Suppose a passenger on an airplane develops an apparent pulmonary embolism; what should, or CAN, you do?
A deep vein thrombosis can develop while a person is on an airplane.
What might be done for help if this DVT migrates and becomes a pulmonary embolism, and a doctor just happens to be on the plane—a doctor who has treated pulmonary emboli?
“You will not show signs of a pulmonary embolus on an airplane,” says Michael P. Zimring, MD, Director, Travel Medicine, LLC at Mercy Medical Center, Baltimore, Maryland..
“The PE usually breaks off from a clot starting in the lower extremities — and that takes a while to develop.
“You usually show signs of a pulmonary embolus after a significant time of first forming a clot in the leg. Sometimes it is fast, but not usually.”
In a hospital setting, the treatment for a pulmonary embolus is IV administration of a “clot busting” or thrombolytic drug.
Doctor on Airplane Suspects Passenger Has a Pulmonary Embolism
But what if a doctor on a plane suspected that a passenger had a PE (based on symptoms, risk factors), and that doctor just happened to have a clot busting drug and syringe in his medical kit?
These are fair questions for a layperson to wonder about.
Though thrombolytics carry the risk of dangerous internal bleeding as a side effect, it’s reasonable for a layperson to wonder about this if a passenger has an apparent pulmonary embolism and is 35,000 feet off the ground.
Diagnosing a Pulmonary Embolism
A pulmonary embolism cannot be confirmed based on just symptoms (sudden difficulty breathing, chest pain, coughing up blood) and risk factors for DVT (prolonged inertia in an airplane, obesity, smoker, among many others).
Back to that doctor on the plane. What if he also has a stethoscope and listens to the distressed airline passenger’s heart?
A pulmonary embolism can change the way the heartbeat sounds through a stethoscope.
Dr. Zimring explains, “A typical physician will not hear a strain of the right heart through a stethoscope, and no one will be able to detect a PE by physical means.
“No one would dare treat a pulmonary embolus by injecting a thrombolytic on a plane because there is no way he could be sure the patient has a PE.
“There are many factors to be taken in consideration before injecting a thrombolytic in the best hospital environment.
“In addition, the physician might not be covered under the Good Samaritan Laws if he did such a specialized procedure in an emergency situation.”
Prevention of Blood Clots Triggered by Air Travel
If you’re worried about developing a pulmonary embolism as a result of flying, take precautions:
Stay well-hydrated throughout the plane trip; exercise the calve muscles every 15 minutes during the flight; don’t be seated for more than an hour; and avoid alcohol.
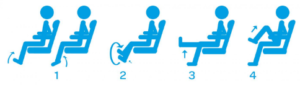
Exercises during air travel
 Dr. Zimring has 40+ years of experience diagnosing and treating a host of medical conditions.
Dr. Zimring has 40+ years of experience diagnosing and treating a host of medical conditions.
 Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
Lorra Garrick has been covering medical, fitness and cybersecurity topics for many years, having written thousands of articles for print magazines and websites, including as a ghostwriter. She’s also a former ACE-certified personal trainer.
.



































