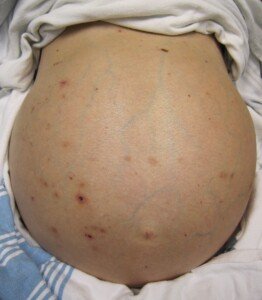
Ascites has many potential causes, but liver disease is notorious for causing this abdominal fluid buildup.
What if heart failure is behind the liver disease?
Is any resulting ascites more likely directly from the heart in congestive heart failure, or is the fluid retention more likely directly from a compromised liver?
If you’ve been living with chronic heart failure for years, you’re likely very aware that this condition can have a negative impact on your kidneys, since the kidneys get about 20 percent of the blood that the heart pumps out.
The kidneys, being very small in size but also being highly vascular, are quite sensitive to reduced blood flow.
The liver, though also very vascular and a greedy recipient of blood, is more resilient than the kidneys in the setting of chronic heart failure.
But this doesn’t mean that over time, its function doesn’t gradually get worse (though on a subclinical level).
For most people with chronic heart failure, cardiac liver disease is never an issue.
In most patients the symptoms of heart failure predominate, and a sudden worsening of heart function (acute heart failure) typically causes fluid buildup in the lungs (pulmonary edema), which in turn puts the patient in respiratory distress.
But ascites?
“Yes, this is possible if portal pressures increase high enough as a result of severe congestive heart failure,” says Daniel Motola, MD, a top board certified gastroenterologist and hepatologist providing same-day and next-day services in NYC with Gotham Medical Associates.
“This form of ascites is called cardiac ascites.” To the layperson, cardiac ascites implies ascites caused by the same mechanism that congestive heart failure causes peripheral or pulmonary edema.
But it comes from liver disease—impaired function—whose root cause is poor cardiac output in this case.
If the liver is sick enough, a chain reaction of biochemical changes results, leading to fluid buildup in the abdomen.
“The protein content is much higher in cardiac ascites, as there is leakage of protein out of the sinusoids of the liver,” says Dr. Motola.
“The sinusoids are normally leaky. However, in non-cardiac ascites due to cirrhosis and portal hypertension the sinusoids undergo capillarization [formation of capillaries] as a result of fibrosis, and thus there is less leakage of protein through the sinusoidal spaces.
“Thus, the protein content of the ascites fluid is lower.”
If you are interested in a consultation with one of Gotham Medical Associates’ gastroenterologists please call us at 212-227-3688 or book online. Our staff will be happy to assist you, your family member or friend.
 In addition to his liver transplant expertise, Dr. Motola offers expertise in chronic liver disease, GERD, IBS, colon cancer screening, endoscopy and disorders of the bile ducts and gallbladder.
In addition to his liver transplant expertise, Dr. Motola offers expertise in chronic liver disease, GERD, IBS, colon cancer screening, endoscopy and disorders of the bile ducts and gallbladder.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.


































