If you suspect your child has sleep apnea and are worried it can affect their lungs if not treated, you are correct.
See a doctor right away about a sleep study for your child.
Children do get sleep apnea. Even thin kids can suffer from this much-misdiagnosed disorder.
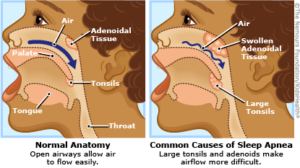
Causes in kids include large tonsils, large adenoids, a big tongue base and a naturally small airway.
Tell-tale signs that obstructive sleep apnea might be present is when a child never seems to have restful sleep – and, during the day, gets drowsy or falls asleep during passive activities, is moody and can’t stay focused.
During sleep, suspicious signs may go as follows:
Every few minutes, it seems, the child fidgets in their sleep, seems to become aroused but not fully awake, takes a sudden gasping breath or snorts, then settles down again. A few minutes later the scene repeats.
Untreated Sleep Apnea’s Effect on a Child’s Lungs
“Many children with OSA often have asthma, and there is thought to be a connection between these disorders,” says Joi Lucas, MD, medical director of pediatric pulmonology at Nemours Children’s Clinic and chief of pediatrics, Lakeland Regional Hospital, FL.
“Asthma is an inflammatory condition, and OSA in children is suspected to produce inflammatory mediators that can contribute to structural changes in the lungs over time.
“Both disorders are associated with difficulty breathing overnight and may cause a decrease in oxygen level.
“However, OSA may worsen asthma. When children with OSA snore this creates vibration of the airway which may lead to and can cause bronchoconstriction and increased airway tone.
“This closure of the airway may lead to exacerbation of asthma.
“Children with severe asthma are evaluated for OSA because of the association between these two conditions.
“Children with OSA also have been shown to have worsened immune function which may make them more susceptible to respiratory illness and other infections.”
If you suspect your child might have sleep apnea, do not dismiss this and assume they’ll outgrow it.
Ask your child’s pediatrician about a sleep study that will detect the presence of OSA.




































