men who are capable of physically or even just emotionally abusing a girlfriend or wife are on the lookout for certain kinds of women to fit this bill.
Men of all types look for certain kinds of women. Violent or physically aggressive men are no exception to this rule.
And likewise, women seek out certain traits in men, the kind of men they feel would be a nice match for them.
Fact is, women have been long stereotyped as being “picky” when it comes to men.
So why wouldn’t an abusive man also have certain requirements, even the “picky” requirements, for his choice of women?
It only makes some sense that a controlling man seeks out specific traits in his women, traits he believes would fit him well.
“I equate these predators to a lion,” points out Mary Jo Fay, RN, MSN, and author of When Your Perfect Partner Goes Perfectly Wrong.
She says, “The lion doesn’t look at a herd of antelope and say, ‘Gee, I should stick to killing off just the old ones.”
Fay continues, from the instinct of the lion, “The babies just started their lives… so I’ll leave them alone.’ The lion just knows he’s hungry and knows that the weakest victim will yield the easiest lunch. Whether that’s the oldest one close by, the baby close by,” etc.
“It’s almost instinctual. He certainly knows not to go after that lead ram … too risky. He might get hurt.”
Cruel men are not superhuman.
They can indeed be intimidated. Fay remarks, “So in the human world, the predator seeks the vulnerable, low self-esteem woman.” This is the woman “who seems to be the caretaker in a crowd.
Caretakers are usually hoping to win approval by pleasing others,” but they just don’t know how to win their own approval. They are the quieter types.
“Predators can smell out the high self-esteem women,” says Fay, “and recognize them as too much work from the get-go.”
How can the self-esteem in a woman be measured?

Certainly it’s not by her job. We can’t equate high self-esteem with her career success, even though it intuitively seems that high self-esteem should be a requirement for career success.
But it’s not. The fact that battered women represent all the educational, occupational and socioeconomic levels contributes to the belief that “any” woman can get trapped with an abusive man.
A major myth is that most abused women are poorly educated and not too intelligent, and have little means.
“As to smart businesswomen getting suckered into this,” says Fay, “these women may feel as though they are good at their profession, but are not great socialites, and not great daters, not very attractive, etc.
“So they, too, struggle with self-esteem issues, although they may be the CFO of a multi-million dollar company.”
Fay adds that “running a big business may not require them to be up-close and personal with someone … so it can be easy to hide behind business plans and quarterly reports.”
In short, “Your job and your personal life can be two very different things!”
While some abusive men go after women in a more instinctive way, other abusive-prone men deliberately feel women out as their potential girlfriends.
- Have you yourself ever met a man who behaved towards you in a peculiar way?
- Perhaps this guy was testing you out.
“I once heard a con man interviewed on the radio,” begins Tina B. Tessina, PhD, a psychotherapist who counsels couples and individuals, and author of The 10 Smartest Decisions a Woman Can Make Before 40.
She explains, “He said he offered prospective victims a stick of gum; he could tell by the way they accepted or refused whether they’d fall for his con. I believe that is the majority stance of abusers.
“They look for a woman they believe they’ll easily intimidate, who will easily fall into the pattern of him being in charge.”
Dr. Tessina adds, “Women who are successful in business can still have a dependent idea of what romance and relationships are.” Yes.
“Even a successful woman can have a low opinion of her loveability,” says Dr. Tessina, “which makes her susceptible to the charm of a man who’ll tell her what she wants to hear.”
 Dr. Tessina appears frequently on radio, TV, video and podcasts, and has been in private practice for over 30 years.
Dr. Tessina appears frequently on radio, TV, video and podcasts, and has been in private practice for over 30 years.
 Mary Jo Fay is a speaker, author and consultant who specializes in relationships.
Mary Jo Fay is a speaker, author and consultant who specializes in relationships.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Sjstudio6
Can a Gallbladder Polyp Turn Into Cancer?
There are different kinds of gallbladder polyps and this includes cancer.
So if it’s been discovered that you have a polyp in your gallbladder, should you panic and assume that it’s cancer?
Will the mass eventually transform into a malignancy?
There are no grounds for panicking or making this assumption, as there are several types of polyps associated with this organ.
A Polyp Was just Discovered in Your Gallbladder
“Gallbladder polyps are outgrowths of the gallbladder mucosal wall that are usually found incidentally on ultrasonography or after cholecystectomy,” says Akram Alashari, MD, a trauma surgeon at Geisinger Medical Center in PA, and author of “THE POWER OF PEAK STATE.”
Two Classes of Gallbladder Polyps
“They are classified as benign or malignant, and benign lesions are further classified as non-neoplastic (e.g., cholesterol and inflammatory polyps, adenomyomas) or neoplastic (e.g., adenomas, leiomyomas),” says Dr. Alashari.
Don’t be unnerved by the “oma” suffix here. “Oma” is the medical term for mass—but the mass can be benign.
“The most common benign neoplastic lesion is an adenoma, a glandular tumor composed of cells resembling biliary tract epithelium.
“It is unclear whether adenomatous polyps represent a premalignant lesion and if so, the frequency with which they progress to carcinoma.”
Cancer-related molecular changes that are seen in gallbladder cancers have not been identified in adenomas.
“Nevertheless, larger polyps are more likely to contain foci of invasive cancer, and some studies suggest a correlation between the presence of gallbladder polyps and the risk of gallbladder cancer.”
Symptoms of Gallbladder Cancer
- Abdominal pain, especially in the upper right region
- Abdominal bloating
- Fever
- Nausea
- Weight loss that is not intentional or explainable
- Yellowing of the whites of the eyes or the skin (jaundice)
Risk factors for this disease include aging, female gender and a history of gallstones.
However, the disease is still rare in people who’ve had gallstones.
Another risk factor is infection of this organ.
Gallbladder cancer is a rare condition. The occurrence in the U.S. is 12.3 per 100,000 men and 27.3 per 100,000 women.

