You abruptly wake up from sleep gasping, feeling like you haven’t taken a breath for a whole minute. Is this your heart?
Could it be cancer or sleep apnea?
Suddenly being awakened by the need for air is frightening even for people who don’t suffer from health anxiety.
For others, they just shrug it off as the effect of gravity on a very relaxed chest that suppresses breathing and think nothing more of it once they take in a gulp of air.
Waking Gasping for Air: Is the Cause Heart Disease, Cancer or Sleep Apnea?
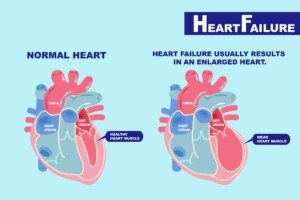
Congestive Heart Failure
“Awakening in this fashion typically is a manifestation of congestive heart failure, a situation wherein a weakened and diseased heart is unable to accommodate the gravitational flow from the horizontally oriented lower body,” explains Morton Tavel, MD, Clinical Professor Emeritus of Medicine, Indiana University School of Medicine, and author of “Health Tips, Myths and Tricks: A Physician’s Advice.”
“When this happens, blood returning from the lower body goes first to the lungs, but is then slowed from entering the weakened heart, which then results in pressure buildup and congestion in the lungs, a process that causes shortness of breath, which is usually relieved when the subject assumes the upright position,” says Dr. Tavel.
Shutterstock/EstherQueen999
When you wake up feeling a choking sensation, are you horizontal or propped up? If you’re horizontal, this doesn’t mean you have congestive heart failure.
But it’s important to know that being propped up during sleep is a widely used tactic among people diagnosed with congestive heart failure.
It makes breathing during sleep a lot easier, as it reduces fluid buildup in the lungs.
If you fear heart failure simply because you keep being jolted out of your sleep gasping for air, you need to ask how likely it is that you actually have this disease.
- If you’re 30, work out, play pickup basketball and never have shortness of breath during the day, it’s a safe bet you don’t have heart failure.
- If you’re over 60, have been getting more and more short of breath during the day, do not exercise and have high blood pressure – you’d better get your heart checked.
A tell-tale sign that the “gasping” is caused by congestive heart failure is that the shortness of breath persists as you continue to remain horizontal.
It is not corrected just because you awaken. It’s not one of those one-time gasps, and then all is fine. It continues, breath after breath. Sitting up relieves it.
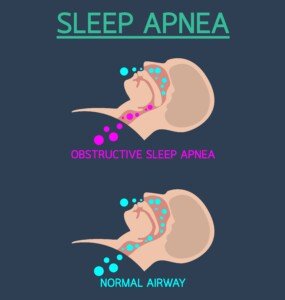
Obstructive Sleep Apnea
Dr. Tavel explains, “A less common cause of gasping for air at awakening is obstructive sleep apnea, which is caused by intermittent partial airway obstruction, accompanied with heavy snoring and periodic awakening.”
Shutterstock/iLoveCoffeeDesign
Are you skinny? If yes, then so what. Thinness does not rule out obstructive sleep apnea.
Though obesity and male gender are risk factors, thin women can have OSA, which is one of the most under- and misdiagnosed medical conditions.
Smoking is a risk factor, and so is drinking alcohol shortly before bedtime.
Smoking causes inflammation of the throat tissue, and drinking increases relaxation of the tissue.
If you don’t smoke or drink, you can still have natural surplus throat tissue that just gets in the way of your upper airway during sleep. A big tongue base also adds to the picture.
Though most people with untreated OSA snore, some patients do not snore.
Untreated sleep apnea’s daytime symptoms can masquerade as benign in cause.
For instance, the young slender woman with OSA who has daytime fatigue and irritability may blame these issues on caring for two young children.
A tell-tale sign that your sudden awakening and gasping for a breath is due to obstructive sleep apnea is that it takes only one deep inhalation to correct the problem – then you’re good to go.
Waking with morning headaches that are gone within 30 minutes of being out of bed are highly suspect for OSA.
