Both GERD and costochondritis can cause enough pain in the chest to stop you cold in your tracks.
These two conditions have very unrelated causes but can produce very similar symptoms.
A comparison between the symptoms of GERD and costochondritis (“costo”).
“Gastroesophageal reflux (GERD) describes the traveling of acid produced in the stomach up into the esophagus, often causing classic symptoms such as heartburn or chest pain, the tasting of something acidic, coughing, difficulty with swallowing food and regurgitation of food or liquid,” explains G. Shelton McMullan, MD, board certified gastroenterologist with Capital Digestive Care in MD.
“Costochondritis, involving the inflammation of cartilage in the rib cage, can also cause chest pain that is sometimes similar to that caused by GERD,” continues Dr. McMullan.
You Know It’s Not Your Heart, So It’s Either GERD or Costochondritis?
“Of most concern for anyone reporting chest pain is whether or not the heart is the cause, so a cardiac evaluation involving at least an electrocardiogram (EKG) and blood work to assess cardiac enzymes is always performed first,” says Dr. McMullan.
If you go to the ER, that’s where you’ll get the cardiac enzyme test to see if you recently had, or are having at that moment, a heart attack. You’ll also get the EKG, a chest X-ray and a D-dimer test.
Chest pain can also be caused by a heart rhythm disturbance, inflammation involving the heart, a tear in the aorta, coronary artery spasms or blockages, pneumonia, a blood clot in the lung and lung cancer.
You can also schedule a cardiac stress test to see how blood flows through your coronary arteries during physical exertion.
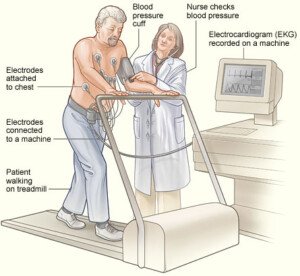
Stress Test
So let’s assume, then, that a complete cardiac workup shows that your heart is in perfect health. You are now wondering which is causing the chest pain: GERD or costo?
Remember, discomfort in the chest has numerous potential causes, but acid reflux and inflammation of cartilage in the rib cage are two very common causes.
“Along with recommendations to make lifestyle changes such as avoiding certain culprit foods and eating/drinking close to bedtime, and acid-blocking medication (such as a histamine blocker like ranitidine or a proton pump inhibitor such as omeprazole), will often be prescribed to be taken regularly for an individual who reports frequent symptoms thought to represent GERD,” says Dr. McMullan.
“These measures will not tend to help a person whose symptoms are solely due to costochondritis, however.
“Many individuals with suspected costochondritis are advised to take a short course of a non-steroidal anti-inflammatory drug (NSAID) like ibuprofen.
“It is very common for individuals with costochondritis to feel discomfort when their ribs, at the site of cartilage inflammation, are pressed on.
“While palpation of the upper abdomen can sometimes cause discomfort in someone who has GERD, this is not always the case.”
Additional Comparisons Between GERD and Costochondritis
The pain from both conditions can come on suddenly.
• In some individuals, GERD is triggered only overnight, and is relieved when they sleep with their torso propped up on a wedge pillow or by elevation of the head-end of their bed.
• When experiencing chest discomfort from GERD overnight, the patient may feel instant relief upon sitting up.
• GERD is not always accompanied by a burning sensation, unpleasant taste or cough.
• The chest pain of GERD may also predictably occur after heavy meals.
• Costochondritis, like acid reflux disease, can be provoked with certain body positions. Both conditions can manifest when someone lies down.
• Unlike GERD, costochondritis can be brought on or made worse by any of the following: pressure from a seatbelt or a hug, coughing, sneezing, deep breathing and exercises like the bench press, dumbbell or machine chest press, and/or dips.
• The chest pain of both conditions may range from dull to sharp.
 Dr. McMullan has published numerous medical abstracts and presented posters related to the management and treatment of inflammatory bowel disease and other gastroenterological conditions.
Dr. McMullan has published numerous medical abstracts and presented posters related to the management and treatment of inflammatory bowel disease and other gastroenterological conditions.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.