Dr. Alashari was formerly with Grand Strand Regional Medical Center in SC as an abdominal and critical care surgeon.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Pressmaster
Lower Stomach Pain from Running Could Be Serious

The pain you experience in the lower abdomen from running is probably harmless, but you may also consider seeing a doctor about it.
“Lower left, or lower right for that matter, pain can be from something as typical as a muscle ‘stitch,’” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
What is the runner’s stitch?
Dr. Leavey explains, “This is a muscle cramp of the abdominal muscles caused by vigorous exercise without good preparation.
“Dropping back to a slower rate, exercising the area, and being sure that you are in good condition and well-hydrated are mainstays of preventing this issue.”
Drink water before you go on your run, as this will help prevent the pain in the lower abdomen. Even if you’re not thirsty, drink that water.
Don’t wait till the cramp comes on to do it. If the lower stomach pain occurs while you’re running, slow to a walk and take out the water, warming down with the walk, then stop and drink up.
Other Possible Causes of Lower Stomach Pain when Running
“However, there are a plethora of issues that can arise apart from this which can cause very similar pains,” says Dr. Leavey.
“Abdominal or inguinal hernias, issues with the intestines or GI tract, and gynecologic problems can also cause pain with running, often indistinguishable from a simple stitch.
“So, if you are having pain, and it does not easily resolve, or if there are any questions at all, you really should see your physician to be sure that nothing serious is going on.”
Women should head first to their gynecologist, even though it may seem logical to head first to the gastroenterologist.
A serious problem with the ovaries could cause pain in the lower abdomen that may become more apparent when running.
A transvaginal ultrasound will give an OBGYN a good view of the ovaries.

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Nausea, Puking from Lifting Weights: Advice from Doctor

Here’s what a doctor advises if you suffer from nausea and vomiting from a weightlifting workout.
“A major cause of nausea and vomiting with weightlifting is doing too much, too quickly, without adequate preparation,” begins Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
“While you should be well-nourished and well-hydrated before vigorous exercise, you need time to digest the food, and let the majority of it leave the stomach.
“Otherwise, that adrenaline rush that you get when you start an exercise set will do just what it does at other times, shut down digestion, divert blood to the arms and legs, and empty out the GI tract.”
Look at it this way: The body is hardwired to summon up certain biochemical responses to a perceived danger.
When you begin a hardcore weightlifting session, the body can’t tell if this is an encounter with a wild boar or a safe training routine inside a building. So the body starts gearing up for a fight or flee response.
To prepare for the fight or escape from danger (a physiological response that came in very handy during caveman times), the body empties the GI tract—you puke.
But why? So that the body could rid as much baggage as possible to be as efficient as possible during the fight or escape from “danger.”
This is why sometimes, a person will upchuck or at least suffer nausea simply upon viewing a grisly scene, such as the aftermath of a motorcycle accident.
Think of the contents of your gut as the equivalent of carrying a weighted rucksack. The rucksack would be a hindrance if you had to fight or run from danger.
So the body should shed it. Likewise, you vomit when faced with what the body perceives as a threat.
And let’s face it—a grueling set of deadlifts and squats could fool the body into thinking it’s time to dump the baggage.