If sleeping on your side eliminates the breath problem, this further points to OSA – a positional type of OSA. But most sleep apnea patients will suffer disordered breathing regardless of body position.
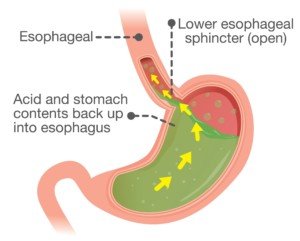
Acid Reflux
“Another uncommon disorder is related to acid reflux, in which case acid is regurgitated retrograde up into the throat, producing the sensation of burning chest pain and choking,” says Dr. Tavel.
“This usually results from an incompetent valve at the end of the esophagus.”
Shutterstock/solar22
The acidic juices from the stomach have made their way up to the vocal cords. This irritates them, leading to a transiently compromised airway.
If the gasping is accompanied by an unpleasant taste in the mouth, coughing or a burning or scratchy throat, you just might have a case of LPR: laryngopharyngeal reflux.
Avoid eating close to bedtime and sleep with your torso propped up to see if that doesn’t improve the situation.
Anxiety
“Anxiety itself can occasionally produce awakening with a sensation of choking or ‘air hunger,’ sometimes associated with a sensation of fear or panic (a panic attack),” says Dr. Tavel.
“What is really happening under these circumstances is hyperventilation or over-breathing, which then often results in lightheaded sensations accompanied by numbness and tingling in the limbs, general weakness, and if extreme enough, a temporary loss of consciousness.”
Have you noticed that the more you worry about choking in your sleep, and the more you anticipate these events happening, the more they actually happen?
They may still be caused by sleep apnea and reflux, but anxiety and fear make the situations worse.
Cancer
It’s not often that a person automatically suspects cancer when they wake in the middle of the night gasping for air.
Usually they will wonder about their heart, sleep apnea or suspect a panic attack or acid reflux.
But a smoker or heavy drinker who knows that smoking and drinking are strong risk factors for laryngeal cancer just might think of cancer before any other condition. Or, they might wonder about lung cancer.
Dr. Tavel says, “Cancer, even when involving the lungs, is not associated with such gasping limited to the awakening process.”
How to Find Out the Cause of Your Overnight Gasping
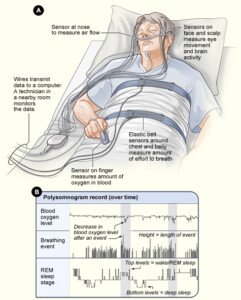
Sleep Study
Have a sleep study done – either at a lab or at home. The home test is easier than you think and is pretty accurate.
Sleep study
It will measure, among other vitals, how many sleep-disordered breathing events you had while asleep.
The study will compute the hourly average. If you have more than four disordered breathing events per hour, you will fit the criteria for a sleep apnea diagnosis.
This means that fewer than five per hour means you’re in the clear, yet these may still be getting caused by airway obstructions.
If it’s under five per hour, no treatment is necessary, but at least you’ll have tremendous peace of mind that you finally know that the cause does not require treatment.
Heart Exam
An echocardiogram will show if you have heart failure. This is an ultrasound of your heart and takes about 20 minutes.
If you have risk factors for heart failure and report issues with breathing during sleep, a cardiologist will surely recommend an echocardiogram.
If your heart functions normally and the sleep study yields zero disordered breathing events, then the issue is probably acid reflux and/or anxiety.
• Try different sleep positions, particularly reclined or propped up to see if that helps.
• Avoid liquor and food close to bedtime.
• Quit smoking.
• Lose weight if you’re overweight.
• Have a dentist screen you for TMJ disorder, as this can actually cause airway obstruction.
Waking in the middle of your sleep gasping for air is frightening, but it’s not a sign that you might suffocate to death or have a heart attack. And stop worrying that it might mean cancer.

Dr. Tavel’s medical research includes over 125 publications, editorials and book reviews in peer-reviewed national medical journals. He was formerly director of the cardiac rehabilitation program at St. Vincent Hospital in Indiana. mortontavel.com
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.



































