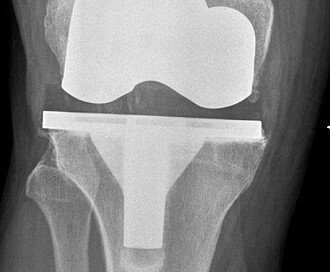
Is Gallbladder Removal Necessary for Only Pain, No Stones?

Wondering if your gallbladder pain warrants the removal of this organ even though you don’t have gallstones?
“Gallbladder dyskinesia [impairment of movement] is a motility disorder that affects the gallbladder,” explains Akram Alashari, MD, a trauma surgeon at Geisinger Medical Center in PA, and author of “THE POWER OF PEAK STATE.”
“Patients with this condition present with biliary-type pain, and investigations show no evidence of gallstones in the gallbladder,” continues Dr. Alashari.
“The diagnosis is made by performing a gallbladder ejection fraction, which is a radionuclide investigation.”
This procedure is called a HIDA scan. “An abnormal gallbladder ejection fraction has a value less than 40 percent.
“Patients with an abnormal gallbladder ejection fraction should undergo cholecystectomy [removal of this organ].
“This procedure has been shown to be effective in curing the symptoms in over 90 percent of patients.”

Dr. Alashari was formerly with Grand Strand Regional Medical Center in SC as an abdominal and critical care surgeon.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/KDdesignphoto
Middle Back Pain after Gallbladder Removal: Causes, Solutions?
Are you suffering from back pain post-gallbladder removal and are wondering what’s causing this and what can be done about it?
“It is not unusual for people who have had laparoscopic cholecystectomy [gallbladder removal] to experience muscular pain in the region of their puncture wounds under the ribs,” explains Akram Alashari, MD, a trauma surgeon at Geisinger Medical Center in PA, and author of “THE POWER OF PEAK STATE.”
“This pain can sometimes radiate to the back and can be confused with gallbladder pain in the early postoperative period.
“This usually resolves after five to seven days and can be treated with a local heating pad.”
The heating pad should be in the form of a water bottle that contours nicely to the curvature of your back.
Additional Pain Following Gallbladder Removal
Dr. Alashari adds, “Patients having had laparoscopic cholecystectomy occasionally experience shoulder pain which is usually due to the carbon dioxide used to inflate your abdomen during surgery.
“This typically resolves within a few days.”

Dr. Alashari was formerly with Grand Strand Regional Medical Center in SC as an abdominal and critical care surgeon.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Freepik.com jcomp
Stem Cell Injection into Total Knee Replacement for Pain Reduction?
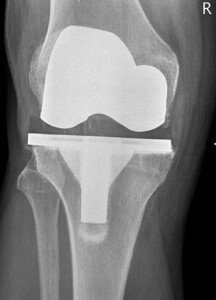
Can stem cell therapy work on a knee that’s had a total replacement?
An orthopedic surgeon who also uses stem cell treatments was asked this question by me, at his seminar, regarding my father who had a total knee replacement in each knee.
This was after the doctor presented information on stem cell treatments for painful joints—the injection would go into tissue, not hardware.
My father had seen many doctors to find out why both knees (post-TKR) were still so painful.
He got different responses from each doctor (including a diagnosis of peripheral neuropathy), and none were able to diagnose him with a failed TKR, though one said that the bone scan showed that they “might” be loosened.
The doctor at the seminar admitted that he had never administered stem cell therapy to someone with a knee replacement. He was touting SCT as an alternative to the knee replacement.
However, he was quite interested in my father’s situation and wanted to give it a try—he was so interested that he reduced the payment by 50 percent.
He is a board certified orthopedic surgeon who performs surgeries on knees, hips and shoulders, and he has performed the stem cell treatment on many patients including former professional athletes (with success), giving it about a 75 percent success rate.
My father, having tried everything, including electro-stim therapy from a chiropractor, endovascular back surgery (since the knee pain was blamed on spinal stenosis by a few doctors), massage and oral and topical painkillers, figured he had nothing to lose.
The doctor allowed me to observe the procedure, which involves injecting the patient’s stem cells into the painful joint.
Though my father has hardware in both knees, the doctor found a “soft” spot where there was tissue, and made the injection there.
The stem cells were harvested from my father’s pelvis, then centrifuged for 12 minutes to separate them from the rest of the blood matter (3,000 gees).
The actual injections took less than 30 seconds.
The doctor said that if this is destined to work, it will take three to four weeks.
The stem cells are supposed to reduce inflammation as well as deliver oxygen and nutrients to the joint—a location that normally doesn’t get much blood circulation.
So, the reduction in inflammation, and the increased amount of oxygen and nutrients, will hopefully result in a notable pain reduction.
Stem cell therapy, as described by the doctor, is a one-time administration, though some patients who experience no alleviation of pain will go in for a second injection and then get results.
But if the first injection works…there’s no need for any additional injections down the road, because the stem cells multiply on their own—but, like cells anywhere else such as skin cells, have a turnover rate, so that the total amount of cells at any given time remains constant and controlled..
The doctor said that if he were to look at the stem cells in my father’s knee six months from now, he’d see the great-great-great-great-great granddaughters of the original cells he injected into the knee.
If this procedure works for my father’s knee pain, the doctor will know he’s really on to something.
UPDATE: The stem cell therapy never made any difference.
But remember, it was done on a patient with hardware in his knee, which is not the norm for this procedure.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Manjunath Ramappa, Andrew Port, CreativeCommons
Can a Painful Fatty Cyst in Your Armpit Come and Go?