Shutterstock/tankist276
Dr. Leavey explains, “Better to have a healthy meal, give time to digest, and start the routine a bit slower to allow the body to acclimate.
“Clearly, as you get more into exercising, this should become less of a problem, but early on it can be a limiting factor.”
Maybe you’ve read that prior to lifting weights you should ingest a good heap of protein. Give a bit more time between doing this and starting your working sets.
Also, as Dr. Leavey says, pay more attention to the warm-up. Don’t just dive into your maximal loads.
To further help prevent vomiting during or after a weightlifting routine, eat something at the 45 minute mark (and this time lapse excludes warming up).
It should be a combination of protein and quick-acting carbohydrates.
Another factor in the barfing up or at least feeling nauseous during weight training is that of having an untrained body, in combination with lack of nourishment.
When I used to be a personal trainer at a gym, the only clients of mine who ever experienced nausea and a little upchucking were not well-trained, and a few of them had not eaten much in the preceding hours.

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/iambasic_Studio
Benign Calf Dent or Muscle Atrophy: Your Last Article!

Here is your FINAL article on the calf dent that you think is a sign of ALS muscle atrophy.
Do calf dents have you terrified you have ALS because you think this is how muscle atrophy should look?
Finding this article means that you are most likely deep within the agony of ALS fear originating from twitching muscles and/or dents in your legs.
You’ve been spending an lot of time inspecting your legs, particularly calves, for muscle atrophy.
Muscle twitching aside, you have discovered dents in one of your calves, or maybe just one dent there, and are wondering why the other calf doesn’t have the same dent or groove.

Could this be a sign of muscle atrophy in the “odd” calf that has the dent?
“No, no, and no,” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
Dr. Leavey continues, “The dents are the definition from the hypertrophied muscles.”
Hypertrophy means the opposite of atrophy: muscle enlargement. If you’re into physique development, you’ll want dents.
You’ll know that these are the result of developed or trained muscle in combination with low body fat in that area.
Have you ever seen a person who has atrophied legs for real?
This would be someone who’s been paralyzed for so long that their muscles have wasted away.
Ever see them in shorts? No dents. That’s because the muscles have become putty.
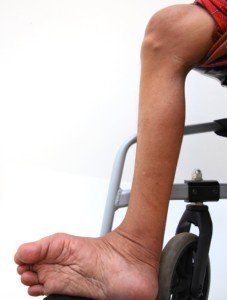
This atrophied leg is smooth and dent-free. Shutterstock/podsy
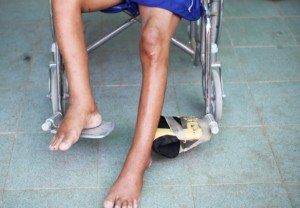
Muscle atrophy but no grooves. Shutterstock/Somchai photo
Dr. Leavey says, “Someone in a wheelchair with paralyzed legs has nice, smooth, albeit useless, legs.” Yes, “smooth.”
What’s really happening is that your mind is playing tricks on you, all because you probably googled muscle twitching.
Though muscle atrophy is the result of ALS, a dent in a calf is not a hallmark sign of muscle atrophy.
Let’s go more extreme about this: bodybuilding. “Bodybuilders build muscles, and those muscles produce the physique and definition that is sought,” says Dr. Leavey.
“If you tried to build a clay model of a lower leg, making each muscle the desired size and shape, you would see that there are grooves and separations between these well-developed muscles.
“It is that very desired result that produces the dents that are seen in such individuals.”
But what if you’re not a bodybuilder?
“Whether bodybuilder or not, we all have the same muscles, in the same places,” says Dr. Leavey.
“Some are just shapelier than others. That means that a well-developed calf muscle may show good definition in a non-bodybuilder, yielding the same dent as the more active individual.
“Perhaps walking on stiletto heels caused a particular muscle to hypertrophy.
“For the most part, such muscle definition yielding ‘dents’ is not pathological.
“If there are any doubts, or if a change develops acutely, though, you should seek medical attention.”
I used to be a certified personal trainer for a major health club chain.
So I know a lot about muscles and body composition.
If you’ve lost body fat recently, and especially if you’ve been exercising more, and you’ve been noticing the development of a dent or two in your calves…this is the result of the fat loss and exercise!
Less fat between your skin and muscles, and firmer, more trained muscles mean increased definition, a.k.a. dents!
Stop worrying! It’s not atrophy! It’s not muscle wasting – it’s muscle growth!
Here is how this whole frightening process develops:
Your lower leg muscle begins twitching. You google this. On the first page of search results are links to ALS information.
Panic ensues. The twitching “spreads.” You read about muscle weakness and atrophy. You begin examining your legs.
Invariably, you discover dents that you swear were never there before.
Your mind begins playing tricks on you. New dents appear overnight.
From a Fitness Expert:
Listen to me: Calf dents are normal. It’s called muscle definition.
If you don’t believe me, open a fitness or bodybuilding magazine and look at the legs. They are full of dents.
In fact, check out magazines on running or soccer. People with low body fat, and especially with toned muscles from running, athletics or weight exercises, will have lower leg dents.
Bodybuilders, physique and figure competitors strive for calf dents as well as grooves everywhere else.

