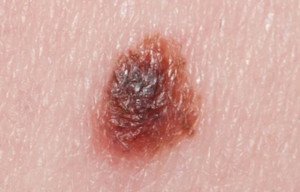
Learn how to produce a very reliable mole map at home for melanoma screening.
I have been “mole mapping” for three years and have learned along the way some excellent mapping techniques, for melanoma screening.
The technique I will describe has one caveat; you must be able to illustrate.
If a mole is on a part of your body that allows you to visually inspect it while your dominant hand draws it, this is a great mapping technique.
I was once watching a mole on my upper inner thigh, and decided to draw it. I held a magnifying glass over it, and with my dominant hand, drew and rendered what I saw.
In order for illustrative mapping to be reliable, you must be able to capture the mole’s nuances, subtle tone variations and other details – and draw them to an enlarged scale.
I drew the mole a lot bigger than its actual size (which was about 2 millimeters).
I drew another one that was on my lower abdominal region (it actually turned out to be a seborrheic keratosis, which can look very much like a mole; it had changed in appearance so I drew it).
The drawing should be a rendering, not merely a line drawing.
This way you can monitor for changes in color tone variation. Another reason to render is because often, the tone variation is gradual or gradated, rather than with a definitive demarcation.
With an illustration at hand, every time you check the mole, you don’t have to wonder if you’re imagining that a certain part of it is darker; or if the darker part of it has spread to fill up more of the mole; or if a darker or lighter part of it has changed shape or spread to take up more of the mole.
Because all you need to do is refer to the illustration, and you can see exactly how the spot appeared last time you checked it, and match the drawing up to what you’re now seeing.
Another way to illustratively do mole mapping is to imprint in your mind what the particular spot looks like.
This is applicable for moles that are located in areas that make it impossible to draw them.
I had one on the back of my neck that I thought was changing, so I imprinted it in my mind: border shape; the shape of the darker portion of it; any gradations.
With a ballpoint pen I drew it enlarged to scale and rendered it. I then monitored it based on this illustration. Soon after, a dermatologist said it was a seborrheic keratosis (these can change).
Being an illustrator also means you can measure whether or not a tiny mole is getting bigger. A “birth mark” on my shin had taken on a reddish tinge, but it was not bigger.
In anticipation that it might be getting bigger (since it was changing colors), I drew this little spot with a pencil to its exact size, on the edge of an index card.
I then could place the stiff edge of the card perpendicular to my shin, against my shin, just a tiny bit away from the mole, which then enabled me to make an accurate visual size comparison.
To add even more accuracy, I drew a spot next to the first drawing that was a little smaller, and one on the other side that was a little bigger.
I’d compare the mole to the middle drawing and it was a spot-on duplication of the size and shape (1 millimeter). After a few days, I noticed that the mole was a hair bigger than the original drawing!
I then lined the mole up with the larger rendition, and they matched in size! This was objective proof that the mole had increased in size!
So, not only had this previously solid brown spot taken on a reddish tinge, it had increased in size.
I had it removed and biopsied. Diagnosis: lentigo simplex (translation: irritated sun spot). The dermatologist’s nurse told me that it had probably been inadvertently rubbed or scratched, even maybe in my sleep.
What a Doctor Says About Moles
“A mole which is reactive to scratching or irritation, and does not have the cardinal signs of melanoma is still considered a benign lesion,” says Dr. Joshua Fox (not my dermatologist), founder and director of New York and New Jersey-based Advanced Dermatology P.C.
“It is benign and not dangerous in any way, even if it were to have some characteristics of the appearance of melanoma.
“It may require symptomatic treatment and observation; however, it will not be treated as melanoma.”
Mole mapping should include, when possible, drawings of your moles, for optimizing melanoma screening.



