Are you noticing that the cyst under your arm seems to disappear, then return, back and forth?
What’s really going on?
The cyst “can get enlarged and inflamed at times and make it feel as though it’s ‘coming and going,’” says Dr. Dendy Engelman, a board certified dermatologic surgeon with Manhattan Dermatology & Cosmetic Surgery.
She further explains, “Most cysts (although there are always exceptions) don’t resolve on their own, but they can certainly fluctuate in size and degree of symptoms (meaning sometimes they can be small and painless and other times they can be enlarged and painful).
“The other potential to consider in the underarm region is an inflamed lymph node.
“This can be the result of many causes — breast cancers, local infection or just a benign process. So, it’s always best to have axillary (armpit) growths evaluated.”
 Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: ©Lorra Garrick
Daily Itching Attacks on Entire Body with Rash: Causes
Sudden attacks of itching all over the body with a rash can mean one of several serious conditions.
What appears to be a rash may also be termed as “hives.”
“Paroxysms of pruritus (episodes of extreme itching) are miserable for patients and are often difficult to determine the etiology (cause) and to manage,” explains Dr. Dendy Engelman, a board certified dermatologic surgeon with Manhattan Dermatology & Cosmetic Surgery.
“Acute or chronic urticaria (hives) can be caused by internal illness (ex: thyroid disease, cancers, blood disorders, kidney or liver disease), medications, environmental exposures- – just to name a few.
“So, a full workup with a thorough history, physical, and blood work evaluation is critical to determining the cause.”
 Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Shidlovski
Flat Mole Rapidly Rises to Pencil Eraser Height

