The GERD and Candida connection is explained by a gastroenterologist.
“Can GERD cause a Candida infection?”
This was the question that I posed to Larry Good, MD, who has been a practicing gastroenterologist for 40+ years. He has a private practice that is located in Lynbrook, NY and is affiliated with Concierge Choice Physicians, a leading provider of personalized care in the U.S.
“Severe esophagitis with deep mucosal injury can predispose to Candida esophagitis,” says Dr. Good.
“This is a very common condition caused by an overgrowth of a fungal organism called Candida albicans in the esophagus.
“This is usually precipitated by the prolonged use of antibiotics or by immunosuppression caused by chemotherapy or other medicines that suppress the immune response.”
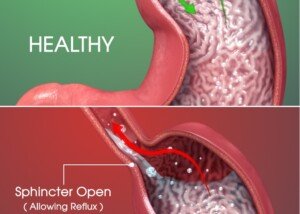
Indeed, GERD (gastroesophageal reflux disease) can lead to a Candida infection because esophagitis can be caused by GERD!
In fact, GERD is the most common cause of inflammation of the esophagus.
If you are taking a course of antibiotics, you should also, simultaneously to that, take a probiotic supplement every day, or eat a probiotic food such as yogurt or kefir (with “live culture bacteria,” the beneficial kind of bacteria).
Antibiotics snuff out the good bacteria that normally lives in your gut. So taking a daily probiotic will help keep the balance in check.
“If the esophageal mucosa is chronically inflamed it becomes more susceptible to this [Candida] infection,” adds Dr. Good.
“Under normal conditions, Candida is not a pathogen. It is part of the normal flora that lives in the mouth, on the skin and in the vagina. Treatment with anti-fungal medications is very effective.”
A Candida infection is called candidiasis.
When it develops in one’s mouth it’s called thrush or, on the medical report, oropharyngeal candidiasis.
It can also occur in the vagina, commonly known as a yeast infection.
In addition to affecting the throat, vagina and esophagus, Candida albicans can also become invasive, getting into the bloodstream and seriously affecting organs.
 Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
Dr. Good has additional expertise in the diagnosis/treatment of IBS and inflammatory bowel disease, and is extremely proactive in genetic testing, individualization of pharmacologic treatment, and risk mitigation in cancer screening/prevention. Concierge Choice Physicians
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.
Top image: Shutterstock/Thomas Foldes