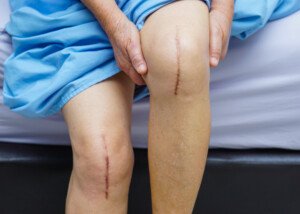
Just how safe or potentially dangerous are the potent blood thinners for joint replacement surgery? There’s something you need to first consider about these important drugs.
Joint replacement runs a high risk for blood clots, which can lead to a fatal pulmonary embolism.
Surgeons routinely prescribe potent blood thinners (anticoagulants) to help prevent a pulmonary embolism — which is when a piece of a blood clot in a lower-extremity vein breaks off and travels to the lungs.
“When looking at the safety of blood thinners after joint replacement surgery, we always have to look first at risk/benefit ratios,” says Barbara Bergin, MD, board certified orthopedic surgeon at and co-founder of Texas Orthopedics, Sports & Rehabilitation Associates.
“There is a higher incidence of blood clots/deep venous thrombophlebitis (DVT)/pulmonary emboli, following total joint replacement.
“This is a potential complication of that surgery. So, when we look at prevention, we look to blood thinners/anticoagulants.
“Traditionally, warfarin/Coumadin was used for prevention of DVT, etc. There are risks to the use of warfarin, particularly to the patient who has just had major surgery.
“Most importantly, there is a risk of prolonged bleeding. This can result in swelling and pain, and sometimes even delayed healing of the surgical site.
“Extreme pain and swelling can have a detrimental effect on the ability for the patient to mobilize and participate in physical therapy. This can result in a poor outcome.
“Wound dehiscence (failure of the wound to heal) can also result in infection, which can be catastrophic in a total joint replacement.
“At minimum, it can result in the need for additional surgery and all its potential risks.
“In time, alternative therapies were developed. Heparins (Lovenox), factor Xa inhibitors (Xarelto, Eliquis) and even aspirin act through different mechanisms, and have been found to provide the needed protection against DVT, as well as the advantage of decreased incidence of major bleeding.
“They are also more convenient to use and don’t require laboratory monitoring.”
In addition to a blood thinning drug, the joint replacement patient’s legs are wrapped in pneumatic compression cuffs.
These inflate automatically every several minutes to improve circulation in the legs, where deep vein thromboses typically develop, though a DVT can develop anywhere.
Another protocol to help prevent blood clots is to get the patient up and walking as soon as possible after surgery.
In conclusion, the risk/benefit ratio means that every joint replacement patient will be put on some kind of blood thinner drug.
How long the drug should be taken is determined from one surgeon to the next.