Should you panic and fear melanoma if a flat mole quickly becomes elevated to pencil eraser height?
I read in a skin care forum of a woman who was very worried about melanoma because one of her moles had suddenly begun rising in height.
“While this most certainly could be a melanoma or a dysplastic nevus, it could also just be a benign keratosis,” says Dr. Dendy Engelman, a board certified dermatologic surgeon with Manhattan Dermatology & Cosmetic Surgery.
A benign keratosis refers to a seborrheic keratosis, or skin barnacle. “They often bleed, if scratched or rubbed, and can look quite ugly despite being benign,” says Dr. Engelman.
These “SK’s” often look like moles. In fact, if you have one on a location of your body that’s difficult to inspect up close, such as your back, it could easily pass for a mole. And you might have had it for years, thinking it’s a mole.
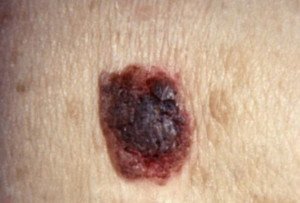
Seborrheic keratosis
Then suddenly it starts changing—and rapidly. This can happen with these skin barnacles.
A dysplastic nevus is a mole, but an atypical one (though benign) that has a higher chance of becoming malignant when compared to typical moles. They appear odd and may even resemble melanoma.
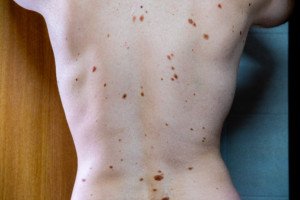
Dysplastic nevi. Shutterstock/Mikel Ugarte Gil
Dr. Engelman says, “Dysplastic nevi can change for a number of reasons; from being rubbed by clothing or inadvertently scratched — without there being significant cytologic atypica microscopically.
“That said, changing nevi almost always warrant a biopsy, but it doesn’t indicate that there’s always an associated malignancy.”
Certainly, if a “mole” rapidly rises in height, especially to that of a pencil eraser, waste no time getting it biopsied.
“Whenever in doubt, one should always get a concerning lesion evaluated by a licensed and trained professional,” says Dr. Engelman. This should be a dermatologist.
But what about nodular melanoma?
Don’t nodular melanomas grow quickly, and by definition, are elevated?
Dr. Engelman says about the OP’s mole problem, “It sounds like a nodular melanoma and it very well may be; however, there are also benign lesions that can rise to the size of a pencil eraser in as short a time as four weeks.
“Certainly, in my hands, if a patient is concerned, it gets removed and examined microscopically. In the ABCDE’s of melanoma, I always say that C not only stands for “color,” but also “concern.’”
 Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Leigh Prather
Do You Have an Itchy Painful Armpit? Cause and Solution
Itchy armpits can drive you crazy. And the more you scratch them, the itchier they get.
The area under the arm may even begin feeling rather painful.
One possible cause — something that may not even occur to many sufferers — is a new deodorant.
Deodorants do not have the exact same ingredients. A new deodorant can cause underarm itching.
A woman posted in an online forum that the itching occurred in only one armpit. But when she ceased using the new deodorant, the problem went away.
Allergic Contact Dermatitis
“It sounds like an allergic contact dermatitis to the deodorant,” says Dr. Dendy Engelman, a board certified dermatologic surgeon with Manhattan Dermatology & Cosmetic Surgery.
Dr. Engelman explains, “It is quite strange that it persisted only in one armpit, but it can happen that we have a persistent hypersensitivity reaction in one area of exposure and not in another.
“Avoidance of the causative culprit (the new deodorant) and mild topical steroids should help the itchy, painful eruption to subside.”
So as annoying or uncomfortable that this situation may be, rest assured it’s not a sign of any serious health problem.
You don’t want to be assuming that there’s cancer in a lymph node under your arm that’s causing the painful itching.
The itching may also be from fabric contact. Keep tabs on what you wear to see if there is a pattern to the flare-ups.
Underarm Care
Make sure your armpits are always clean. Wash gently. Never scrub or aggressively rub.
You’ll also want to keep them shaved, since hairiness can contribute to itchiness.
When you shave, be very, very gentle and patient. Do not rush through it or press the razor hard into the skin.
Shaving will reveal if there are any problems that can be involved with the itching, such as a skin tag or seborrheic dermatitis — which is notorious for itching and stinging.
It appears as pink/red and sometimes flaky patches of skin.
 Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
Versed in the latest techniques and technologies, Dr. Engelman provides a wide range of services including fat removal, mole excision, Mohs surgery and skin cancer treatment.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Chinnapong
Muscle Twitching: Why You Should Feel Good About Twitching Muscles