How many dents or grooves can you count in this bodybuilder? Shutterstock/Jasminko Ibrakovic
In fact, their jargon for calf dents is striations, cuts and rips. I’ve had personal training clients who, upon discovering dents in their legs and arms, became ecstatic and pointed them out to me:
“Look! I never had this before!” IT’S MUSCLE DEFINITION.
And in your case, you just never noticed it before. Muscle definition fluctuates.
So even if you know you never had a calf dent before, this is no cause for alarm.
Because muscle definition is variable over time, due to fluctuating eating habits, fluctuating exercise habits, and other factors that affect body composition and appearance — including water retention.
If you want to know what muscle atrophy REALLY looks like, look at the legs of someone in a wheelchair.
If anything, their atrophied calves had NO dents! Atrophied muscle that has turned flaccid and limp is dentless, because it’s not firm enough to show definition.
Anxiety causes twitching to rapidly spread, and it causes you to discover things that have always been there. So re-read this article!

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Top image: Shutterstock/Joaquin Corbalan P
A Woman’s Ribs Showing Doesn’t Mean She’s Too Thin!
Here is why you shouldn’t assume a woman is unhealthy or too skinny just because her ribs show.
Many women have ribs that show. Some are undernourished, weak and unhealthy, while others can deadlift 250 pounds, knock off pushups, have all the energy in the world and never feel sick.
As a fitness expert and former personal trainer, I’m going to give you my perspective, and then I’ll give you the perspective from an internal medicine doctor whom I interviewed for this article.
If you don’t believe that feats of strength and endurance don’t indicate one’s health status, then consider this:
Many women with visible ribs have excellent cholesterol profiles, a perfectly normal heart and digestive system, low blood pressure, normal blood work and have beautiful skin and strong nails.
A woman who truly is too thin will most often show ribs.
However, I’ve seen women, whom I considered underweight, who were not showing ribs.
They were underweight in that they lacked muscle mass and had weak, frail looking arms and legs, and a frail looking torso – but the ribs were not showing in these “skinny fat” women.
If I lift my arms, my ribs will show. If I’m lying on a bench at the gym with my arms upward, and especially up-and-back, boy, do my ribs show.
They also show prominently if I’m leaning against something with my hands, arms outstretched, or if my arms are above me as when I’m in the “up” position of a lat pull-down exercise, or in the hanging portion of pull-ups/chin-ups/hanging leg raises.
However, I’m a physique athlete and avid powerlifter, and even though my ribs are visible, I also have visible muscle mass.
Physique and other athletes with controlled eating habits have visible ribs.

Freepik.com/artusofronov

Shutterstock/DuxX
These kinds of athletes typically are very conscious about the quality of the foods they eat.
They normally avoid fast food and other kinds of junk food, eating these items only occasionally.
They snack on healthy foods like fruit, salads and nuts, rather than chips, ice cream, candy and cookies.
They limit white sugar; some avoid it altogether.
How can people say these women are not healthy just because their ribs show?

Shutterstock/vectorfusionart
“For the average woman, reducing body weight to the lower range of the ‘normal’ scale, say a BMI of 18, may well result in the collar bones and lower rib margins being visible,” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
“With stretching or bending, an overall view of the rib cage, though not being able to walk down individual ribs, may be evident.
“Since it is subcutaneous body fat that defines a woman’s curves and masks such structural anatomy, one could conceive that a woman scant on fat, with muscle comprising a higher fraction of the BMI, would have visible ribs.
“This would be unique to the individual, though, and should not be held as an ultimate goal.”

So what if her ribs show. Look at her strong, trained legs! She is not underweight. Freepik.com/artursafronov