If you fear you might have esophageal cancer, can you always expect eventual food impaction?
Or could the tumor grow in a way that food impaction wouldn’t necessarily result?
A person might begin having symptoms that are seemingly related to a digestive issue.
Digestive problems are extremely common and have numerous benign causes, but can also be caused by cancers including that of the esophagus.
Worsening symptoms don’t always mean a malignant tumor.
And, the first sign of esophageal cancer doesn’t start out with a bang.
Anyone who’s full of anxiety over new symptoms, and is familiar with esophageal cancer, will know that this disease leads to food impaction if left untreated.
Food impaction means that food gets completely stuck in the esaphagus above the tumor because the tumor blocks it from going down further.
Keep in mind that the sensation of “stuck food” doesn’t necessarily mean a tumor.
Many people with GERD report the sensation of food being “stuck” in their chest.
Is food impaction from esophageal cancer always inevitable?
“Definitely yes,” says Alex Little, MD, a thoracic surgeon with a special interest in esophageal and lung cancer.
“In earlier years, perhaps because of patient denial or difficulty obtaining medical care, more patients than today showed up with advanced cancer and complete esophageal obstruction with food impaction.
“This happens now but less frequently.
“Patients seem more likely now to present with progressive dysphagia — but still able to swallow soft foods and liquids.
“But there is no question, untreated esophageal cancer will progress, completely occlude the esophageal lumen and cause food impaction.”
Dysphagia Defined
Dysphagia is difficulty swallowing. However, what most laypeople don’t know is that doctors define “swallow” to include the process of food going down the esophagus and into the stomach, and not just when it gets past throat level.
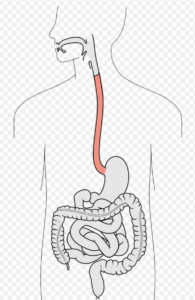
Olek Remesz,wiki-pl,Orem, commons
So if someone easily swallows food past their throat – this is only the first phase of swallowing.
The next phase is down the esophogus. If there is an obstruction from a tumor, this will interfere with this phase of swallowing.
The food initially will get past the tumor, but as the cancer gets bigger, less and less food will be able to get past it, and eventually if left untreated, even soft foods will get completely blocked.
But even before complete occlusion occurs, the patient will find it impossible to continue dealing with the problem, which will include regurgitation of the food into the mouth.
Though regurgitation into the mouth can happen to any healthy person simply from eating too much too fast, or from having acid reflux issues, this benign regurgitation is usually mostly a small amount of bad tasting liquid that’s sometimes re-swallowed or spat out. It may contain a tiny amount of solid matter.
With esophageal cancer, the regurgitation is high volume and may contain a lot of solid food.
Attempts to get more food down will result in continued regurgitation and distress.
Complete Impaction from the Time of First Symptom Onset: How Long?
“The length of time required for a tumor to cause complete obstruction is dependent on several factors,” says Dr. Little.
“One is the time required for a tumor to grow to a size sufficient to nearly or completely fill the esophageal lumen.
“We have no hard data; not all cancers grow at the same rate, and some enlarge more in a vertical than a horizontal orientation.
“The latter would be more likely to produce early complete obstruction.
“We have no real idea of the time that passes from the first malignant cell to complete obstruction.
“Tumors grow at variable rates but, based on the short time it takes to progress from mild to severe dysphagia, they probably double in size every one or two months.
“In terms of time from the first symptom to complete obstruction, patients progress from a sensation of food sticking — when many seek help — to an inability to swallow anything solid (a state of food impaction) — within a few months. Never as much as a year.
“So, the sooner patients respond to the first symptom, the better. And physicians must always take seriously the complaint of new dysphagia.”

 Alex Little, MD, trained in general and thoracic surgery at the Johns Hopkins University School of Medicine; has been active in national thoracic surgical societies as a speaker and participant, and served as president of the American College of Chest Physicians. He’s the author of “Cracking Chests: How Thoracic Surgery Got from Rocks to Sticks,” available on Amazon.
Alex Little, MD, trained in general and thoracic surgery at the Johns Hopkins University School of Medicine; has been active in national thoracic surgical societies as a speaker and participant, and served as president of the American College of Chest Physicians. He’s the author of “Cracking Chests: How Thoracic Surgery Got from Rocks to Sticks,” available on Amazon.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.



