Muscle twitching is quite a popular topic, but not one you’ll hear a lot about at the water cooler.
In cyberspace, twitching muscles are discussed quite prominently, because muscle twitching, though extremely common, is also a symptom of one of the most feared fatal diseases: amyotrophic lateral sclerosis (ALS).
But twitching muscles don’t mean you have ALS, any more than a little gas means you have colon cancer.
Unfortunately, once a person gets into the “I think I might have ALS” groove, the anxiety over this can become chronic — unless the person learns to see muscle twitching for what it really is: just tired muscles working their issues out.
“The delicate balance between nerves, their stimulation and chemistry, and the muscles they feed is often affected by fatigue, stress, caffeine or other quite benign influences,” says Marc I. Leavey, MD, a primary care physician with 40-plus years of experience.
He adds: “When the balance is not correct, the muscle can twitch in a seemingly random fashion, not under your control.
“It does not take much; staring at the computer screen too long can start the lower lid dancing.

Freepik.com, jcomp
“The vast majority of such twitching is self-limiting, and resolves with correction of the underlying defect.
“As with many other weird symptoms, if it is not getting better, or if it seems really abnormal, see your health care professional.”
Anyone with a lot of muscle twitching will tell you that movement almost always stops the twitching.
Perhaps this is because when a muscle is forced to work, it’s not relaxed enough to twitch.
And anyone who twitches a lot will tell you that most muscle twitching occurs while in a relaxed state.

This is maybe because a relaxed, at-rest muscle can “feel free” to twitch all it wants.
Dr. Leavey says, “Try this: Stand in a doorway and lift your arms, hard, into each doorpost. Hold that position for about 30 seconds.
“Now step out and let your arms relax by your sides. OMG – MY ARMS ARE COMING UP ALL BY THEMSELVES!
“By stressing one group of muscles, resting them allows the other group, that was opposed by the exercise, to take action.
“Similarly, muscles are always adjusting our balance and status, shifting weight on the chair or feet, and, if you are at rest, you’re going to feel that.
“You’ll feel a twitch or movement that makes no sense. Well, to your body, it does.”
The reason why there is a certain percentage of people out there who obsess about the possibility of having ALS is because they were in the wrong place at the wrong time: They googled those keywords: muscle twitching.
Googling these words will bring up links to ALS, but also multiple sclerosis, a few other neurological disorders and Lyme disease.
One day I put my legs through a punishing weight routine at the gym.
They were sore the next day; delayed onset muscle soreness. But I used my treadmill that next day, running on top of the soreness.
My hamstrings were aching and stiff, and I took to sitting at the computer for an extended time.
Lo and behold, the twitching began in my hamstring muscles. But I must say, it felt GOOD! It was almost like tiny fingers were giving me a nice massage.
It felt like miniature fingers were in there, working their way around in my beat muscles, working out the accumulation of lactic acid and other byproducts of anaerobic exertion (from the weightlifting and also the cardio).
And when the twitching began dissipating, I was disappointed. I wanted this automatic massage to continue.
But I guess the job of the twitching muscles was completed; perhaps the lactic acid had been dispersed.
So next time your muscles twitch, don’t despair; think of it as your body’s built-in massage mechanism for fatigued muscles.

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Cookie Studio
Why Does Running Increase the Urge to Urinate?
Is it just imaginary, or does running really increase your need to take a leak?
Have you ever noticed that you seem to have to urinate more when you’re running, whether it’s outdoors or on a treadmill? There are a few explanations for this.
The first one comes from Marc I. Leavey, MD, a primary care physician with 40-plus years of experience.
He explains, “The act of running, itself, can cause pressure or shifting of abdominal or pelvic organs, putting pressure on the bladder, with the results that cause a pause.”
The second explanation is that while exercising, you’re guzzling more water than you think you are, and hence, you eventually have to relieve yourself before the workout is completed.
Freepik.com
A third explanation is that you actually don’t have to relieve yourself any more frequently when you run, but rather, you’re more sensitive to even just a little urine buildup in your bladder when you’re doing any kind of impact activity — of which running is one.
In other words, it’s very important to you to be as comfortable as possible when doing aerobic exercise.
So even a tiny bit of urine in your bladder will get your attention — the same amount that would go ignored if you were sitting at a computer.

