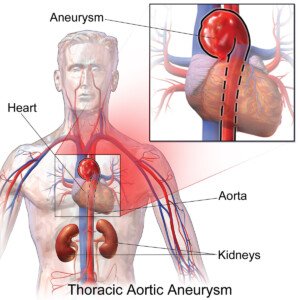
Stent graft technology for the repair of an ascending thoracic aortic aneurysm is a marvel of medical advancement.
Stent technology continues to evolve; soon, endovascular repair (stent grafting) will be more common with ascending aortic aneurysms.
Currently, fusiform ascending aortic aneurysms cannot be repaired with stent grafting (endovascular repair) because the placement of the stent requires landing zones.
The ascending aorta has openings that are formed from the vessels that branch off the top of it where it begins arching.
A stent graft would overlap one of these openings in order for the graft to be set in place.
If one of these portals is obstructed, then adequate blood supply will not flow through the vessel branch and reach other parts of the body.
The descending aorta has no openings formed by vessel branch-offs; hence, stent grafts can be set in place with generous landing zones.
This is why endovascular repair of a descending aortic aneurysm is rather common.
New Stent on the Block

A new kind of stent—multilayer—has been developed, and Grayson H. Wheatley III, MD, is leading the way.
He has years of experience as an aortic disease surgeon with TriStar Cardiovascular Surgery in Nashville, TN.
“The advantage of this stent is that because the stent has an open structure, it can cover branches without interfering with flow,” explains Dr. Wheatley.
Dr. Wheatley further explains that “the stent can be used in the ascending aorta and if additional landing zones are needed, it can cover the coronary arteries or the great vessels.”
The great vessels are the ones that branch off the aorta’s arch.
“This may be the best solution for ascending aortic aneurysms,” adds Dr. Wheatley.
“There wouldn’t be blood flowing into the aneurysm around the stent except in rare cases where the aneurysm goes all the way to the aortic valve (called aortic root aneurysms).”
When will endovascular treatment of an ascending aortic aneurysm become more common?
“We are working with the FDA to initiate a trial for high risk surgical patients with complex aneurysms.”
Normally, when the diameter of a TAA reaches close to 6 cm, it’s time for repair in a patient who has not been having symptoms, and does not have a connective tissue disorder or a bicuspid aortic valve.
(Patients who do have at least one of these variables have a lower measurement threshold before surgical repair is warranted.)
Learning about this threshold got me thinking about how all of those people, who are under 5.7 cm but greater than 4 cm, must continuously live on what I call the disability list, not to mention the anxiety that a sudden charge of emotions, straining on the toilet or lifting a child might cause a rupture.
Could the new multilayered stent graft lower the threshold measurement?
After all, living with a TAA is unnerving; why wait for it to reach 5.8 cm when it can be endovascularly repaired at 4.5 cm?
Lowering the threshold is a potential possibility, says Dr. Wheatley. “The decision on when to treat an aneurysm is based on the risk of rupture versus risk of surgery.
“With this new stent, the risk of the surgery would potentially be much lower and thus we might be able to treat patients earlier with smaller aneurysms, but this has yet to be studied with this device.”
The evolution of a milestone in stent technology is only beginning; you will be hearing a lot more about this remarkable advance in endovascular stent grafting for thoracic aortic aneurysms.
More About the Stent
Dr. Wheatley explains: “This type of stent functions differently than coronary stents even though they both have an open mesh.
“This stent was developed by a team of engineers who understood fluid dynamics and the role of blood flow in an aneurysm sac.
“These specialists took their understanding of fluids and applied it in a way that no one had previously thought of with regards to treating aneurysms.”
Update As of 2026
Progress has shifted more towards custom branched/fenestrated stent grafts and hybrid arch devices rather than multilayer versions.
Endovascular aortic technology overall has advanced significantly. The big development is that the FDA has approved the NEXUS Aortic Arch Stent Graft System in 2026 for certain aortic arch diseases and chronic dissections.
The ascending aorta and arch have long been considered the “last frontier” for endovascular repair.
 Dr. Wheatley is an internationally recognized expert in aortic treatments and specializes in open and endovascular repair of complex aortic diseases plus the surgical treatment of coronary artery disease and valvular heart disease.
Dr. Wheatley is an internationally recognized expert in aortic treatments and specializes in open and endovascular repair of complex aortic diseases plus the surgical treatment of coronary artery disease and valvular heart disease.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.