Do you have GERD symptoms, and were you diagnosed with GERD, but your upper endoscopy was normal?
There was no sign of inflammation, irritation, acid injury or anything else visible on endoscope – yet you’ve been having classic symptoms of gastroesophageal reflux disease.
Your doctor even told you, based just on a clinical exam and medical history, that the top three likely culprits are “GERD, GERD and GERD.”
So why have the upper endoscopy?
This is a very reasonable procedure for patients who are worried that their chronic acid reflux issues may have led to Barrett’s esophagus – which CAN be seen via endoscopy.
Patients may also be concerned that their symptoms could be the result of an ulcer, esophageal stricture or some other abnormality that an endoscopy will pick up on.
If the patient hears, “Your esophagus is normal,” this will be incredibly reassuring!
Nevertheless, the patient may still be experiencing symptoms of excess acid being refluxed into the esophagus and even reaching the throat.
Why can an upper endoscopy be normal in the presence of GERD?
“This is a very good question, and there are several reasons why upper endoscopy can be normal in those with GERD symptoms,” says Santosh Sanagapalli, MD, a consultant gastroenterologist, endoscopist and specialist in esophageal disorders.
It’s not GERD. “Firstly, so-called ‘GERD symptoms’ are not always due to GERD – and this is the case even where there is a ‘typical’ history and response to antacids,” explains Dr. Sanagapalli.
“The most typical GERD symptoms are heartburn (burning sensation behind the breastbone) and regurgitation (feeling of fluid rising up the chest and/or into the throat).”
Less common GERD symptoms include upper abdominal discomfort or burning, excessive burping, a pressure or discomfort when burping, a stuck-food feeling in the chest, a burning throat and a hoarse voice.
The chest and abdominal symptoms “can be found in other esophageal conditions also, e.g., eosinophilic esophagitis, achalasia, reflux hypersensitivity and functional heartburn,” says Dr. Sanagapalli.
“All of these conditions can present with a normal endoscopic appearance and need other investigations to be differentiated from GERD, e.g., esophageal manometry, barium swallow, esophageal histology, 24hr pH testing.”
• Eosinophilic esophagitis: An autoimmune disorder in which white blood cells build up in the wall of the esophagus. The buildup is usually an allergic reaction to one or more foods that the patient is eating.
• Achalasia: The lower esophageal sphincter fails to open when you swallow food.
• Esophageal hypersensitivity and functional heartburn: Reflux-like symptoms despite no excess of acid reflux on 24hr pH testing, and with other esophageal disorders excluded
When it’s GERD. “Even when GERD is established to be definitely present by a 24hr pH study (the gold standard test), the endoscopy can often appear normal,” says Dr. Sanagapalli.
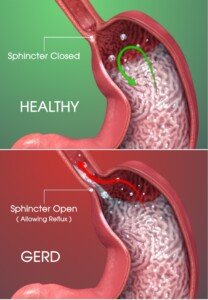
Scientific Animations, Creative Commons/BY-SA/Attribution-ShareAlike 4.0 International
“In fact, we know that the majority of patients with established GERD will have a normal endoscopy.
“This is termed ‘non-erosive reflux disease,’ i.e., reflux is present, but has not damaged the lining of the esophagus, so no abnormality can be visualized at endoscopy.
“Symptoms can nevertheless still be present, because acid in the esophagus can still stimulate pain receptors even when inflammation is not present.
“This is especially the case in patients who are already taking PPI’s at the time of endoscopy, as PPI’s are very good at healing the inflammation of the esophagus — but may not necessarily lead to complete resolution of symptoms.”
What does a normal endoscopy mean – or NOT mean?
“Therefore, it is important to be aware that a normal endoscopy does not mean that a patient does not have GERD,” continues Dr. Sanagapalli.
“Endoscopy is great for identifying worrying diagnoses such as cancer and other structural abnormalities in the esophagus, e.g., hiatus hernia.”
If an esophageal tumor is big enough to cause symptoms (which, without treatment, will keep getting worse to the point of causing great distress), it’ll be easily visualized upon upper endoscopy. A biopsy will confirm diagnosis.
“While sometimes positive in GERD cases, it cannot be used to rule out GERD,” says Dr. Sanagapalli of the upper endoscopy.
“Therefore, patients with persistent GERD symptoms and a negative endoscopy should proceed to have 24hr reflux pH testing.
“This more definitively determines whether or not a person has GERD by measuring the amount of acid reflux occurring over a 24hr period.”
 Dr. Sanagapalli is a gastroenterologist and director of the Esophageal Disorders Center at St Vincent’s Hospital, Darlinghurst. He performs diagnostic and therapeutic endoscopic procedures, and enjoys providing comprehensive and holistic care to patients with a wide variety of disorders affecting the gastrointestinal tract.
Dr. Sanagapalli is a gastroenterologist and director of the Esophageal Disorders Center at St Vincent’s Hospital, Darlinghurst. He performs diagnostic and therapeutic endoscopic procedures, and enjoys providing comprehensive and holistic care to patients with a wide variety of disorders affecting the gastrointestinal tract.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.



