Dr. Leavey was formerly with Mercy Medical Center in Baltimore, MD, where his focus was primary care and internal medicine. He has a blog, STRING OF MEDICAL PEARLS.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Noise vs. Odor Sensitivity: Which Should You Tune Out?

Why are people told to “just tune out” annoying sounds, but these very same critics don’t feel this way when something begins stinking really bad?
How many times have you complained about a noise and were told to “just tune it out”?
Ever wonder if your critic could apply this same advice—tuning it out—should he or she suddenly find themselves sitting next to someone at the movie theatre with underarm odor?
“Oh, just tune it out,” someone once told me when I mentioned that a strange humming had started up in my bedroom wall.
It turned out to be from a water pump a few blocks away, and the water pipes running up the street were conducting the sound.
If I had told this person, “Lately there’s this strange smell coming from my heating vent,” he would have told me to check it out, get it resolved.
Next time you label someone with “noise sensitivity” and/or tell them to “just tune it out,” ask yourself how you’d feel if you were met with this same reaction upon complaining that your coworker, whom you must work close beside with every day, has really bad body odor or foul breath. Yes, just tune it out.
Or how about the reek of sewage? Suppose right outside your house, where you like to sit on the deck, there develops the stench of sewage.
- Could you tune this out?
- If it bothers you, does this mean you have some kind of “sensitivity” to odors?
- Does it mean you have some kind of glitch in your brain or obsessive compulsive thought disorder?
Of course not! So why do people who complain of noise pollution or some kind of intrusive sound get labeled as being “sensitive to noise” or neurotic?
Granted, a foul or burning-type smell should be investigated, as it could indicate a problem that needs prompt mitigation.
If you suddenly smell chemicals, gas, something burning or what seems to be rotting flesh, this should not be ignored.
But there are other bad odors that you know are harmless, such as someone’s armpits and breath.

Shutterstock/Aaron Amat
Yet why not tune these benign odors out? I can go on and on with this, because I just don’t get why people are quick to invalidate noise complaints but not odor complaints.
One time my brother told me to “just ignore it” in reference to some kind of noise I had complained about.
I fired back, “If you think tuning it out is so easy, let’s imagine your neighbor is playing a recording artist whose voice you absolutely cannot stand—volume up—all day long. Could you tune it out?” He had nothing to say about that.
What does a doctor say?
“We have five senses, they say, but the five are not really created equal,” says Marc I. Leavey, MD, a primary care physician with 40+ years of experience.
Smell, it turns out, may well be the first sense of which we are aware. The sense of smell is hardwired to an area at the top of the nasopharynx, called the cribriform plate, and is active essentially at birth.
“The sense of smell helps us find food, recognize the scent of our mother, and other vital needs.
“While we can hear from an early age, the startle of a baby to a loud sound is evidence of that we need to learn what sounds mean, learn language and music.
“These learned sounds need processing by the brain to be understood; and can thus be filtered out. Scents that are primary stimuli to our senses are not so easily ignored.”
Noise Sensitivity vs. Odor Sensitivity
There actually exist disorders relating to the intolerance of sound. One such condition is called phonophobia.
But if you’re complaining that the water pump to your apartment complex’s pool squeaks throughout the night, interfering with your sleep, this is not a sign of phonophobia — or another disorder called hyperacusis, which is intolerance to sound.
Certain sounds are intolerable to some people but embraced by others. A classic example is that of children’s screams during play. You either hate this or delight in this, it seems.
Same with thunder. Some people enjoy hearing the rumbles, while others are put on edge. Some people love opera music while others cringe.
But when it comes to bad odors…the aversive nature is universal. How many people like the stench of garbage?
How many people do you know enjoy inhaling sewage odor or the stench of a public porto-o-potty?
Does anyone like the smell of rotting fish or vomitus? How about hot tar?
And I doubt that anyone hates the aroma of freshly baked bread, brewing coffee and a bouquet of flowers — though something tells me not to bet on that.